Abstract
Most esophageal food impactions either pass spontaneously or are treated endoscopically. Severe food impactions can require extensive endoscopic therapy that potentially could lead to procedure-related complications. There are few alternate therapies available when endoscopy fails. Traditionally, pharmacologic therapy with glucagon has been performed with varying success. This case report and discussion will outline the management of a complete food impaction and medical therapies available when first-line endoscopic treatment fails. We present a case in which the endoscopic intervention for esophageal food bolus impaction was unsuccessful.
Introduction
Foreign body ingestion and esophageal food bolus impaction (EFBI) are common gastrointestinal (GI) emergencies with an annual incidence of 13:100,000. 1 While the majority of cases resolve spontaneously, 10%–20% require endoscopic intervention. 2 Meat bolus impaction in edentulous elderly individuals encompasses the leading cause of food impaction among the adult population, and patients with pre-existing esophageal pathology are at higher risk.3,4 The presence of sialorrhea is important, as this finding can lead to further complications, such as pulmonary aspiration requiring emergent airway protection with endotracheal intubation. 4 Additional complications of esophageal foreign body include fistulas, abscesses, pneumomediastinum, mediastinitis, pneumothorax, ischemic necrosis and perforation. 5
Pharmacologic agents are often used prior to endoscopy in patients with esophageal soft bolus impaction. 3 Although no one agent is superior to another, butylscopolamine, glucagon, calcium channel blockers (CCBs), benzodiazepines and nitrates are among the current treatment options available.3,5 Glucagon is one of the most widely agents in the Emergency Department (ED) for EFBI despite the lack of literature supporting its efficacy. 5
For complete esophageal food impactions or those not relieved spontaneously, flexible endoscopy is first-line therapy for both diagnostic and therapeutic purposes. 4 The success rate of flexible endoscopy in such cases is over 95%, with minimal complications. 3 Endoscopy should be performed within 24 h to relieve food impaction. The highest incidence of complications occurs with impaction or foreign body in the esophagus, with complication rates increasing proportionately to the dwell time. 3 With refractory food impactions that are not relieved with endoscopic therapies, pharmacologic therapy becomes more crucial. We present a case in which the endoscopic intervention for EFBI was unsuccessful and pharmacologic treatment became necessary.
Case presentation
A 53 year-old White male presented to the emergency department with dysphagia to liquids and solids for 1 day. He reported eating boneless chicken the night prior when he felt the food get lodged in his throat. In the emergency department, his vital signs were stable and physical examination was unremarkable. Food impaction was suspected and gastroenterology was consulted.
Esophagogastroduodenoscopy (EGD) was performed and impacted meat, approximately 6 cm in diameter, was visible in the lower third of the esophagus at 35 cm from the incisors (Figure 1). Attempts were made to gently push the soft bolus into the stomach with the endoscope but were unsuccessful. Multiple attempts, over the course of several hours, to relieve the food bolus with Roth Net retrievers, biopsy forceps, tripod forceps and dilation balloons were also unsuccessful (Figure 2). The patient remained intubated in the intensive care unit with recommendations to give glucagon 0.5 mg intravenously (IV) once every 6 h overnight and repeat EGD in the morning. Of note, the patient also received benzodiazepines while intubated for sedation.
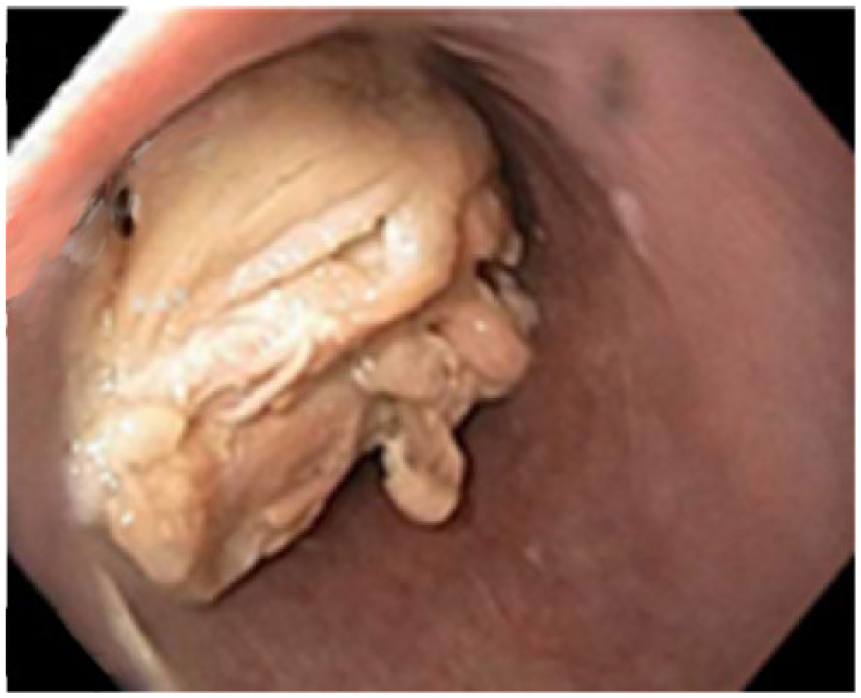
Impacted food bolus (chicken) in the lower esophagus at 35 cm from the incisors.

