Abstract
Submission of cases of suspected animal abuse and neglect (AAN) to veterinary pathologists is increasingly frequent. These cases require modification of postmortem procedures and written reports, as the questions asked by courts typically differ from those asked in routine diagnostic cases. Here we review the practice of veterinary forensic pathology as it applies to cases of companion AAN, as well as the fundamental principles of forensic pathology, the components of a forensic necropsy, and the goals of the necropsy in cases of blunt-force trauma, projectile wounds, and starvation. Future directions and endeavors in veterinary forensic pathology are broached.
Keywords
Introduction to Veterinary Forensics
While the notion that cruelty to animals is a symptom of depravity predates sociological studies, there has been a recent global increase in the enforcement of laws regarding animal care and the enactment of tougher laws regarding animal abuse and neglect. One driving force behind this change has been the affirmation of the link between animal abuse and various types of interpersonal violence, including child abuse, domestic violence, rape, robbery, and homicide. 31 Animal abuse at a young age appears to be predictive of later interpersonal violence, 19,37 and there is strong evidence that individuals are often violent toward animals and people concurrently. 5
Definitions of and criteria for animal abuse and neglect vary among jurisdictions, countries, and cultures. However, in general, animal abuse is an act of commission and gives satisfaction to the perpetrator. 43 Animal abuse is often legally defined as gross neglect, physical trauma, sexual abuse, hoarding, cockfighting, or dog fighting. In contrast, animal neglect occurs when a person deprives an animal of food, water, shelter, or veterinary care and is frequently an act of omission stemming from ignorance. 43
Changes in laws and their enforcement have created a demand for forensic veterinarians (FVs), who possess a special combination of knowledge and skills. They are familiar with laws concerning animals in their jurisdiction and are points of contact for law enforcement officers when cases of suspected AAN occur. They simultaneously care for the injured or debilitated while documenting their condition and collecting evidence. They may have some training in crime scene investigation (eg, blood splatter analysis, DNA collection). FVs may conduct all or part of a postmortem investigation, including the necropsy, consulting with specialists, and referring samples as needed. Finally, FVs tie together all information garnered from the postmortem investigation, witness statements, crime scene analyses, and so on; compose a final report for use in court; and prepare to testify.
The duties and responsibilities taken on by FVs overlap with forensic physicians and nurses, who care for survivors of crimes, and forensic pathologists (FPs), agents of public health who conduct the portion of the postmortem investigation relating to the body. In some countries and jurisdictions, FPs are called to scenes of unwitnessed deaths, accidents, suicides, and crimes, to inspect the body and its effects in the context where it was found. Subsequently, FPs perform an autopsy, histology, and ancillary testing; determine the cause of death (COD); and prepare a final, summary report for use in court along with their testimony. FP training in many countries, including the United States, Canada, Australia, and England, comprises medical school and 3 to 5 years of postdoctoral training, often in the form of a residency in anatomic pathology and a fellowship in forensic pathology. FPs consult with a wide variety of experts in other forensic fields, such as forensic anthropologists, experts in the identification of human skeletal remains and lesions; forensic entomologists, who use arthropod biology to address legal questions; and forensic odontologists, who specialize in dental remains and bite marks.
The practice of VFP is often an adaptation of its counterpart human field. Although veterinarians may draw upon the same general knowledge as FPs, a significant proportion of human forensic pathology case material is irrelevant to veterinary species (eg, drug overdoses and suicides). The inverse is also true. Common case types in veterinary forensic pathology, such as neglect, are less well studied in human forensic pathology, where criminal cases of fatal child and elder abuse and neglect are apparently rare. Many cases in VFP, such as those involving dog fighting and cockfighting, illegal rodeos, ritualistic animal sacrifices, exotic animal importing/exporting, hunting out of season, and poaching, have no counterpart.
Despite decades of activity on an international scale, including seminars, symposia, the publication of many articles and multiple books, and the formation of wildlife and veterinary forensic organizations, the field of VFP remains in its infancy. Still, as long as veterinary pathologists are regarded as experts in animal death, they will receive forensic cases. Thus, the onus is upon veterinary pathologists to educate themselves about VFP and to further the development of the field. The purpose of this review is to familiarize veterinary pathologists with the terminology and basic techniques of VFP and the aims of the necropsy in specific, select case types of companion AAN: trauma, projectile wounds, and neglect and starvation.
Fundamentals of Forensic Pathology
The practice of forensic pathology is not markedly different from other work in pathology, but it does differ. Like any branch of pathology, the practice of VFP requires an awareness of the questions being asked of the pathologist. In VFP, simply conducting a necropsy, compiling morphologic diagnoses, and generating a standard report are at best insufficient and at worst irrelevant if it does not
The Scene
A unique aspect of forensic pathology is the importance of the “scene” or “locus”—the surroundings in which a death occurred and/or a body is discovered. The importance of the scene in forensic pathology is analogous to the importance of the medical history in diagnostic veterinary pathology. Knowledge of the scene (eg, ambient temperature, availability of shelter, location and amount of food and water, presence of other animals, amount of urine and fecal soiling, and the presence of wire, batteries, and other hazardous debris) may be crucial to interpreting changes noted at necropsy and establishing a pathophysiologically valid and likely COD. Examining a body within its scene is similar to a taking a medical history; it requires practice and skill, and the information may be critical, helpful, noncontributory, or wholly misleading. Note that it is routine in FP to determine a COD based on evidence from the scene when the autopsy does not reveal one but rules out competing, likely CODs. It is for these reasons, and the frequency of autopsies without significant findings, that the police investigation and crime scene analysis are at least as important as the autopsy.
