Abstract
Objective
This study aimed to assess the prevalence and associated factors of male sexual dysfunction in a population of young men using validated tools to evaluate erectile function and its contributing factors.
Methods
A community-based cross-sectional study was conducted between April 2023 and August 2024 among married men aged ≤40 years in Saudi Arabia. Participants were randomly selected from public gatherings across five regions and interviewed using the International Index of Erectile Function and Sexual Health Inventory for Men. Sociodemographic and clinical data were collected, including comorbidities, body mass index, physical activity, income, educational level, job, and depression screening result. Statistical analyses included descriptive statistics, nonparametric tests, and multivariable linear regression to identify factors associated with erectile dysfunction.
Results
A total of 196 men participated in the study. Of these, 77 (39.2%) were diagnosed with erectile dysfunction. According to the Sexual Health Inventory for Men score categories, 119 (60.7%) men had no significant erectile dysfunction, 29 (14.8%) had mild erectile dysfunction, 19 (9.7%) had mild-to-moderate erectile dysfunction, 15 (7.6%) had moderate erectile dysfunction, and 14 (7.14%) had severe erectile dysfunction. Multivariable linear regression analysis revealed several significant associated factors for better erectile function (based on the International Index of Erectile Function score), namely, higher income and an initial negative screening result for depression. The International Index of Erectile Function score was 12.65 points (95% confidence interval: −17.37 to −7.92; p < 0.0001) lower in participants with an initial positive screening result for depression than in those with an initial negative screening result for depression.
Conclusions
These results suggest that sexual dysfunction in younger men is not only influenced by physical health but also closely linked to psychosocial factors such as low income and depression. Further longitudinal research and multidisciplinary approaches are required to develop comprehensive targeted interventions for sexual dysfunction in young men, with an emphasis on mental health and socioeconomic conditions.
Introduction
Male sexual function consists of several domains, including desire, orgasm, ejaculation, and erectile function. 1 These domains operate differently through interactions with neuronal, hormonal, and vascular physiological factors. These functions can be pathologically impaired by various disease processes, including diabetes mellitus, atherosclerotic vascular disease, neurological disorders, and emerging factors such as obstructive sleep apnea. 2 The prevalence of male sexual dysfunction increases with aging, and it is a common complaint among older men. 3 Globally, studies have reported that up to 30% of men aged <40 years experience some form of sexual dysfunction, most commonly erectile dysfunction (ED) and reduced sexual desire. 3 In Middle Eastern societies, the true burden may be under-recognized due to sociocultural stigmas that limit open discussion. 4 Sexual dysfunction can adversely affect quality of life and might negatively affect men’s well-being and hence partner relationships. 5
Although sexual dysfunction is well-studied in older men, its prevalence, severity, and psychosocial impact among young men, particularly in Saudi Arabia, remain underreported. Moreover, there are no specific guidelines to manage sexual dysfunction in this population. Although a few studies have examined the prevalence and etiological factors of sexual dysfunction in young men, 6 most have not addressed the risk factors with a detailed analysis to identify associated risk factors. Despite improvement in the diagnostic workup and management options among the older age group, there has been a lack of data and guidance for the management of sexual dysfunction in young males as well as the evaluation of psychosocial and organic factors in both partners. In the current report, we present a detailed analysis of the prevalence and associated factors of sexual dysfunction among young men with the aim of exploring other contributing factors in Saudi Arabia as well as a detailed analysis of all sexual domains.
Material and methods
Study population and data collection
Institutional ethical review board approval was obtained in accordance with the Declaration of Helsinki 1975, as revised in 2024. A community-based cross-sectional study was conducted based on an interview utilizing the International Index of Erectile Function (IIEF). It is psychometrically effective and has been linguistically validated in different languages, including Arabic. It is readily self-administered in research or clinical situations.7,8 The participants were randomly sampled from public gatherings in five different regions of Saudi Arabia after providing consent to participate in the survey between April 2023 and August 2024. The sample size was determined based on feasibility and expected response rates, aiming to capture sufficient variability in sexual function among young married men. Although no formal power calculation was performed, a minimum sample size of 190 participants was considered to allow for subgroup analysis and multivariable modeling with adequate statistical precision. All participant data were fully deidentified to ensure anonymity and prevent any possibility of individual identification. The inclusion criteria were age ≤40 years, male sex, and currently married, as it is impossible to assess sexual function based on masturbation. After an individual agreed to participate with an informed electronic consent, he was interviewed by the medical staff members trained to administer the IIEF, who were available to explain the questions to the participants if needed. After providing consent, the participants completed the electronic survey by themselves to maintain the confidentiality of data. The reporting of this study conforms to the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines. 9
Outcome measures
The primary outcome was the IIEF score. This questionnaire comprises 15 items that examine the 5 main domains of male sexual function: erectile function, orgasmic function, sexual desire, intercourse satisfaction, and overall satisfaction. Each question is answered on a scale from 0 to 5. Additionally, the outcome of ED severity was assessed using the Sexual Health Inventory for Men (SHIM), an abridged and slightly modified 5-item version of the IIEF.
