Abstract
This report describes the clinicopathological features of a case of diffuse scaling dermatitis that occurred in a 16-week-old female athymic nude (CrTac:NCr-Foxn1nu ) mouse. Gross presentation was suggestive of Corynebacterium bovis infection (scaly skin disease). However, C. bovis was not isolated from the skin of the affected animal or from the skin of unaffected CrTac:NCr-Foxn1nu mice housed in the same cage or room. Staphylococcus xylosus was instead isolated in high numbers from the skin lesion, whereas only a few colonies were recovered from the skin of unaffected mice. Microscopically, the affected skin was characterized by chronic hyperplastic and hyperkeratotic dermatitis with focal ulcerations, extensive serocellular crusts, and intralesional clusters of Gram-positive coccoid bacteria. Although gross presentation of the reported case was suggestive of C. bovis infection, epidemiological, histopathological, and bacteriological findings definitively ruled out an outbreak of scaly skin disease. A diagnostic hypothesis of hyperplastic and hyperkeratotic dermatitis associated with opportunistic S. xylosus infection was formulated based on increased bacterial burden and presence of intralesional Gram-positive coccoid bacteria.
Background
Scaly skin disease, also referred to as hyperkeratotic dermatitis or coryneform hyperkeratosis, is an infectious condition of mice caused by Corynebacterium bovis and characterized by diffuse scaling dermatitis. 7,9,11 Microscopically, skin lesions are characterized by marked acanthosis, orthokeratotic hyperkeratosis, and sparse granulocytic and mononuclear cell infiltrate in the underlying dermis. 7,9,11 Immunodeficiency and hairlessness have been demonstrated to be the 2 major predisposing factors for the development of this condition. In this context, spontaneous outbreaks of overt clinical disease, usually characterized by high morbidity and low mortality, mainly affect athymic nude (Foxn1nu ) mice and, to a lesser extent, hirsute SCID (Pkrdcscid ) and hairless SKH1-Hrh r mice. 7,9,11
Severe outbreaks of scaly skin disease in athymic nude mice have been described in northern Italy during the 1990s. 9 Several mouse facilities, belonging both to private pharmaceutical companies and institutes of biomedical research, were concurrently involved. These outbreaks posed a serious hazard mainly for the consequences of the infection on the pathobiology of the numerous xenotrasplant models used in preclinical studies (ie, increased toxicity of chemotherapeutic agents and decreased tumor growth). 7,11 This critical situation prompted the affected facilities to adopt, in concert with the companies supplying the athymic nude mice, drastic but successful measures of eradication and strict surveillance procedures. 9 A high level of attention is still present in many facilities in northern Italy despite no further recorded outbreaks of scaly skin disease since 1996. In these facilities, athymic nude and SCID mice presenting with scaly skin lesions are routinely processed for histopathology and bacteriology to rule out a possible implication of C. bovis.
