Abstract
Thoracic trauma is commonly encountered in daily clinical practice; however, blunt thoracic trauma in patients with congenital cystic adenomatoid malformation (CCAM) is rare. CCAM rupture denotes a broad spectrum of manifestations on imaging and may be misdiagnosed as many other conditions. Consequently, this leads to inaccurate treatment and poor patient outcomes. We report the case of a girl with the initial diagnosis of a cavitary lung lesion that was likely a traumatic pulmonary pseudocyst or CCAM. The patient received medical therapy for 20 days; however, her condition did not improve. Subsequently, she underwent right lower lobectomy. Ruptured CCAM was confirmed during surgery and with histopathology. No complications occurred postoperatively, and the patient made a good recovery.
Keywords
Introduction
Congenital cystic adenomatoid malformation (CCAM), also known as congenital pulmonary airway malformation (CPAM), is a congenital anomaly of the lower respiratory tract belonging to a heterogeneous group of benign hamartomatous disorders involving tissue from different pulmonary origins. 1 CCAM is characterized by a proliferation of terminal bronchioles and is classified into five major subtypes. CCAM is a rare entity with an incidence of 1 per 11,000 to 35,000 live births, and the rate is higher during mid-pregnancy.1–3 Currently, with advancements in imaging modalities, the vast majority of CCAMs are discovered prenatally or in the early stages of life.2,3 Depending on the size and location of the masses, clinical presentation may vary from asymptomatic to progressive respiratory distress. 4 Distinguishing CCAM from mimicking lesions is very important to guide accurate treatment and to avoid serious consequences. 5 Here, we present a case of CCAM mimicking a traumatic pulmonary pseudocyst and discuss how to distinguish between these two entities. The case information was studied retrospectively using the patient’s medical records and archived images.
Case report
A 10-year-old girl was admitted to the hospital 1 hour after sustaining blunt trauma to the chest in a motorcycle accident. Her medical history included recurrent episodes of nonspecific pneumonia without treatment. Her family history was unremarkable. She complained of chest pain without hemoptysis or dyspnea. She was normotensive, with a blood pressure of 110/60 mmHg; pulse rate: 100 bpm, respiratory rate: 20 breaths per minute, body temperature: 37°C, and peripheral capillary oxygen saturation: 99%. Physical examination revealed ecchymosis and tenderness over the lateral right lower chest wall, and auscultation revealed diminished breath sounds in the right lower lung field. Laboratory results for total blood count, metabolic panel, coagulation profile, and inflammatory markers were within normal limits.
Chest X-ray performed within 3 hours of the trauma showed a cavitary lesion with surrounding infiltrative shadows in the right lower lung and a small amount of pneumothorax ipsilaterally (Figure 1). There was no associated pleural effusion or rib fracture. Computed tomography (CT) was performed shortly thereafter for further evaluation. CT revealed a large thick-walled air–fluid cavitary lesion with smaller satellite cysts scattered nearby, interspersed with areas of alveolar lesions, patchy ground-glass opacities, and consolidations in the right lower lung lobe. This lesion communicated continuously with a small amount of pneumothorax in the right pleural space (Figure 2). No previous chest imaging was available for comparison.

Chest radiograph showing a thick-walled cavity (asterisk) with peripheral alveolar opacities (arrowheads) in the right lower lobe and a small amount of pneumothorax (arrows).

Chest CT images showing thick-walled multicystic lesions (asterisks) with an air–fluid level and a maximum size of approximately 4 × 5 cm in the right lower lung lobe. There is patchy ground-glass opacification and consolidation around the cysts (arrowheads). Note the right pneumothorax (arrows).
The lesion was initially diagnosed on imaging as a cavitary lesion of a ruptured lung due to the trauma, leading to pneumothorax. The differential diagnosis was traumatic ruptured lung abscess, traumatic pulmonary pseudocyst, or traumatic ruptured CCAM. A lung abscess was ruled out because the results of subsequent tests performed for further evaluation, namely Gram stain, acid-fast stain, and sputum culture for bacteria, fungi, and tuberculosis were negative. A traumatic pulmonary pseudocyst lesion could not be excluded because these can present immediately after trauma.
