Abstract
Introduction:
University students are at a high risk for mental health difficulties. Occupational performance coaching is an action-oriented and strengths-based approach that can help clients set and accomplish personally valued goals. We carried out a pilot project to evaluate a tele-rehabilitation occupational performance coaching service for university students within an occupational therapy fieldwork placement.
Method:
A pretest post-test design was used. Severity of symptoms of depression, anxiety and stress and goal achievement were measured before and after the intervention and semi-structured interviews were carried out with student clients and student therapists. Development of student therapist competencies were noted.
Results:
Thirty-five student clients enrolled in occupational performance coaching and participated in 1–6 sessions. They identified academic, health, social and vocational goals. Through occupational performance coaching, clients made important progress on their goals. Following occupational performance coaching, clients demonstrated statistically significant improvement in anxiety and depression. The occupational therapy students attained competencies comparable in number and level to those achieved in more traditional placements.
Conclusion:
Occupational performance coaching is a potentially valuable addition to student mental health services. Such a service can be provided by supervised fieldwork students.
Introduction
Many students experience multiple stressors and feel overwhelmed with managing daily occupations. University students are at high risk for mental health problems. Most of them are in an age group (late teens to late twenties) when many psychological disorders appear (Solmi et al., 2022). Furthermore, some students are separated from their families, facing adulthood without being ready, and subject to the stresses of academic life (Pedrelli et al., 2015). The COVID-19 pandemic and resultant public health restrictions and school closures to in-person learning, have further impacted university students’ mental health. Research indicates that university students have experienced problems including higher levels of reported depression and social isolation; stress, anxiety, and sleep disruption during the pandemic (Chaturvedi et al., 2021; Prowse et al., 2021).
In 2020, the President’s Advisory Committee on Mental Health and Wellness at the University of Ottawa (Canada) developed a series of recommendations in response to the growing number of students reporting mental health problems including stress, contemplation of suicide, and difficulties in academic performance. Recommendations included the development of a stepped care model to facilitate access to services, and support of students’ involvement in mental health initiatives on campus (University of Ottawa, 2020). To contribute to mental health services and provide mental health fieldwork experiences for occupational therapy (OT) students that could be carried out on-line, the occupational therapy program developed an occupational performance coaching (OPC) (Graham et al., 2021) telehealth service. The primary aim of this pilot study was to determine whether an OPC service led by OT students, helped their clients (other university students) meet academic and personal goals and decrease symptoms of depression, anxiety, and stress.
Literature review
The prevalence of mental health problems among university students is a global concern (Bayram and Bilgel, 2008). Recent surveys demonstrate that over half of all students have experienced anxiety or depression severe enough to affect their daily functioning (American College Health Association, 2019). The WHO’s international college student project examined the prevalence of six common mental disorders among 13,984 first year college students across eight high-income countries (Auerbach et al., 2018). Findings revealed a 21% lifetime prevalence of major depression and a 35% lifetime prevalence of at least one mental health disorder. Generalized anxiety disorder was the second most common mental health problem reported (18.6%), followed by alcohol use disorder (6.8%) and substance use (5.1%). Other studies have found a similar high prevalence of depression, anxiety, and substance use disorders among college students (De Girolamo et al., 2012).
Beiter et al. (2015) examined the correlations of depression, anxiety, and stress among a sample of undergraduate university students and reported main life concerns by participants. Notable findings were that many different areas of emotional functioning and life roles were affected, including: “academic performance, pressure to succeed, post-graduation plans, financial concerns, quality of sleep, relationship with friends, relationship with family, overall health, body image, and self-esteem” (p. 93). The COVID-19 pandemic has further affected mental health among young adults, particularly university students, with depression, anxiety, and stress, attributing to restrictions owing to the pandemic including physical distancing and confinement measures (Galea et al., 2020; Husky et al., 2020). Lifestyle disruption including financial and/or job loss, social isolation, and change in relationships, sleep patterns, and fitness routines, have also been noted in the literature (Chaturvedi et al., 2021; Prowse et al., 2021). Koelen et al. (2021) explored students at risk for mental health difficulties prior to the pandemic and during the pandemic and identified protective factors and risk factors for various problems including depression, anxiety, loneliness, and sleep disruption. An interaction was found among protective factors such as emotional support, active coping, social contact with family and friends, and stress which influenced students who reported mental health problems. In particular, stress related to the pandemic “was associated with larger increases in depression-anxiety, which was in turn associated with larger increases in other mental health symptoms including stress and insomnia” (p. 4).
Health and well-being are influenced by the ability to participate in daily life activities and social roles (Law et al., 1998). Research on coping highlights the importance of active coping mechanisms (Taylor and Stanton, 2007). However, many university students feel overwhelmed and could benefit from support as they begin to identify, organize, and address the many tasks associated with being a student. Others need support in developing regular outlets for re-energizing, such as a hobby or exercise routine, or in gaining control over valued activities in the context of the pandemic restrictions. A multipronged approach to improving access to services that promote student mental health and performance has been recommended (MacPhee et al., 2021).
