Abstract
Background:
The craniofacial implants are used for retaining the prostheses although these are costly and often require complex laboratory procedures. The aim of this case report is to describe a case of successful rehabilitation of partial ear loss with long-term soft liner and mechanically retained by custom-made heat-cured acrylic attachment.
Case Description and Methods:
A female patient underwent a scalp avulsion injury and lost major portion of her hair and upper part of the left ear till the antitragus. A partial auricular prosthesis was fabricated, and mechanical retention was achieved through custom-made heat-cured acrylic attachment engaged in anatomic undercuts of remained ear.
Findings and Outcomes:
Permanent soft liner provided a life-like appearance and consistency to the prosthetic ear and bonded to custom-made heat-cured acrylic attachment through chemical cross-linking.
Conclusion:
Patient accepted the prosthesis satisfactorily without any social and psychological embracement. This technique simplified the clinical and laboratory procedures and reduced the cost of the prosthesis.
Clinical relevance
The use of permanent soft liner is esthetically acceptable and can cross-link with acrylic resin to allow the bonding between the custom-made acrylic retentive element and the prosthesis.
Background
Extraoral prosthesis is difficult not only in terms of esthetic construction but also to retain the prostheses. The fabrication of ear prosthesis is considered to be one of the more difficult maxillofacial reconstructions due to severe undercuts and convolutions present on the ear’s surface. 1 Craniofacial implants intended for retention of auricular prosthesis provide very good support and retention to the prosthesis2–4 and improve not only patient’s appearance but also quality of life. Although it is a costly treatment option, to achieve a successful result, proper planning is of utmost importance regarding total number of implants, their position and orientation, and the attachment of ear prosthesis with the implant retentive structures. This includes complex laboratory procedures, such as fabrication of an accurate casting, fitting of the cast bar, and the use of clips to attach the prosthesis with the bar.
In this case report, we have described a case of poor lady in whom successful rehabilitation of partial ear loss was done with acrylic-based long-term soft liner and mechanical retention was achieved through custom-made heat-cured acrylic attachment. The advantage of using the acrylic-based long-term soft liner with custom-made heat-cured acrylic attachment was that it not only provided a life-like appearance to the prosthesis but also bonded chemically to the heat-cured acrylic attachment through cross-linking reaction.