Covariates
Current age was categorized based on the median age of the sample (36 years). The body mass index (BMI) was categorized as ≤28 kg/m2 and >28 kg/m2, defined based on the median cutoff point. The Charlson Comorbidity Index (CCI) was categorized based on no comorbidities and ≥1 comorbidity. Educational level was categorized into three groups: high school, bachelor’s degree, and higher education. Occupation was categorized into three groups: unemployed, employed with a nonmilitary job, and employed by the military. Income was categorized into five groups. Physical activity was defined as any regular activity performed for more than 30 min per session, three times a week. Two simple questions were used to rule out depression; a positive screening result is indicated by the person answering “yes” to one or both questions, as recommended by the National Institute for Health and Care Excellence (NICE). 10 It is known as Patient Health Questionnaire (PHQ)-2, which demonstrates suitable sensitivity in identifying individuals with major depressive disorder. It is considered a valuable tool for primary healthcare settings due to its effective screening modality, and it is used in our clinical practice when evaluating patients initially for ED. 10 Smoking was categorized into three groups: nonsmoker, active smoker, and ex-smoker. Finally, prostate disease was defined as the presence of pelvic pain syndrome or lower urinary tract symptoms over the past 4 weeks, with a positive selective urine test and/or prostatic secretion culture, as reported by the study participants.
Statistical analysis
Descriptive statistics were used to report the baseline characteristics and proportions of the studied risk factors. Quantitative variables such as age, BMI, and IIEF scores were initially assessed for normality using visual inspection and distribution statistics. As most continuous variables were not normally distributed, they were summarized using medians and interquartile ranges and analyzed using nonparametric tests (Mann–Whitney U and Kruskal–Wallis H tests). For linear regression analysis, continuous variables were categorized based on the median cutoff points or clinically relevant thresholds to facilitate the interpretation of associations with odds ratios and 95% confidence intervals (CIs) and to control for confounding variables. All statistical tests were performed using STATA software version 17 (Stata Corp LP, College Station, TX, USA). All tests were two-sided with a significance level set at p < 0.05.
Results
A total of 196 participants aged ≤40 years completed the survey. Of these, 77 (39.2%) had ED based on the SHIM score. Based on the SHIM score categories, 119 participants (60.7%) had no significant ED, 29 (14.8%) had mild ED, 19 (9.7%) had mild-to-moderate ED, 15 (7.6%) had moderate ED, and 14 (7.14%) had severe ED. Furthermore, the maximum IIEF score was 75, with higher scores indicating better overall sexual function across five domains. In this study, a mean IIEF score of 59.1 ± 16.4 reflects moderate impairment in at least one or more domains. Figure 1 shows the percentage of study participants with at least a one-point loss in the five domains of the IIEF.

The percentage of study participants with at least a 1-point loss in the five domains of the International Index of Erectile Function.
Table 1 shows the stratified baseline characteristics of the study variables based on the mean IIEF and SHIM scores. Factors associated with adverse erectile function among the participants included a lower income, ≥1 comorbidity based on the CCI, initial positive screening result for depression, and being unemployed (p < 0.05). Table 2 shows the study variables stratified based on the sexual domains of the IIEF. Interestingly, BMI showed no significant association with sexual function across all domains. Moreover, prostatitis/pelvic pain syndrome adversely affected sexual desire (p = 0.01).
Stratified baseline characteristics of the study variables with mean results of the IIEF and SHIM scores.