Impacted bolus cast in lower esophagus after multiple removal attempts at 35 cm from the incisors.
Repeat EGD performed the following day showed that the food bolus had spontaneously passed (Figure 3). The esophagus appeared normal and multiple biopsies were taken from the proximal and distal esophagus to rule out eosinophilic esophagitis (EoE). The biopsy results showed features suggestive of reflux in the proximal and distal esophagus. There was no histological evidence suggestive of EoE. We postulate that the patient did not finish the oral phase of digestion, causing the partially chewed meat bolus to reach the esophagus where it was lodged. This likely caused significant esophageal spasm in a physiological attempt to push the bolus into the stomach, rendering the complete endoscopic removal a challenge. He was discharged with a proton pump inhibitor twice daily and told to follow up with GI in the clinic. The patient was called 1 week after his procedure and he was doing well without repeat episodes of dysphagia.

Food bolus in the gastric antrum.
Discussion
This case report describes a seldom necessary pharmacologic approach to refractory esophageal food impaction. The cast of meat was so extensive; the endoscope could not dislodge or traverse the impaction, making it impossible to treat. There is no consensus regarding the management of esophageal food impaction when endoscopic intervention fails. Several pharmacologic agents are available when there are difficulties related to endoscopy; despite the limited information about their efficacy in the literature, glucagon has been the most widely supported.
Intravenous glucagon is the most widely used agent for EFBI in the ED; it has few adverse side effects which can include nausea, vomiting and diarrhea. 1 Doses of 0.25 and 0.5 mg have been shown to reduce the mean resting pressure of the lower esophageal sphincter (LES). 1 Higher doses of glucagon are not more effective in reducing LES pressure. 4 Glucagon has little effect in relaxing smooth muscle–containing anatomical barriers such as esophageal rings or strictures. Hypersensitivity to glucagon and history of pheochromocytoma or insulinoma are contraindications to its administration. 1
Few studies have investigated the use of glucagon alone in the resolution of EFBI because it is commonly given with other agents such as benzodiazepines, as seen in our case. 5 One randomized study investigated the effects of IV diazepam on resolution of EFBI but found no significant difference when compared to placebo. 6 A large retrospective study found patients treated with glucagon and a benzodiazepine were more likely to have resolution of the EFBI; resolution with glucagon alone was seen in one-third of patients, comparable to the rate of placebo previously reported in the literature. 7
CCBs work on the smooth muscle of the esophagus by depleting intracellular calcium. 1 One study reports a significant decrease in LES pressure on manometric recordings for more than 1 h after 10–20 mg of sublingual nifedipine.5,8 Patients with diffuse esophageal spasm have been shown to reduce the amplitude and frequency of non-peristaltic contractions after nifedipine.6,9 Routine use of CCBs in the acute management of esophageal impaction is not currently recommended in current guidelines. 1
Hyoscine butylbromide, buscopan, is a peripherally acting antimuscarinic and anticholinergic agent, widely used in other countries for its anti-spasmodic activity to relax the LES. 1 The evidence supporting the efficacy in relieving esophageal food impactions is sparse and studies have shown inconsistent findings.1,10 A study by Basavaraj et al. 10 demonstrated that patients who received buscopan had similar rates of food bolus dislodgement to patients who had spontaneous resolution.
Conclusion
Although there are limited data to support each of the various medical therapies, they are still widely used in clinical practice due to their safety profile and lower cost compared to endoscopy and availability. There have been very few investigations on pharmacologic therapy for esophageal food impaction; this case is an example of the importance of pharmacologic therapy and the need for further studies in this field.
Footnotes
Acknowledgements
L.S. acquired the data, reviewed the literature and drafted the manuscript. R.B. provided the endoscopic images, edited and critically revised the manuscript. K.R. edited and critically revised the manuscript. M.M. designed, edited and critically revised the manuscript for intellectual content. S.D.M. edited, critically revised the manuscript for intellectual content and is the article guarantor. J.S.S. edited and critically revised the manuscript for intellectual content.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethics approval
Our institution does not require ethical approval for reporting individual cases or case series.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
