Abstract
Determining the cause of death in animals recovered from bodies of water, swimming pools, or other water-containing vessels is challenging. Animals recovered from water may or may not have drowned. The diagnosis of drowning is usually one of exclusion, requiring information from the crime scene, recovery scene, the medical history or reliable witness accounts. While there are characteristic macroscopic and microscopic lesions of drowning, none are specific and are dependent on the volume and tonicity of the drowning medium. Beyond interpreting the postmortem findings, the court may ask pathologists to comment on the behavioral and welfare implications of drowning. This requires an understanding of the drowning process, which is a complex series of sequential, concurrent, and overlapping cardiorespiratory reflexes, electrolyte and blood gas abnormalities, aspiration, physical exhaustion, and breathlessness eventually culminating in death. This review addresses the mechanisms, lesions, and diagnostic issues associated with drowning in nonaquatic companion animals.
Determining the cause of death in animals recovered from bodies of water, swimming pools, or other water-containing vessels is challenging. The key question is this: was the animal alive when it entered the water? 60 The diagnosis of drowning is usually one of exclusion, requiring information from the crime scene, recovery scene, the medical history, or reliable witness accounts. 14,67,71,77 Tides, currents, people, or other animals may move the body from the original scene, and postmortem changes due to submersion, injuries, or scavengers can introduce artifacts and obscure lesions. Animals may be disposed of in water following death due to other causes, or conversely, may be removed from the water after drowning (Fig. 1).
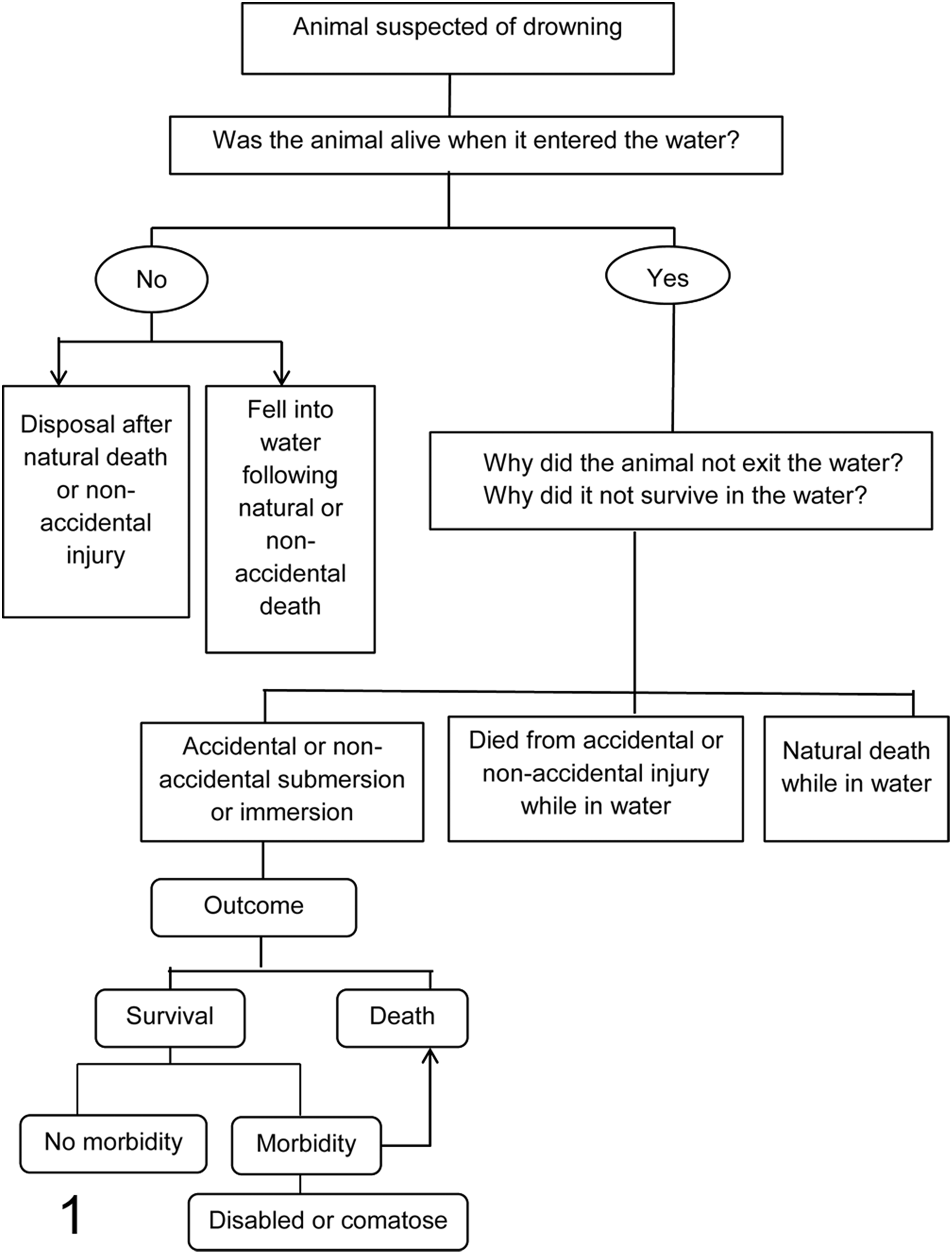
Possible scenarios of bodies recovered from water.
