Abstract
John Davies Thomas (1844–1893) described a two-ounce drop-bottle for chloroform in 1872 while he was a resident medical officer at University College Hospital, London. After working as a ship’s surgeon, he settled in Australia. In May 1875, Thomas presented a paper on the mortality from ether and chloroform at a meeting of the Medical Society of Victoria in Melbourne, Victoria. Surveys conducted in Europe and North America had established that the mortality from chloroform was eight to ten times higher than that from ether. At that time, chloroform was the most widely administered anaesthetic in Australia. Thomas’ paper was published in The Australian Medical Journal and reprinted by the Medical Society of Victoria for distribution to hospitals in the Colony of Victoria. Later that year, Thomas moved to Adelaide, South Australia, where he may have been influential at the Adelaide Hospital in ensuring that ether was administered more often than chloroform. It does not appear that Thomas’ papers on anaesthesia had a significant effect on the conduct of anaesthesia in Victoria or New South Wales.
On 5 May 1875, Dr John Davies Thomas read a paper comparing the mortality from ether and chloroform at a monthly meeting of the Medical Society of Victoria. The importance of Thomas’ paper was apparent to the members of the Society who attended the meeting. At the suggestion of one of the surgeons, it was decided that the Medical Society of Victoria would distribute the paper to hospitals in the Colony of Victoria. Thomas’ paper was published later that month in the Society’s journal, The Australian Medical Journal, 1 and reprinted by the Society as a pamphlet. 2
Thomas was at that time a resident surgeon at Clunes Hospital in Victoria. He was a recent migrant to the Australian colonies, having worked a few years earlier as a resident medical officer and ‘chloroformist’ at University College Hospital, London, UK. The paper that he presented in Melbourne was, according to anaesthesia historian Gwen Wilson, the first ‘reasoned evaluation’ of the mortality associated with ether and chloroform presented by a person with ‘special knowledge of anaesthetics’. 3 Wilson, however, had not associated Thomas with his eponymous chloroform drop-bottle, described by him in 1872 while he was working in London. 4
This article will examine the medical career of John Davies Thomas, who worked for a few months in the Colony of Victoria in 1874–1875, before moving to Adelaide, South Australia. In the 1880s, Thomas became an authority on hydatid disease. He was one of the leading South Australian doctors of the nineteenth century. In this article, particular emphasis will be placed on Thomas’ contributions to anaesthesia: his experience in the administration of anaesthesia in London, his description of a drop-bottle for chloroform, as well as his papers on the mortality associated with anaesthesia. John Davies Thomas should not be confused with the surgeon David John Thomas (1813–1871) who performed the first operation under etherisation in Melbourne in August 1847. 5
Information on Thomas was initially gleaned from published obituaries and biographies. As might be expected, there were inconsistencies in some of the reported details. Where possible, Thomas’ biographical details were verified by examination of contemporaneous notices in newspapers and medical journals, and in the official records of institutions such as the Adelaide Hospital and the University of Adelaide.
John Davies Thomas (1844–1893)
John Davies Thomas (Figure 1) was born in Swansea, Wales, on 11 October 1844, the eldest son of Rev. Thomas Thomas, a Congregational minister.6–10 Two of his maternal great uncles served as naval surgeons under Horatio Nelson. 8

John Davies Thomas, MD, FRCS (1844–1893). Photograph by Johnstone O’Shannessy and Company, 55 & 57 Collins Street East, Melbourne, Australia. Image from the State Library of South Australia, B 9387/89.
Thomas studied medicine at University College, a member institution of the University of London. The university received a royal charter in 1836 to award degrees to students of affiliated schools and colleges. The calendars of University College record that Thomas first enrolled in the medical course in 1862–1863. Thomas obtained a bachelor of medicine (MB) degree in 1869, and a doctor of medicine (MD) degree in 1871.
During his medical training Thomas received a number of certificates of honour, along with several silver and gold medals.
8
Three awards—in medicine, midwifery and forensic medicine—are mentioned in the dean’s report for 1868–1869:
11
At the second M.B. Examination: at the Examination for Honours in Medicine, Mr. John Davies Thomas obtained the second place, and a Gold Medal, with the number of marks qualifying for the Scholarship. At the Examination for Honours in Midwifery, Mr. John Davies Thomas obtained the first place, the University Scholarship of £50 per annum, tenable for two years, and a Gold Medal. At the Examination for Honours in Forensic Medicine,… Mr. J. D. Thomas obtained the second place in the Third Class.
