Abstract
Visceral leishmaniasis (VL) is a parasitic disease that can trigger haemophagocytic syndrome (HPS), making its prompt diagnosis crucial. The application of metagenome next-generation sequencing (mNGS) provides a rapid diagnostic approach, particularly for patients with negative bone marrow aspiration results. We present here, a case of a male patient in his early 50s who presented with fever and abdominal pain. Routine examinations failed to identify its specific cause. However, diagnosis through mNGS helped prevent a potentially fatal outcome.
Background
Visceral leishmaniasis (VL) also known as kala-azar or black fever, is a tropical disease transmitted between humans and vertebrates through infected female sandflies. 1 Without timely treatment, mortality rate can reach 95%. 2 Diagnosing VL is difficult, especially when it is complicated by haemophagocytic syndrome (HPS), which leads to a more complicated clinical picture.2,4,5 VL shares several clinical signs and symptoms with HPS, further complicating the differentiation between the two conditions. 4 While diagnosis of VL involves identifying the parasite in living tissues, such as the bone marrow, spleen, liver, and lymph nodes, 1 HPS is diagnosed according to the Hemophagocytic lymphohistiocytosis (HLH)-2004 Diagnostic Criteria. 6 The diagnosis requires genetic evidence of a mutation associated with HPS or the presence of at least five of eight criteria. 6
We present here, a case of a patient who experienced a persistent fever lasting over a month, with routine tests failing to determine its cause. However, using metagenomic next-generation sequencing (mNGS) for diagnosis, ultimately prevented a potentially fatal outcome. mNGS is a valuable diagnostic tool for ruling out other infections and enabling rapid, effective diagnosis.
Case presentation
The patient, a man in his early 50s, presented to his general practitioner with a two-week history of fever, abdominal pain, cough and fatigue. His body temperature was 40°C. He had no previous history of alcohol consumption, herbal medicine use, or drug use. Additionally, he had no history of hypertension, coronary heart disease, diabetes, hepatitis, tuberculosis, typhoid, malaria, or other infectious diseases. The patient initially received anti-infection treatment at two different hospitals, but the results were unsatisfactory.
Eleven days after his initial presentation, he attended our hospital’s fever clinic (28 November 2022) and laboratory tests showed a negative COVID-19 polymerase chain reaction (PCR) result. The patient was admitted to our haematology department two days later (30 November 2022), Physical examination showed his temperature had remained high (38.6°C), he had tenderness in the right upper quadrant, tenderness in the thoracic spine (T6–T10), referred pain in the right upper quadrant, and no abnormalities in the chest and abdomen. Further laboratory tests were conducted. Although his white blood cells (WBCs), neutrophils and platelets were within normal ranges, he had elevated levels of liver function enzymes, C reactive protein (CRP), procalcitonin, and interleukin (IL)-6 and his erythrocyte sedimentation rate (ESR) was high (Table 1). In addition, he had low levels of haemoglobin, and albumin. Comprehensive screening for infectious agents returned negative results. These included tests for: hepatitis; human immunodeficiency virus (HIV), Epstein-Barr virus (EBV); cytomegalovirus (CMV); Mycoplasma infections; Chlamydia; Legionella; Adenovirus; Respiratory syncytial virus (RSV). Blood culture results were also negative. Tests for tumour markers, vasculitis, antiphospholipid antibodies, autoimmune antibodies, and rheumatoid arthritis (RA) factors showed no abnormalities. The patient had a persistent cough, and high-resolution lung computed tomography (CT) showed left interlobar pleura thickening, mild cardiomegaly, and a small amount of fluid in the left thoracic cavity. Abdominal ultrasound confirmed hepatosplenomegaly, his liver’s right lobe measured 15.8 cm (maximum oblique diameter) and his spleen was 5.4 cm thick and 14.1 cm long. No space-occupying lesions were observed. Superficial lymph node ultrasound showed enlargement in the neck, armpit, and groin. The patient was prescribed empirical anti-infection therapy (levofloxacin, 0.5 g qd) and liver-protective medication (sodium glucuronate, 0.266 g bd).
Laboratory test results.

Abbreviations: WBC, white blood cells; AST, aspartate transferase; ALP, alkaline phosphatase; GGT, glutamyl transpeptidase; ALT, alanine aminotransferase; CRP, C-reactive protein; ESR, erythrocyte sedimentation rate; IL-6, Interleukin 6.
Haemphagocytosis was noted upon examination of the bone marrow smear. A subsequent bone marrow biopsy showed primitive and proplastic erythrocytes with scattered megaloblastic transformations, middle and late juvenile cells, rod-shaped segmented nuclei in the granulocytic system, and 4–12 megakaryocytes per high-power field (HPF). Megaloblastic anaemia was considered. Biomarker analysis showed elevated ferritin levels (1312 ng/ml [normal range: 13–150 ng/ml]), low folic acid levels (7.95 nmol/l [normal range: 10.4–78.9 nmol/l]), and normal vitamin B12 levels (589 pmol/l). The following were also elevated: soluble CD25 (sIL2R), 7533 pg/ml (normal range <6400 pg/ml); triglycerides, 2.73 mmol/l (normal range 0–1.7 mmol/l). Fibrinogen levels were within the normal range (2.02 g/l, normal range, 2.0–4.0 g/l). Immunoglobulin and complement C3 levels were within the normal range. Complement C4 levels was slightly elevated at 0.58 g/l. Four days later on 04 December, 2022, the patient was prescribed the antibiotic, meropenem (1 g tds) and on 05 December, 2022, received dexamethasone (15 mg/d) and intravenous immunoglobulin (IVIG, 25 g/d). However, due to financial constraints, the patient discontinued IVIG after four days despite his persistent intermittent fever.
