Abstract
Zenker’s diverticulum (ZD) is a bag-like pharyngeal pouch that protrudes to the outside of the pharynx. It is thought to be an acquired disease that occurs following the dysfunction of laryngopharynx muscle, and certain body shapes may be predisposed to this condition. We report a 56-year-old female of slim build with ZD. Computed tomography scanning revealed a hypodense lesion on the left posterior side of her upper esophagus that was filled with air and had no obvious wall. To verify this finding, a barium esophagogram was carried out which showed a round pouch at the level of the 6th cervical vertebral body that communicated with the esophagus through a narrow neck. ZD was subsequently confirmed by endoscopy. These findings provide further evidence in support of a body shape predisposition for ZD.
Keywords
Introduction
Zenker’s diverticulum (ZD), also known as a pharyngeal pouch, hypopharyngeal diverticulum, or pharyngoesophageal diverticulum, is an acquired disease characterized by a bag-like pouch protruding from the pharynx that is caused by the dysfunction of laryngopharynx muscle. 1 From an anatomy and histology perspective, ZD should be categorized as a pulsion diverticulum (pseudo-diverticulum). The demonstration of a connection from the pouch to the hypopharynx or esophagus in real-time is considered to be positive for ZD diagnosis. Typical clinical manifestations of ZD appear to be related to the size of the diverticulum, and open or minimally invasive surgery is the main form of treatment. It has been speculated that certain body shapes may predispose individuals to this condition, but further study is needed to confirm this.
Case study
A 56-year-old Chinese female of slim build complained of a neck mass that had persisted for 2 years. Her weight was 45 kg and her height was 1.6 m, giving a body mass index (BMI) of 17.60 kg/m2. Physical examination showed a small protrusion on the left side of her neck that caused pain upon pressure. Her medical history included a partial thyroidectomy following adenoma of the right lobe 7 years previously. A horizontal scar on the lower right side of her neck was noted.
A computed tomography (CT) scan disclosed a hypodense lesion on the left posterior side of her upper esophagus. The lesion contained air and had no obvious wall. Most of the lesion was filled with multiple air bulbs with a low-density substance between the bulbs (Figure 1). The lesion did not appear to communicate with either the trachea or esophagus. The left upper lobe of her thyroid was slightly compressed. To verify CT findings, she underwent esophagography after swallowing barium. This revealed a round pouch at the level of the 6th cervical vertebral body which communicated with the esophagus through a narrow neck (Figure 2). The bottom margin of the pouch was rough. A diagnosis of ZD was made based on esophagography findings. A CT scan with an extra slice was performed to obtain sufficient evidence for a diagnosis of diverticulum. Residual barium was detected throughout the center of the lesion both on the scout image and the axial image (Figure 3). ZD was subsequently confirmed by endoscopy (Figure 4).
