Abstract
Background:
The wearing of socks and insoles may affect the ability of the foot to detect tactile input influencing postural balance.
Objectives:
The aim of this study was to investigate whether (1) thick socks adversely affected the elderly postural balance and (2) orthopedic insoles could improve the elderly postural balance while wearing thick socks.
Study design:
Repeated-measures study design.
Methods:
In total, 14 healthy older adults were recruited. A monofilament test was conducted to evaluate foot plantar sensation with and without thick socks. Subjects then performed the Romberg tests under three conditions: (1) barefoot, (2) with socks only, and (3) with both socks and insoles. Postural balance was assessed by measuring the center of pressure movement during standing in each experimental condition.
Results:
Thick socks significantly decreased the monofilament score (p < 0.001), suggesting reduction in ability to detect external forces. All center of pressure parameters increased significantly while wearing thick socks (p < 0.017), implying reduction of postural stability. They then decreased significantly with the additional use of insoles (p < 0.017).
Conclusion:
Previous studies have documented the changes in plantar pressure distribution with the use of orthopedic insoles. This study further suggests that such changes in contact mechanics could produce some balance-improving effects, which appears not to have been reported earlier.
Clinical relevance
Wearing thick socks reduces plantar pressure sensitivity and increases postural sway which may increase risk of falls. Orthopedic insoles and footwear with similar design could potentially be a cost-effective method in maintaining postural balance when wearing thick socks.
Background
Falls and fall-induced injuries are associated with high morbidity and mortality rate, significant reduction of quality of life, and enormous hospitalization expense. 1 Plantar tactile sensation plays a critical role in balance control, as it provides the central nervous systems with instantaneous and continuous information on the characteristics of the ground support surface and the movement of the body relative to the foot. 2 Declined plantar tactile sensation can induce poor balance and predispose risk of falls. 2 Aging, diabetic neuropathy, and rheumatoid arthritis can lead to impairment in plantar tactile sensation. 3 In addition, some footwear could reduce the tactile input to the plantar surface of foot and consequently influence the postural stability. 4
Wearing thick or even multiple layers of socks could improve comfort 4 and protect the feet from frostbite during cold weather. 5 However, the use of socks could be linked to increased falling risks.4,6 The reason behind this phenomenon could be that the soft materials under the feet could attenuate the plantar tactile sensory input,4,6 which is crucial for balance control. This mechanism could also explain the poorer postural stability caused by either wearing shoes with soft soles 4 or standing on a soft foam surface. 7
Previous studies have attempted to modify the physical properties of the footwear in order to aid balance, as reviewed by Hatton et al. 8 Shoe soles and insoles made of hard materials were shown to have positive effects on improving balance. 8 It was also reported that adhering a flexible plastic tubing to the margin of foot sole 9 and some small semi-rigid plastic nubs or spikes to the insoles 10 enhanced plantar sensory input and balance. However, these designs tended to cause some pain and discomfort and altered the normal gait patterns of the users, 10 which limited their application in daily life. Meanwhile, some other studies suggested that vibrating insoles can enhance plantar sensory input and thus improve balance. 11 As the vibrator was made of rigid steel, however, users complained of pain and discomfort when using vibrating insoles. 8 It has also been suggested that the economic and practicality problems associated with vibrating insoles may outweigh their beneficial effects on balance control. 8
Orthopedic insoles are conventionally used to treat foot pain and correct foot deformity in patients. 12 Arch supports, metatarsal pads, and heel cups are key components of a pair of orthopedic insoles. Arch supports relieve plantar fasciitis by supporting the longitudinal arch and relieving soft tissue stretch. 13 Metatarsal pads relieve pain over the metatarsal heads by redistributing loadings to the metatarsal shafts. 14 Heel cups help to grasp the heel in a more neutral position. 15 Some studies reported that balance could be improved by reducing foot pain, 16 correcting foot deformities,17,18 and putting the foot and ankle joint in a more stable position15,19 on using orthopedic insoles. However, it is not known whether these balance-improving effects can still be retained in people without any foot pain or deformity.