On the 12th day of hospital admission, metagenome next-generation sequencing (mNGS) was used to test for infectious diseases and Leishmania donovani was identified in 47% of the sample (Figure 1). Subsequently, the patient was treated with pentavalent antimony (0.6 g qd). After completing a 6-day treatment cycle, the patient experienced relief from fever and hepatosplenomegaly.
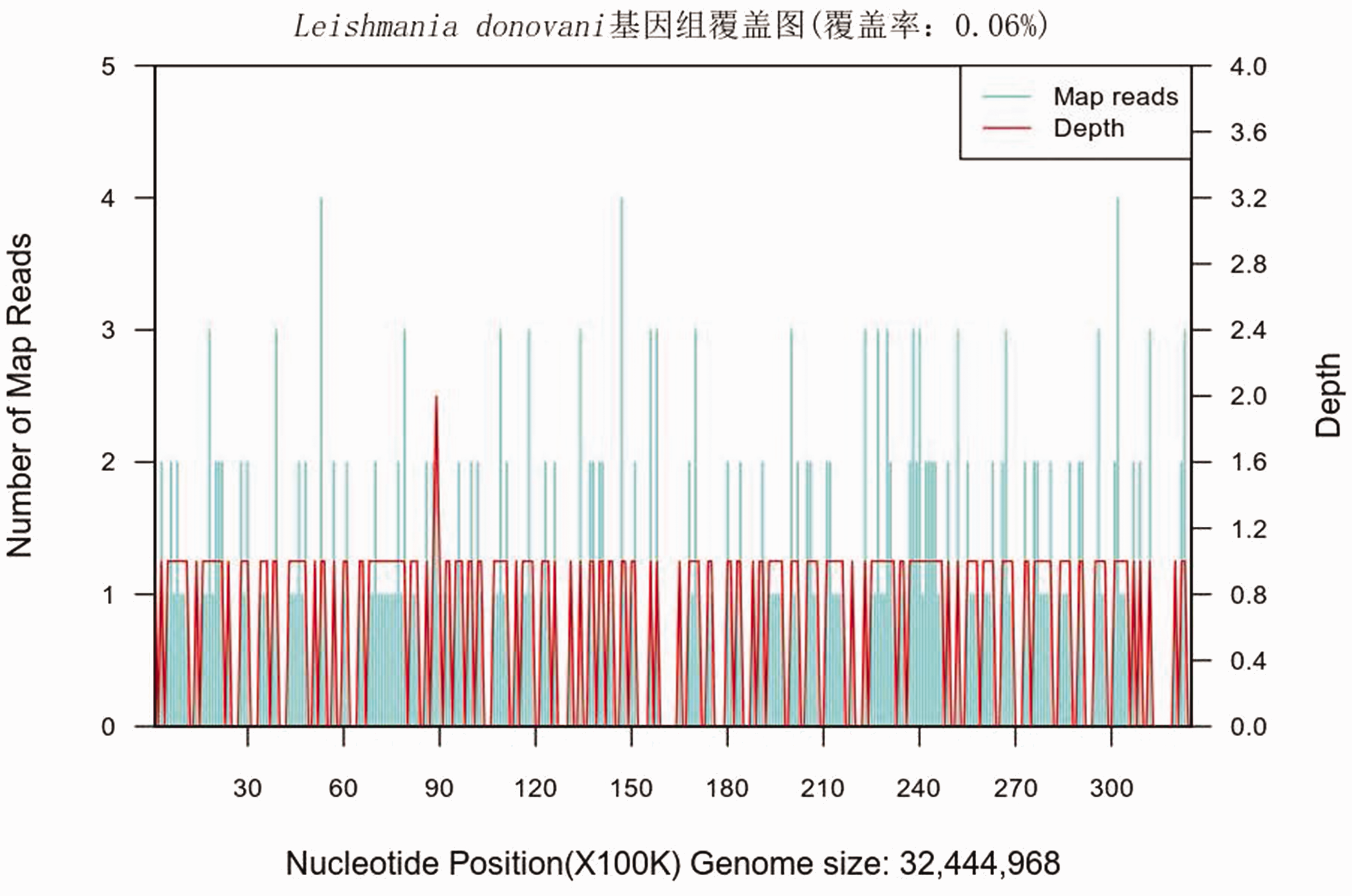
Leishmania donovani genome coverage map (coverage rate 0.06%).