The Body as Evidence
The body presented for necropsy in forensic cases is more than a carcass. It is evidence. Because a necropsy is a one-time-only event, forethought should be given to the ancillary diagnostic tests that could be indicated and the samples required. 43
As always, the timing and method of disposal of remains should be made clear with submitters prior to necropsy and documented in the final report. Some submitters may request the remains be held until the case is adjudicated in the event the defense requests a second necropsy. This is impractical if not impossible for most facilities. Moreover, second necropsies are often impossible due to the common practices of animal cremation and rendering, whereas for people, entombment, deep burial, and/or embalming make second autopsies more feasible. Finally, the necropsy itself alters the appearance of organs and their relationship to each other, obfuscating, if not destroying, lesions.
51
For these reasons, worthwhile second necropsies are generally limited to cases in which the first necropsy was recent and limited in scope. In contrast,
Cause, Mechanism, and Manner of Death
Determining the COD is often the primary goal of the postmortem investigation. In forensic pathology, the concept of COD has been broken down into subtypes to put finer points on the pathophysiologic sequence of events and to accommodate death certificates.
21
The COD that is generally of interest to the courts is known as the primary, proximate, or underlying COD and is defined as the
CODs are in contrast to the mechanism(s) of death, the altered physiology and/or biochemistry set into motion by a COD. Mechanisms of death are, by definition,
The manner of death is a classification scheme that exists almost exclusively for epidemiological purposes. All human deaths are placed into 1 of 5 categories: accident, homicide, suicide, natural, or undetermined. The complied data are used to track trends and guide public health recommendations. Manner of death would appear to be of little use in VFP, not only because the terms and conditions frequently do not apply to animals 5,9 but also because no national or international database of forensic pathology investigations exists, to the authors’ knowledge.
Occasionally, the cause and mechanism of death may remain unknown after the autopsy, but the circumstances strongly suggest a criminal manner of death. For example: a human body is found in an abandoned building, in a closet, wrapped in plastic with the limbs bound. The autopsy does not reveal a COD. In this situation, even with an undetermined COD, declaring the manner of death a homicide has important legal implications. Comparable circumstances can and have occurred in VFP. For instance: the body of an animal is found within a container submerged in a body of water, and the necropsy reveals no significant lesions and no evidence of euthanasia. Ascribing an animal death to presumptive abuse or neglect when the cause and/or mechanism of death is undetermined has unknown legal implications, which would likely vary among jurisdictions and countries.
Significant differences between the human and veterinary fields of medicine necessitate adaptation of the concepts cause, mechanism, and manner of death to VFP. This is perhaps most evident in cases where the animal has been euthanized. Except in cases of disease surveillance, overpopulation, or unwanted behavior, euthanasia of animals is nearly always performed due to illness or injury, and as such, euthanasia is nearly always an immediate, and not primary, COD. Thus, a primary COD should be proffered in all cases in which euthanasia is the immediate cause of death. The primary COD in cases of euthanasia is often simply the rationale given for euthanasia (eg, spinal fracture). If the reason proffered for euthanasia is nonetiologic specific (eg, “debilitated”), the underlying COD should be determined by the postmortem investigation. Bear in mind that whether an animal survived, succumbed, or was euthanized as a result of abuse or neglect might be irrelevant in the eyes of the law. What is more often relevant is whether a criminal abuse or neglect was committed, not the outcome of events. Proper identification of the primary COD will aid the court in this endeavor.
If the methods used for a given species do not meet local, national, and/or species-specific standards, such as the American Veterinary Medical Association (AVMA) guidelines on euthanasia, 2 then the act is not euthanasia—it is just plain killing. Distinguishing between approved methods and the unlawful killing of animals, no matter how purportedly painless or rapid, can be critical in cases of alleged animal abuse, as a defendant may claim that he or she was simply “euthanizing” an animal. Courts unfamiliar with standards may accept this argument, and so the difference should be highlighted in the written report.
Questions of Time
Questions of time and duration are common in FP and VFP. Common questions include the time of death (TOD), whether injuries were sustained antemortem or postmortem, the age of injuries, the ages of multiple injuries relative to each other, and the duration of disease, pain, and suffering. The first question is often the most difficult to answer with a reasonable degree of medical certainty, whereas the latter questions are often far easier to answer and often more important in cases of AAN.
Establishing an accurate and precise TOD persists as the holy grail of forensic pathology, despite decades of research. Although time is the constant by which we are used to measuring change, decomposition—autolysis plus putrefaction—is not constant over time but influenced by myriad factors such as the temperature of the body at the time of death, the ambient temperature, the surrounding environment (air, water, ground), ambient pH (water or soil), disease state (fever, bacteremia, etc) at the TOD, and scavenging by animals or insects, to name just a few. Although a thorough discussion of methods used to determine the TOD is outside the scope of this article, types of evidence used in determining TOD include corporal evidence such as drying of mucous membranes, sclera, and skin slippage; environmental evidence such as species and stages of insects present; and anamnestic evidence, such as the last time the animal was seen alive. 39
Algor mortis, cooling of the body after death, is used in some cases to roughly determine TOD. Core body temperature is recorded at the scene where the body is found using specially designed thermometers, along with ambient temperature. Scant research to determine rates of cooling for a variety of body conditions, hair coats, and environments has been conducted in veterinary species. 15,41
In summary, the amount of information available for determining TOD in veterinary species is extremely limited. Given the limited amount of information, as well as the persistently imperfect and inexact science of time of death determination, currently veterinary pathologists may be as well served by personal experience as by sophisticated rectal probes.
Questions of Vitality
Establishing the vitality of injuries—that is, whether injuries were sustained antemortem or postmortem—is frequently best answered by histologic examination of the lesion. The presence of hemorrhage confirms that an injury was vital or at least perimortem, whereas the nature of inflammatory infiltrates and/or granulation tissue, if any, may be used to roughly assess the age of the injury. 12
Despite advances in the field, including better characterization of histologic changes and the increasingly routine use of immunohistochemical stains to age wounds in people, 12 histologic aging of wounds is an imperfect science, especially in veterinary forensic pathology, as discussed in a recent review. 34 Studies of histologic and cellular characteristics of different types of wounds (lacerations, incisions, hematomas) over time in a given species with the specific aim of addressing forensic questions are sorely needed. Until then, veterinary pathologists will have to adapt studies that do exist for veterinary species and adopt what is known about the forensic histopathology wounds in people as they see fit, although this may be perilous.