OPC is an evidence-based OT intervention that helps people engage or re-engage in personally valued activities. Its components have been carefully developed using self-determination theory, adult learning theory, and solution-focused therapy. These theories inform the key components of OPC: emotional support, client-centered goal setting, guided strategy development to achieve goals, and individualized education (Graham et al, 2021; Kessler et al., 2018).
Using a strength-based, autonomy-supporting approach, the coach provides emotional support and structure as clients identify and work towards personally relevant goals. From a solution-focused rather than a problem-focused orientation, clients are guided to identify solutions to challenges and to transfer successful strategies to performance of other meaningful activities. This guided approach of OPC contrasts with a directed approach of many other strategies (e.g., psychoeducational). Rather than making recommendations or teaching a set of skills, the coach uses reflective questioning to enable the client to explore, select and experiment with strategies to address their unique goals (Graham et al., 2021; Kessler et al., 2018). Clients are thereby supported to develop the knowledge, skills, and self-efficacy required to take on future participation challenges.
We believed that OPC, provided to university students by student occupational therapists, could help them develop personalized, effective ways to deal with the many occupational challenges that they face in their everyday lives. Therefore, the main purpose of this study was to investigate the application of OPC with university students. We hypothesized that OPC would also decrease symptoms related to depression, anxiety, and stress, as students were encouraged by successes in dealing with their occupational challenges. Finally, we believed that providing OPC would be a rich practical learning experience for student occupational therapists, allowing them to develop valuable skills and competencies.
Method
The OPC service
An OPC fieldwork placement was offered to six OT students during their fourth fieldwork experience in the second year of their entry to practice master’s program. The OPC service ran from mid-February to mid-April 2021. This placement fulfilled accreditation requirements for at least one fieldwork experience in mental health.
Initial group training was provided to the OT students by three OT professors, a university mental health counsellor, and a manager from the university international office. The curriculum included theoretical foundations in OPC, mental health, suicide prevention, private practice; implementation of OPC through role plays and case studies; and the delivery of virtual care or telerehabilitation. Ongoing student learning was supported through bi-weekly team huddles involving the students and supervisor, weekly community of practice meetings to foster clinical reasoning through review of clients and evidence-informed practice, and mentoring meetings in which students met individually with the supervisor on a weekly basis or more often as needed. Consistent with requirements of the College of Occupational Therapists of Ontario, student therapists were supervised by a registered occupational therapist who was responsible for completing the mid-term and final fieldwork evaluations.
Promotion of the OPC service to develop a client referral base included presentations to the university Counselling Services and the International Office staff and emailing directors of a number of university programs. Clients were assigned to each student occupational therapist as referrals for the OPC service were received. The OPC service was offered in English or French based on clients’ preferred language. Clients were seen weekly by the student occupational therapist through telerehabilitation for 45- to 60-minute sessions. Following each session, the student occupational therapist provided summaries to clients about their OPC goals and action plans. In addition to providing OPC to student clients, the student occupational therapists developed formats for keeping client records and developed materials and presentations to describe the OPC service to students and stakeholders such as Counselling Services and the International Office.
Consistent with procedures for all fieldwork in the University of Ottawa program, students were evaluated using the Monitoring Tool for the Development of Clinical Competencies (M.O.T. DECC) (Beaudoin et al., 2007). This tool consists of 27 essential competencies and criteria to determine whether students have obtained the required skill level expected at the end of each of the required five fieldwork placements in the OT program.
Evaluation of the OPC service
We used a pre- /post-test design to measure the impact of the program on student client occupational performance and satisfaction, and mental health. We used a qualitative descriptive method to explore the experience of the student clients and student therapist.
Data collection
Three sources of data were used to determine the outcomes of OPC on the student clients. First, to determine changes in student clients’ abilities to manage occupational challenges, the Canadian Occupational Performance Measure (COPM) was used (Law et al., 2014). The COPM was developed to determine subjective change in occupational performance in client-identified goals. Each client completed the COPM with their student occupational therapist during the first or second OPC session, and then again during the last session. A mean change of 2 is considered clinically significant (Law et al., 2014). The number of sessions attended was noted for each student client.
Second, to determine changes in mental health, the Depression, Anxiety and Stress Scale (DASS-21) was used (Lovibond and Lovibond, 1995). The short version consists of 3 self-report scales comprising seven items per scale measuring depression, anxiety, and stress. As we wished to focus on student clients’ strengths and occupational goals, we invited students to complete the DASS-21 outside of the OPC sessions before and after receiving OPC through accessing a survey link if they wished to do so. Student clients were asked to respond to each subscale from 0 (did not apply to me at all) to 3 (applied to me very much or most of the time). Sum of scores per scale were multiplied by a factor of 2 to achieve the full-scale score.
