Abstract
Background:
Problem-based learning (where rather than feeding students the knowledge, they look for it themselves) has long been thought of as an ideal approach in teaching because it would encourage students to acquire knowledge from an undetermined medium of wrong and right answers. However, the effect of such approach in the learning experience of prosthetics and orthotics students has never been investigated.
Objectives:
This study explores the implications of integrating problem-based learning into teaching on the students’ learning experience via implementing a research-informed clinical practice module into the curriculum of last year prosthetics and orthotics undergraduate students at the University of Jordan (Amman, Jordan).
Study design:
Qualitative research pilot study.
Methods:
Grounded theory approach was used based on the data collected from interviewing a focus group of four students.
Results:
Students have identified a number of arguments from their experience in the research-informed clinical practice where, generally speaking, students described research-informed clinical practice as a very good method of education.
Conclusion:
Integrating problem-based learning into teaching has many positive implications. In particular, students pointed out that their learning experience and clinical practice have much improved after the research-informed clinical practice.
Clinical relevance
Findings from this investigation demonstrate that embedding problem-based learning into prosthetics and orthotics students’ curriculum has the potential to enhance students’ learning experience, particularly students’ evidence-based practice. This may lead to graduates who are more knowledgeable and thus who can offer the optimal patient care (i.e. clinical practice).
Background
Problem-based learning (PBL) is a relatively new approach in teaching (i.e. since the 1970s) that focuses on involving the students in knowledge enquiry. PBL differs from the typically used problem-solving learning approach, in that it encourages students to acquire knowledge from an undetermined medium of wrong and right answers rather than from a predetermined medium of only right answers. In this way, a student decides on the information they wish to acquire and how it is relevant to their area of study. 1
Many researchers have identified several benefits of implementing PBL in clinical teaching such as improving learners’ skills in (1) acquiring knowledge, (2) interpolating information and (3) communicating with team members.2 –4 However, in their meta-analysis, Albanese and Mitchell 5 documented that weaknesses can be found in PBL and that when teachers want to implement PBL, they must take into account the cost, the cognitive variations between students and the time at which students are directed to PBL as part of their training. Taking into consideration the benefits and weaknesses of PBL, Barrows 6 has suggested that a successful PBL should lead to improving students’ skills in self-learning, understanding and clinical-reasoning as well as encouraging students to learn more.
In recent years, PBL has been a subject of interest as a teaching method, 7 and despite being studied in different fields, the effectiveness of PBL for prosthetics and orthotics (P&O) students has never been identified. Therefore, and driven by their belief that PBL has a strong impact in the process of teaching, the P&O staff at the University of Jordan (Amman-Jordan) has implemented an imperative change in the way the clinical practice module is executed for P&O undergraduate students within semester two of their last year. The module extended over a four-month period (840 practical hours). Students were not only taught how to make a prosthesis or an orthosis, they were also directed towards developing their evidence-based practice. It was stipulated that such a change would assist students’ understanding of the P&O principles as well as developing their learning experience and may lead to research output.
Methods
Module
The developed module was termed ‘research-informed clinical practice’ (RICP) (in this term, research means the act of searching for knowledge from the literature) and was undertaken in the clinic. It involved random assignment of four patients to each student (two requiring orthotic and two requiring prosthetic treatment). Based on the literature and an evidence-based experimentation, students were responsible for assessment of the patient’s condition, identifying an intervention strategy, manufacturing, checking and finally delivering the actual treatment (prosthesis/orthosis) to the patient. These responsibilities were performed under the supervision and guidance of the supervisors (certified P&O lecturers) who provided direct supervision whilst dealing with the patient and manufacturing the prosthesis/orthosis, and an indirect supervision (via e-mails) while searching the literature. For each of the four assigned patients, the student had to submit a portfolio and case study after study and undertake an oral examination once the treatment was delivered.
Before the module was started, students undertook an induction week to familiarise them with the concept of the RICP and to train them on literature search using different databases (e.g. PubMed). By the completion of the module, feedback on the RICP was collected from a focus group.
Subjects
In order to examine students’ holistic experience of RICP, focus group interviews with a randomly selected sample were conducted. The sample represented half of the fourth-year cohort (n = 7). In particular, after assigning numbers to each of the 14 fourth-year students, seven numbers were randomly selected and names (recruited students) were then revealed.
The interviews aimed at obtaining the students’ general opinion of RICP and whether RICP was advantageous over the traditional teaching method (i.e. problem-solving learning). In the interviews, the students were asked five questions listed in Table 1. These questions were adopted from an earlier study conducted in an attempt to address the same objectives of this study but in the field of radiography. 8
Student interview questions.