History and Gross Findings
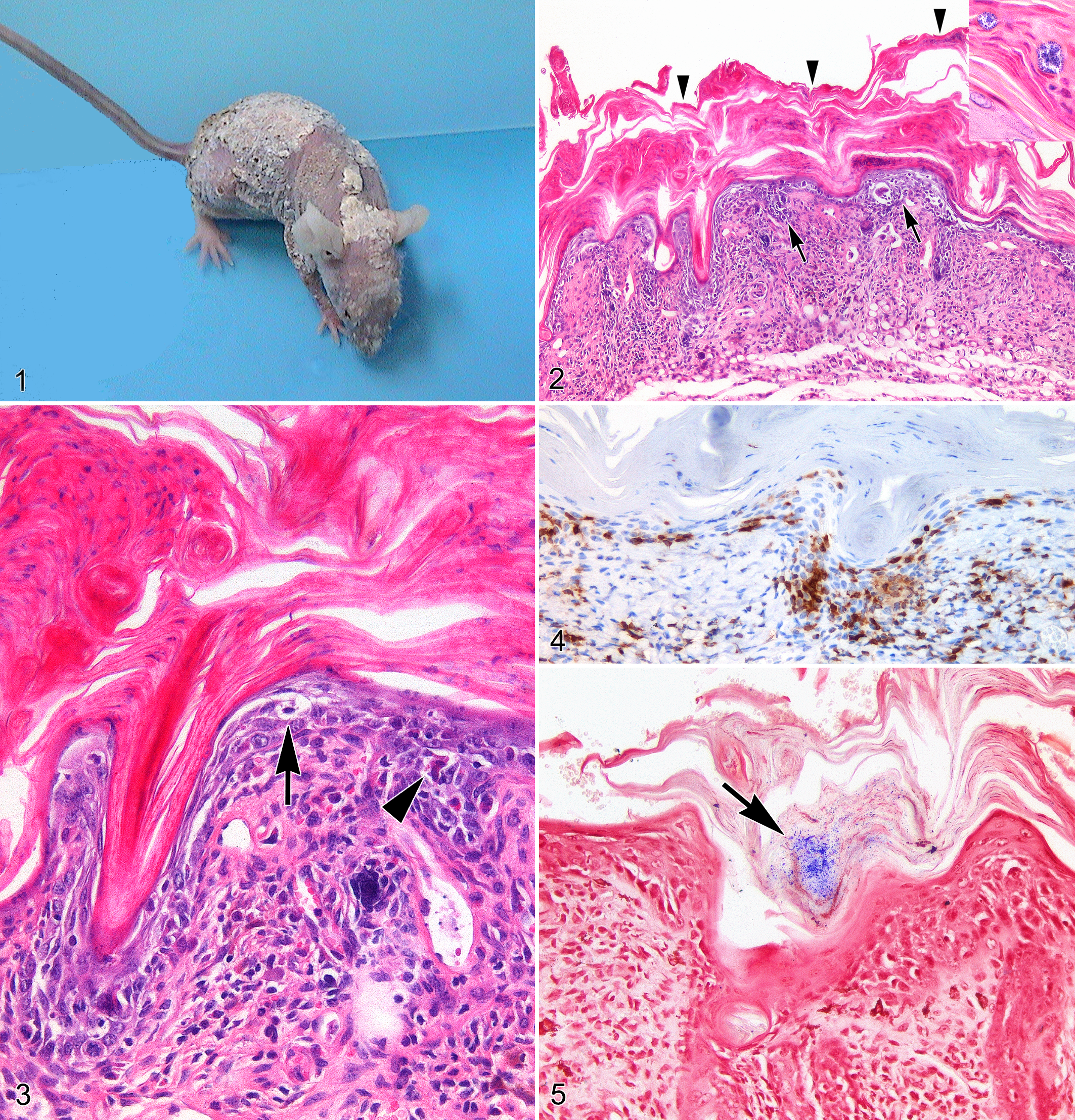
A 16-week-old female CrTac:NCr-Foxn1nu mouse was referred because of the progressive development of diffuse scaling dermatitis. Grossly, the affected skin was covered by variable-sized adherent keratin flakes. Lesions were first observed along the dorsum and then, within a week, progressively spread to involve the entire epidermal surface (Fig. 1). With the progression of skin lesions, the mouse also showed a relevant body weight loss (>20%), hunched posture, and labored breathing. All the other mice housed in the same facility appeared clinically healthy.
Bacteriological examination was performed as described elsewhere 9 on samples collected from representative skin areas (ie, dorsal, axillary, and interscapular region) of 6 CrTac:NCr-Foxn1nu mice, including the mouse with scaling dermatitis, a cagemate, and 4 females randomly selected from the same room. All these mice were then sacrificed by CO2 inhalation followed by cervical dislocation. A complete necropsy was performed on the mouse with scaling dermatitis, and representative samples of skin lesions, salivary glands, thyroid, lungs, heart, liver, spleen, kidneys, pancreas, stomach, small intestine, large intestine, gonads, genital tract, urinary bladder, cervical and mesenteric lymph nodes, brain, sternum, and vertebrae with bone marrow were collected in 10% neutral buffered formalin and routinely processed for histological evaluation with hematoxylin and eosin (HE) stain. Serial sections from skin lesions were stained with the Gram and Periodic Acid Schiff (PAS) method and immunostained for CD3 and CD45R/B220 as previously described. 3,8 Histology with HE, Gram, and PAS stain was also performed on representative samples of dorsal skin collected from the other 5 unaffected CrTac:NCr-Foxn1nu mice housed in the same cage or room.
All the mice analyzed in the present study were part of a SPF barriered facility housing approximately 5000 athymic nude (including both CrTac:NCr-Foxn1nu and Crl:NU-Foxn1nu strains) and 1000 SCID (including both CB17/Icr-Prkdcscid /IcrCrl and IcrTac:ICR-Prkdcscid strains) mice. The facility was included in a health monitoring program developed in accordance with Federation of European Laboratory Animal Science Associations (FELASA) guidelines and tested negative for ecto- and endo-parasites and for the following viruses and bacteria: ectromelia virus, lymphocytic choriomeningitis virus, minute virus of mice, mouse adenovirus type 1 (MAd FL), mouse adenovirus type 2 (MAd K87), mouse cytomegalovirus, mouse hepatitis virus, mouse norovirus, mouse parvovirus, mouse rotavirus (EDIM), pneumonia virus of mice, reovirus type 3, Sendai virus, Theiler’s murine encephalomyelitis virus, Clostridium piliforme, Bordetella bronchiseptica, Citrobacter rodentium, Corynebacterium kutscheri, Mycoplasma spp, Pasteurella spp, Salmonella spp, Streptobacillus moniliformis, β-hemolytic streptococci, and Streptococcus pneumoniae. The colony tested positive for Helicobacter rodentium.