Finally, to gain further insight into how the service had been helpful to students, semi-structured interviews with eight student clients, sampling purposively to allow for variation in gender and undergraduate and graduate status were planned. These interviews were carried out by a research assistant.
Two sources of data were used to determine the impact of providing the OPC service on the student therapists. First, we evaluated student learning outcomes using their end of placement scores on the M.O.T.DECC. (Beaudoin et al., 2007). The M.O.T.DECC is used to evaluate the development of student competencies all fieldwork experiences at the University of Ottawa OT Program. It contains 27 competencies. Each is noted as addressed or not. Besides, student performance on each addressed competency is evaluated using six possible scores: experiencing difficulties, making progress, novice, intermediate, ready to practice. Over the course of students’ fieldwork placements, increasing levels of competency are expected so that each of five clinical placements has a specific expected level.
Second, a research assistant carried out semi-structured interviews with each of the student occupational therapists at the end of the placements to explore their perceptions of the OPC fieldwork placement and the impact on clients.
Data analysis
To describe the types of goals that the student clients identified, all COPM goals were compiled and organized into general areas using content analysis; examples were selected for illustration. To assess goal attainment, average COPM scores for performance and satisfaction both pre and post OPC were calculated for each student client. Paired t-tests were calculated to determine the statistical significance of the differences between performance and satisfaction before and after OPC. Similarly, paired t-tests were calculated for differences in symptoms of depression, anxiety, and stress noted on the DASS 21 before and after the OPC sessions. In addition, changes in the level of severity of each symptom were noted and the distribution of changes in levels was noted. All statistical analyses were completed with an alpha of 0.05 using SPSS (v28, IBM Corp, Armonk, NY).
Finally, to determine the impact of providing OPC on the student therapists, the proportion of competencies addressed and the proportion of competencies achieved by each of the students were presented descriptively. Student client qualitative interviews were analyzed using content analysis.
We applied for ethics review to the University of Ottawa Research Ethics Board but were informed that due to the nature of this program, a review was not required.
Results
Student clients
A total of 35 student clients enrolled in the service. Student clients were predominantly female and just over half were undergraduate students (Table 1). Clients participated in 1–6 sessions each (mean = 3.85, SD = 1.40).
Student clients enrolled in OPC.
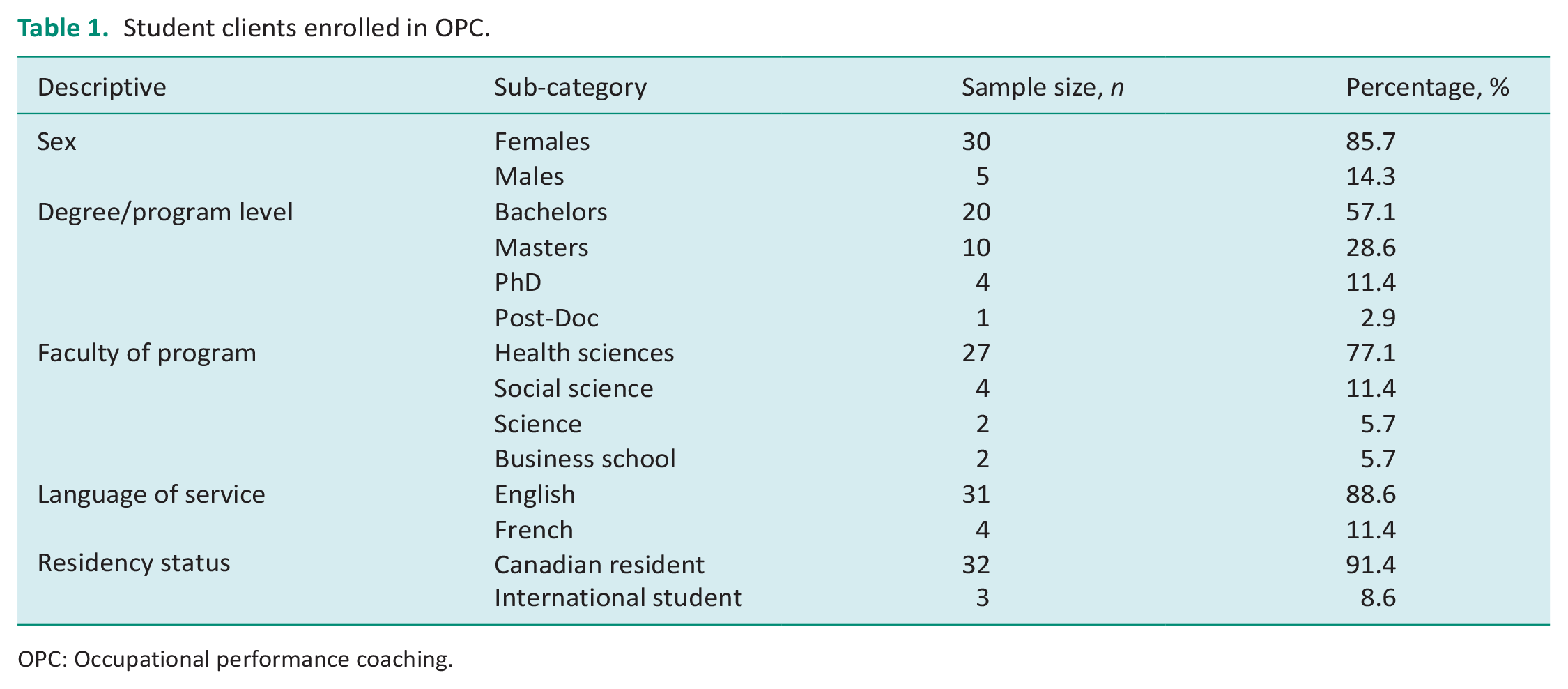
OPC: Occupational performance coaching.