Questions Specific to Cases of Animal Abuse and Neglect
In cases of AAN, veterinary pathologists should be prepared to be asked questions regarding the time to insensibility, that is, the length of time between the onset of the underlying COD and the point at which conscious nociception was lost. As experts in pathophysiology, veterinary pathologists are well equipped to answer this question. Veterinary pathologists should also be prepared to answer—or prepared to decline to answer—questions regarding the degree and duration of pain and suffering.
The Forensic Necropsy
Background Information
As with any other case, pathologists should collect as much information as possible prior to the necropsy. In AAN cases, this includes crime scene photos, police reports including witness statements and statements made by the accused, prior medical history, and treatments including type and method of euthanasia, if applicable. Frequently, little to none of this information is available, or it is not requested. If pathologists are asked to examine histologic sections, a copy of the necropsy report and any images obtained should be requested. Finally, the questions the submitter would like answered should be made clear, preferably in writing. This clarifies goals, averts unrealistic expectations, and prevents oversights.
Radiographs
Obtaining whole-body radiographs prior to necropsy is an easy way of discovering and documenting the presence of metallic objects such as bullets and microchips, as well as bony lesions such as fracture calluses, and has been advocated as a standard practice. 33 Obtaining radiographs before removing the body from the materials it was received in keeps radiological tables clean and ensures that items that may have become dislodged from the body, but are still in the shipping materials, are detected.
The interpretation of radiographs taken prior to presentation of the body to a pathologist should be documented either by the veterinarian who obtained them or by a veterinary radiologist. Interpretation of radiographs obtained by pathologists is limited only by individual experience and comfort but should minimally denote the presence or absence of displaced fractures and radio-opaque foreign material, as is standard practice by forensic pathologists.
Photography
Photographs are a critical and indispensible component of a forensic necropsy. They are used to establish identity and document lesions, and they are frequently submitted as evidence. They are also useful reminders of the necropsy findings for the pathologist preparing for an appearance in court. All photographs should be taken with members of the court and jurors in mind, remembering that these people are unaccustomed to looking at carcasses and that images ruled too graphic can be barred from court. Photographs should be composed, objective images, with minimal gore. It is essential that images be in focus, with the lesion in or near the center of the image, on a clean, plain background, with minimal background distractions such as utensils, equipment, and personnel. Knives, scalpels, and other necropsy instruments have no place in professional photographs. Small lesions can be pointed out with a blunt instrument (such as a scalpel handle) or triangular piece of paper, but it must be clean and not distract from the feature being illustrated.
Generally, at least 2 or more photos of each and every lesion need to be obtained: (1) a distant view, to put the lesion in the context of its surrounding anatomic landmarks, and (2) a close-up for detail. Every photograph should include a scale and case number. For small lesions, where the scale and case number could obscure the area of interest, 2 close-up photographs, one with the scale and case number included and one without, are recommended.
In FP, considerable attention is paid to establishing and confirming identity at the time of autopsy. Although this is less emphasized in VFP, extra care to document identifying qualities of the carcass should be performed. Photographs obtained at necropsy start with the materials in which the body arrived, if sent by mail. Any items accompanying the body, such as blankets, should be documented photographically. Each case should include photographs of the dorsal, ventral, right, and left aspects of the body and the face. Unusual or identifying marks, including tattoos and areas of white coat color on horses, such as collars, should also be photographed.
Courts generally, but not universally, accept digital photography. Original images (files) should be kept on a secure server or transferred to a compact disk and stored in a secure location. Altering or amending copies of images, such as adjusting the contrast and adding arrows and labels, may be permissible in some jurisdictions, as long as the original image is maintained and as long as the content of the image is not altered. It should be noted in the final report that images were obtained at necropsy, or they may not be considered official and therefore barred from court.
The External Examination
A distinguishing feature of forensic necropsies is the importance of the external examination. The external examination serves a number of purposes, including detection of not only lesions but also evidence. A central tenet of forensic sciences is Locard’s exchange principle, which states every contact—such as between a weapon and victim, between a perpetrator and the scene—leaves trace physical evidence (eg, fingerprints, hair, DNA). 41 This trace material is most often deposited on the body rather than within it.
The external examination begins with inspection of the materials in which the body was received. Plastic bags, towels, and blankets in contact with the body should be fully opened and examined for physical evidence such as projectiles, accelerants, and blood from wounds. The examination continues with the body itself and proceeds as a complete physical examination, paying special attention to the nails/claws/hooves, teeth and oral cavity, eyes, ears, perineum, and external genitalia, looking for trace evidence and trauma. For example, inferior and superior oral labial frenulum tears, mandibular symphyseal fractures, nondisplaced hard palate fractures, lingual lacerations, broken teeth, and abraded and avulsed nails may be seen in cats assaulted by people or attacked by dogs.
Diagramming numbered injuries onto simplified drawings of the body or body regions (eg, skull) speeds documentation. They also allow others to quickly grasp the number and location of injuries and, when numbered, find their corresponding description in the written report. They are also a clear, easy way of presenting findings in court and as such are staples of forensic autopsy reports. To be considered part of the official report, diagrams must be dated and signed.