The definition and terminology associated with drowning, as with other types of asphyxia are varied. 5,75 Before 2002, definitions were classified as “drowning” if fatal, or “near-drowning” if the patient survived even temporarily, and both were divided into those cases in which aspiration of water was present or absent. 5 In 2002, the definition of drowning and its possible outcomes were decided by an international expert committee of the World Health Organization (WHO): “Drowning is the process of experiencing respiratory impairment from submersion/immersion in liquid” and “outcomes are death, morbidity and no morbidity.” 5 The following terms referring to drowning, described in depth by Idris et al, 32 are no longer recommended: passive, silent, wet, dry, active, secondary 5,32 or near-drowning. 64 The revised terminology has been applied in at least 1 review of canine drowning 28 and we recommend that it be adopted by veterinary pathologists. Submersion signifies that the entire body is under water, whereas immersion refers to the body being partly covered with water, although the airway must be immersed for drowning to occur. 32
The frequency of drowning in animals is unknown. An estimated 388000 people drown annually and it is the third leading cause of accidental death worldwide. 66 The peer-reviewed veterinary literature on accidental and nonaccidental drowning in animals is scarce, 1,6,28,31,58,60 although the topic is covered briefly in several veterinary forensic textbooks. 18,50,59 Accidents while in water including electrical shock, entrapment, entanglement, and neurologic dysfunction such as ataxia and epilepsy are reported in animals that have drowned, or have been resuscitated following rescue from water. 1,30 Experiments in which dogs or other animals were drowned to determine physiological and biochemical responses to various volumes, temperatures and salinity of water or other liquids 2,3,8,11,17,26,27,53,55,57,72,73,82,83 provide information into the drowning process. Because most of these experiments were done between 20 and 200 years ago, the lack of consideration for the welfare of animals used in these experiments is often disturbing. Although we and others recognize this, 60 useful information applicable to veterinary forensic pathology can be gained from these experiments. The objective of this paper is to review the mechanisms, lesions and diagnostic issues associated with drowning in nonaquatic companion animals.