The student clients set goals related to academics, health, financial well-being, professional development, and time management. Examples of student goals are provided in Table 2.
Examples of student client OPC goals.
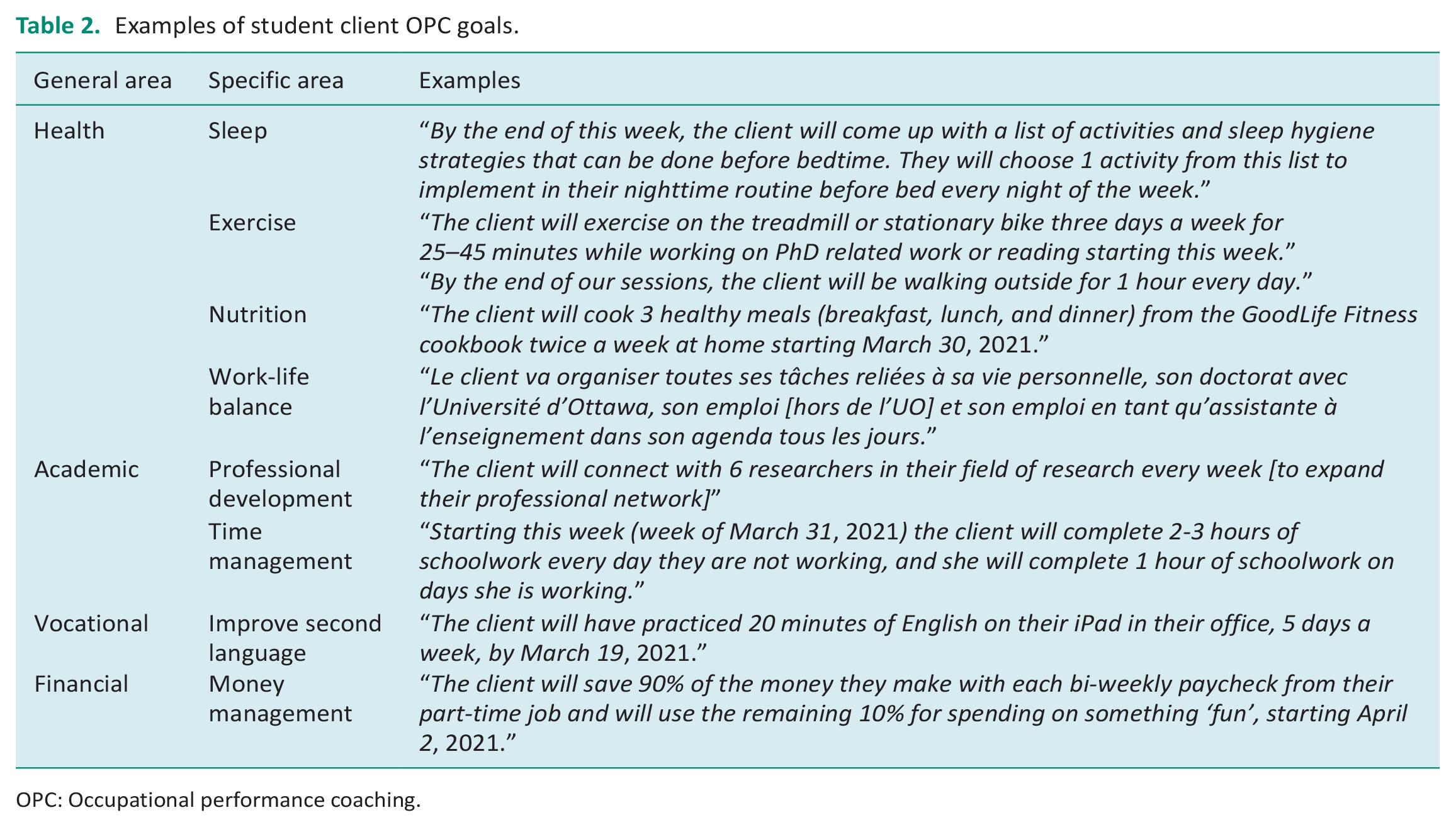
OPC: Occupational performance coaching.