Case description and methods
A 48-year-old female patient was referred to the department for fabrication of an auricular prosthesis. The patient had a scalp avulsion injury while scything 2 years back. She lost major portion of her hair and some part of the left ear in that injury. Upper part of the ear till the antitragus was lost, and the lower part was intact (Figure 1). Patient was a poor village lady and could not afford implants. After carefully examining the site, we found some scope for anatomic retention from the remaining ear present, and we decided that an auricular prosthesis retained by custom-made acrylic attachment and adhesives would be made.
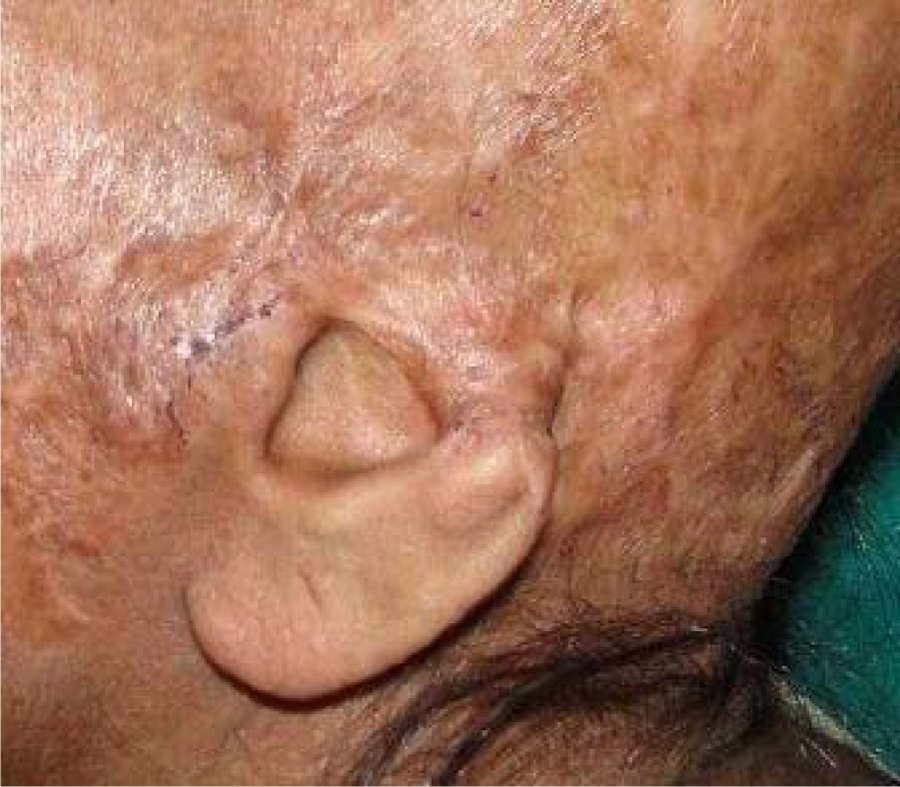
Patient with partial ear loss.
The patient was made to lie on the dental chair in supine position and was turned to the right side so that the left side of face was facing upward. Patient’s inner ear was blocked out by using lubricated cotton, and facial hairs were protected by a light application of petroleum jelly (Vaseline; Hindustan Unilever Ltd, Mumbai, India).The defect site was boxed by a ring of modeling wax (Metrodent, Mumbai, India) to control the flow of the impression material. An irreversible hydrocolloid impression material (Zelgan 2002; Dentsply India, Gurgaon, India) was mixed with 1.25 times the normal amount of water to adjust its flow properties. The impression material was poured in a smooth layer over the area and was covered by gauze pieces embedded in it to provide retention for the rigid plaster backing required for tear-free removal of the impression. Mechanically spatulated type II dental plaster (Dentex; Prevest Denpro Ltd, Jammu, India) was spread over the gauze, and its setting was verified by tapping sound. After removal of the impression, it was inspected for any defects and was poured with vacuum-spatulated type IV dental stone (Kalabhai; Karsor Pvt. Ltd, Mumbai, India) in two stages to avoid distortion by weight of the stone, making at least a 1-cm-thick base. On the resultant stone cast, markings were made superiorly, inferiorly, anteriorly, and posteriorly for orientation.
A custom-made attachment was fabricated on the cast with autopolymerizing acrylic resin (Trevalon; Dentsply India, Gurgaon, India) and was tried on the patient’s face for proper extensions and fit (Figure 2). This cold-cured attachment was extended anteriorly into the external acoustic meatus and posteriorly extended to encircle the lobe with its two limbs. The outer limb was extended to the cymba conchae, and the inner limb was extended to the back of the remaining lobe.