The reporting of this study conforms to CARE guidelines. 7 The patient provided consent for publication of his anonymised data. Publication of this case report was approved by the Medical Ethics Committee of the First Affiliated Hospital of Shihezi University (KJ2024-101-02).
Discussion
Visceral leishmaniasis (VL) ranks as the second deadliest tropical and subtropical disease following malaria. 8 Each year, there are approximately 500,000 new cases and 50,000 deaths worldwide, although these numbers are believed to be underreported. 9 VL remains a significant public health issue in many developing countries. 5 VL is primarily found in seven countries (Brazil, Ethiopia, India, Kenya, Somalia, South Sudan, and Sudan) accounting for over 90% of global cases. 9 In recent years, VL has rapidly reemerged in regions of China that had previously achieved elimination. 10 Sporadic cases have been reported in several Chinese provinces, including Sichuan, Gansu, Xinjiang, Shanxi, Shaanxi, and Inner Mongolia. Clinical manifestations include irregular fever, wasting, progressive liver and spleen enlargement, lymphadenopathy, panhaemopenia, and hyperglobulinaemia, which overlap with symptoms of HPS. 5 Traditional diagnostic methods for VL consider bone marrow smear examination the gold standard.5,9 Recently, molecular biology methods have significantly improved diagnostic efficiency, with PCR detection targeting specific Leishmania gene sequences achieving sensitivity exceeding 95%.
HPS, also known as haemophagocytic lymphohistiocytosis (HLH), is characterised by non-malignant histopathological features. 5 Clinical manifestations include fever, pancytopenia, hepatosplenomegaly, hypofibrinogenemia, hypertriglyceridemia, elevated ferritin levels, abnormal cellular immune function, decreased natural killer (NK) cell activity, and the presence of haemophagocytic cells in bone marrow smears. 5 This condition is characterised by the continuous activation of cytotoxic T lymphocytes and NK cells, leading to the secretion of inflammatory factors, tissue damage, and multiple organ dysfunction. 5 HPS can be classified into two categories, the primary or genetic form and a secondary or acquired form. 5 Primary HPS is associated with inherited immune deficiency states often linked to gene mutations such as PRF1 and UNC13D. Secondary HPS is acquired and often linked to underlying conditions such as tumours, infections, and autoimmune diseases. 11 Epstein-Barr virus (EBV) has been suggested to be the most common infection associated with HPS in children.5,12 While VL-associated HPS is considered rare, Leishmania is regarded as the most common protozoan triggering infection-related HPS.5,13–15
As mentioned earlier, diagnosis of HPS requires genetic evidence of a mutation or the presence of at least five of eight criteria.5,6 Although the HPS-2004 diagnostic criteria were not initially fully met in this patient due to cytopenia affecting fewer than two lineages and abnormal triglyceride and fibrinogen levels not meeting the thresholds, the criteria ultimately became applicable. However, diagnosis and treatment were delayed. Additionally, because serological and molecular tests for VL were not routinely performed at our centre, conventional diagnostic methods were unable to identify the infection source. Given the possibility of a rare pathogen, mNGS tests were conducted to help identify the cause. Due to its high throughput and efficiency, mNGS is an invaluable tool for diagnosing infectious diseases, especially those caused by atypical pathogens. Once the pathogen's nucleic acid sequence was obtained, comparisons with database samples helped identify the species of the microorganism responsible. 16 The mNGS method offers a high speed, wide detection range, with high sensitivity and specificity. Early evaluation of mNGS indicators can promptly identify pathogens and guide clinical treatment, potentially improving outcomes.17,18 However, its high-cost limits widespread use.
With regard to VL-HPS, the primary focus should be to treat VL itself. Currently, pentavalent antimony and amphotericin B are the first-line treatments. 5 If a patient responds poorly to treatment, adjustments may be necessary. For HPS, corticosteroids (methylprednisolone 1–2 mg/kg/d) and IVIG (1 g/kg/d for two days) is used for mild-to-moderate cases, while severe cases may require etoposide (150 mg/m2 twice a week).5,6 However, most HPS patients improve spontaneously after VL treatment. 19 Prognosis assessment should prioritize (1) controlling the primary disease, which includes resolving fever, reducing spleen size, and improving blood cell counts; (2) monitoring changes in inflammatory markers, such as a decrease in ferritin and soluble CD25 levels; and (3) assessing improvements in organ function. It is recommended to conduct follow-up visits every two weeks for the first three months, thereafter, monthly visits until six months. Long-term follow-up should focus on monitoring the risk of relapse, particularly in patients with compromised immune function.
This diagnostic and treatment process highlights the importance of multidisciplinary collaboration and the value of new diagnostic technologies in managing complex cases. Future research should concentrate on (1) developing faster and more accurate diagnostic methods and (2) creating prognosis prediction models. These advancements will enhance the prognosis for patients with VL-HPS.
Footnotes
Declaration of conflicting interests
The authors declare there are no conflicts of interest.
Funding
This study was supported by a grant from the Innovation and Entrepreneurship Platform and Base Construction Plan of the Corps Branch of the National Hematology Clinical Research Center (2021CA002).