Thomas became a ship’s surgeon in the P & O Steam Navigation Company. His first assignment was on a ship travelling to India. He had intended to return to London, but his ship was ordered to sail to Australia. He continued to work as a ship’s surgeon for another two years. Between June and October 1874, he was the ship’s surgeon on the Ellora, travelling between Sydney and Melbourne. 12 In June 1874, while he was the ship’s surgeon on the Ellora, Thomas registered his qualifications in Victoria, an indication that he intended to settle in the colony (Medical Board of Victoria, certificate number 750, issued on 27 June 1874).13,14 He continued to work on the Ellora until October 1874. 12 On 4 November 1874, Thomas attended a monthly meeting of the Medical Society of Victoria as a ‘visitor’. 15
It is not clear whether Thomas made any attempts to work in Melbourne, either at the Melbourne Hospital or in private practice. His first hospital appointment in Australia was at Clunes Hospital, where he worked for around six to nine months as the resident surgeon (or resident medical officer). Clunes is 35 km north of Ballarat, Victoria, and 150 km from Melbourne. His appointment at the hospital was reported in The Ballarat Star newspaper on 8 December 1874. 16 In February 1875, he was elected as a member of the Medical Society of Victoria. 17 Six months later, The Australian Medical Journal reported that ‘Dr. J. D. Thomas, late of the Clunes Hospital, has been appointed Senior House-surgeon to the Adelaide Hospital.’ 18
Thomas registered his qualifications with the South Australian Medical Board on 6 October 1875. 19 To register in the colony he would have to present his diplomas and certificates to the Medical Board’s secretary at least three days before a board meeting, attend one of the quarterly meetings of the Medical Board where he would be required to make a declaration regarding his medical training, and pay a fee of one guinea. Thomas’ name appears on a list of ‘duly qualified Medical Practitioners’ published in The South Australian Government Gazette, 7 October 1875. 20
Thomas was the senior house surgeon at the Adelaide Hospital for about a year (at that time the hospital admitted around 2000 patients in a year, and had a daily average of 160 inpatients, who were attended by one senior and one junior house-surgeon). In November 1876, The Australian Medical Journal carried a notice that Thomas had ‘resigned the senior house surgeonship of the Adelaide Hospital’. 21 However, hospital records indicate that Thomas remained a senior house surgeon at the hospital until the end of the year. His involvement with the hospital did not end with his resignation. He was appointed in 1878 to the hospital’s Board of Management. In 1880, he was appointed as an honorary medical officer (from 1883 this appointment was known as ‘honorary physician’). Thomas retired from the honorary position in 1884. He was reappointed in 1887, and remained an honorary physician at the hospital until 1890 when he retired because of ill health.
After resigning as a senior house surgeon at the Adelaide Hospital, Thomas became a partner in the medical practice of Dr Hugh Ferguson (1831–1887) in Glenelg, South Australia. On 10 June 1878, Thomas married Eleanor, fourth daughter of the Hon. Walter Duffield, MLC, of Para Para Estate, Gawler, South Australia. 22 Either in the year of his marriage, or sometime in 1879, Thomas joined Dr Horatio Thomas Whittell (1826–1899) in partnership. By December 1879, Whittell was intending to leave the area and Thomas may have then acquired Whittell’s medical practice. On 31 December 1883, Dr Alfred Austin Lendon (1857–1935) became a partner of Thomas.
Thomas had remained a member of the Medical Society of Victoria after he had moved to South Australia. During the 1880s, his primary research interest was hydatid disease, a parasitic disease then endemic in the Australian colonies. Over a period of 11 years, Thomas published more than 30 papers on the natural history of the parasite and on hydatid disease. While the majority of his papers were presented and published in Australia, he did publish papers in The Lancet, The British Medical Journal, Proceedings of the Royal Society of London and in veterinary journals. Thomas also read papers on hydatid disease before the Royal Society of South Australia. In 1877, he had been elected fellow of the Royal Society of South Australia, and member of the Philosophical Society of Adelaide. Besides the published papers, his prodigious research appears in a number of pamphlets and books. In 1884, Thomas published a book on hydatid disease. 23 A second volume of his papers on hydatid disease was published posthumously in 1894. 8
In 1885 Thomas travelled to Europe where he undertook medical studies and visited hospitals in London and Vienna. He left Adelaide for London on 3 January 1885 on the RMS Valetta. In June 1885, two of his papers on the dog tapeworm were communicated by Dr TS Cobbold to the Royal Society of London. Thomas read a paper on the treatment of pulmonary hydatid cysts at the Annual Meeting of the British Medical Association held in Cardiff, July 28–31, 1885. His partner Lendon remarked that Thomas believed he could return to work at University College Hospital, London. 24 In their partnership agreement, Thomas had declared his ‘intention of taking a holiday with a certain proviso in case he [Thomas] stayed on in London’ (papers of Dr Alfred Austin Lendon, PRG 128, State Library of South Australia, Adelaide, SA).
After an absence of 18 months, Thomas returned to Adelaide on 3 July 1886 on the RMS Ballarat. He resumed his medical practice in the city and was appointed in November 1886 as a lecturer on the ‘Principles and Practice of Medicine and Therapeutics’. 25 Thomas held this appointment in the Adelaide Medical School jointly with Dr, later Sir, Joseph Verco (1851–1933).