RICP: research-informed clinical practice.
Ethics
Ethical approval (reference number: 1/2013–2014) for conduction of this study was granted from the University of Jordan scientific research ethical committee. Once granted, and for the purposes of this study, recruited students were approached by the principal investigator (i.e. module coordinator). All recruited students were orally informed about the aim of the study and the procedure of the interview. In addition, they were assured of confidentiality and anonymity during and after the interviews. Those who agreed to take part in the study were asked to sign a written consent form. Of the seven recruited students, three did not attend the interview for personal reasons.
Data collection
The interviews took the form of an informal face-to-face conversation in which questions were directed to each student in the same order presented in Table 1. Students answered the questions without interruption. Only one student was interviewed at a time.
In order to keep the conversation smooth, the interviews were audio-recorded. To ensure anonymity, each student in the focus group was given a number that was used to label his or her interview record. The interview was estimated to take about 30 min to be completed.
Data analysis
The recordings from the focus group members were transcribed verbatim in a manner that reproduces the interviews. 9 Grounded theory was then used to analyse the data.10 –12 Unlike other research methods, grounded theory is used to discover a theory rather than to verify or test an existing theory. Particularly, after data collection, the data are labelled in categories and interrelationships between these categories are identified from which a theory is developed.
Initially, open coding was used to categorise and subcategorise the data. In order to create a discriminate coding and as suggested by Strauss and Corbin, 13 questions were made precise and specific. Five categories were identified, including students’ outcome from the RICP (i.e. gained knowledge), students’ perspective about integrating RICP in teaching, students’ evidence-based practice, students’ enthusiasm to conduct research and changes in students’ clinical practice. Three subcategories were also identified including constructive student’s experience, devastating student experience and improved students’ research practice.
Second, axial coding was used to (1) compare the transcript with the five categories, (2) link categories and subcategories, (3) specify the subcategories’ properties and dimensions and (4) identifying difference in student’s experience when integrating RICP into teaching. Finally, selective coding was used to recognise the ‘story’ by identifying the main category, relating it to the other categories and validating relationships after gaps in categories had been filled (taking into account any significant variation within the categories).
Results
Table 2 shows students’ quotes classified based on the five categories identified by the open coding. In general, all students of the focus group had a positive impression of the RICP; they described it as a very good or effective method of education: It was the best learning experience I have ever had.
Students’ quotations categorised based on five categories discovered in the open coding.
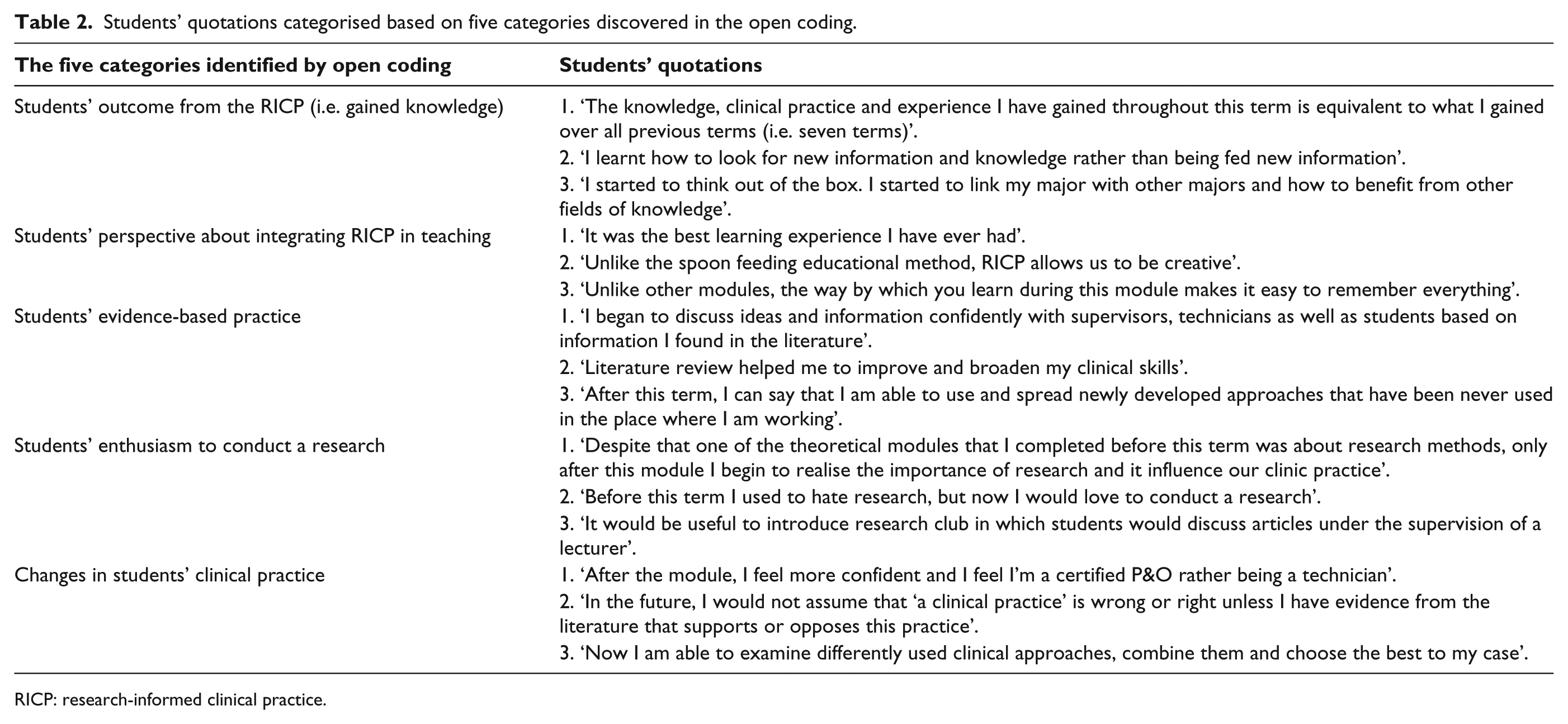
RICP: research-informed clinical practice.
Additionally, students agreed that RICP enhanced their clinical experience as it was organised to allow working with a relatively large number of patients (students used to deal with no more than one patient in each of the previous terms, whereby in this term they dealt with four patients). In fact, students spent all working hours (i.e. 8 a.m. till 2 p.m.) over all working days (i.e. Sunday–Thursday) in P&O clinics in which they had a direct contact with patients. Students were instructed to complete their case reports after 2 p.m. at home or at the university computer laboratories.