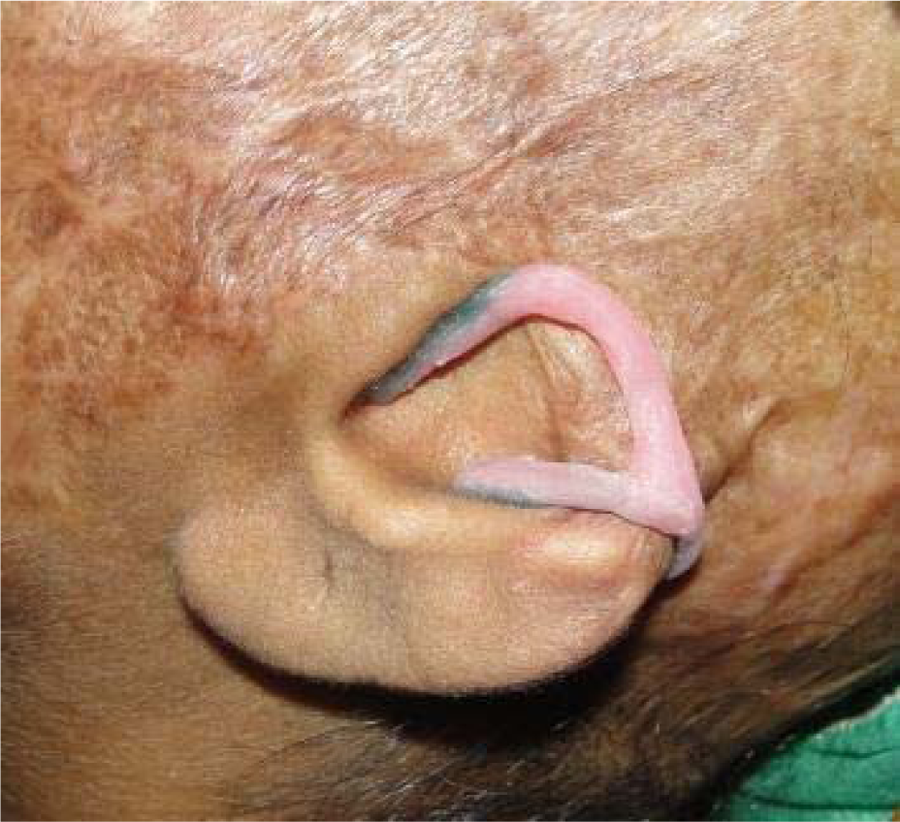
Try-in of custom-made acrylic resin retentive attachment.
An ear form was selected by choosing an individual with a similarly proportioned ear, and impression was made in the similar manner as described earlier. Molten modeling wax was poured into the ear mold, and after solidification, the solidified wax form was retrieved and was checked for contour and size. The tissue surface of the wax form was softened, and with the help of the orientation markings on the working cast, it was seated on the defect area. Minor modifications were done to adapt it properly onto the remaining ear on the cast and match it with the contralateral ear. This wax form was attached to the previously formed custom-made cold-cured attachment, and trial was done on the patient’s face to check for fit of the prosthesis, horizontal alignment with normal ear, its projection in relation to the side of the head, and marginal integrity during simple jaw movements from all aspects (Figure 3).
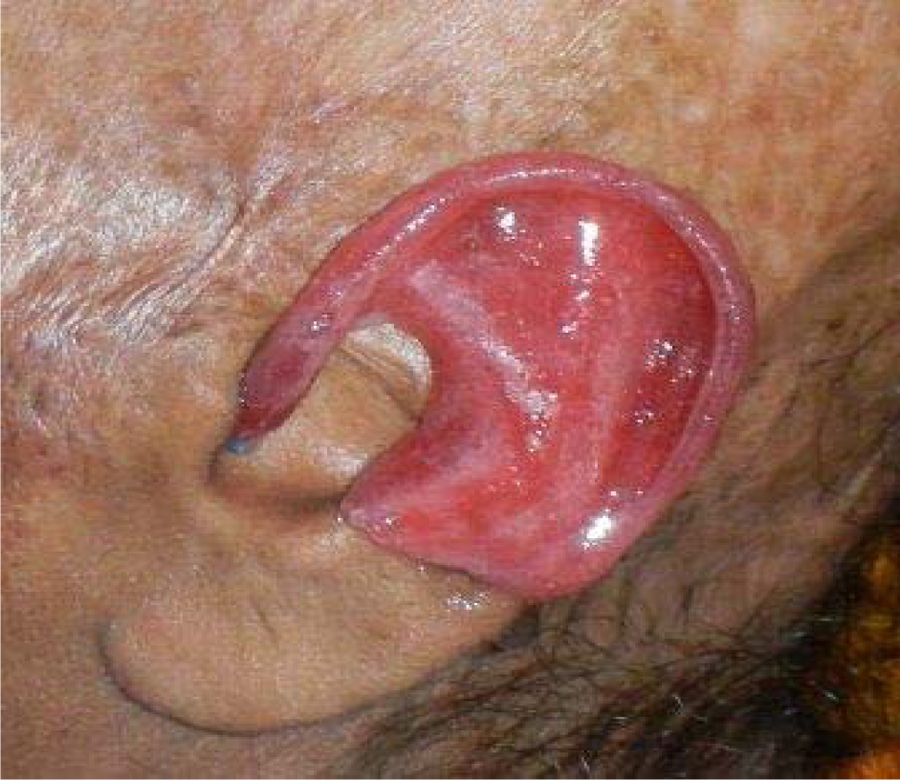
Wax pattern try-in of partial ear prosthesis.