Thomas had been a member of the council of the University of Adelaide since 1877—he was elected by the senate in December 1877, and re-elected in 1880. He had resigned from the council in February 1885 (his resignation became effective while he was overseas). He was re-elected as a member of the council in 1888, and remained a member until 1891. Also in 1877, the university conferred on him a doctorate in medicine (MD) ad eundem gradum. The university calendars reveal that in 1878 Thomas delivered a course of public lectures on ‘Elementary Physiology’. 26 As a member of the University Council, Thomas would have been intimately involved in the deliberations and planning that occurred over a period of several years before the Adelaide Medical School was opened. The first lectures in the medical school commenced in March 1885 with seven students, six of whom completed the first year.27,28 Established in 1874, the University of Adelaide is the third oldest university in Australia.
Thomas was the president of the South Australian branch of the British Medical Association, 1887–1888. He succeeded Joseph Verco, who was the Association’s president (1886–1887) when the first Intercolonial Medical Congress of Australasia was convened in Adelaide in 1887 (the jubilee year of South Australia). Verco was president of the Congress; Thomas was one of 12 vice-presidents of the Congress, ten of whom were presidents of other colonial medical societies and associations.
Thomas’ partnership with Lendon was dissolved at the end of 1887. Three years later, a chronic form of paralysis (described in some accounts as ‘general paralysis’) compelled Thomas to retire from active work and as a lecturer at the medical school. He made a short trip to New Zealand after his retirement. On his return to Adelaide, Thomas may have lived for a short time at Waverley (a village or township in the Adelaide Hills, now part of the town of Crafers). For the last two or three years of his life, Thomas lived in the township of Blackwood (now a southern foothills suburb in the City of Mitcham, approximately 14 km from central Adelaide) where he died on 30 January 1893, aged 48. 6
At the time of his retirement, Thomas was working on a second volume on hydatid disease. After his death, his papers were edited and arranged by Dr Lendon, and published posthumously in 1894. 8 This volume contains a memoir of Thomas, with a description of his career and a few words regarding his character: ‘By nature, he was gentle and kindly, warm-hearted, generous, and affectionate. He was very honest, straightforward and outspoken, and, perhaps, somewhat over impulsive. He was sympathetic in voice and manner, as well as at heart, and was much beloved by his patients.’ 8
In 1896, Thomas’ widow, Mrs Eleanor Davies Thomas, donated £400 to the University of Adelaide to establish annual scholarships in memory of her husband. In 1934, a further £200 was bequeathed to the Davies-Thomas scholarship fund. The Dr Davies-Thomas scholarship (also known as the Dr Davies-Thomas prize) is now awarded annually by the University of Adelaide to the student who is placed first in the whole of the fourth year medical examination. In 2014, the value of the scholarship was A$200.
Dr WT Hayward, retiring president of the South Australian branch of the British Medical Association, remarked on Thomas in an address to the association in 1911: ‘Dr Davies Thomas will always be remembered for the valuable work he did in connection with hydatid disease. Wonderfully industrious in all matters connected with his profession he made himself proficient in the German language while he was in active practice in order that he might study German medical literature. A ready writer and fluent speaker, his papers and speeches were a feature in the work of the branch. Death overtook him at the zenith of his fame.’ 29
Thomas’ contributions to anaesthesia
Thomas’ chloroform drop-bottle
In March 1872, while he was a resident medical officer at University College Hospital in London, Thomas published a description of a ‘drop-bottle for chloroform’ (Figure 2). 4 Thomas had in fact devised the drop-bottle in 1871—this detail was revealed by Thomas in the paper he read in Melbourne in May 1875. 1 Made by Mayer & Meltzer of Great Portland Street, London, Thomas’ drop-bottle was a two-ounce (16 fluid drachms or approximately 57 ml) graduated glass bottle with a spring-loaded metal stopper. Pressure on the flat disc of the stopper allows the liquid anaesthetic to flow from the spout. A spring closes the dropper when pressure on the disc is released. An 1890 catalogue of Down Bros. listed a similar drop-bottle called a ‘Spring Top’, probably a copy of Thomas’ drop-bottle. 30

Description of a ‘drop-bottle for chloroform’ – published by John Davies Thomas in The Lancet, 2 March 1872. 4 Image courtesy of Bayerische Staatsbibliothek München, bsb11033986, image 294. Reproduced with the permission of Elsevier.
There is one notable difference between the illustration of the drop-bottle in Thomas’ original communication in The Lancet, 4 and the illustrations of the bottle that were published in textbooks and catalogues. In Thomas’ original description (Figure 2), the drop-bottle is graduated from the bottom (1 drachm) to the top (16 drachms). 4 In the first edition (1893) of Frederick Hewitt’s textbook, Anaesthetics and their Administration (Figure 3), 31 and in a catalogue of Mayer & Meltzer, 32 the drop-bottles are graduated from the top (0 drachm) to the bottom (16 drachms). (One fluid drachm in the British Imperial System is equivalent to 3.55 ml in the metric system.)