The Process and Mechanism of Drowning
The drowning process is complex, involving sequential, concurrent and overlapping cardiorespiratory reflexes, electrolyte and blood gas abnormalities, aspiration and swallowing of liquid, vomition, struggling, involuntary movements and physical exhaustion, breathlessness, or “air-hunger” 4 eventually culminating in death. 7 The central mechanism of drowning is rapid and persistent hypoxemia following the introduction of liquid at the entrance of the airway. 17,40,46,53,56,72 Arterial oxygen decreases immediately, 17,39,56 and is accompanied by acidosis and hypercarbia, although the arterial levels of carbon dioxide (CO2) are considerably below 17,56 the 95 mm of mercury required for CO2-induced narcosis. 21,45,56 It is for these reasons that drowning is not considered an acceptable method of euthanasia by the American Veterinary Medical Association 41 and others 4,45 and is considered inhumane. 41 The survival time is inversely proportional to the volume of fresh or salt water aspirated in dogs, 53,56 although aspiration of as little as 5 mL of salt or fresh water in dogs causes rapid and persistent hypoxia without significant hypercarbia. 53,56
The drowning process (Fig. 2), reviewed extensively in the medical literature 5,14,32,40,46,51,67,71,84 and largely based on experiments in dogs, incorporates behavioral and biological responses to drowning. 2,17,44,53,56,83 This has been categorized into the 5 phases of drowning (Table 1). 52
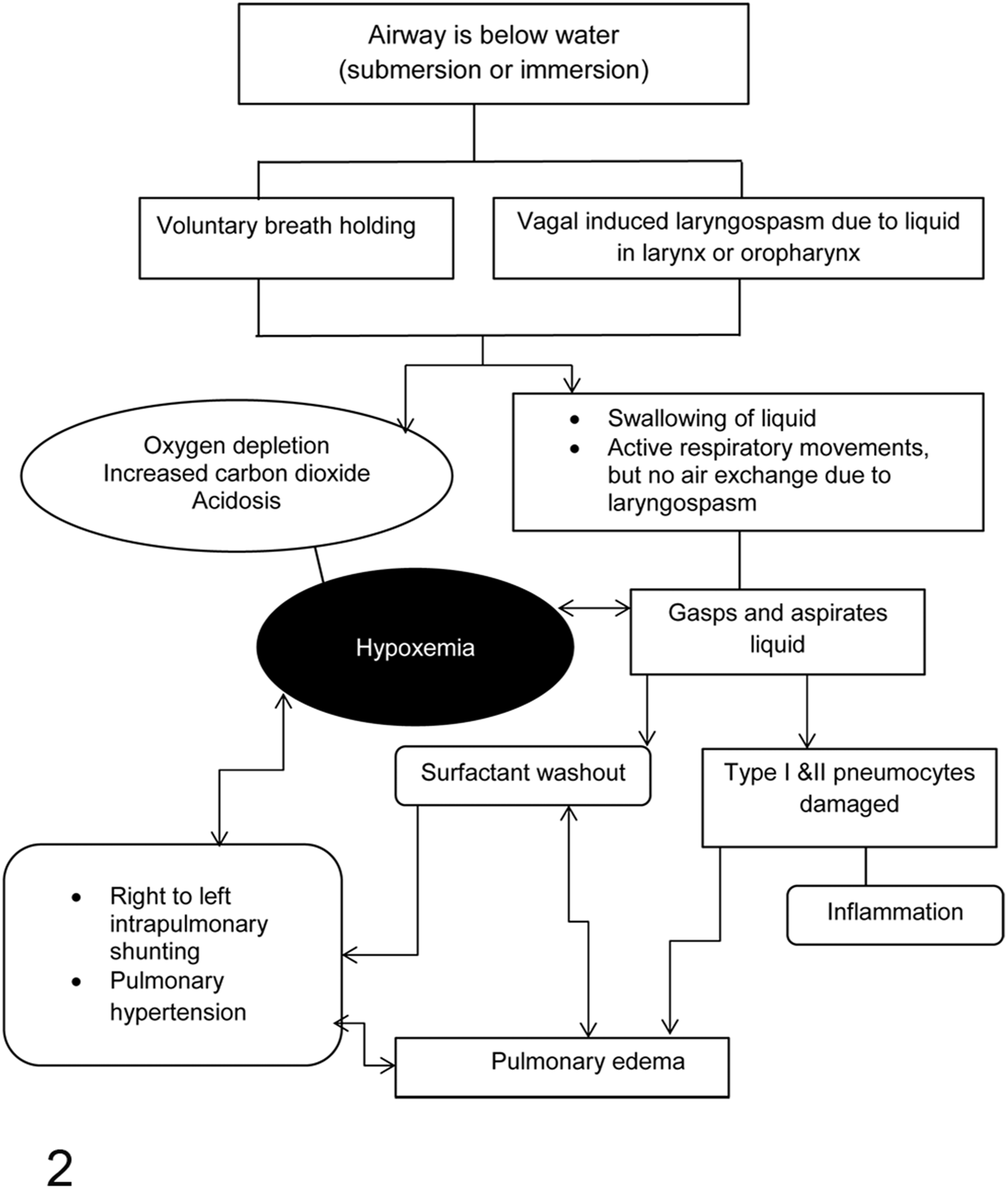
The drowning process.