The knowledge, clinical practice and experience I have gained throughout this term is equivalent to what I gained over all previous terms (i.e. seven terms).
RICP was also thought to encourage student’s creativity: Unlike the spoon feeding educational method, RICP allows us to be creative.
Students explained this by the fact that they had to study, search and learn by themselves (self-learning) about their patients’ medical condition to find the most appropriate prosthetic or orthotic prescription (i.e. evidence-based) rather than being instructed by a supervisor. Self-learning was made achievable by providing students with an intensive training on literature search strategy and how to use different databases to find information relevant to the case(s) they were assigned to deal with. Students seemed to value this self-learning approach that was inherently implemented in the RICP; students believed that it helped them to effectively absorb knowledge: Unlike other modules, the way by which you learn during this module makes it easy to remember everything.
Students were prompted to criticise the medical prescriptions prescribed by the rehabilitation or orthopaedic consultants and to propose evidence-based alternatives if possible. This seemed to improve the self-image of some students: After the module, I feel more confident and I feel I’m a certified P&O rather being a technician.
Students mentioned several aspects that helped them to learn during RICP. Most of the students agreed on two main aspects: the induction week and the supervision. In regard to the induction week, as discussed before, this aimed at familiarising the students with the module requirements and to provide them with basic research skills (i.e. literature search, critical appraisal and how research is conducted) required to complete this module successfully.
The focus group suggested that supervision was particularly important in directing the learning process. Supervisors mainly provided the students with feedback on their case reports and directly instructed them in clinics. In several instances, however, supervisors also directed students towards the relevant references and articles and explained unfamiliar concepts/principle of therapeutic or measurement techniques (such as motion capture systems). This was conducted through regular discussion meetings or informally whenever the student sought for help. The nature of the discussion meetings seemed to positively influence the students’ self-confidence and to break the sense of hierarchy between lecturers and students: I began to discuss ideas and information confidently with supervisors, technicians as well as students based on information I found in the literature.
Nonetheless, it has to be mentioned that not all supervisors appeared to provide efficient feedback to the student’s reports or enough number or duration for discussion meetings. Students generally sought help from other supervisors (not assigned to him or her) whenever they received an unsatisfactory feedback.
Whenever I felt that the feedback was not good enough, I sought the help from another supervisor who is not assigned to me.
In clinical practice (i.e. during clinical work), the majority of the students found it problematic to have feedback from different supervisors on one case. In particular, in some occasions, they had conflicting feedback from different supervisors: Having different supervisors in the practical part was a source of confusion as I got sometimes contradicting feedback.