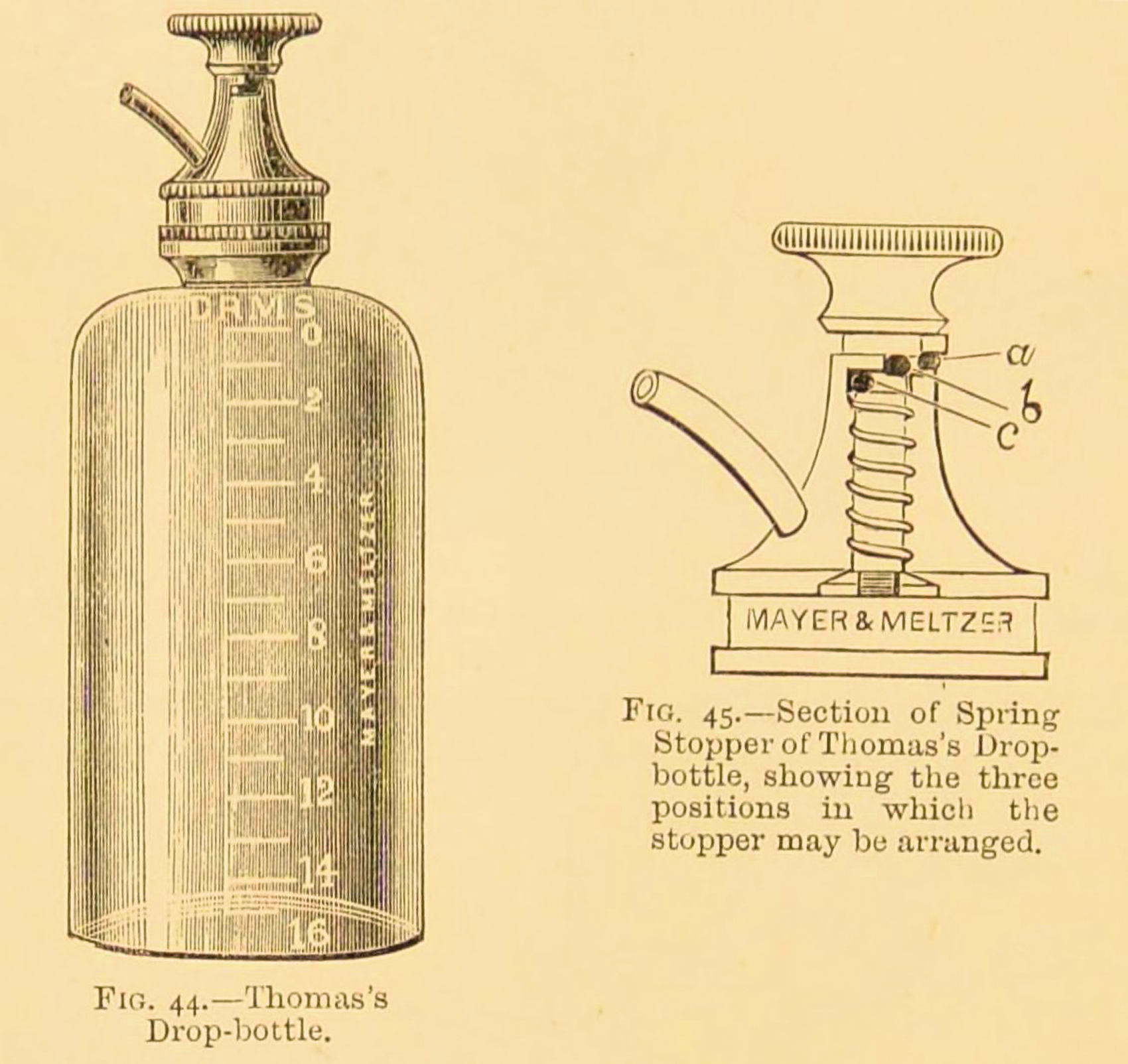
Illustration of Thomas’ drop-bottle and a section of the modified stopper introduced by Dr Sheppard. From Frederick Hewitt’s Anaesthetics and their Administration (1893), p. 192. 31
The spring stopper of Thomas’ drop-bottle was modified (Figure 3) by a Dr Sheppard, probably Charles E Sheppard (d. 1891) who was ‘Second Chloroformist to the Middlesex Hospital; Anaesthetist to Guy’s Hospital (Dental School) and the National Orthopaedic Hospital’.33,34 The chloroform drop-bottle with Sheppard’s modification (a stopper with a ‘pin and bayonet catch’) was listed in a Mayer & Meltzer catalogue in 1900 as ‘Sheppard’s–Thomas’ Drop Bottle’. 32 The catalogue lists chloroform bottles of two sizes: 2-ounce and 4-ounce.