The 5 Phases of Drowning in Dogs. 51

Initially, there may be a few deep respirations, although breath holding and vagal mediated laryngospasm usually occur upon submersion 8,44 with an abrupt decrease in arterial oxygen. As little as 2 mL of water contacting the larynx or aspirated into the lung, can cause laryngospasm in dogs. 2 The laryngospasm may last 1.5–2 minutes during which arterial CO2 increases 72 and acidosis develops. 17,30,40 Bradycardia 2,54,81 occurs immediately following submersion 8,26 or after brief tachycardia. 17,27 Blood pressure immediately increases and then progressively decreases. 27,53
Submerged, nonanesthetized dogs struggle violently for 1.5 minutes, 44,52 and because the glottis is closed, thoracic inspiratory movements are attempted and liquid is swallowed, but 2,64,81 gas exchange does not occur. If unconsciousness occurs due to hypoxemia, the larynx relaxes and water is aspirated, 47 or, if the animal remains conscious, apnea ceases and water is aspirated and swallowed due to deep inspiratory gasping. 43 After 3 minutes, spasmodic convulsions and seizures occur 27,44 and over distension of the stomach with water causes violent vomition. 44 Electroencephalograph (EEG) activity varies with the duration of initial apnea: the EEG became isoelectric at about 3 minutes in dogs with brief initial apnea, whereas dogs with initial apnea of 2 minutes had an erratic EEG, that was isoelectric at 30 seconds, then reactivated at 2 to 3.5 minutes before becoming flat. 81 Cardiac asystole or observed death occurs usually within 5 minutes, but occasionally up to 10 minutes following submersion. 8,27,44,52,56,72,85 The initial hypoxemia in fresh and salt water drowning is intensified by pulmonary edema, and is exacerbated by exponential catecholamine release, subsequent vasoconstriction, cardiac arrhythmias, 17 pulmonary hypertension, and right to left intrapulmonary shunting. 17,33,46
Electrolyte and intravascular changes during drowning depend on the salinity and/or volume of water aspirated. The biochemical effects of water are primarily osmotic 53,55,82,83 and not temperature related. 17 Distinguishing between salt water and fresh water drowning is given little clinical significance in people, 46,64 although some think that it does impact successful resuscitation and chance for survival, 17 but it is important to the forensic investigation. 16
Hemodilution, hypervolemia, decreased serum sodium, chloride, osmolality, hematocrit, and hyperkalemia occur in dogs drowned in fresh water. 17,55,72,82 The changes are temporary due to redistribution of fluids within the body 53,72 although the hemodilution and electrolyte alterations may persist if the volume of water aspirated is 22mL/kg or above. 72,82 In dogs, aspirated fresh water penetrates the circulation within 3 minutes, 47,53 and an estimated 10% of the body weight can be absorbed by the lungs during fresh water immersion. 17 Dilutional hypovolemia was not present in a case series of dogs and cats resuscitated following submersion in fresh water. 30 Hemolysis in dogs was not evident until over 5mL/lb (2.3mL/kg) of water was aspirated. 54 Volume dependent ventricular fibrillation is common, occurring in many but not all dogs drowned by volumes of 20mL/lb (9.1mL/kg) but not by 10mL/lb(4.5mL/kg). 53 The ionic charges responsible for the surface-tension properties of surfactant are altered by fresh water which results in alveolar instability and pulmonary atelectasis. 51,53 Atelectatic alveoli are perfused, but not ventilated, and there is right to left intrapulmonary shunting, 51 further exacerbating the hypoxemia.