On average, student clients made important progress on their goals as documented with the COPM. Participants experienced a mean change of 3.03 (2.91) in performance and 3.52 (2.56) in satisfaction with performance. These changes were both statistically and clinically significant (Table 3).
Goal achievement: COPM.
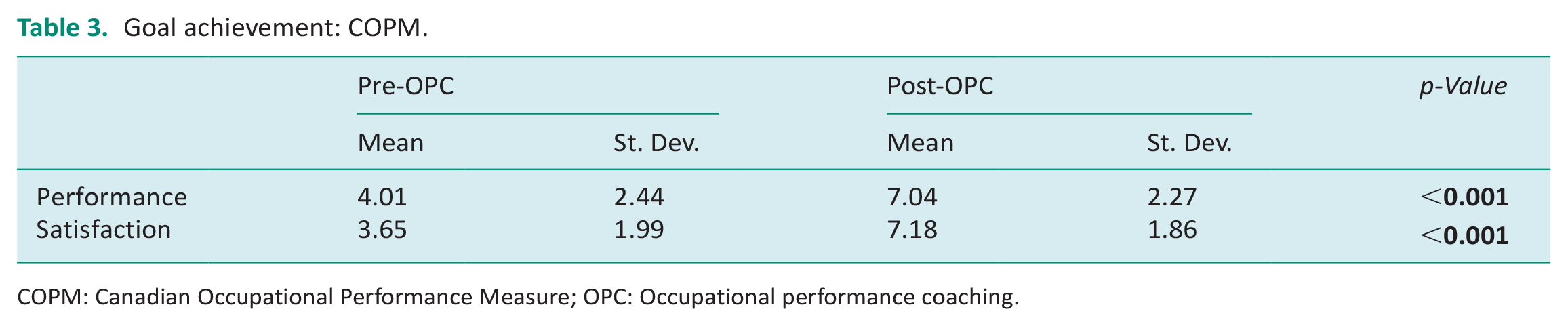
COPM: Canadian Occupational Performance Measure; OPC: Occupational performance coaching.
Eighteen students completed the DASS-21 before and after their OPC sessions. Prior to OPC, 12 students (67%) demonstrated moderate to severe symptoms of depression, anxiety, or both before OPC. Following their participation in OPC, only two students were still demonstrating moderate to severe depression or anxiety symptoms. On average, student clients demonstrated statistically significant improvement in anxiety and depression and change in stress symptoms that approached statistical significance (Table 4).
DASS-21 results.
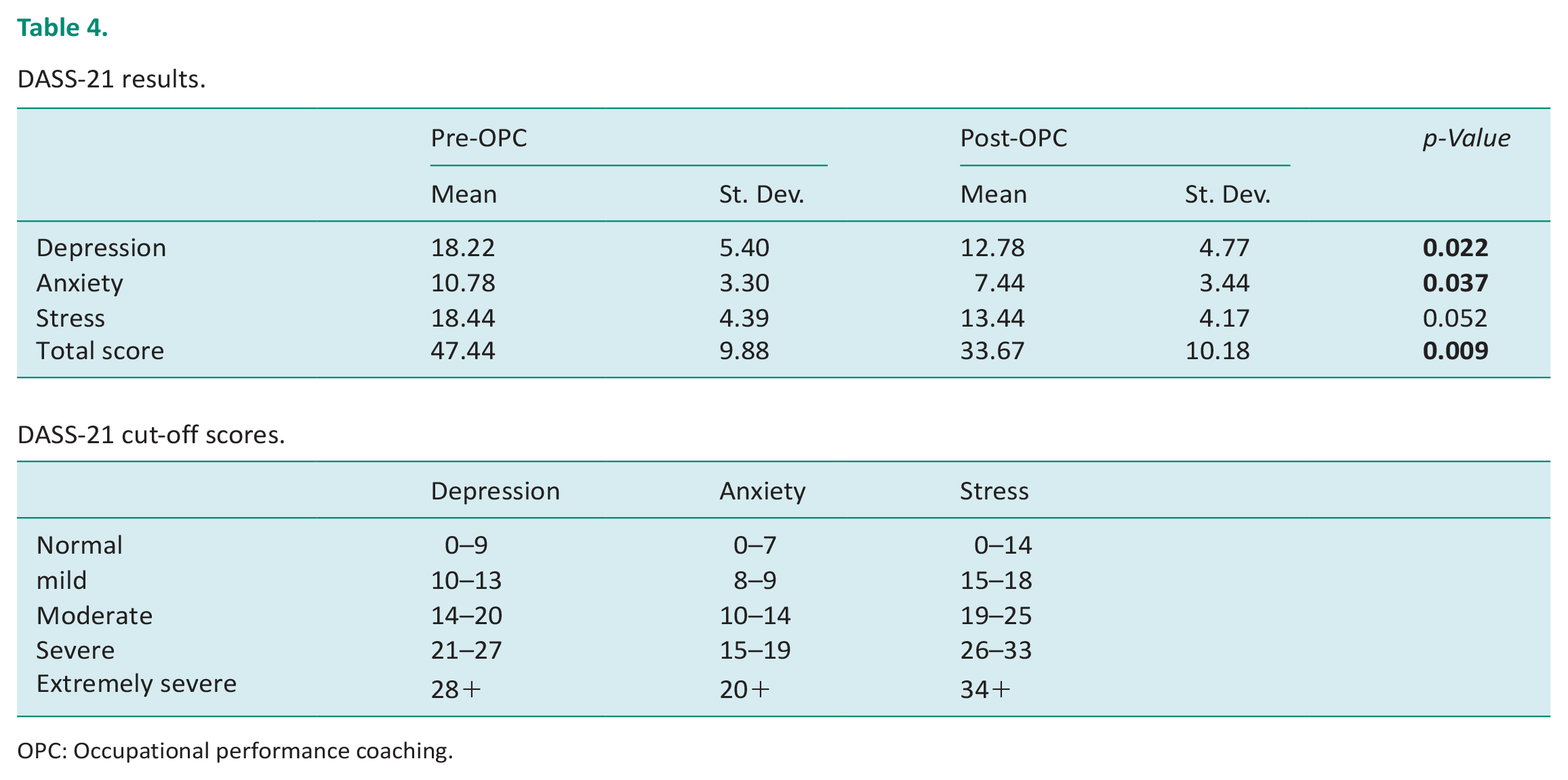
OPC: Occupational performance coaching.
Qualitative student client feedback
During the final session, student clients were asked by their student occupational therapist if they would agree to be contacted for an interview regarding their OPC experiences. Of the 36 student clients, 24 student clients agreed to be contacted, but only four responded to an email requesting an interview. All were females: two were undergraduate students and two were graduate students. Interviews were transcribed and content-analyzed by the first author. All names are pseudonyms.
The student clients described OPC as helpful, but very different from other kinds of help they had received. Three themes emerged from the qualitative data: learning to breakdown goals into manageable tasks, learning to adjust strategies, and disconcerting at the beginning of the OPC process.
Learning to breakdown goals
Student occupational therapists helped clients to analyze their meaningful goals and break these down into achievable actions. Clients were guided to specify the details of their action plans and strategies in their own words: [My student therapist] really helped me to learn that that if you do make a goal then you should break it down into how you are going to do it. . . rather than just making a goal like “I want to work out more” to think, ‘OK, how am I going to do that? Like, I’m going to set out my workout clothes in the morning,. . .
The following quote illustrates student occupational therapists’ use of coaching questions to facilitate clients’ envisioning of a plan for goal enactment: She was really helpful in helping me to lay out a plan. She had steps, like how was I feeling right now about this goal and what could I do to achieve it, and how am I going to be sure that I keep up with it, how can I be accountable for it. Really just asking a lot of questions that I don’t normally think of or plan out. . .Before [I’d set the goal like] I really want to get an A on this midterm, but there would be nothing in between, like, how am I going to do this? so having that training helped me make better goals in the future. . .it was something I’d never really been taught before.