Thomas’ papers on chloroform and ether
On Wednesday, 5 May 1875, Thomas read a paper at an ‘ordinary monthly meeting’ of the Medical Society of Victoria (held at 117 Collins Street East, Melbourne) on the mortality associated with chloroform and ether anaesthesia. 1 His interest in the subject would have been longstanding, undoubtedly relating to his appointment four to five years earlier as a ‘chloroformist’ at University College Hospital, London. Moreover, one of his patients in London had died during the administration of chloroform. Thomas remarked that he had been complimented by Joseph Clover for the care with which he had administered chloroform, and ‘yet with all his care he had had a death, so that he believed the most careful administration was not an entire assurance against risk’. 1 Apart from ether and chloroform, Thomas had also administered nitrous oxide and bichloride of methylene. He had concluded that ether was the safest anaesthetic agent, and thereafter had used it exclusively: ‘for a long time past I have used no other.’ 1
Thomas’ paper, entitled ‘A consideration of the respective merits of chloroform and vinic ether as general anaesthetics’ (Figure 4), was published later that month in The Australian Medical Journal. 1 In an introductory note to the published paper, Thomas defended his use of the term ‘vinic ether’, a term which he claimed ‘has been long in use by certain chemists in England’. 1 The adjective ‘vinic’—relating to, contained in, or derived from wine—was rarely used in medical publications where the preferred terms were ‘ether’ or ‘sulphuric ether’.

Title of the paper read by John Davies Thomas in Melbourne on 5 May 1875 at a meeting of the Medical Society of Victoria. Thomas’ paper was published in the May 1875 issue of The Australian Medical Journal. 1
At the suggestion of Melbourne surgeon William Gillbee (1825–1885), Thomas’ paper was reprinted by the Medical Society of Victoria for distribution to hospitals in the Colony of Victoria. Gillbee’s suggestion is recorded in the discussion that followed the presentation of the paper. 1 The publication of the reprint is documented in the January 1876 issue of The Australian Medical Journal (the January issue usually carried a report of the Society’s annual meeting and a review of the Society’s activities during the previous year): ‘Copies of Dr. Thomas’s paper on Chloroform and Ether were sent to all the hospitals in Victoria, also at the Society’s cost.’ 35
The reprint of Thomas’ paper was listed by John Alexander Ferguson in his seven volume Bibliography of Australia (published between 1941 and 1969). 36 Ferguson, though, had listed just one copy of the reprinted article—a copy held by the Mitchell Library (now part of the State Library of New South Wales). 36 Enquiries by the author (RPH) have identified other copies of the pamphlet in Australian libraries—copies are held by the Barr Smith Library, University of Adelaide (Figure 5), and the History of Medicine Library, Royal Australasian College of Physicians, Sydney, NSW. It is likely that a copy of the pamphlet is held in the archives of AMA Victoria that were donated to the Medical History Museum, University of Melbourne. One copy of the pamphlet is listed by the University of Alabama, Birmingham, Alabama, USA.

Title page of the reprint of John Davies Thomas’ paper on chloroform and ether, originally published in the May 1875 issue of The Australian Medical Journal. Image courtesy of the Barr Smith Library, University of Adelaide, Adelaide, SA.
Gwen Wilson observed that Thomas’ paper was ‘an important one in the history in Australia, for not only was it the first reasoned evaluation of ether v chloroform presented to a medical society by a man with special knowledge of anaesthetics, but it was the first paper on any subject which a meeting voted should be printed and copies sent to every hospital in Australia.’ 3 Thomas’ paper was, in fact, sent to every hospital in the Colony of Victoria. 35
It was also a lengthy paper—20 pages in total, including the discussion which followed Thomas’ presentation. With the ‘limited means’ at his disposal when preparing the paper, Thomas had collected 172 fatal cases ‘attributable to the effects of chloroform itself’—he had excluded ‘cases where death occurred during self-administration’. 1
The most striking statistics presented by Thomas were the anaesthesia mortality rates: the almost ten-fold difference in mortality between ether (1:23,204) and chloroform (1:2723), figures that had been published in America in 1870.1,37 The paper by Edmund Andrews (1824–1904) of Chicago does, however, include statistics from hospitals in Britain and Continental Europe. 37 Thomas also cited a British estimate of deaths under chloroform (1:2500), a figure that was similar to the one published by Andrews. Despite the fact that there would have been inconsistencies in the disclosure of fatalities and the collection of case numbers, the reported figures do not leave any doubt that there was a substantial difference in the safety of the two anaesthetic agents.
Although Thomas’ paper was considered ‘important’ by Gwen Wilson, she observed that its clinical impact was limited, even after it was published. According to Wilson, ‘The discussion on the paper at the meeting, together with the decision to circulate it, might lead to the supposition that chloroform would, from that evening, vanish from Victoria. They stood up, those men, one and all, and said yes, ether was safer, yes, ether should be universally employed – and went straight out next day and gave chloroform.’ 3
Before ending the May 1875 paper, Thomas spoke about anaesthesia equipment and his technique for inducing anaesthesia with each agent. He declared that he had no experience with the administration of a mixture of one part alcohol, two parts chloroform and three parts ether that was recommended by the Chloroform Committee of the Royal Medical and Chirurgical Society (now known as the Royal Society of Medicine). This mixture, also known as the A.C.E. mixture, has been attributed to the Scottish physician and physiologist George Harley (1829–1896).