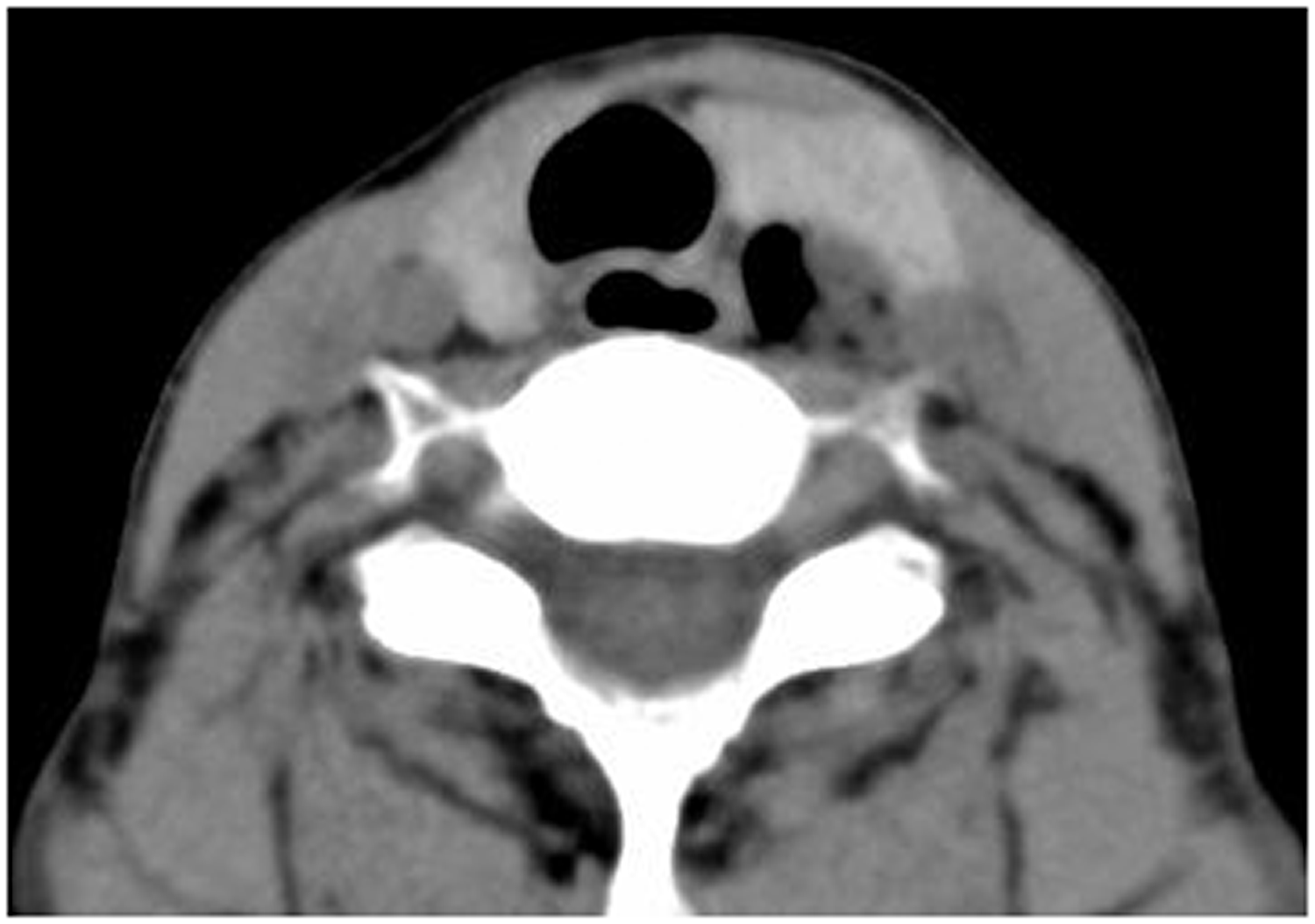
Cervical CT cross-sectional scan showing a round cyst cavity filled with air on the left side of the esophagus and the back left lobe of the thyroid. Dorsal hypodense bulbs are visible

Anteroposterior esophagogram after barium swallow showing a cyst cavity filled with barium protruding outwards to the esophageal contour at the level of the 6th cervical vertebra.

Cervical CT cross-sectional scan showing barium residue in the cyst cavity on the left side of the esophagus.

Endoscopy showing a wide cyst cavity containing food residue on the left side of the cervical esophagus.
A detailed medical history taken after the diagnosis showed that the patient had experienced choking episodes during swallowing in the past year. She also reported discomfort in her neck when turning her head to the left, and described once vomiting retained food. An occasional gurgling sound could be heard from her pharynx, and the esophageal mass could be retracted after being compressed.
The reporting of this study conforms to CARE guidelines, 2 and written informed consent to publish was obtained from the patient. The study was approved by the Ethics Committee of Hebei General Hospital.
Discussion
Diverticula are bag-like pouches that protrude from the digestive or urinary tracts. The diverticulum wall is formed from the lining of the tract from which it derives. Acquired or congenital factors leading to structural deformation of this wall can result in diverticula. 3
ZD usually occurs as a sac-like outpouching formed by mucosal and submucosal layers at the posterior wall of the esophagus above the cricopharyngeal muscle, which is the junction of the pharynx and the esophagus at the level of the 6th cervical vertebral body. It occurs in 0.01% to 0.11% of the population, 3 twice as frequently in males than in females, and is more common in North Europe, Canada, and the USA, and rarely seen in Asian countries. Because ZD can be asymptomatic, its exact prevalence is likely to be underestimated.3,4 It was first described by the English surgeon Ludlow in a case report published in 1767. 5 A century later, the German pathologist Zenker first described the histologic characteristics of this diverticulum. 5 Since then, pharyngeal pouches have been referred to as ZD. Based on its anatomy and histology, ZD should be categorized as a pulsion diverticulum (pseudo-diverticulum).