Experiments involving animals have been performed in accordance with the Italian Laws (D.L.vo 116/92 and following additions), which enforce EU 86/609 Directive (Council Directive 86/609/EEC of November 24, 1986, on the approximation of laws, regulations, and administrative provisions of the member states regarding the protection of animals used for experimental and other scientific purposes).
Differential Diagnoses
The main differential diagnoses that need to be considered in cases of diffuse scaling dermatitis affecting athymic nude mice are (1) scaly skin disease caused by C. bovis infection, (2) hyperkeratotic skin conditions associated with low environmental humidity, and (3) hyperkeratotic dermatitis associated with severe infections by opportunistic bacteria, as suggested by anecdotal reports. 7
Bacteriological and Microscopic Findings
A high number of Staphylococcus colonies (colony-forming units [CFU] >250), identified as Staphylococcus xylosus by the API-STAPH assay (bio-Merieux sa, Marcy l’Etoile, France), were recovered from the skin of the mouse with scaling dermatitis. A few colonies (CFU <10) of coryneform bacteria were recovered from the same mouse and further identified with the API Coryne (bio-Merieux sa) as Corynebacterium urealyticum and Corynebacterium pseudodiftericum. A few colonies (CFU <10) of both S. xylosus and C. pseudodiftericum were also recovered from the skin of unaffected CrTac:NCr-Foxn1nu mice housed in the same cage or room. Bacteriologically, none of the examined mice tested positive for C. bovis.
Microscopically, the skin of the mouse with scaling dermatitis was diffusely thickened, displaying marked, both interfollicular and infundibular, regular epidermal hyperplasia. Affected epidermis also exhibited diffuse orthokeratotic and, to a lesser extent, parakeratotic hyperkeratosis accompanied by extensive serocellular crusts (Fig. 2). Small foci of full-thickness epidermal necrosis/ulceration with massive neutrophilic infiltration of the subjacent dermis were sporadically observed. Neutrophilic exocytosis with small subcorneal pustule formation was prominent in the hyperplastic epidermis bordering areas of ulceration. Inflammatory changes in nonulcerated areas were characterized by cell-poor infiltrates of lymphocytes diffusely obscuring the interfollicular and infundibular dermo-epidermal junction with multifocal hydropic degeneration of basal keratinocytes (Fig. 3). Immunohistochemically, dermo-epidermal lymphocytic infiltrates were mainly composed of CD3-positive T cells (Fig. 4), whereas only a few CD45R/B220-positive B cells were observed. Clusters (1–2 μm in diameter) of Gram-positive coccoid bacteria were scattered among serocellular crusts (Figs. 2 and 5). The following additional findings were also occasionally noticed within the hyperplastic epidermis: spongiosis/reticular degeneration, single keratinocyte apoptosis/necrosis, and suprabasal epidermal clefting. None of the other organs/tissues sampled from this mouse showed relevant microscopic changes. Microscopically, skin samples obtained from clinically unaffected mice were unremarkable. In all the examined cases, PAS staining invariably failed to identify fungal organisms. After this case, no cutaneous lesions reminiscent of scaly skin disease were observed in any of the mice housed in the facility.
Diagnosis
Based on the above findings, a diagnostic hypothesis of diffuse chronic hyperplastic and hyperkeratotic dermatitis associated with an opportunistic skin infection caused by S. xylosus was formulated.
Discussion
Although the gross presentation of the reported case was suggestive of scaly skin disease, the epidemiological, clinical, histopathological, and bacteriological findings definitively ruled out an outbreak of C. bovis infection. The epidemiology of scaly skin disease in nude mice is characterized by high morbidity and low mortality rates. 7,9 Description of spontaneous outbreaks and transmission experiments clearly demonstrated the highly contagious nature of this condition. After its entry into a naive facility, C. bovis infection is readily transmitted among susceptible animals by direct contact and fomites with an incidence of nearly 100%. Once established, C. bovis infection tends to be persistent, but skin lesions spontaneously resolve within a few days and generally do not recur in animals that have recovered. 7,9,11 In addition, nude mice suffering from scaly skin disease typically do not show any sign of systemic illness. 7,9,11 All these aspects are in contrast with the severe but sporadic nature of the infectious skin condition described in this study. Scaling dermatitis occurred only in a single animal and was accompanied by progressive deterioration of the general clinical condition, possibly reflecting systemic repercussion of skin inflammation. In addition, the microscopic skin lesions described here include changes, such as parakeratotic hyperkeratosis, foci of full-thickness epidermal necrosis/ulceration, and subcorneal pustules formation, which are not typically observed during scaly skin disease. 7,9,11
Likewise, the hypothesis that skin lesions may have been caused by low environmental humidity appears unlikely for a series of reasons: (1) no alterations of the standard housing conditions were reported, (2) alterations in standard housing conditions resulting in low environmental humidity should have equally affected all the mice maintained under the same ventilation system/unit, and (3) epidermal hyperkeratosis associated with low environmental humidity is primarily described as a noninflammatory condition.