Death due to salt water aspiration is more lethal than freshwater aspiration, 8,9,36 requiring half (10mL/lb [4.5mL/kg]) the aspirated volume as for fresh water (20mL/lb [9.1mL/kg]). 53,56 Drowning in hypertonic fluids of 2.5%-3.5% or seawater results in hemoconcentration, increased serum sodium, osmolality and potassium. 17,56 The aspirated hypertonic fluid pulls fluid from the circulation into the alveoli, damaging the basement membrane, with washout of surfactant and reduced lung compliance. 24 Ensuing pulmonary edema decreases the ventilation/perfusion ratio and right to left intrapulmonary shunts develop. 46 Type I and II pneumocytes 10,88,89 and alveolar capillary endothelium 10,36 are damaged by both fresh and salt water. Neither hemolysis nor ventricular fibrillation are features of experimental seawater drowning. 82,83
Drowning ultimately results in progressive cerebral hypoxia 46 and death. Irreversible injury occurs in selective regions of the brain within 4–10 minutes and persistent coma develops within a few minutes after that time period. 23,62 The precise outcome of hypoxic injury due to drowning is difficult to predict even if the individual is rescued and resuscitated. 87
Cold Water Immersion, Autonomic Conflict, and Hypothermia
Humans suddenly submerged in water 5°C below body temperature may become unconscious and develop cardiac arrhythmia possibly due to vagal stimulation and/or catecholamine release. 17,19,49,64,76 The parasympathetic and sympathetic responses following rapid submersion and breath holding are the diving response and cold shock response respectively. 76 These responses are due to several reflex reactions that produce a predictable sequence of physiological events. 22 The diving response of apnea and bradycardia found in all marine and land vertebrates studied, 76 is initiated by activation of the cold receptors of the face via the ophthalmic and maxillary divisions of the trigeminal nerve, although vagal receptors in the pharynx and larynx produce similar responses. 76 Cold thermoreceptors of the skin also mediate the sympathetic associated cold shock response which causes tachycardia, hyperventilation, peripheral vasoconstriction, and hypertension. 19,76 Both responses can cause cardiac arrhythmias independently, or together by issuing conflicting, simultaneous signals to the heart. 22,37,76
Within 2 minutes of submersion in cold water, core body temperature decreases more rapidly and deeply than with immersion, 17 due to the aspiration of larger quantities of water and contact with the large surface area of the pulmonary circulation. Primary hypothermia due to submersion is fatal when rectal temperatures drop to 20°C, or below. 63 The onset and duration of cardiorespiratory and cerebral responses were similar in dogs that had their tracheas clamped and submerged in 0–1°C water, 85 compared to those submerged in normothermic or cold water but allowed to aspirate water. 2,44,82,83 The absolute and relative decreases in rectal and cerebral temperatures were proportional to the submersion time. Spontaneous circulation could be restored in 75% of the dogs over the course of 1.5 hours using cardiopulmonary bypass, although spontaneous breathing and return of EEG activity occurred in only 56% of the dogs. 85 While these experiments concluded that resuscitation of hypothermic submerged dogs is possible by extending the time for reversible cerebral hypoxia, 17 the experimental protocol removed the effects of aspirated liquid on the cardiopulmonary system.
Morbidity
A case series of 25 dogs and 3 cats resuscitated following submersion in fresh water concluded that the prognosis for survival is good if respiratory tract failure and cardiac arrhythmias do not develop. 30 Level of consciousness upon presentation, even coma, was not associated with outcome. 30 Complications in animals that survive drowning include reduced mentation or neurological deficits, 51 noncardiogenic pulmonary edema, 29 septic pneumonia, 6 and acute respiratory distress syndrome. 30
Macroscopic and Microscopic Lesions of Drowning
Distended, heavy, edematous lungs that fail to collapse, and stable froth in the trachea, mouth, or nasal passages are characteristic of drowning (Fig. 3), but they are not specific, as these may be due to other causes. 46,48 Emphysema aquosum is a term used in medical forensic pathology to describe over-inflated, water-logged lungs with histologic findings of alveolar dilation, thinning of alveolar septa and compression of alveolar capillaries. 48,77 However, this term should be avoided in veterinary pathology and it is better to specifically describe the lesions for clarity. Tables 2 and 3 list macroscopic and microscopic lesions in drowned animals. In individual cases, these lesions may or may not be present. Stable froth in the tracheobronchial tree (Fig. 4), larynx and, nostrils can be produced only by a live animal 59 and may also arise with other causes of pulmonary edema. 46 Blood-tinged froth is produced by hemolysis of red blood cells within the fluid. 52 A mare rescued from drowning had stable red froth at the nares and continued to expectorate this material by paroxysmal coughing. 1 Foreign material deep within the tracheobronchial tree and lungs is compatible with aspiration rather than passive entry following death (Fig. 5). 59 The presence, severity, and type of pulmonary macroscopic and microscopic lesions are not uniform, even within the same histological section (Fig. 6).