Histology
The major roles of histology in forensic pathology are (1) to confirm, refute, or refine diagnoses made upon gross examination; (2) to be the first line of ancillary diagnostic investigation when necropsy does not reveal the COD; (3) to rule in or out natural, spontaneous disease (eg, pancreatic exocrine insufficiency in cases of emaciated dogs); and (4) to establish a rough age of lesions and the ages of lesions relative to each other. 26 All forensic necropsies should include collection of a full set of fixed tissues, with focused examination of major organs, lesions, and tissues to rule out likely competing differential diagnoses.
Ancillary Tests Unique to Forensic Pathology
Forensic cases may require ancillary testing infrequently employed by veterinary pathologists. A comprehensive review of various tests and their application is outside the scope of this article, but veterinary pathologists should be aware of some of the more common tests employed, such as ballistics (see below), forensic entomology (live insects may be collected, along with specimens fixed in 70% ethanol), 9 accelerant testing (immediately collect and store material or tissue in all-metal airtight containers), and DNA testing (see University of California at Davis’s Veterinary Genetics Laboratory website). 43,52 The potential applications of DNA analysis are virtually limitless and, in cases involving companion animals, have been used to tie suspects to crime scenes and specific dogs to specific bites, identify stolen dogs, and reveal ties between (successfully prosecuted) criminals who, among other illegal activities, engaged in dog fighting. 52 Regardless of the test, contacting the laboratory that will be analyzing the samples to obtain specific recommendations regarding collection and submission is critical.
The Written Report
The format, content, and style of reports currently employed by a veterinary pathologist may be sufficient for use in court for some cases. However, using a format specifically designed for forensic cases, modeled after those used by forensic pathologists and familiar to members of the court, helps ensure the report’s admissibility and increases its utility. Also, by acting as a checklist, a forensic-specific format also helps ensure a complete and thorough documentation of the necropsy.
The exact format and level of detail used by forensic pathologists varies, but it should focus on the description and interpretation of the lesions that contributed to the cause of the death, with minimal space given to incidental lesions. The report should include those attending the necropsy, presentation of the body, postmortem changes/evidence of decomposition, external examination, internal examination, gross description of lesions, COD, and summary. The gross description should contain a listing of major organs and body regions (head, spine, neck), accompanied a description of lesions or absence thereof. Negative findings must be recorded so that it is clear when an organ was either examined and found to be normal or not examined. 51 This degree of documentation is critical as the pathologist may be called to testify weeks, months, or even years after the necropsy. Results of ancillary diagnostic tests, including histologic examination, if any, should also be included in the final report. The summary, the cause, and mechanism of death should be explained in a paragraph format, use laymen’s terms, and employ clear, concise, direct statements, with the court as the intended audience.
Proper forensic pathology terminology should be used. Common terms, including
To determine a COD is to render an opinion. As the degree of certainty will vary from case to case, a scheme of “degrees of certainty” may be used to qualify conclusions:
18
Undetermined (less than 50% certainty) Reasonable medical or investigative probability (50%–70% certainty) Preponderance of medical/investigative evidence (70%–90% certainty) Clear and convincing medical/investigative evidence (90%–99% certainty) Beyond any reasonable doubt (99% certainty) Beyond any doubt (100% certainty)
Use of these terms provides an internal guidepost as to how confident one was while the case was still fresh in the mind; confidence may wane as time passes and court dates approach.
As with any case, before a report is finalized, necropsy photographs should be reviewed to ensure all lesions photographed are described in the report. The report should be double-checked for typographical and clerical errors, preferably by someone other than the person who composed it. Simple mistakes are easy ways for attorneys to call into question a pathologist’s aptitude and ability.
The Forensic Necropsy: Selected Case Types
Cases of alleged companion AAN often fall into one of a few types: trauma, projectile wounds, and neglect and starvation. The goals of the necropsy for each of those case types are briefly considered here.
Traumatic Wounds: Blunt Force Trauma, Lacerations, and Incised Wounds
The objective of the necropsy in cases of trauma is to document the extent of the wounds, determine their relative age and age relative to one another (one incident of trauma vs multiple incidents), and differentiate vital from and postmortem wounds and artifacts.
To identify traumatic lesions in veterinary species, one must conduct a thorough external examination as well as reflect the skin of the entire body, as there is frequently little to no external evidence of blunt-force trauma in many species. 9,51 Shaving/plucking should be considered to aid in the recognition of lesions, as fur and feathers may hide wounds. 51 However, shaving alone will rarely reveal all areas of blunt-force trauma (Figs. 1, 2). The reasons for this are likely due to differences between people and animals in the presence and thickness of pelage, composition and amount of dermal collagen, and dermal vascular supply. These differences also probably account for the rarity of patterned injuries, in which the instrument of blunt-force trauma leaves a contusion or abrasion in the shape of the object (Figs. 3, 4).