Later in the year Thomas submitted another paper on anaesthesia, this time as the senior house surgeon of Adelaide Hospital. This paper was published in The Australian Medical Journal in two parts, the first in November 1875, and the concluding part was published in January 1876.38,39 Thomas reported that animal experiments conducted in London and Florence had shown that chloroform had a direct depressant action on the heart. He had written to doctors in America for information on deaths from ether. One of the replies he had received was from the Boston surgeon Henry Jacob Bigelow (1818–1890), who had witnessed the first public demonstration of surgical etherisation on 16 October 1846 at the Massachusetts General Hospital.38,39
Use of chloroform and ether at the Adelaide Hospital
At the Adelaide Hospital, a death from chloroform occurred on 25 January 1875, followed ten weeks later by a second death on 1 April. (In One Grand Chain, Gwen Wilson reported that the second fatality from chloroform occurred on 3 March. 3 ) In the latter half of the year, Thomas commenced his appointment as a senior house surgeon at the hospital. Wilson has noted that ether was the preferred anaesthetic employed at the Adelaide Hospital from 1875. 2
However, it is not clear when this transition might have occurred. At the time of writing, there was no information to establish whether the preference for ether as an anaesthetic occurred before Thomas’ arrival at the hospital, or whether he was instrumental in promoting the administration of ether instead of chloroform. As a senior house surgeon, Thomas would have administered anaesthesia or supervised its administration at the hospital. After resigning as a senior house surgeon, Thomas would have been able to continue promoting etherisation at the hospital through his honorary appointment at the hospital and as a member of the hospital’s Board of Management. Undoubtedly, South Australian lives would have been saved by avoiding chloroform.
The annual reports of Adelaide Hospital for the years 1875 and 1876 do not contain any statements regarding the aforementioned deaths under chloroform, or any statistics on the anaesthetics that were administered. During 1875, the number of operations performed at the hospital was 213, with 14 deaths. In 1876, the number of operations had increased to 314 (eight deaths).
Discussion
Although Thomas did not publish any papers on anaesthesia after 1876, he had perhaps given greater attention to the safety of anaesthesia than any other doctor in the Australian colonies at that time. His exceptional intellect and scientific curiosity could have made him a leader in efforts to make anaesthesia safer. However, there were no opportunities at that time in Australia for specialisation or research in anaesthesia. The first hospital appointments in Australia of an anaesthetist or ‘chloroformist’ were made in 1888. 40 Laboratory research into the cause of death under chloroform would not be conducted in Australia until the late 1890s. 41
Thomas, as a senior house surgeon and later as an honorary physician at the Adelaide Hospital, may have been influential in ensuring that ether became the preferred anaesthetic agent at the hospital. (The author could not locate any primary source documents to verify this statement which is based on Gwen Wilson’s assertion in One Grand Chain. 3 ) In contrast in Victoria, Thomas’ paper did not lead to any significant change in the administration of anaesthesia. Chloroform remained the most commonly used anaesthetic at the Melbourne Hospital and at other Victorian hospitals. Likewise in New South Wales, chloroform would remain the most widely used anaesthetic agent for several more decades, well into the twentieth century.
Chloroform had a number of advantages over ether. The most important perhaps was that chloroform was more pleasant to inhale and more potent as an anaesthetic, resulting in a smoother and more rapid induction of anaesthesia. Recovery from chloroform anaesthesia was more rapid than after etherisation, and there was less postoperative nausea and vomiting. Unlike sulphuric ether, chloroform was not flammable. Two leading proponents of chloroform—James Young Simpson and John Snow—ensured that it remained the most commonly used anaesthetic in the United Kingdom and its colonies. James Y Simpson (1811–1870), Professor of Midwifery at Edinburgh University, was one of the most influential doctors in the mid-nineteenth century. He had introduced chloroform as an anaesthetic in November 1847. Understandably protective of his innovation, Simpson did not recognise, or would not admit, that there were significantly more fatalities associated with chloroform than with ether. He staunchly defended the safety of chloroform even as the number of deaths continued to rise. Furthermore, he failed to understand the cause of the fatalities associated with chloroform. John Snow (1813–1858) was the English physician, anaesthetist and epidemiologist who developed a scientific approach to advance our understanding of the new technique for producing insensibility. Snow’s extensive publications on anaesthesia and his endorsement of chloroform would have promoted its acceptance by ordinary doctors who would not have been as experienced and adept as he was in administering chloroform.