Orthopedic insoles may also have some positive effects on balance for those without foot pain or deformity. Previous studies measuring plantar pressure distribution indicated that orthopedic insoles increased the contact area between the foot and the support surface.15,17 In addition, orthopedic insoles redistributed the plantar pressure by increasing the pressure over the metatarsal shafts and reducing the pressure over the heel and the metatarsal heads which are the commonly painful sites. 20 It just happens that the midfoot metatarsal shaft region was shown to have higher tactile sensitivity than the heel and the metatarsal heads. 3 The increased contact area and the elevated pressure over some more sensitive regions could enhance plantar tactile input, which gives traditional orthopedic insoles the potential to improve balance of people with deficits of plantar tactile sensation. However, to date, there have been no investigations of this hypothesized effect.
Different balance assessment tests have been applied in clinical practice, including the Brunel Balance Assessment, Berg Balance Scale, and Weight Shifting Test.21,22 In laboratory setting, the use of force plates allows assessment of balance to be more objective and sensitive to changes, as compared to clinical balance assessment tests. 21 Increase in center of pressure (COP) movements during standing is typically considered to be an indication of decreased postural stability. 23 More importantly, fallers tend to have more static postural sway than nonfallers. 24
This study evaluated the effects of wearing a pair of thick socks on postural balance of older adults and then further investigated whether orthopedic insoles could produce any significant changes in postural balance while wearing thick socks. Postural balance was assessed by measuring the movement of COP. It was hypothesized that conventional orthopedic insoles could improve postural balance of older adults, which was adversely affected by the use of thick socks. This study potentially uncovers the balance-improving effects of traditional orthopedic insoles and sheds new light on the application of a low-cost and practical solution for improving balance.
Methods
Subjects
Convenience sampling approach was used to recruit 14 healthy older adults aged over 65 years in this study. The subjects were fully independent, living in a community-based setting, and capable of unassisted ambulation. Subjects did not have pes planus (flat foot), pes cavus (high arch), or foot pain, as assessed by a certified orthotist. In addition, the subjects did not have self-reported history of foot injury or neurological or vestibular disorders. All subjects were able to follow the instructions and procedures of the research protocol.
All subjects provided written informed consent before participating in the study. Ethical approval was granted from the authority of local university.
Design of insoles
Figure 1 shows the insoles used in this study. They were commercially available (Foot Specialist Footcare & Products Co. Ltd, Hong Kong, China) full-length insoles made of medium firm (30–35 Shore A Hardness) ethylene-vinyl acetate (EVA), with medial longitudinal arch supports and heel cups. They were originally indicated for conditions of flat foot, plantar fasciitis, and metatarsalgia. A metatarsal pad was added to the prefabricated insoles just proximal to the second and third metatarsal heads. Three different heights of metatarsal pads (4, 6, and 8 mm) were used. The thickest possible metatarsal pad without causing discomfort was selected for each subject. The lengths of the insoles were selected, and the heights of the pads were adjusted by a certified orthotist prior to the experiment.
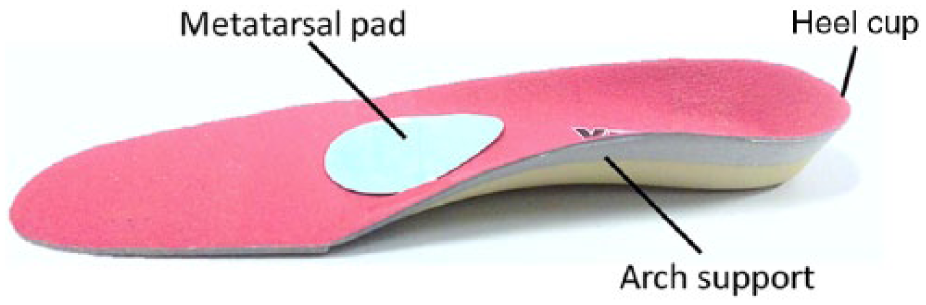
Design of the orthopedic insole.
The socks
A pair of thick socks, which was below the ankle joint, was used. The socks (88515016; Baleno Co. Ltd, Hong Kong, China) were commercially available, with a thickness of 4.5 mm at bottom, and composed of 80.6% cotton, 16.7% polyamide, and 2.7% spandex.