Rarer forms of cervical esophageal diverticula include Killian’s diverticulum and Laimer’s diverticulum. The former occurs in the Killian–Jamiseon triangle (located inferior to the cricopharyngeus on both sides of this muscle’s insertion into the cricoid cartilage). The latter is formed in Laimer’s triangle (located inferior to the cricopharyngeus in the posterior midline above the confluence of the longitudinal layer of esophageal muscle). Killian’s triangle is a triangular area lacking a muscular layer at the pharyngoesophageal junction, whose weakness makes it difficult to resist pressure during swallowing. It is located above the transversal fibers of the cricopharyngeal muscle and under the oblique fibers of the inferior pharyngeal constrictor muscle, both of which contribute to the upper esophageal sphincter. Laimer’s triangle is covered only by a circular layer of esophageal muscle.6,7
The etiology of ZD remains unknown. Because it is commonly identified among patients older than 50 years of age but is rare in those younger than 30 years old, it is considered an acquired disease caused by laryngopharynx muscle dysfunction. Occlusive mechanisms are thought to be the most important in its development, including uncoordinated swallowing, and impaired relaxation and spasm of the cricopharyngeal muscle; this gives rise to high pressure in the distal pharynx, making its wall herniate through the point of least resistance. 8
Our patient was of short stature and slim build, with a BMI of only 17.60 kg/m2. Certain body shapes have been suggested to be predisposed to ZD, including slim patients whose possible sarcopenia might cause ZD. However, few studies have reported cases with a predisposed body habitus, or even those with low weight, height, or BMI. It is likely that some figure predisposition exists, and that disease occurs through loss of tissue elasticity and decreased muscle tone. Together with two published cases reporting a male patient of 39 kg and 1.63 m in height with a BMI of 14.67 kg/m2, 2 and another male of 58 kg and 1.63 m in height with a BMI of 21.83 kg/m2, 3 this study provides further evidence supporting a body figure predisposition. However, further research is still needed for verification.
Typical clinical features of ZD may be related to the size of the diverticulum. Patients with a small ZD seldom complain of their symptoms. Conversely, patients with a large diverticulum always report multiple discomforts including dysphagia (80%–90%), regurgitation (60%), cough (30%–40%), halitosis, and weight loss.3,4 Moreover, the sound of gurgling has been reported in patients with ZD while swallowing food. Secondary pneumonia after chronic aspiration was reported as the first complaint of some patients with ZD, and severe complications of ZD include diverticulitis (secondary to food and liquid entrapment), ulceration, bleeding, perforation (during endoscope passage), and, rarely, canceration.
Barium swallow, as a noninvasive examination, offers more advantages in diagnosing ZD than CT. 5 These include the ability to show a connection with the hypopharynx or esophagus in real-time, which is considered affirmative for the diagnosis. If a patient undergoes CT scanning without oral contrast that detects a gassy sac beside the laryngopharynx or esophagus, esophagography is of critical importance in reaching a diagnosis. Although upper gastrointestinal endoscopy would confirm the presence of a diverticulum, most patients would not choose this approach initially. The contractive osculum of the diverticulum might account for disconnection to the hypopharynx or esophagus, as seen in the presentation of our patient. Differential diagnoses should include a cervical space abscess, neck trauma, or a tracheo-esophageal fistula after interventional therapy, which could all appear as areas of low density in cervical soft tissue.
Open or minimally invasive surgery is the main therapeutic method for ZD, though there is no consensus among surgeons regarding the choice of treatment.2–10 In open surgery, the diverticulum can be resected (diverticulectomy), suspended and fixed on the hypopharyngeal wall (diverticulopexy), or invaginated into the esophagus (diverticular inversion) followed by cricopharyngeal myotomy. Because of a lower risk of complication, morbidity, and mortality, minimally invasive surgery is gaining in popularity. Moreover, if the diverticuloscope is positioned transorally, the common wall containing cricopharyngeus muscle fiber between the esophageal lumen and diverticular sac can be disclosed, thereby enabling division of the septum to be performed. 11