Goals for participation in different occupations were identified by clients focused on solutions: I found it really helpful from the first meeting. . .Because school was on-line, [I had to work on] really keeping myself motivated and keeping up with the work. We also worked on goals that had more to do with managing school and my personal life, accomplishing what I wanted in both aspects and balancing it all, so that was helpful too. Some smaller more specific goals like an upcoming midterm and how to study for that.
Learning to adjust strategies
Clients experimented with strategies they identified in OPC to achieve their self-identified goals and discussed the effectiveness of these strategies in weekly sessions with the student occupational therapist. Clients were guided to evaluate their plan and modify or create new strategies for successful goal attainment: The transition from being an undergraduate student to a master’s student is a transition that is hard for anyone. . . it’s a lot more independent work. I was struggling to stay motivated. . . The thing that’s cool about OPC is that you pick your own strategies. . .at that time I was quite tired. . .I had gotten into some really unhealthy working habits and I wanted to get out of that cycle. . .we worked on turning off my phone til noon, deleting social media apps and using timers. . .writing a list of things I need to do in the day and how long it should take me. . .each day of the week keep a record of what I was accomplishing. . . I created a bedtime [routine] for myself: at 9 OK I shut off my computer. . .before I would work 12 hours a day and I was just making myself sick. . .realizing that strategies this particular time may not work, realizing that if a strategy doesn’t work, that doesn’t mean there’s something wrong with you, you just need to adjust the strategy.
Disconcerting at the beginning of the OPC process
The shift from therapist-led to client-led goal setting and evaluation of their action plans was initially challenging for some clients. They were guided to identify participatory goals in terms of person, task, and context: I found it frustrating, but I liked that it worked. She kept asking ‘what did you do that worked before?’ And I couldn’t think of anything. And then I kept thinking it over and she kept asking . . . eventually I came up with stuff and so we implemented those actions steps. . . For my task completion goal my actions steps were writing my tasks out on a whiteboard and then alternating between study spaces and varying planned tasks and starting homework before 8:30-9. These were all things that I had done before but I had never combined them, and just having them written out so that if I ever get stuck I can go back to these action steps.