S. xylosus was isolated in high numbers from the skin lesions of the affected mouse, whereas only a few colonies were recovered from the skin of the unaffected animals housed in the same cage and room. S. xylosus is typically reported as a nonpathogenic commensal bacterium that commonly inhabits the skin and mucous membranes of a variety of mammals, including the mouse. 1,5,7 Reports of S. xylosus as a cause of opportunistic infection of mouse skin are limited to a few episodes of necrotizing and ulcerative dermatitis all involving immunocompromised hosts. 1,5,7 S. xylosus has never been implicated before in the development of diffuse hyperplastic and hyperkeratotic dermatitis grossly resembling scaly skin disease. Nevertheless, the increased bacterial burden and the presence of numerous clusters of Gram-positive coccoid bacteria in the serocellular crusts support the hypothesis that S. xylosus may be actually associated with the episode of scaling dermatitis reported here.
This work and previous descriptions of S. xylosus dermatitis in athymic nude mice suggest that infections caused by this opportunistic bacterium are associated with severe and often fatal systemic signs of disease despite the lesions being confined to the skin. 1 As already hypothesized by Bradfield and colleagues, 1 the implication of S. xylosus–derived toxins may in part explain the systemic clinical repercussions resulting from skin infections. In particular, the well-documented ability of coagulase-negative staphylococci (including S. xylosus) to produce a vast array of superantigen toxins (SAgs) should be taken into account as these molecules play a pivotal role in the induction of an acute and often fatal systemic clinical condition commonly referred to as toxic shock syndrome (TSS). 6 Nonspecific polyclonal activation of T cells by SAgs is central to the pathogenesis of TSS. 2 CrTac:NCr-Foxn1nu mice (as well as all other stains of mice homozygous for the Foxn1nu mutation) completely lack thymus and therefore are T cell deficient. Nevertheless, extrathymic T-cell maturation is commonly observed in athymic nude mice, especially when they are exposed to infections. 10 In this context, the demonstration of a dense population of CD3-positive lymphocytes infiltrating skin lesions supports the assumption that S. xylosus–derived SAgs may have contributed to the severe manifestations of systemic disease described in this report. Diffuse dermatitis with impairment of the epidermal barrier resulting in transepidermal fluid loss and consequent dehydration should also be considered among the possible concurrent causes of the clinical manifestations observed.
Few colonies of coryneform bacteria different from C. bovis (C. urealyticum and C. pseudodiftericum) were recovered from all the animals tested. Various species of coryneform bacteria such as Corynebacterium group G1, Corynebacterium group ANF, Rhodococcus equi, Corynebacterium jeikeium, and Corynebacterium minutissimum are often isolated from the skin of athymic nude mice without signs of dermatitis and are considered commensal organisms unable to generate opportunistic infections. 4 Based on this nonpathogenic nature, it is unlikely that C. urealyticum and C. pseudodiftericum have contributed to the development of the skin lesions described in this report.
In the reported case, it was not possible to achieve a definitive diagnosis since Koch’s postulates generally do not apply to opportunistic pathogens, making it difficult to determine the actual etiopathogenetic role of S. xylosus in the development of the clinicopathological entity observed. 11 The demonstration of SAgs production by the colonies of S. xylosus recovered from the skin lesions may have further supported the hypothesis that bacteria-derived toxins are actually implicated. In a previous study, the pathogenicity of specific mouse isolates of S. xylosus recovered from skin lesions of athymic nude mice was tested via intradermal inoculation of pure cultures in syngeneic animals. 1 These experiments did not completely reproduce the disease, indicating that beside immunodeficiency and defects in the epidermal barrier, other predisposing factors contribute to promote the pathogenicity of S. xylosus in athymic nude mice.
There have been anecdotal reports of hyperkeratotic dermatitis in athymic nude mice associated with severe infections by opportunistic bacteria. 7 However, these associations have never been documented by published studies. Although final conclusions cannot be drawn by the description of a single case, the present work suggests that opportunistic S. xylosus infection in athymic nude mice may have a role in the development of skin lesions resembling scaly skin disease.
Footnotes
Acknowledgements
We gratefully acknowledge Silvia Grassi (IZSLER, Sezione di Milano) and Marco Brevi (DIPAV, School of Veterinary Medicine, Università degli Studi di Milano) for technical assistance.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