The patient received conservative treatment with broad-spectrum antibiotics, fluids and electrolyte therapy, respiratory support, and close monitoring of vital signs or abnormal symptoms for 20 days; however, her symptoms and imaging findings did not improve. Therefore, she was re-evaluated by a multidisciplinary team comprising radiologists, internists, and thoracic surgeons, and the unanimous diagnosis was CCAM rupture due to trauma. This diagnosis was thoroughly explained to the patient and her caregiver, and she underwent right lower lobectomy (Figure 3). Histological findings of the resected specimen revealed multiple cysts composed of fibrous walls lined by ciliated cylindrical cells, without bronchial cartilage. There were also scattered areas of interstitial perivascular hemorrhage, intravenous thrombosis, enlarged alveoli, thin septa, and rupture. The final diagnosis was CCAM type 1. The patient gradually improved, and she was discharged after 10 days. She was followed-up for 1 year and remained healthy.
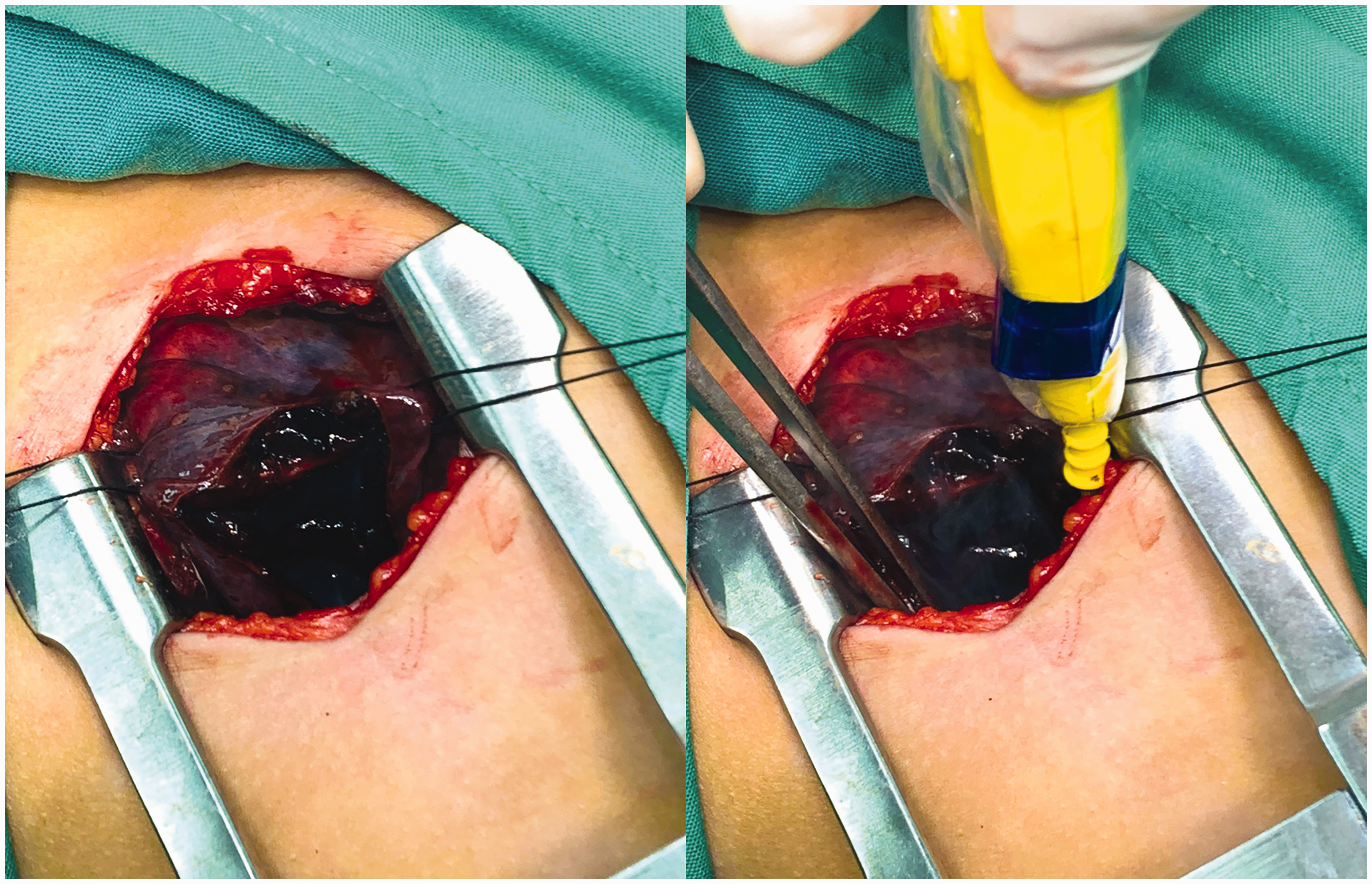
Operative photographs of open right lower lobectomy showing lung contusion and hematoma formation.