After obtaining satisfactory results, the wax pattern was invested to create a mold in two parts to produce life-like characterization. Following dewaxing, the area of the custom-made attachment on the mold cavity was filled with heat-cured acrylic resin (Trevalon), and the area of the remaining ear lobe was filled with a freshly mixed previously matched base color mixture of acrylic-based long-term soft liner (PermaSoft soft denture liner; Dentsply India, Gurgaon, India) using acrylic pigments to provide skin color and opacity to the mixture. The excess material was expressed using light pressure and was processed and finished following manufacturer’s instructions. Extrinsic coloration was done after separating from mold in required areas to match the color of the prosthesis with the skin color as closely as possible, and the patient was trained to correctly place the ear in proper position (Figure 4). For additional retention, patient was advised to use adhesive (Pros-Aide Adhesive, Northvale, NJ, USA). Instructions were given on prosthesis hygiene, maintenance, and recalled checkups. The patient was also advised to camouflage the prosthesis by using hair wig and to wear light earrings to divert attention.
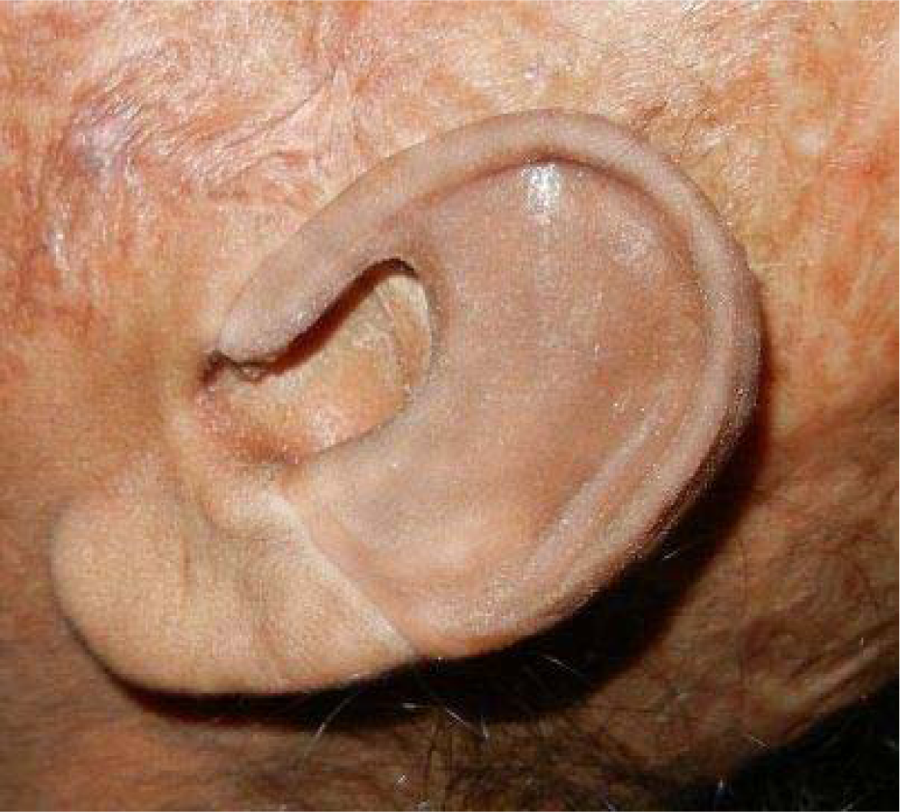
Partial auricular prosthesis retained with heat-cured acrylic attachment.