Procedure
This study was conducted in a university human locomotion laboratory. A Romberg test was conducted to assess the static balance following the standard procedures, 25 which were shown in a previous study to have high test–retest reliability. 26 The subjects were instructed to stand quietly on a force platform without shoes, with arms crossed resting on the opposite shoulders and eyes closed. Subjects were instructed to stand in the center of the force platform with the medial sides of the foot touching each other, following the protocols of Romberg test. The insoles were fixed in the same position on the force platform by adhesive tape for the insole condition. Balance was assessed under three test conditions: (1) without socks or insoles (Condition 1), (2) with socks but without insoles (Condition 2), and (3) with both socks and insoles (Condition 3). In each testing trial, subjects were instructed to stand as still as possible for 90 s. Each test condition was repeated three times consecutively for each subject. Between each condition, each subject was given a 10-min rest to eliminate possible effects of fatigue. The three test conditions were coded, and the testing order of the three different conditions was randomly generated for each subject.
Outcome measures
A 5.07/10-g Semmes-Weinstein monofilament (Connecticut Bioinstruments, Inc., Bronx, NY) was used to assess the effects of wearing thick socks on the ability of plantar surface of the foot to detect external forces, following the testing procedures as specified in Slater et al. 27 During the test, three sites at the plantar surface of foot were assessed including the hallux, the first and fifth metatarsal heads, with and without wearing the thick socks. At each site, the monofilament was pressed to the skin at 90° with a force of 10 g (0.1 N) to produce bowing for at least 1 s, which guaranteed the applied forces be kept consistent over the experiment. Two applications and a sham application were performed at each site. The sequence of the actual and sham applications was randomized. The subjects were instructed to respond “yes/no” after each application to indicate whether they could sense the touch of the monofilament with their eyes closed. Scores of each subject were marked from 0 to 3 based on the number of correct answers at each test site. 27 The higher scores of the monofilament represented the better detection of plantar pressure stimulations. All monofilament tests were performed by the same examiner.
A force platform (OR6; Advanced Mechanical Technology, Inc., Watertown, MA) sampling at 1000 Hz was used to measure the relative location of the COP signals to the coordinate origin of force platform. The real-time COP was recorded and used to calculate COP-based parameters. Based on the computed changes of locations of COP and their time of occurrence, the (1) mean velocity (mm/s), (2) root mean square distance (mm), (3) the 95% confidence circle area (mm2), (4) the 95% confidence ellipse area (mm2), (5) sway area (mm2), and (6) range of COP in anteroposterior (AP) and mediolateral (ML) directions (mm) were calculated using Microsoft Excel. 28
Statistical methods
Data analysis was performed using Statistical Package for Social Sciences (SPSS, version 21.0; IBM Corporation, Armonk, NY). Wilcoxon signed-rank test was used to compare the monofilament score with and without wearing the thick socks. One-way repeated-measures analysis of variance (ANOVA) with Bonferroni corrections was performed to study whether significant differences existed in all measured COP parameters among the three conditions. If significant differences were found in the ANOVA, post hoc pairwise comparisons were performed by conducting t-tests with Bonferroni corrections. The level of significance for post hoc tests was set at 0.05. During data analysis, the person who analyzed data did not know the content of each test condition as conditions were coded.
Results
In total, 14 elderly subjects (4 females and 10 males, aged 70.2 ± 3.4 years, height 162.8 ± 7.9 cm, and weight 63.6 ± 10.0 kg) participated in the study.
Table 1 shows that the average monofilament score decreases significantly from 2.8 to 1.1 after using the socks (p < 0.001). The percentage decreases of monofilament score at hallux, first metatarsal head, and fifth metatarsal head were 61.9% (p < 0.001), 63.4% (p < 0.001), and 61.1% (p < 0.001), respectively.
Comparison of monofilament score with and without using socks among older adults (n = 14).