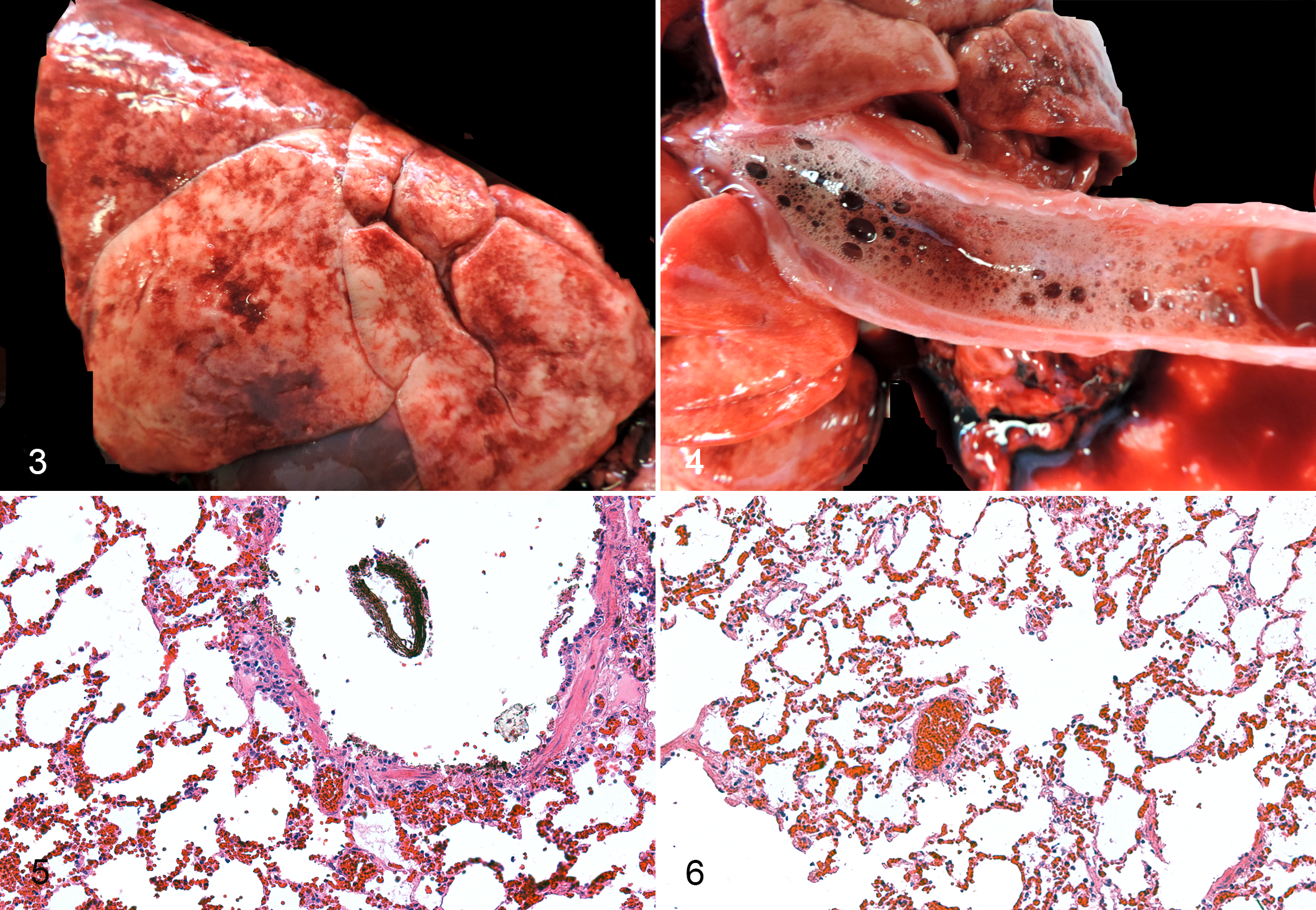
Macroscopic Lesions of Drowning Documented in Animals.