In America, chloroform was not as frequently administered as ether. In contrast, chloroform remained the most widely used anaesthetic agent in the United Kingdom and its colonies, notwithstanding the number of fatalities associated with it. Even though the cardiac effects of chloroform were increasingly recognised in the latter part of the nineteenth century, compelling evidence that ventricular fibrillation occurred during the sudden cardiovascular collapse caused by chloroform would not be elucidated until the first decade of the twentieth century.
Benjamin Ward Richardson’s estimate of the deaths from chloroform (1:2500) in the United Kingdom was similar to figures that were reported in other large surveys.1,37 More alarming, however, was the state of affairs in institutions that had considerably higher fatalities, ranging from 1:300 to 1:1000. Two reports suggest that the larger surveys may have underestimated the fatalities associated with chloroform.
The first is a report prepared by Melbourne anaesthetist Edward Henry Embley (1861–1924) for the annual report of Melbourne Hospital, 1908–1909. Embley’s ‘Honorary Anaesthetist’s Report’ was reproduced by Gwen Wilson in One Grand Chain (Volume 1, p. 376). During the year covered by the report, anaesthesia was administered for 2642 operations: local or regional analgesia was used for 349 cases; general anaesthesia for 2293 cases. Chloroform was administered in 505 cases: it was the sole anaesthetic in 290 cases, and in 215 cases chloroform was combined with ether (207 cases) or ‘somnoform’ (eight cases). There were three fatalities ‘under anaesthesia’—two deaths occurred under chloroform, and one death occurred in association with spinal analgesia. (‘Somnoform’ was a mixture of three liquid anaesthetics: ethyl chloride, methyl chloride and ethyl bromide; introduced in 1901, it had a short-lived popularity.)
A year later (1910), Embley published a paper in which he cited figures from St Bartholomew’s Hospital (London, UK) for the decade 1891–1900: chloroform was administered in 23,452 cases, with 20 deaths (one death for 1173 cases); ether was administered in 15,495 cases, with no deaths. 42
Although the problem with chloroform was recognised almost immediately after its introduction as an anaesthetic agent, relatively few surgical operations were performed at that time. Thus, we expect fatalities attributable to chloroform would occur rarely in the career of the average doctor, and years apart in any institution. The infrequent deaths would create an illusion of safety, allowing the anaesthetic to become more widely accepted. Sporadic fatalities may not be correctly attributed, and it would take several years for a recognisable pattern of cases to emerge. By then, the average doctor, having become accustomed to administering chloroform, would have been reluctant to change because there were no alternative anaesthetics with similar efficacy and ease of administration.
Another consideration regarding the acceptance of chloroform as an anaesthetic is the relatively low number of chloroform deaths in comparison with other causes of death in the nineteenth century. Although chloroform deaths were reported in the press and medical journals, there were considerably more deaths from accidents and outbreaks of infectious diseases such as influenza, measles, diphtheria, typhoid and cholera—as well as the ever-present tuberculosis, which caused up to a quarter of all deaths in the early nineteenth century. With regard to hydatid disease, Thomas quoted the official government figures for deaths from the disease in the Australian colonies. In a 20-year period (1862–1881), 584 deaths in Victoria were attributed to hydatid disease, although by the end of the period surveyed, there were 48 deaths in a year. 8
In 1893, James W Barrett published a brief communication on ‘Deaths from chloroform in Melbourne and suburbs.’ 43 There were 16 deaths from chloroform in a five-year period from 1888 to 1892; about three deaths per year for a population that Barrett estimated as 450,000. Barrett wrote, ‘The total is not as high as I had expected, but “ ‘tis enough.” ’ 43 Chloroform was ‘more dangerous to life than snakes, since the death-rate from snake-bite for the whole colony, and chloroform for Melbourne, are about the same.’ 43 The figures cited by Barrett may be disputed. His article, just over a page in length, cannot be considered as a wide-ranging review or analysis.
In Australia in the 1880s, several proposals for the appointment of an anaesthetist or ‘chloroformist’ were rejected by hospital management committees. Gwen Wilson has documented the missed opportunity to appoint a chloroformist at Melbourne Hospital in 1882. 44 The use of the term ‘chloroformist’ could be an indication of the preference for chloroform over ether. The first hospital appointments of an anaesthetist (or ‘chloroformist’) were made in 1888 at St Vincent’s Hospital in Sydney, and at the Alfred Hospital in Melbourne. 40 Dr Geoffrey Frederick Travers, the Alfred Hospital’s honorary ophthalmologist since 1886, was appointed as the hospital’s honorary chloroformist in June 1888. Travers resigned from both positions in 1891 to pursue further studies in ophthalmology.
Anaesthesia-related laboratory research would only commence in Melbourne in the 1890s. Embley, who was the honorary anaesthetist at the Melbourne Hospital (he was appointed in 1894) and a lecturer in anaesthetics at the University of Melbourne, conducted animal experiments to investigate the cause of sudden death under chloroform. 41 Embley’s research was published in 1902 in three articles in The British Medical Journal, the research having already earned him an MD from the University of Melbourne in 1901.45–47 By the first decade of the twentieth century, there was convincing evidence from experimental studies, including those of Embley, of the cardiotoxic effect of chloroform, despite the fact that the mechanism of cardiac arrest was not fully understood at the time.