OT student competencies
The OPC fieldwork provided students with the opportunity to work on 24 of the 27 competencies of the M.O.T.DECC. Appendix 1 illustrates the core competency domains in the M.O.T. DECC and those not addressed during the OPC placement, and those not attained. During the placement, all students attained the expected level for 20 of these 24 competencies. Two of the students attained the expected level for 23 of the 24 competencies. Half of the students exceeded expectations in 2 of the 24 competencies addressed.
All six OT students, five females and one male, were interviewed. Qualitative interview findings revealed that all of the student therapists appreciated the opportunity to act autonomously in the fieldwork placement, scheduling their own clients, and providing OPC sessions independently with their clients. They viewed the experience as an opportunity to build a practice from the ground up. As well, student therapists believed that the placement provided an excellent opportunity to develop essential interview and relationship-buildings skills, and to help clients identify and work towards meaningful, activity-focused goals.
Listening to the clients, listening to what their priorities are, what's most important to them [not] imposing your own ideas your own values [so] they would come in with their own goals, their own strategies. . . and you would you empower them and not judge . . .let them play out [their own strategies] and let them learn for themselves . . . was, I think, a very good competency to develop. I developed a sense of autonomy and responsibility to make sure everything was correctly done because it was my own caseload and my own clients.
Logistics in developing a client base for referral to OPC led to frustration with having lower numbers of student clients than hoped for. Additionally, student therapists were often limited in the number of sessions they could provide for clients due to difficulties related to ramping up the service and the fixed period of the fieldwork placement. Students also reported that while the fieldwork supervisor provided outstanding support, she was stretched quite thin supervising six students; they would have appreciated more supervision during student therapist-client virtual OPC sessions.
Discussion and implications
In this study, the student clients experienced a number of occupational challenges including academic, relational, and financial, consistent with findings from the literature on factors contributing to university students’ mental health (Beiter et al., 2015; Husky et al., 2020; Pedrelli et al., 2015; Sakin Ozen et al., 2010). We hypothesized that OPC would decrease student clients’ symptoms related to depression, anxiety, and stress related to life stressors.
We demonstrated that OPC provided by student occupational therapists can be effective in helping students work towards their goals and finding effective strategies to deal with challenges in their meaningful occupations. The most notable change in mental health was the decrease in depressive symptoms as measured by the DASS-21. It is possible that mobilization of their own strengths and knowledge to develop and enact effective plans to meet challenges decreased the symptoms of depression.
Our evaluation provides initial evidence that OPC provided by student occupational therapists can help university students achieve academic and other personal goals and improve symptoms of depression and anxiety, however further research is needed. The major limitation of this evaluation was the fact that the current study design and methodologies provide only provisional evidence that OPC supports the achievement of positive mental health outcomes. We recommend a pragmatic trial across a number of universities to investigate the effectiveness of OPC relative to usual treatment (mental health counselling) for university students’ mental health and wellness.
Further research should also gather information more broadly on student client experience of OPC. As noted in the results, only four of the twenty-five clients who initially agreed to be contacted for an interview actually responded to a request for one from the research assistant. A notable potential explanation for this low participation was the timing of the interviews. The OPC program was conducted during the winter term, but the interviews did not occur until the spring-summer break. Student availability and interest for an interview may have been low at this time. Providing student clients with a structured written questionnaire with room for comments may yield greater student client participation.
Among university students, there is an increasing need for accessible and effective services on campuses to support student mental health (Council of Ontario Universities, 2017; Sharp and Theiler, 2018). There is a substantial body of research examining the association between various forms of psychosocial support and mental health (Hefner and Eisenberg, 2009); however, studies indicate that students may be reluctant to seek help due to the stigmatization of mental health problems and silence about mental health in the university environment (Colizzi et al., 2020). A student-led OPC service may mitigate some of the barriers to seeking services by working with someone at the same level (student peer) in an empathic and trusting environment. This “egalitarian relationship” (Overton and Medina, 2008: p. 428) coupled with student occupational therapist training in mental health coaching is unique and mutually beneficial for all those involved in the OPC service.
We envisioned that the OPC service would provide a rich learning experience for student occupational therapists, allowing them to develop valuable skills and competencies. The OPC placement also provided additional mental health placement opportunities that were needed for student trainees. As it was designed, the placement allowed experiential learning about developing and managing a private practice including knowledge of OT regulatory requirements, governmental legislation, ethical practice, and professional standards. Increasingly occupational therapists work in private practice, and this was a rare opportunity to learn essential skills such as contributing to the development of a virtual care OT service and scope of practice, maintaining client documentation and record-keeping, promoting OT and OPC, and independently maintaining and storing client files. Student occupational therapists learned how to provide safe and ethical mental health services through virtual care. While this telerehabilitation approach was necessitated during the pandemic restrictions, it may also help improve availability and accessibility more generally.