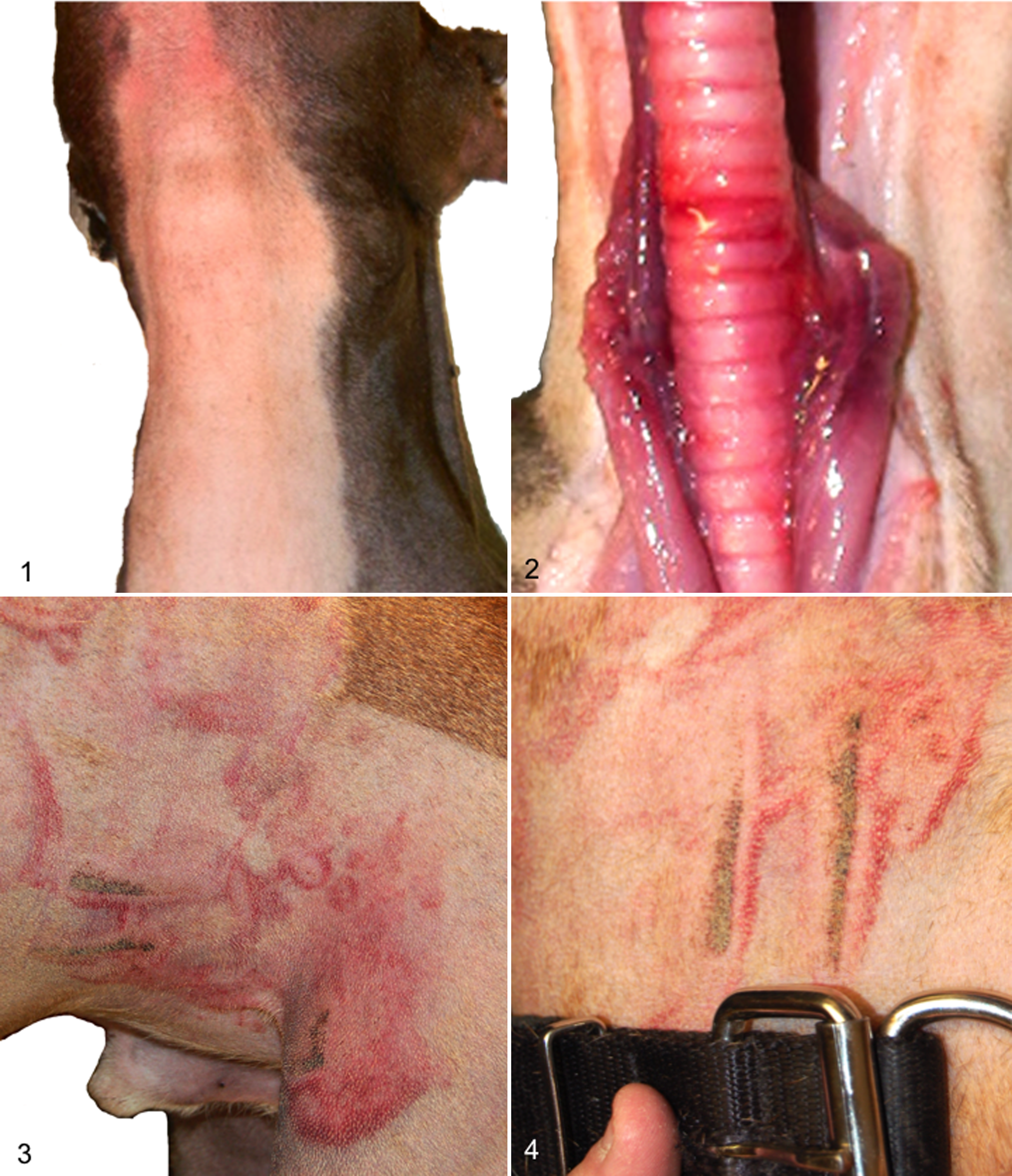
Areas of impact are often apparent only after reflection of the skin and the subcutis, which reveals contusions (bruises). A bruise forms in the vicinity of the impact but may not manifest at the
Blunt trauma may also result in abrasions, in which the epidermis is eroded due to friction or compression upon impact. Antemortem abrasions are red-brown, whereas postmortem abrasions are pale yellow with a translucent “parchment” appearance. 13 Postmortem abrasions are commonly observed on equine carcasses moved after death. Histologic examination of abrasions may be used to roughly estimate their age, based on the general sequence of events of wound healing (hemorrhage, infiltration of leukocytes, and regeneration and fibrosis), and bolstered by species-specific knowledge of infiltrates and processes, where applicable.
A laceration results when tissue is torn by shearing or crushing forces, such as the impact of a blunt instrument or a fall against a hard surface. 13 Skin lacerations are deeper than abrasions, extending into the dermis and often the subcutis. The sine qua non of lacerations is irregular wound margins that are also often abraded and/or bruised. Another unique feature of lacerations is tissue bridging: the presence of intact blood vessels or nerves at the deep aspect of the wound that run from one margin to the other. 13
Lacerations should be differentiated from incised wounds, which have clean, straight margins with no or minimal abrasion and bruising. Incised wounds are produced by sharp or pointed instruments. 13 An incised wound that is deeper than it is long is a stab wound. 13
Almost invariably, pathologists will be asked to differentiate accidental injury from nonaccidental injury. The difficulty of differentiation varies on a case-by-case basis, but aspects of the case history can raise the suspicion of abuse, such as more than 1 fracture of differing ages in the same animal, or a history inconsistent with the nature and severity of the injuries. 32 If the case involves 1 or more fractures, underlying primary or secondary systemic bone disease should be ruled out. 29
Ultimately, despite the fact that studies of the patterns of injures sustained by companion animals in motor vehicle accidents 6,22,40,44,46 and falls from heights 17,49,50 exist, and there is at least 1 report of patterns of nonaccidental injury to domestic cats, 11 studies comparing the nature, distribution, and severity of nonaccidental vs accidental injuries have yet to be made. Thus, the pathologist must rely on the history, experience, postmortem investigation results, and the primary literature available, to attempt to discern the nature of the trauma.
Projectile Wounds: Air Guns, Firearms, and Arrows
The necropsy objectives are to (1) identify the entry wounds and, if present, exit wounds; (2) document the extent of internal injury; (3) recover the projectile(s) if there is no exit wound; and finally, if a firearm was used, (4) determine the direction and range of fire. Reconstructing the exact path of the projectile within the body is a laudable, but not absolutely necessary, goal.