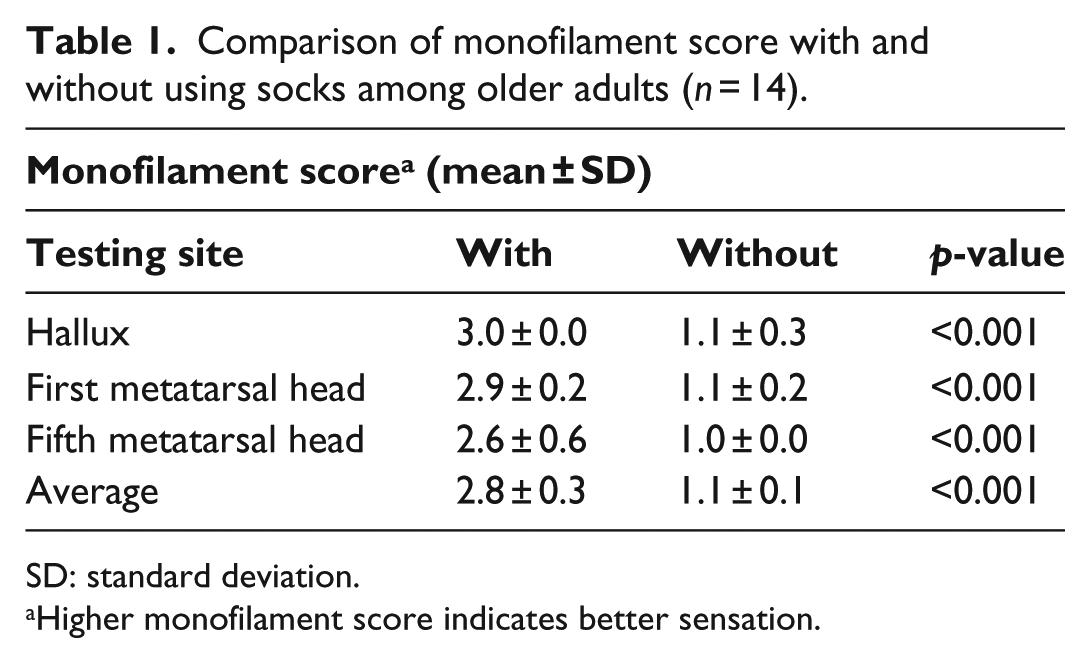
SD: standard deviation.
Higher monofilament score indicates better sensation.
A typical example of the COP trajectory in three experimental conditions in an elderly subject is shown in Figure 2. As shown in Figure 2(a) and (b), Condition 2 (with socks) induced a larger COP sway area than Condition 1 (without socks). The sway area of COP was then reduced in Condition 3 (using insoles, with socks; Figure 2(c)).
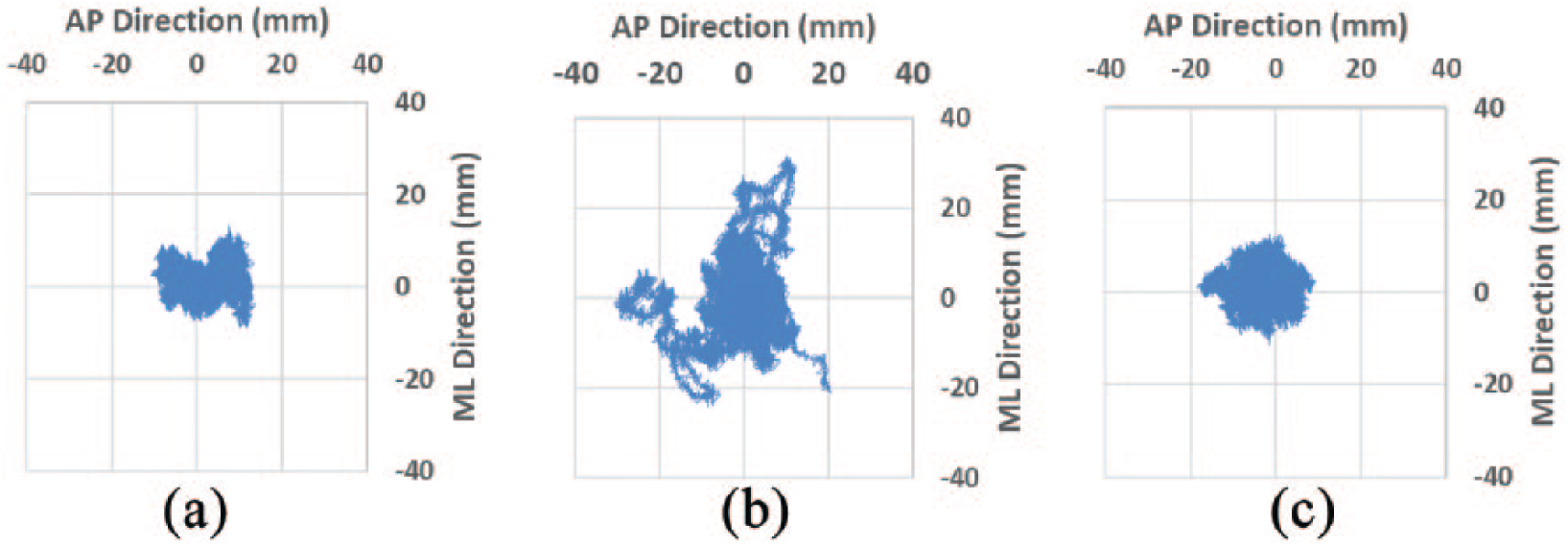
The COP trajectory in three different conditions in one elderly subject: (a) no socks or insoles, (b) with socks and no insoles, and (c) with socks and insoles.