The requirement for ethics approval for this study was waived because our institution did not require ethical approval for reporting individual cases or case series. This report was prepared in accordance with the ethical standards of the institutional ethics committee and with the 1964 Helsinki Declaration. Written informed consent was obtained from the patient's family for publication of this case and all accompanying images. The reporting of this study conforms to the CARE guidelines. 6
Discussion
Cystic and cavitary lung lesions are broad-spectrum diseases commonly observed on imaging and may comprise congenital lobar emphysema, pulmonary sequestration, congenital cystic adenomatoid malformation, bronchogenic cyst, pleuropulmonary blastoma, airway diseases (congenital bronchial atresia, congenital bulla, bronchiectasis, cystic fibrosis, congenital bronchiectasis, Williams–Campbell syndrome), infectious diseases (bacterial, fungal), parasitic disease (e.g., hydatidosis), collapsed lung, septic embolism, collagen vascular diseases (e.g., rheumatoid arthritis), systemic diseases (e.g., granulomatosis with polyangiitis, sarcoidosis, Langerhans cell histiocytosis, lymphangioleiomyomatosis, lymphocytic interstitial pneumonia), and traumatic pseudocyst.7–9 In this discussion, we focus on two diseases that were relevant to the differential diagnosis of traumatic CCAM rupture in our case: pulmonary abscess and traumatic pulmonary pseudocyst.
First, pulmonary abscess appears as a complication of pneumonia, and patients present with fever, productive cough, and chest pain.8,10 Pulmonary abscesses can sometimes rupture spontaneously or secondary to chest injury, which leads to pneumothorax, empyema, or the development of bronchopleural fistulas. 11 Abscesses manifest on CT as air–fluid cavitary lesions with thick walls, and they are peripherally enhanced with contrast and have central necrosis.8,11 Pulmonary abscesses can occur anywhere in the lungs.8,11 Most abscesses can be treated conservatively; however, percutaneous drainage is necessary in approximately 20% of cases. 11 The imaging findings in our patient were very similar to those of a ruptured lung abscess; however, this was excluded because there was no recent history of lung infection, and markers of infection were negative.11,12
Second, traumatic pulmonary pseudocysts develop following a high compressive force transmitted to the lung parenchyma. 13 This condition mainly occurs after blunt trauma to the chest but is also seen with penetrating wounds. 14 The force of the impact lacerates the lung tissue via rapid compression and decompression of the thorax and leads to cavernous lesions in the lung tissue, particularly when a closed glottis impedes the passage of air through the upper airways.13,15 If there is no communication between the cavities and the pleural space, air and fluid escape from the parenchyma and fill the cavity. The underlying mechanism of traumatic pulmonary pseudocyst, especially in children and young adults, is that when the thorax is elastic, the parenchyma is vulnerable, and with an intact visceral pleura, a large pressure gradient is generated between the proximal obstruction and multiple hyperinflated alveoli.7,13 A pseudocyst lesion was excluded in our patient because the cavitary lesion communicated with the pleural space; therefore, pseudocyst formation was unlikely. However, some studies have shown the coexistence of traumatic pulmonary pseudocyst and pneumothorax, but with no communication between the pseudocyst lesion and the pleural space.5,16,17 Pseudocysts can appear immediately or within a few hours after trauma and can change rapidly in size and shape on imaging studies over time. 3 This can help distinguish traumatic pulmonary pseudocysts from other cavity lesions. Pulmonary pseudocysts are usually treated conservatively and tend to resolve completely within 4 months.3,18 Traumatic pulmonary pseudocysts with severe complications may require surgery.18,19 The lesion in our patient did not decrease in size within 14 days; therefore, traumatic pulmonary pseudocyst may occur less frequently than CCAM.
Conclusion
Distinguishing between cystic and cavitary lung lesions is difficult because of their relatively similar appearance on imaging. However, the management of these lesions is distinct; therefore, a combination of medical history, laboratory testing, imaging studies, and the course of the disease is needed to make an appropriate diagnosis.
Research Data
Research Data for Traumatic rupture of congenital cystic adenomatoid malformation mimicking traumatic pulmonary pseudocyst: a case report
Research Data for Traumatic rupture of congenital cystic adenomatoid malformation mimicking traumatic pulmonary pseudocyst: a case report by Van Trung Hoang, The Huan Hoang, Hoang Anh Thi Van, Thanh Tam Thi Nguyen, Vichit Chansomphou in Journal of International Medical Research
Footnotes
Acknowledgements
We would like to thank the patient and her guardian for permission to use her images and case information.
Author contributions
All authors contributed to the study conception and design. All authors read and approved the final manuscript.
Availability of data and materials
There are no data to share. All patient details have been mentioned in the manuscript.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