First, survey radiographs are obtained to determine the extent of bony injuries and if a projectile that needs to be recovered is present. 27 After this, projectile wounds on the body are identified by looking and feeling for blood-soaked fur, which, if not still wet, is often “spiked” by clotted blood and dried fluids. If no projectile is seen on radiographs, but an entry or exit wound is found, the corresponding entry/exit wound also needs to be identified. If these cannot be identified on external examination, reflecting the skin and examining the subcuticular side can facilitate the process 9 —or accidentally obscure or destroy wounds if not performed with care. Once identified, avoid probing wound paths, as this tends to create false tracts. 47
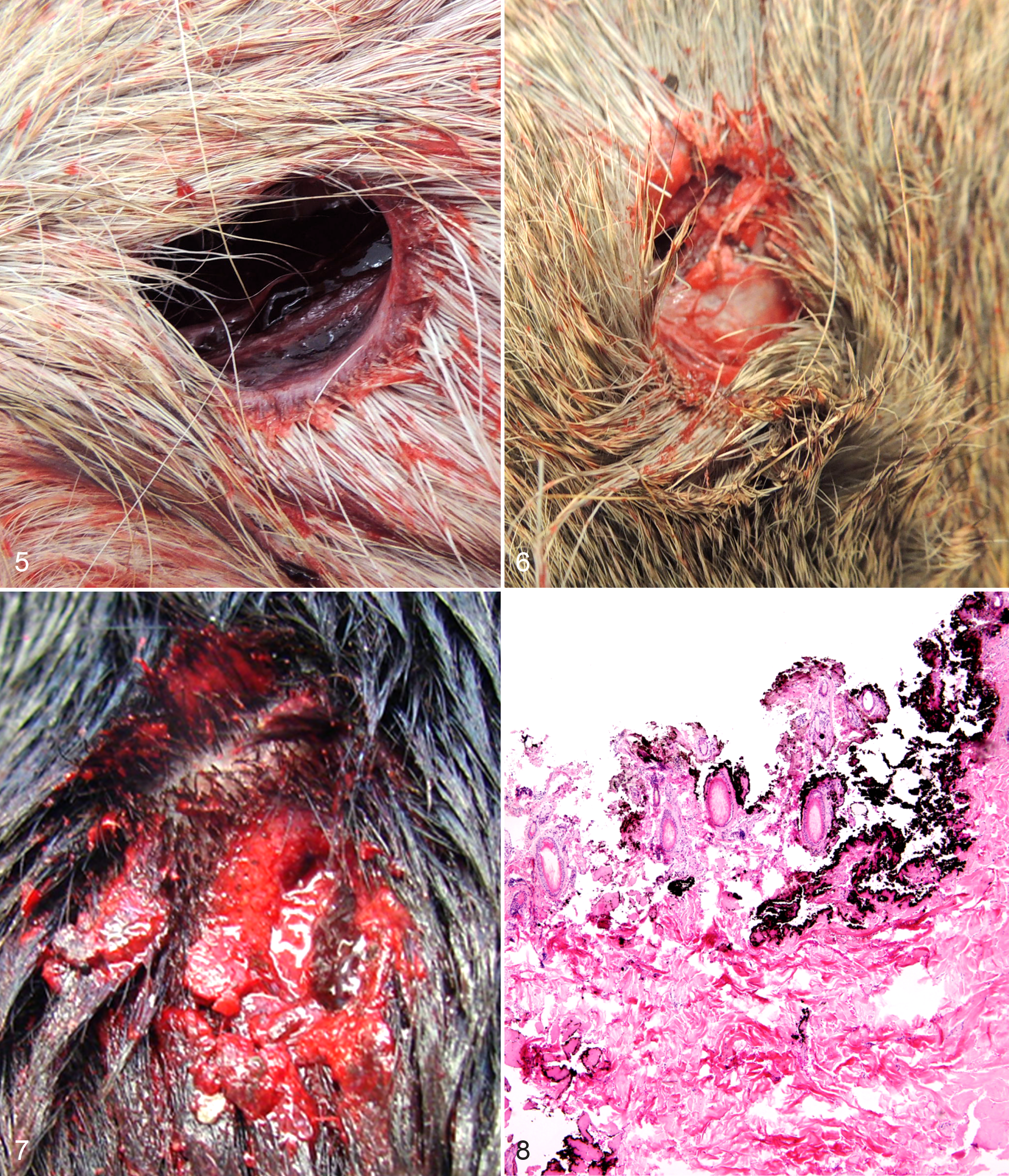
Projectile wounds may be perforating (ie, pass though the body completely) or penetrating, with the projectile coming to rest in the body, where the prosector may recover it. Entry wounds are often characterized by their perfectly circular to oval shape, with finely abraded margins (Fig. 5). Exit wounds may be any shape (round, oval, stellate, crescent, etc), are generally irregular in outline
Differences in entry and exit wounds are the result of projectile tumbling (rotation around the short axis), distortion, and fragmentation as the bullet travels through the body. When the projectile first strikes an object, it is traveling fast and straight, but as it travels through the body, it loses energy and starts to tumble.
14
The most commonly used projectiles have far less energy by the time they exit the body, if they exit at all. Full-metal jacket bullets are one exception to this general rule. The classic entry and exit wound patterns do not apply to entry wounds over bony prominences or to ricocheted projectiles—those that strike the body after striking another surface first.
14
Differentiating entry and exit wounds in these cases can be difficult, but the principle that an exit wound will be larger and more irregular still applies, as the physics are unchanged. Finally, it should be noted that the diameter of skin and soft tissue wounds is
The margins of an entry wound should be closely inspected for beveling of the skin margin—abrasions formed by the projectile rubbing up against the skin at an angle just before it enters the body (Fig. 7). If a projectile strikes the skin perpendicularly, an abrasion margin will either not be appreciable or form a complete ring. Beveling indicates the direction from which the bullet came and, hence, the position of the shooter. 14 This information is critical in affirming or refuting a shooter’s account of events. Often shooters will claim self-defense against an attacking dog, but beveling indicates the dog was shot from the side or behind.