Discussion
In addition to quality and manner (in clinical practices) of supervisor’s feedback, students also found RICP time-consuming and very demanding. This might be mainly due to the nature of the orthotics and prosthetics programme that has theoretical and clinical requirements. Students additionally faced some difficulty in accessing the literature due to limited number of databases accessible from the University of Jordan.
Despite teaching in an Arabic country, English language is used to run the entire P&O programme. However, students are not familiar with academic writing in English, nor do they read research articles in English. Therefore, students need continuous and regular feedback from supervisors. After the RICP, students mutually agreed that it helped them in improving their academic English writing skills. Also, RICP built a belief that self-learning is not impossible: I learnt how to look for new information and knowledge rather than being fed new information.
Clinically, students appeared to benefit from the literature in which novel techniques and/or cutting-edge technology are introduced. Probably, students also felt more certain about the outcome whenever they read literature that is related to the case(s).
Literature review helped me to improve and broaden my clinical skills.
Students, moreover, begun to critically assess any clinical practice even if it had been widely accepted and used by practitioners: In the future, I would not assume that ‘a clinical practice’ is wrong or right unless I have evidence from the literature that supports or opposes this practice. Now I am able to examine differently used clinical approaches, combine them and choose the best to my case.
Although the students in the focus group value the advice of experienced practitioners, they collectively revealed their tendency (as a direct result of RICP) to review the literature in order to learn how to deal with unfamiliar cases. They highlighted that they will not be afraid to introduce to others any newly empirically supported clinical practice that they find in the literature or to suggest any improvement to currently used practices.
After this term, I can say that I am able to use and spread newly developed approaches that have been never used in the place where I am working.
Finally, although all students had completed a module in research methods before RICP and had a vague idea about it, only a few valued the role of research in scientific development.
However, following RICP, and perhaps because students read articles related to actual cases that they dealt with, students showed a better understanding of research methods and felt the importance of research. Moreover, students felt very enthusiastic about conducting more research following the RICP.
Despite that one of the theoretical modules that I completed before this term was about research methods, only after this module I begin to realise the importance of research and its influence on clinical practice.
Interestingly, some of the students became interested in research and expressed their desire to conduct research: Before this term I used to hate research, but now I would love to conduct research.
Notably, a student suggested establishing a research club at the University of Jordan aiming to change the student’s prospective towards research: It would be useful to introduce research club in which students would discuss articles under the supervision of a lecturer.
Perhaps due to the nature of a P&O programme which is derived from different fields of knowledge, students seemed to understand the importance of team work in research and the holistic nature of research in which it is possible to borrow concepts and paradigms from other fields of knowledge.
I started to think out of the box. I started to link my major with other majors and how to benefit from other fields of knowledge.
In summary, RICP aimed at enhancing students’ self-learning skills and encouraging them to build a nexus between knowledge and their clinical practice. Evidence from this investigation shows that PBL was more successful than traditional approaches in terms of students’ satisfaction and evidence-based clinical practice. In addition, students have identified an improvement in their academic performance through and following the RICP which was reflected on their marks. This suggest that implementing PBL into the curriculum of P&O undergraduates is worthwhile particularly because previously identified weaknesses in PBL from the literature 5 (e.g. high cost) were not faced in this investigation.
Nevertheless, further investigations in this area of research are needed. In particular, studies on larger sample sizes are needed to make generalisation of obtained results possible. Also, students were introduced to RICP just at the beginning of the module, whereby introducing the student to RICP in a preceding term may have been more beneficial in many aspects (i.e. better literature search skills and understanding of knowledge). Finally, in this investigation, the RICP covered both prosthesis and orthosis aspects, whereby a RICP that focuses on orthosis and another on prosthesis (executed on two different terms) may be more useful for students.
Conclusion
The aim of this study was to explore the value of integrating PBL into the teaching process of the P&O undergraduate students. Evidence from the focus group shows the usefulness of such integration. In particular, students demonstrated that the RICP helped them in understanding the concepts behind their clinical practice and that their way of dealing with patients in terms of diagnosing, prescription and manufacturing has positively improved. Moreover, students expressed increased interest in incorporating evidence into clinical decisions and using the literature to support their work as an P&O clinician. Moreover, students’ ambition to pursue research has been boosted in that they chose to undertake research.
Information gained from this study will help informing and developing the content of the P&O undergraduate curriculum in a way that further integrates PBL into teaching. Also, this information will be used for further research which recruits larger sample sizes.
Footnotes
Author contribution
All authors contributed equally in the preparation of this manuscript.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