Conclusion
Thomas had graduated from his medical studies in London with distinction. While working as a resident medical officer at University College Hospital, London, he had been appointed as the hospital’s chloroformist. The health problems that forced him to resign from the hospital in 1872 may have induced him to settle in Australia.
In March 1872, Thomas described a two-ounce drop-bottle for chloroform that he had devised sometime in 1871.1,4 Thomas’ drop-bottle was manufactured by Mayer & Meltzer—the company also sold Dr Sheppard’s modification of Thomas’ drop-bottle. 32
The death of one of Thomas’ patients under chloroform in London may have been the initial stimulus to his enquiries into the mortality associated with anaesthesia. While working at Clunes Hospital in Victoria in 1875, Thomas was ‘emboldened’ to prepare his paper by two recent deaths under chloroform ‘in a neighbouring colony’ (the deaths in February and April 1875, in Adelaide, South Australia). In May 1875, Thomas presented a well-researched paper on the subject at a monthly meeting of the Medical Society of Victoria (held in Melbourne). His paper was published in The Australian Medical Journal 1 and reprinted by the Medical Society of Victoria for distribution to hospitals in Victoria. 2
Thomas had almost certainly given greater thought to the safety of anaesthesia than any other doctor in the Australian colonies at that time. His experience and intellect could have made him a leader in efforts to make anaesthesia safer, especially if he had remained in London. However, in Australia in the 1870s, there were no prospects for hospital appointments for a doctor who had a special interest in anaesthesia. The first appointments of anaesthetists at Australian hospitals would be made in 1888, more than a decade after Thomas’ arrival in the colony. Although Thomas did not publish any papers on anaesthesia after 1876, he may have been influential at the Adelaide Hospital in ensuring that ether was administered more often than chloroform. It does not appear that Thomas’ papers on anaesthesia had a significant effect on the conduct of anaesthesia in Victoria or New South Wales.
Supplemental Material
sj-pdf-1-aic-10.1177_0310057X211031569 - Supplemental material for John Davies Thomas: Chloroformist in London and pioneer South Australian doctor
Supplemental material, sj-pdf-1-aic-10.1177_0310057X211031569 for John Davies Thomas: Chloroformist in London and pioneer South Australian doctor by Rajesh P Haridas in Anaesthesia and Intensive Care
Supplemental Material
sj-pdf-2-aic-10.1177_0310057X211031569 - Supplemental material for John Davies Thomas: Chloroformist in London and pioneer South Australian doctor
Supplemental material, sj-pdf-2-aic-10.1177_0310057X211031569 for John Davies Thomas: Chloroformist in London and pioneer South Australian doctor by Rajesh P Haridas in Anaesthesia and Intensive Care
Supplemental Material
sj-pdf-3-aic-10.1177_0310057X211031569 - Supplemental material for John Davies Thomas: Chloroformist in London and pioneer South Australian doctor
Supplemental material, sj-pdf-3-aic-10.1177_0310057X211031569 for John Davies Thomas: Chloroformist in London and pioneer South Australian doctor by Rajesh P Haridas in Anaesthesia and Intensive Care
Supplemental Material
sj-pdf-4-aic-10.1177_0310057X211031569 - Supplemental material for John Davies Thomas: Chloroformist in London and pioneer South Australian doctor
Supplemental material, sj-pdf-4-aic-10.1177_0310057X211031569 for John Davies Thomas: Chloroformist in London and pioneer South Australian doctor by Rajesh P Haridas in Anaesthesia and Intensive Care
Footnotes
Author contribution(s)
Acknowledgements
The author would like to thank Laurie Mather, Richard Bailey, Michael Cooper, John Crowhurst and George Bause for reviewing the manuscript.
The author is grateful to the librarians and archivists at the State Library of South Australia for documents relating to John Davies Thomas and Alfred Austin Lendon, and for scanning the 800-page (unpublished) autobiography and reminiscences of Dr Alfred Austin Lendon (1857–1935): ‘Papers of Dr Alfred Austin Lendon,’ PRG 128, State Library of South Australia, Adelaide, SA.
The author has also been assisted in his research by librarians, archivists and curators at other institutions: History of Medicine Library, Royal Australasian College of Physicians, Sydney, NSW; Wood Library-Museum of Anesthesiology, Schaumburg, Illinois, USA; Australian and New Zealand College of Anaesthetists, Melbourne, Vic; Heritage Office, Royal Adelaide Hospital, Adelaide, SA; University of Adelaide Archives and Barr Smith Library, University of Adelaide, Adelaide, SA; Brownless Biomedical Library and Medical History Museum, University of Melbourne, Melbourne, Vic; and Archives, Royal Melbourne Hospital, Melbourne, Vic.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