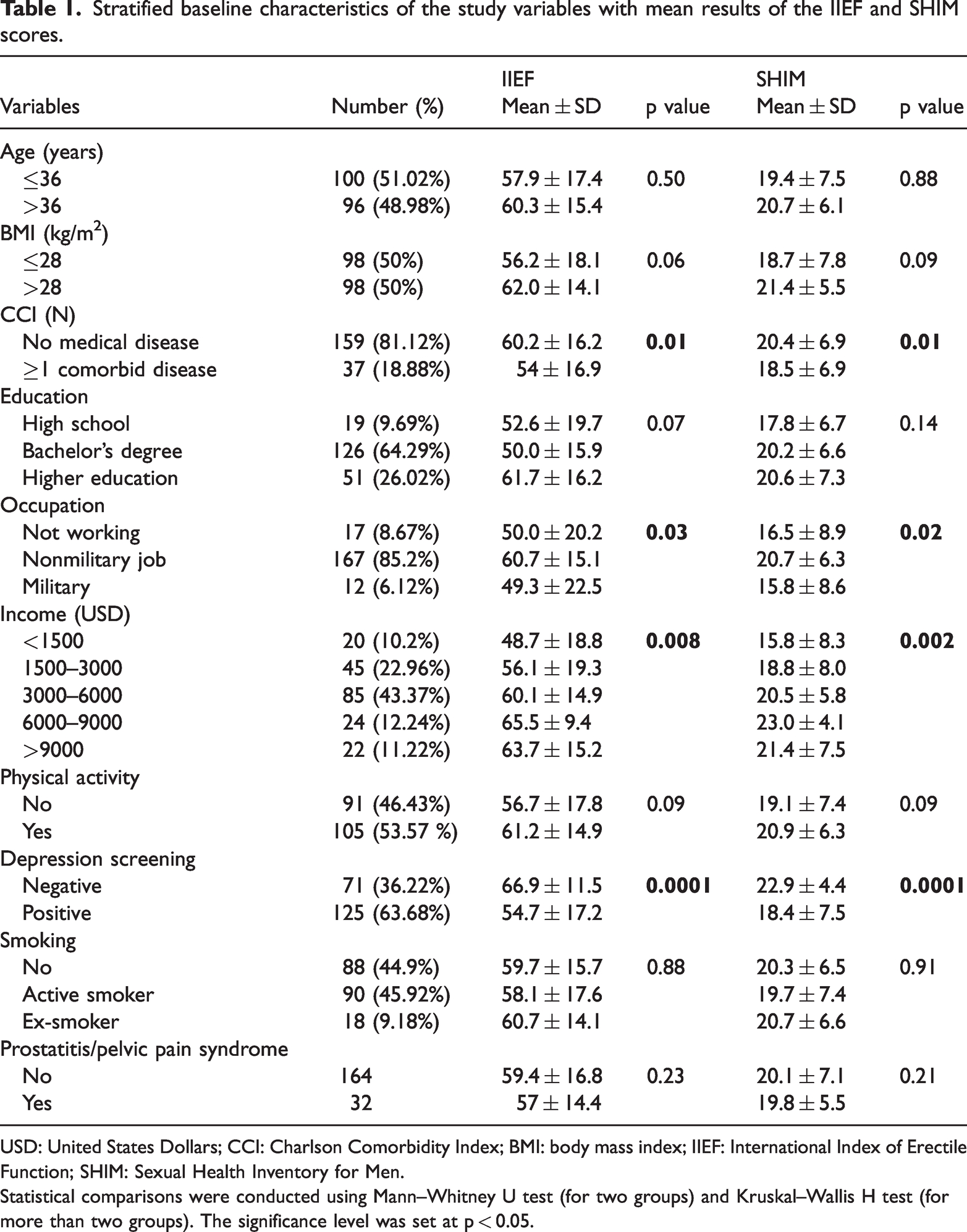
USD: United States Dollars; CCI: Charlson Comorbidity Index; BMI: body mass index; IIEF: International Index of Erectile Function; SHIM: Sexual Health Inventory for Men.
Statistical comparisons were conducted using Mann–Whitney U test (for two groups) and Kruskal–Wallis H test (for more than two groups). The significance level was set at p < 0.05.
The scores (mean ± SD) for the five domains of the International Index of Erectile Function stratified by the study variable categories.

USD: United States Dollars; CCI: Charlson Comorbidity Index; BMI: body mass index.
The significance level was set at p < 0.05.
Multivariable analysis revealed several significant associated factors for better erectile function (based on the IIEF score), namely, higher income, initial negative screening result for depression, and higher BMI. The IIEF score was 12.65 points (95% CI: −17.37 to −7.92; p < 0.0001) lower in participants with an initial positive screening result for depression than in those with an initial negative screening result for depression. Furthermore, a higher income was associated with better erectile function (Table 3).