In human cases where a firearm was used (ie, a weapon that uses gunpowder), marks left on the skin by the barrel, hot gasses, and gunpowder can indicate the range from which the animal was shot: contact, close contact, or distant. Soot, which is black and can be wiped off of the skin, is produced by the hot gasses exiting the muzzle and is only seen in contact range, where the firearm is held up against the body when fired. Stippling, in which punctate black spots of unburned gunpowder that cannot be wiped away surround the entrance wound, may be seen in close contact range (<0.6 meters). Other indicators of contact or close range include the presence of wadding in wounds from shotgun injuries. 45 Distant range shots are those greater than 0.6 meters. They leave no gross marks or material in or around the wound, although 66% of human distance range entry wounds contain soot/powder residues in histologic section. 38
Finding soot and stippling on the pelage of animals poses a challenge, and detecting it may be impossible due to the presence of fur and feathers. Close inspection and photography of the entry wound, followed by careful wiping with a white paper towel to determine if soot is present, are recommended. This may be followed by carefully shaving the area to identify any stippling. If there is any question as to the nature of the wound, retaining the shaved hairs for gunpowder residue testing is prudent.
Histologic examination of skin margins surrounding firearm entrance wounds made at contact and close range reveals black granular pigment at the superficial aspect, along with amorphous, hyper-eosinophilic, heat-denatured collagen (Fig. 8). These features can be used to confirm a wound is a bullet entry wound, even in decomposed skin. 12
Air guns, also known as pellet or BB guns, are weapons that propel spherical or mushroom-shaped projectiles using compressed air or gas instead of gunpowder. Because they do not use gunpowder, the distance between the fired weapon and the target cannot be determined from examination of wounds. Identification of entry and exit wounds follows the same principles as with firearms, however.
If a projectile is present in the body, it should be photographed in situ and then removed using the fingers or plastic instruments. Touching projectiles with metal instruments should be avoided, as instruments can ruin microscopic patterns on the bullet, confounding ballistic testing. Generally, only projectiles fired from rifled weapons (handguns, rifles) can be analyzed for ballistic patterns, although some air weapons are rifled. Regardless of the presence or absence of rifling, all projectiles have the potential to be linked back to a perpetrator, and so this type of physical evidence should never be disregarded or discarded. All projectiles should be rinsed, dried, and stored in a paper envelope to prevent corrosion. 43 Collaboration with a specialist in ballistics may be required to identify the specific weapon or type of weapon used, but pathologists must be able to identify and describe the wounds and their role in the death. 10
Arrow wounds are occasionally encountered in companion animals. Modern hunting bows, arrows, and tips are designed to create a linear, fairly narrow, perforating wound, as opposed to projectiles, which often cause an erratic, broad, bruised path of tissue destruction that may or may not perforate the body. 45 Arrow entry wounds are a type of incised wound, with cleanly cut hair at the skin wound margins. Exit wounds also often resemble incisions and are larger than entry wounds. 47 Arrows slice through tissue, whereas projectiles from air guns or firearms tumble, crush, and tear. Although arrows can fracture bones, including long bones, they do not possess the kinetic energy to fracture vertebra and cause breaks with minimal fragmentation, unlike bullets whose high-energy wound channel often contains pulverized grains of bone. 47
Neglect and Starvation
The goal of the necropsy is to document the condition of the body and to rule in or out concurrent disease that accounts for it. Cases of neglect are united by 1 or more of the following physical manifestations of inadequate husbandry: unkempt and/or dirty hair coat, overgrown nails/claws/hooves, dental disease, reduced body condition, and external and/or internal parasitism.
If the hair coat is severely matted, it should be shaved off in as large and complete sections as possible and kept as evidence. It should also be weighed—in some cases, it is a significant proportion of carcass weight. 43 The type and relative number (severity) of external parasites, if present, should also be documented. The skin should be inspected for decubitus ulcers and dermatitis, especially around the perineum. Hooves that are overgrown should be hemi-sectioned and examined for evidence of laminitis, and paw pads of cats and dogs should be checked for ingrown nails. Dental lesions such as missing teeth, fractures, and advanced or abnormal wear should be documented using dental charts. Feces or loops of intestine should be submitted for qualitative and quantitative parasite analysis, even if parasites are not grossly evident.
In many cases of neglect, the body condition—the amount of adipose and skeletal muscle—is markedly reduced. Extreme reduction in body condition results in emaciation. Terms to describe this state and the mechanisms responsible for it abound, with overlapping and inconsistent lay, medical, nutritional, and forensic definitions.
29
The term
Causes of NEB may be divided into those that are exogenous and endogenous. These correspond to the terms (1)
When disease that could account for an emaciated state is not found by the necropsy, the cause of death is starvation. 28 To avoid confusion, the report should also clearly state that a necropsy can only be used to rule out endogenous causes of starvation and cannot be used to prove exogenous causes, circumstances, or intent, such as out-competition for food by cohorts or willful withholding of food. These require additional information, including the animal’s environment (the scene) and reported feeding practices.
An accurate, objective, and descriptive assessment of body condition, specifically the location and relative amount of adipose, is critical in cases of undernutrition. Loss of body condition results from the loss of subcuticular and visceral adipose tissue and atrophy of skeletal muscle. Body condition scores are a semi-quantitative assessment of body composition, especially percent body fat and muscle. For consistency and clarity, a published body condition scoring system should be used and cited. A 1 to 9 scoring system for dogs and cats has been shown to be repeatable within observers and consistent between observers, and in addition, the body composition estimated by these scoring systems has been validated with dual-energy x-ray absorptiometry. 23,24 In all cases, and especially if a published scale is not available for a given species, a thorough photographic documentation and description should be made of the visibility and palpability of bony prominences on external examination.
On internal examination, the relative amount of adipose and/or serous atrophied fat in the omentum, perirenal area, epicardium, and bone marrow should be documented, as these are sites from which internal fat reserves are used. The gastrointestinal tract should be opened along its entire length, and the gastric contents should be closely examined (a sieve aids this step), photographed, and a portion frozen for possible subsequent testing. The relative amount (abundant, adequate, or scant), nature, and quality of the digesta (kibble, table scraps, sand, etc) and any foreign objects should be noted in the report.