There were two major challenges to delivering the OPC service. First, OT fieldwork placements occur at specific times of the year between coursework. This created challenges related to ramping up the program and, particularly, ramping down the program. That is, many more students signed up for the program than could be seen during the 8-week placements in February–March 2021. Second, the student supervision, which included obtaining client consent for student service, providing adequate supervision of sessions to ensure client safety and adequate treatment, and reviewing and signing off on all health records, as well as meeting regularly with students to monitor their progress, required a full-time supervisor. To mitigate these challenges, we recommend the hiring of an OT to help guide and support such a service. This therapist could provide student supervision during placement periods and then continue to see student clients throughout the rest of the year.
Conclusion
This study served as an important first phase in assessing a new contextual approach in OPC and will contribute to improving mental health services and support for university students. Students who received OPC demonstrated achievement of personally identified goals and decreased mental health symptoms. Student therapist provision of OPC worked well but was only available during the fixed fieldwork period. The following recommendations are proposed to expand the OPC service: (1) share our experience with OPC with other university OT programs to increase knowledge about this innovative fieldwork placement and potential for application, and (2) integrate OPC into the continuum of mental health and wellness services offered at post-secondary institutions to build evidence for OPC.
Key messages
Student clients demonstrated statistically significant improvement in anxiety and depression following OPC
OPC offered to undergraduate and graduate students in a university setting and provided a unique mental health fieldwork placement in OT
What this study has added
An OPC service delivered by telerehabilitation for the mental health of university students demonstrated positive outcomes for student clients and OT students, when provided over an 8-week fieldwork placement.
Supplemental Material
sj-docx-1-bjo-10.1177_03080226231161270 – Supplemental material for Student-led occupational performance coaching in a university setting
Supplemental material, sj-docx-1-bjo-10.1177_03080226231161270 for Student-led occupational performance coaching in a university setting by Mary Yvonne Egan, Darene Toal-Sullivan, Dorothy Kessler, Elizabeth Kristjansson and Michael Joseph Del Bel in British Journal of Occupational Therapy
Footnotes
Appendix
OT student competencies developed during fieldwork.

| All students attained or exceeded standard expected | Not all students attained expected standard | Not addressed |
|---|---|---|
| Competency 1. Professional accountability | ||
| 1.1 Practices in an ethical manner | ||
| 1.2 Manages practice-related records and documentation | ||
| 1.3 Demonstrates commitment to lifelong professional development | ||
| 1.4 Contributes to the development of knowledge in OT | ||
| 1.5 Adheres to and supports legislative statutes (e.g., respects standards of practice) | ||
| 1.6 Contributes to other student education in OT | ||
| Competency 2. Occupational performance practice process | ||
| 2.1 Establishes a professional relationship with the client or client representative | ||
| 2.2 Names, validates, and prioritizes occupational performance issues | ||
| 2.3 Selects theoretical approaches | ||
| 2.4 Identifies occupational performance components and environmental conditions | ||
| 2.5 Identifies strengths and resources of partners in the intervention | ||
| 2.6 Develops an action plan based on targeted outcomes | ||
| 2.7 Implements plans | ||
| 2.8 Evaluates and analyzes occupational performance outcomes | ||
| 3. Organization of practice, leadership, and interpersonal relationships | ||
| 3.1/3.2 Utilizes and communicates conceptual and theoretical orientations relevant to OT and communicates the scope of practice to client or intended audience | ||
| 3.3 Establishes parameters and structure for services | ||
| 3.4 Applies knowledge of current sociocultural, economic, political factors | ||
| 3.5 Demonstrates leadership in practice | ||
| 3.6 Establishes collaborative communication with colleagues, team members and relevant stakeholders | ||
| 4. Quality management of OT services | ||
| 4.1 Engages in a continuous process for evaluation and improvement of quality of service | ||
| 4.2 Engages in continuous evaluation of the services provided | ||
| 4.3 Interprets, utilizes, and communicates results of evaluation of the quality of the services provided | ||
| 5. Management and promotion of OT services | ||
| 5.1 Uses information and communication technology to support current and future OT services | ||
| 5.2 Manages or participates in the management of human resources; |
||
| 5.4 Participates in the promotion of OT | ||
OT: occupational therapy.
Research ethics
The Health Sciences and Science Research Ethics Board of the University of Ottawa waived the requirement for approval.
Patient and public involvement data
During the development, progress, and reporting of the submitted research, patient and public involvement in the research was not included at any stage of the research.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) declared no financial support for the research, authorship, and/or publication of this article.
Contributorship
MYE and DTS researched the literature. MYE conceived the study. MYE and DTS wrote the first draft of the manuscript. ME and MJDB were involved in data analysis. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