Findings and outcomes
Permanent soft liner provided a life-like appearance and consistency to the prosthetic ear and bonded to custom-made heat-cured acrylic attachment through chemical cross-linking. Apart from the visual and mental reimbursement, auricular prosthesis also helped to straight the sound waves into the auditory canal and to maintain a conducive environment for the inner ear membranes, which can improve hearing significantly. The patient accepted the prosthesis satisfactorily and is using it comfortably since the past 6 months without any adverse event as evident in the recall appointment schedule.
Discussion
Loss of any part of human body is very traumatic to the patient. It affects the patient not only physically but also mentally. The patient’s overall personality, personal and social life, and confidence level are badly affected due to the loss.5,6 An ideal requirement for extraoral prosthetic reconstruction is that the prosthesis should not look like prosthesis, so that the casual observer does not find any significant difference in the area of rehabilitation that would draw his or her attention to differentiate the prosthetic reconstruction from the natural part.
Auricular prosthetic reconstruction has several advantages over the surgical reconstruction as being less expensive, ease of fabrication, allowing periodic evaluation and cleaning of the surgical site, and providing an alternative in patients in whom surgical reconstruction is not possible. 7 However, there are certain limitations of prosthetic reconstruction as well, such as difficulty to hide the skin–prosthesis margin, difficulty in matching skin color that keeps changing all the time, need for regular repair and/or replacement, and fear of removal of the prosthesis during rigorous activity.
The ideal material for auricular prosthesis should have the properties of biocompatibility, flexibility, lightness, low thermal conductivity, durability, moldability, patient comfort, ease of cleansing, and physical and chemical inertness.8,9 The currently available materials for maxillofacial prosthesis include acrylic resins, polyurethane elastomers, and silicone elastomers. 10 The extraoral facial prosthesis can be fabricated by a combination of silicone elastomer and a rigid polymeric material, for example, acrylic, urethane dimethacrylate (UDMA), vacuum-formed cellulose acetate, or glass fiber–reinforced composite (FRC). 11 The average clinical life of a maxillofacial prosthesis is about 6–12 months; therefore, it needs to be refabricated before this lifetime. 12 According to the manufacturers’ claim, the shelf life of the acrylic-based long-term soft liner (PermaSoft soft denture liner) is 2 years 13 depending upon the handling characteristics of the prosthesis. Among the various materials available for maxillofacial prosthesis, acrylic resin being a rigid material is more durable, and its margins can be thinned out easily but not esthetically as pleasing as a flexible material like silicone. Silicone prostheses offer a more natural looking and cosmetically elegant means to camouflage large auricular defects, 8 but the disadvantages of silicone include its lack of bonding with the acrylic resin or metal and lack of tear strength in thin sections. In this case, we used a custom-made acrylic attachment for retention of the prosthesis and resin-based long-term soft liner material for the ear prosthesis reconstruction. Due to similar chemical compositions, the acrylic resin–based liners made a chemical bond with the heat-cured poly(methyl methacrylate) (PMMA) polymer. 14 The acrylic-based soft liner not only allowed the bonding between the custom-made attachment and the prosthesis through chemical cross-linking but also gave a life-like appearance and consistency to the prosthetic ear. During the processing of the ear, we used only a two-piece mold instead of a three-piece gypsum mold that is recommended for fabrication for ear prosthesis to prevent tearing of silicone material in thin marginal portions during retrieval. 1
Several skin adhesives are compatible with the acrylic resin, adhere well under the moist conditions, and are simple to use. The use of adhesive improved the overall retention of the prosthesis adding to the retention obtained by the custom-made retentive attachment.
Conclusion
A technique of fabricating a partial auricular prosthesis using long-term soft liner and retaining by the combined use of custom-made heat-cured acrylic attachment and chemical adhesive was described. This technique simplified the clinical and laboratory procedures and reduced the cost of the prosthesis.
Footnotes
Conflict of interest
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