In many domestic animals, bone marrow is the last anatomic location to undergo serous atrophy of fat, 3,25,42 and in people, serous atrophy of marrow adipocytes has been shown to correlate with extreme weight loss as well as leukopenia. 1,48 The percentage of bone marrow fat may be quantified for recently deceased (<24 hours) horses, cattle, dogs, pigs, cervids, and sheep by submitting an entire intact femur for analysis to the Purdue Animal Disease Diagnostic laboratory. This test might also be useful in bovine and equine cases with a postmortem interval (PMI) of 30 to 60 days, 25 but the test has not been validated for other species with PMIs greater than 24 hours. Given the range of possible PMIs, ambient temperatures, and environments (exposed, buried, soil acidity, etc), the results of this test might not be sound in a forensic context. Finally, although multiorgan atrophy is common and well documented in malnourished people, 28 and there are scattered reports of starvation-associated liver atrophy for a variety of vertebrates, 29 organ weights as they relate to body condition or adipose stores appear not to have been used in a forensic context.
The ideal body weight of the animal should be estimated and the difference between it and the actual carcass weight noted in the report. 28 In people, a loss of 35% to 50% of ideal body weight may cause death. 28 The suspected mechanisms of death in starved people include ventricular arrhythmias due to presumptive electrolyte depletion/imbalances, infections resulting from compromised immunity, and/or sepsis due to loss of barrier function of the skin or gastrointestinal (GI) tract. 28 These mechanisms, especially GI epithelial barrier breakdown, may occur in animals as well, as gastric erosions associated with mild to marked melena are a frequent finding in emaciated dogs (personal observation). There is also experimental evidence indicating GI immunity compromise in starved rodents. 16,20
Questions regarding the duration and/or severity of undernutrition are inevitably asked, and an estimate should be reported, 28 based on experience and published data where possible. Alternatively, estimations may be sought from those with additional species/breed-specific experience or expertise. For a variety of reasons, most notably ethical concerns, few studies in any species have examined rates of weight loss over the period required to reduce a healthy body condition to an emaciated state. Information regarding the caloric needs of many species for a variety of physiologic states (eg, lactation) in a laboratory setting has been published, 35,36 but correlations between rate of weight loss and caloric deficit, even in a laboratory setting, have not been well studied for companion animals, and applying this information to individual cases from nonlaboratory settings is fraught with difficultly. Minimally, what can and should be said for an individual animal is that caloric intake either was or was not adequate to maintain a healthy body condition and that disease either does or does not account for the emaciated state.
Veterinary Forensic Pathology: Future Directions
Over the past 75 years, the breadth, depth, and sophistication of veterinary pathology have grown immensely. The field of veterinary forensic pathology has expanded rapidly over the past decade, and continued growth is expected; the public has not lost interest in prosecuting offenders of violent crimes committed against animals. In addition, the field of forensic pathology as a whole is also entering a new era, with reevaluation of old assumptions and exploration of molecular techniques.
Veterinary pathologists have the opportunity to act as leaders in this rapidly developing and highly visible field and see it mature into a more robust science through the publication of case reports, retrospective analyses, and original research. This growth could be further fostered by the creation of forums for interested veterinary pathologists to collaborate and consult with each other, as well as active participation by veterinary pathologists in organizations such as the International Veterinary Forensic Science Association, the Society for Wildlife Forensic Science, the American Academy of Forensic Sciences, and the International Association of Forensic Sciences. Recently, there have been a number of presentations in the field of VFP at national and international meetings, including the 2011 C. L. Davis/ACVP Symposium on Forensic Veterinary Pathology, the 2011 American Academy of Forensic Sciences Conference, the 2011 European Veterinary Conference Voorjaarsdagen (Holland), and the 2011 MedVep (Revista Científica de Medicina Veterinária; Brazil).
Perhaps in the future, veterinary pathologists will act as forensic pathologists and become involved in investigations, starting with inspection of the body at the scene, to the necropsy, through ancillary testing and into the courtroom. This integrated approach ensures the best understanding and accurate interpretation of lesions possible. Currently, a common arrangement is for the scene investigation and/or necropsy to be completed by a forensic veterinarian, with involvement of the veterinary pathologist for necropsy or histopathology alone. This is a suboptimal arrangement, but it is the current state of affairs, and its shortcomings are at least partially ameliorated if reports and photographs of the scene and necropsy are provided to the veterinary pathologist.
A significant advantage of partnerships between forensic veterinarians and veterinary pathologists is that forensic veterinarians often have intimate knowledge of the kinds of environments from which forensic cases originate. For instance, they can warn pathologists that a body seized from illicit drug labs may be contaminated with noxious gases or caustic compounds. Injuries to horses used in illegal rodeos may produce distinct traumatic lesions unfamiliar to veterinary pathologists but pathognomonic to forensic veterinarians. Coupling this specialized knowledge with pathologists’ training and skills yields high-quality results.
This review is not meant to be regarded as authoritative or to establish standards of practice. No such standards exist yet, nor could they, as legal precedent in the VFP field is limited and often inconsistent. Veterinary pathologists’ experience will vary significantly with geography, jurisdiction, and individual cases. However, the guidelines outlined here represent the combined experience of veterinarians, pathologists, and lawyers with extensive experience in this nascent field.
We hope that this review will increase the aptitude and confidence of veterinary pathologists handling forensic cases. Veterinary forensic pathology is neither rocket science nor routine, but any pathologist who is aware of the needs of the courts and willing to modify his or her practice to meet those needs may conduct a proper forensic necropsy. These cases can be costly in time and energy, but the rewards in personal satisfaction, service to the community, and contribution to the welfare of people and animals are far greater.
Footnotes
Acknowledgements
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