Table 2 presents the quantitative data of COP parameters in three experimental conditions (n = 14). The results of one-way repeated-measures ANOVA revealed the existence of significant difference in COP parameters among three experimental conditions. All COP parameters increased significantly when wearing socks (Condition 2 vs Condition 1, p < 0.001) and then decreased significantly when wearing both socks and insoles (Condition 3 vs Condition 2, p < 0.001). No significant difference was found comparing Condition 3 with Condition 1 (Condition 3 vs Condition 1).
Comparison of COP parameters in three experimental conditions in older adults (n = 14).
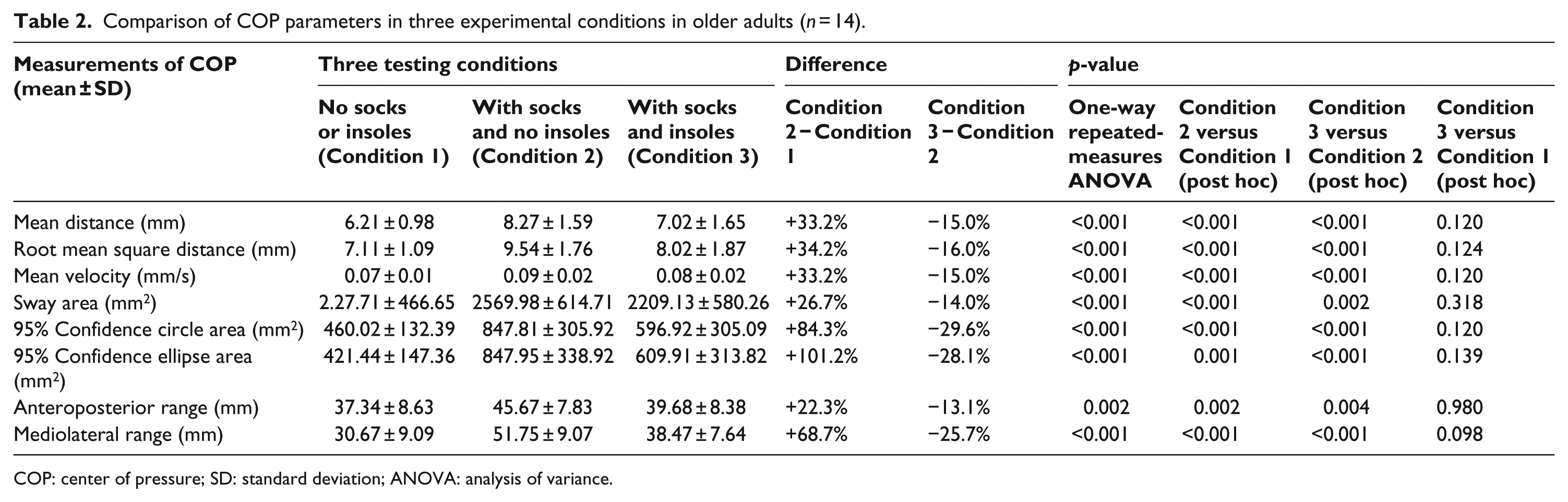
COP: center of pressure; SD: standard deviation; ANOVA: analysis of variance.