Microscopic Lesions of Drowning Documented in Animals. 60

In humans, the external foam and stable froth may persist for several days, even with the onset of putrefaction. 46 Both features may disappear, or are altered by the effects of time, handling, storage, and freezing of the body prior to postmortem examination. Investigators should provide, or pathologists should request photographs and documentation of the animal at the recovery scene especially if the postmortem examination is not immediate.
The amount of liquid penetrating the lungs depends on the respiratory efforts, laryngospasm and time of cardiac arrest. 47 Previously, the majority of drownings in people were classified as “wet-drowning” and the 10–15% without evidence of aspiration as “dry-drowning.” A review of 1590 cases of drowning in humans indicates that the estimate of “dry-drowning” is closer to 2%. 47 “Dry” lungs in human victims were attributed to many causes such as sudden cardiac arrhythmias, 76 cardiac arrest or laryngospasm following submersion, 47 may represent one end of a spectrum of drowning lesions or, more likely, deaths in water due to natural causes or are bodies disposed in water. 47,52,64 The significance and pathophysiology of “dry-drowning” is debated in medical forensic pathology, 47 and it is recommended that these terms should now be avoided. 32 The pathophysiology of “dry-drowning” in humans may not parallel that in animals: regardless of the volume of water aspirated in dogs, even low volumes caused hypoxemia and decreased lung compliance. 55,56 A lack of significant fluid aspiration has been attributed to laryngospasm 44 or the failure to gasp. 2 Lungs lacking evidence of aspiration are documented in experimental drownings of muskrats and beavers that had a mucus plug in the trachea. 26
Additional findings in humans that may support a diagnosis of drowning are pleural effusion, subdural discoloration of the petrous temporal bone due to congestion or hemorrhage in the mastoid process and middle ear, hemorrhage in the neck muscles, a contracted spleen, 46,71,77 Paltauf’s spots and hemolytic red staining of the aortic intima, 13,15 and left heart. 92 Paltauf’s spots are subpleural, intraalveolar hemorrhages, blurred due to hemolysis. 46 It is uncertain from the veterinary literature whether these lesions have been accidentally overlooked as subpleural hemorrhages are shown in Figures 3 and 5.
The appearance and approximate volume of gastric contents should be documented as swallowing of water is common during drowning, 2,44 and if vomited, may be aspirated. Gastric mucosal lacerations due to over distension of the stomach with water are sporadically reported in human drowning victims. 46 Elevated liver enzymes in animals resuscitated following submersion were attributed to hepatic hypoxia and necrosis, but this cannot be confirmed as histopathological examination of liver was not described. 30 Hepatocellular necrosis 6 was confirmed in 1 dog that aspirated water from a drainage ditch, but it cannot be determined if this was due to the initial drowning or sequelae such as cardiorespiratory failure. Myocardial lesions of contraction bands and rupture of intercalated discs in the cardiac myocytes of rats drowned in either salt or fresh water, 35 may be due to excessive catecholamine release.
A thorough postmortem examination will aid in determining if significant intercurrent diseases are present, 30 and a medical history of conditions such as epilepsy would also be useful particularly in determining why an animal was unable to extricate itself from the drowning medium. Hyponatremic encephalopathy due to excessive intake of fresh water (water intoxication) should also be considered, particularly in animals that play or train in fresh water. 86
Weights such as blocks, tires or chains bound to the animal indicate intentional submersion of the body, but if present, should not be used to corroborate if the animal was alive or dead at the time of submersion. Contusions, subcutaneous hemorrhages, or other lesions of blunt force trauma of the head, neck, or limbs may be present in animals that were forcibly immersed or submerged in water. 50,59
Postmortem Changes
The postmortem submersion interval and postmortem changes that occur while in water and following retrieval may make examination and determination of the cause of death even more challenging. Early changes are skin maceration, lividity, rigor mortis, and algor mortis, and late changes include initial putrefaction, advanced putrefaction including adipocere formation, and skeletonization. 25,46 Adipocere is a waxy material produced on bodies submerged in water that results from degradation of adipose tissue by endogenous and bacterial enzymes. 74 Postmortem changes in the water, as on land, are time- and temperature-dependent. 46 The lower temperatures of bodies of water usually retard rigor mortis and accelerate body cooling. 