Multivariable regression analysis.

CI: confidence interval; OR: odds ratio; USD: United States Dollars; IIEF: International Index of Erectile Function; SHIM: Sexual Health Inventory for Men.
The significance level was set at p < 0.05.
Discussion
We found that sexual dysfunction among young men in Saudi Arabia is not uncommon. In addition to the contribution of medical comorbidities, psychosocial factors such as depression, employment, and income are significantly associated with adverse sexual function. Furthermore, multivariable regression analysis revealed that income and depression are independent factors that affect overall sexual and erectile function in the young male population. We collected the data from a random community-based sample; hence, the findings reflect the real-world evidence of sexual function in men aged ≤40 years in Saudi Arabia.
The observed prevalence of ED in our study population (39.2%) is notably higher than that reported in several international studies focusing on similarly aged cohorts. For example, a US-based population study reported an ED prevalence of approximately 20% among men aged <40 years, while studies from Europe and East Asia have documented rates ranging from 15% to 25% in comparable age groups.11,12 The higher occurrence in our study may be somewhat attributed to cultural, psychological, and lifestyle factors specific to the Saudi context, including higher rates of physical inactivity, stigma surrounding mental healthcare, and a tendency toward delayed help-seeking behavior. Additionally, the use of direct interviews administered by trained medical personnel may have improved disclosure, thereby increasing detection rates. This highlights the importance of understanding ED not only as a physiological condition but also as a condition influenced by sociocultural dynamics that may differ significantly across countries.
Several sociodemographic and health-related factors were significantly associated with sexual function. Notably, participants with higher income, no comorbidities, and no signs of depression exhibited significantly better sexual performance across IIEF domains. These findings align with those of previous reports suggesting a strong interplay between psychosocial well-being, economic stability, and sexual health. Depression emerged as the most impactful factor, with affected participants showing an average reduction in IIEF score of 12.65 points. This reinforces the bidirectional relationship between mood disorders and sexual dysfunction, a connection well-documented in both clinical and community settings.
The current study makes several contributions. First, we assessed the prevalence of male sexual dysfunction among married young men in a conservative society with religious and cultural norms where the associated risk factors have never been assessed. In Saudi Arabia, the minimum age of marriage for men is 18 years. 13 It is important to set an appropriate age for marriage to protect the welfare of individuals, ensuring that they are emotionally and mentally prepared for marriage. There has been a rapid change in the Saudi society regarding the age of marriage based on the economic status, occupation, and educational level, all of which contribute to an individual’s mental status. 14 Hence, mental stability has an impact on sexual drive, as elaborated in the present study. The prevalence of male sexual dysfunction differs across countries. The prevalence found in the present study is higher than that reported in European countries. 15 An Australian study 16 showed that the prevalence of male sexual dysfunction was 54% among the Australian population aged 18–55 years. The study also showed that sexual dysfunction increased significantly with aging. Another study 17 reported that up to 10% of men aged <40 years reported ED, and the prevalence increased markedly after 40 years of age. 17
Second, our study provides supporting evidence regarding the natural history and etiological factors of sexual dysfunction among the young male population that is secondary to psychosocial factors rather than organic factors, as observed in middle-aged and older men. We controlled for potential confounders that are related to sexual dysfunction in older men. Our data are consistent with the findings from a Swiss group who confirmed sexual dysfunction among Swiss young men with depression. 18 Interestingly, BMI did not demonstrate a significant association with erectile function across any of the IIEF domains in our cohort. Although this may reflect the relatively young age and potential metabolic resilience of the study population, existing literature suggests several biological pathways through which elevated BMI may adversely affect male sexual function. Obesity is associated with reduced serum testosterone levels due to increased aromatization of androgens in adipose tissue, leading to a state of relative hypogonadism. Furthermore, obesity is linked to endothelial dysfunction, insulin resistance, and low-grade systemic inflammation, all of which can impair penile vascular integrity and nitric oxide availability—key mechanisms underlying normal erectile physiology.19–21 A recent review highlights these multifactorial pathways, emphasizing how obesity disrupts both hormonal balance and vascular function essential for sexual performance. 22 This discrepancy between our findings and the established pathophysiological links between BMI and ED suggests a need for larger longitudinal studies in younger populations to determine the threshold at which adiposity begins to exert measurable effects on sexual health.