Discussion
Falls and fall-induced injuries are major public health problems, and continuous efforts have been made to improve older population and patients’ balance. Previous studies showed that orthopedic insoles increased the plantar pressure at relatively more sensitive areas over the metatarsal shafts 20 and the total contact area between the foot and the footwear.15,17,20 This study further suggested that such changes in contact mechanics could lead to improved static balance of people, whose balance had been affected by the use of thick socks.
The monofilament scores indicated that the thick socks lowered the ability of the foot to sense the external forces. The bowing of the monofilament during the test ensured that the magnitude of force (i.e. 10 g/0.1 N) applied was kept constant in both conditions of with and without wearing thick socks. 29 The lower monofilament scores with the use of thick socks suggested that the deformation of socks may distribute the forces and reduce the mechanical pressure acting against the foot, which restricted the plantar foot to detect less mechanical stimulations at the interface between foot and ground. The increase in postural sway while wearing thick socks further indicated and supported the importance of feedback from plantar tactile afferents in maintenance of balance, which is in accordance with previous studies that reported that falling risks could be increased by the use of socks.4,6 This raises concern, particularly for those who are prone to falls, about the use of thick socks which could impair balance. The findings were in accordance with previous studies which reported reduced static balance after an intervention of plantar desensitization, achieved by exposing subjects’ feet to ice for a few minutes 30 or injecting anesthetic solution 31 and asking the subjects to stand on a soft foam surface. 7 This study observed that socks alone could decrease postural stability. Clinicians need to be aware of this when making clinical decisions.
Following the increase in all COP parameters as the effect of wearing thick socks, all COP parameters then significantly reduced while using the orthopedic insoles with thick socks. In fact, no significant difference was found between the condition of barefoot and the condition of wearing both thick socks and insoles. This indicated that the negative balance effects of thick socks were dampened by the use of orthopedic insoles. A previous study revealed that nonfallers tended to have smaller COP range (16.5% and 14.2% smaller in ML and AP directions, respectively) and mean velocity (15.0% slower) compared with fallers 24 during standing. Coincidently, this study showed that the insoles reduced these parameters to similar percentages (reduction of approximately 15%) in older adults. Additionally, it is interesting to note that the degree of improvement in postural stability after using orthopedic insoles is similar to the condition of using higher cost vibrating insoles. 11 Future studies should investigate the potential effects of orthopedic insole in balance improvement under more diverse medical and physical conditions. The effects of orthopedic insoles on postural balance of people with impairments in plantar tactile sensation caused by aged degeneration, diabetic neuropathy, and rheumatoid arthritis 3 under various characteristics of shoe soles and supporting surfaces can be investigated. Future studies should also look into the potential relationships among plantar tactile sensation, plantar forces, and balance, which are largely unexplored.
This study did not involve a shoe condition. In addition to orthopedic insoles, some shoes with similar designs of heel cups and arch supports could have a similar balance-improving effect, which merits further investigation. Future studies could consider investigating the effect of socks and orthopedic insoles on postural balance when subjects are wearing standardized shoes.
Limitations of study
This study recruited healthy older adults only. Future study could investigate the effect of orthopedic insoles on balance in population with higher risk of falls. To eliminate the possible effects of shoes on postural balance, this study required all subjects to stand without any shoes on force plates when assessing the balance. Future studies should investigate the combined effects of orthopedic insoles and different types of shoes on balance, since different physical properties of shoes were found to have affected balance. 8
Conclusion
This study investigated the immediate effect of orthopedic insoles on postural balance of older adults, whose balance was adversely affected by the use of thick socks. After using the thick socks, the subjects’ static postural sway increased. This raises concern for people who are prone to falls about wearing thick socks. On using insoles, this study showed that the subjects then exhibited significantly less static postural sway. Insoles with an arch support, a metatarsal pad, and a heel cup were traditionally used to treat foot pain and deformity. This study indicated their potential of an additional benefit of balance improvement. This sheds new light on the application of a low-cost and practical solution for improving balance, which appears not to have caught much attention.
Footnotes
Author contribution
All authors contributed equally in the preparation of this manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by The Hong Kong Polytechnic University Research Studentship (grant number: RTNR), The Health and Medical Research Fund of Hong Kong SAR (grant number: HMRF11122231), and the Institute of Active Aging, The Hong Kong Polytechnic University.