25,46 Decomposition while in water is slower than on land however, once a body is removed from the water, the process rapidly accelerates. The body initially sinks and then rises to the surface once putrefactive gases increase buoyancy. 74 If the water is cold enough, putrefaction may not occur and the body may never resurface. Depending on the duration and conditions of submersion, hair may slip from the skin and the entire body may be waterlogged. 46 Scavenging by aquatic animals and trauma inflicted by natural and man-made elements of the aquatic environment, may create postmortem lesions or may alter or destroy antemortem lesions. 46 Water may dilute antemortem hemorrhages, and projectile, sharp force, or blunt force injuries may be obscured or effaced by maceration. A small study in 3 dogs identified enhancement of the supravital histological changes of myofibre “disintegration” in muscle traumatized up to 6.5 hours of death and submersed in seawater. 78
Ancillary Tests Used in Determination of Drowning
Lung Weights
The increased weight of lungs and pleural fluid used to support the diagnosis of drowning in humans is unreliable as many variables influence the result. 32,38,47,64 Lung weights of 1000g 77 to 1400g 38 used to confirm drowning in humans is misleading as there is no agreement in the medical literature regarding normal lung weights. 47 Similarly, reference values for postmortem lung weights are not available for most breeds of animals and application of allometrically determined lung weights 43,79 require further validation if applied in a forensic context. A drowning index of the weight ratio of the lungs and pleural effusion to the spleen has been proposed in humans to be more accurate than absolute lung weights, 61 although it is affected by postmortem interval and has a relatively low sensitivity and specificity of 66% and 77.5% respectively. 80 It remains to be determined if this measurement is accurate or applicable to animals.
Diatoms
Perhaps no other ancillary test in the diagnosis of drowning in humans has received as much attention, scrutiny, and debate as the use of diatoms. 14,20,34,42,46,47,65,67 –70,77,90 Diatoms are unicellular algae with a silica cell wall (frustrule) that makes them inert to acids, high temperatures and enzymatic digestion. 91 The use of diatoms as a diagnostic test for drowning is based on the assumption that the individual must be alive for them to be aspirated, penetrate the alveolar-capillary membrane, enter the circulation, and enter tissues including marrow. 6,74 If meticulous and usually time-consuming techniques are used to retrieve diatoms, usually from the bone marrow, their presence in large numbers may corroborate a diagnosis of drowning, and their unique characteristics may identify the location and drowning medium of the victim. The sensitivity of the method is relatively low and depends on the time of year when the algae bloom. 70 The specificity may be high with the appropriate techniques; however, the prospect of contamination during the postmortem submersion interval and sample preparation is high, resulting in false positive results. 25 As diatoms have been found in bodies not recovered from water and in living people, the possibility that they enter the circulation from ingested food must be considered. 91 Although diatoms were identified in the tracheal wash of a dog that aspirated during a seizure in a water-filled drainage ditch, 6 application of the diatom test to confirm drowning in animals requires additional rigorous validation studies.
Electrolyte Tests
Differentiation between salt water and fresh water drownings using electrolyte levels in blood or vitreous humor does not appear to have been widely accepted. The Gettler test comparing chloride levels in right and left ventricular blood, 77 is determined to be unreliable. Elevated vitreous humor sodium levels in cases of salt water drowning and decreased levels in fresh water drowning, proposed as a marker of the drowning medium, 16 may be useful but require further validation.
Conclusion
Diagnosis of drowning is difficult 12,46,48,50,59 as bodies recovered from water may or may not have drowned. A thorough postmortem examination is necessary to identify and document the presence and absence of lesions that may corroborate or rule out death due to drowning, to identify intercurrent disease that may have influenced the animal’s behavior in or around the water and to identify traumatic injuries consistent with nonaccidental injuries of forced submersion or immersion. While there are characteristic macroscopic and microscopic lesions of drowning, none are specific. Additional information from the crime scene investigators, including witness accounts, an accurate history, previous medical conditions of the animal, and disposition of the body when retrieved from the drowning medium are often needed to allow the pathologist to consider the postmortem findings in context.
Footnotes
Acknowledgements
We thank Dr Sean McDonough and Dr Murray Hazlett for their photographic contributions.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