Third, we analyzed sexual function by utilizing the IIEF, a validated instrument, to explore the association between different sexual domains and potential risk factors. We found that sexual desire and orgasm are associated with different risk factors, including educational level, occupation, income, an initial positive screening result for depression, comorbidities, and prostatitis. There have been very few studies addressing sexual desire among young men. In a study involving 591 young men aged 28–35 years in the Swiss general population, the authors reported that desire impacts overall sexual function. 23 Nonetheless, they found that sexual desire was greater in men with depression, a finding that supports our study.
We found that among the surveyed men, sexual desire was most affected. Approximately 79% of the men showed at least a one-point loss for the sexual desire domain. Consistently, sexual desire was most affected in Australian men aged 20–39 years. 24 Although previous studies have addressed sexual dysfunction, there has been limited investigation regarding orgasmic disorder in young men, and there have been no studies that have reported the detailed factors contributing to sexual desire and orgasmic disorders in young men. We found that depression is the factor most strongly associated with male sexual dysfunction, including sexual desire and orgasmic satisfaction, consistent with a previous study among young men. 25 In this literature review, 26 they concluded that anxiety and depression are associated with ED in young men and that there is a reciprocal relationship between these factors and ED. It is also well known that ED increases with aging,14,21 and it has been associated with various physical illnesses, including cardiovascular, endocrine, and neurological diseases. Understanding the multifactorial nature of male sexual dysfunction in young men is essential for effective diagnosis and management. Addressing psychological and lifestyle factors among young men through counseling and behavioral therapy, in conjunction with medical interventions when appropriate, can improve outcomes. 27 Additional studies focusing on large and diverse populations are needed to better understand the underlying mechanisms and develop tailored interventions for young men experiencing sexual dysfunction. Given the psychological underpinnings of sexual dysfunction identified in this study, particularly the strong association with depression, integrating culturally adapted psychological interventions is essential. In the context of Saudi Arabia and similar conservative societies with both religious and cultural norms, approaches that align with local values and norms are more likely to be accepted and effective.
This study has addressed several limitations of previous research on sexual dysfunction among young men. First, previous studies used self-report questionnaires, which may have introduced bias due to underreporting or overreporting of symptoms (based on personal perceptions) and may have been affected by social stigma. Furthermore, in our study, we excluded single young men due to the impact of culture on the manner of individual response. Hence, our study findings can be generalized to the married young male Saudi population. Second, most of the studies examined a homogeneous sample in terms of ethnicity, socioeconomic status, and/or cultural background, limiting the applicability of the results to more diverse populations. Third, many studies neglected the psychological impacts. Although some researchers have focused on physical treatments, there is a dearth of research on the psychological impacts of sexual dysfunction or the effectiveness of psychological interventions. Although we addressed these limitations, our study is limited by its design. A cross-sectional design provides a snapshot in time that can capture associations but not causation. Longitudinal studies are needed to better understand causal relationships and the progression of ED over time. Furthermore, our study lacked an interdisciplinary approach that combines insights from the partner’s perspective in addition to medicine, psychology, and social sciences. This tactic could offer a more comprehensive understanding of sexual dysfunction. Indeed, addressing sexual dysfunction in young people requires a multifaceted research approach that encompasses the prevalence of sexual dysfunction; nonorganic psychosocial factors such as anxiety, depression, income, and education; and organic factors that influence the cultural context and effectiveness of interventions. Prioritizing this area of study will enhance our understanding and ultimately improve the sexual health and well-being of younger individuals.
Conclusion
Sexual dysfunction in younger men may be adversely influenced by several factors, including low income, depression, and comorbidities. These findings suggest that sexual dysfunction in younger men is not only influenced by physical health but also closely linked to psychosocial factors. Further longitudinal research and multidisciplinary approaches are required to develop comprehensive, targeted interventions for sexual dysfunction in younger men, with an emphasis on mental health and socioeconomic conditions. Additionally, beyond the urology clinic, a multidisciplinary approach that includes mental health specialists should be considered when managing sexual disorders.
Footnotes
Acknowledgments
We would like to thank the data collecting team for their contribution. Artificial intelligence was used to improve the language and grammar of the text.
Author contributions
Data curation: E.R.; Formal analysis: E.R.; Investigation: E.R.; Methodology: E.R. and K.S.; validation: E.R.; Writing–original draft: E.R. and K.S.; Writing–review & editing: E.R. and K.S.
Data availability statement
All datasets are available and will be provided upon request.
Declaration of conflicting interests
The authors declare no competing interests.
Funding
No fund to declare.
