Abstract
Percutaneous nephrolithotomy (PCNL) remains an important method for treating upper urinary calculi. However, bleeding and peripheral vascular injury are serious complications of PCNL. Injury of the inferior vena cava accompanied by secondary thrombosis has rarely been reported clinically. We treated a patient who experienced bleeding during PCNL to establish a channel. A catheter was used to make a renal fistula, and the inferior vena cava was implanted. The wound was fixed and compressed by balloon injection, and secondary thrombosis and repeated infection occurred after the operation. A filter was then placed, the water balloon was released, and the fistula was removed. The anti-bacterial and anticoagulant filter was removed. This major complication was successfully managed. In our patient, during PCNL, the renal fistula entered the inferior vena cava by mistake. If this issue cannot be treated in time, it can easily lead to the formation of secondary thrombosis. A fistula can be extracted through an inferior vena cava filter, and anticoagulant treatment and other conservative treatment regimens can be used to treat patients in this situation. These treatments avoid the possibility of further damage from open surgery.
Keywords
Introduction
Percutaneous nephrolithotomy (PCNL) is an important technique in the treatment of upper urinary calculi. 1 Intraoperative vascular injury and postoperative hemorrhage remain serious complications of PCNL. Injury of the inferior vena cava combined with thrombosis is rare clinically, and its treatment is troublesome. Therefore, there has not been much experience for creating a standard treatment for this condition.2,3 In this study, we report a case of inferior vena cava injury and secondary thrombosis after PCNL. We also discuss the relevant literature on managing PCNL.
Case presentation
The reporting of this study conforms to the CARE guidelines. 4
In September 2018, a 48-year-old woman was diagnosed with multiple calculi in both kidneys before surgery and underwent right PCNL in a local hospital. A right PCNL was performed through the right renal vein into the inferior vena cava. The instrument used for puncture was a conventional 18 G puncture needle, while the dilator used was a conventional disposable fascial dilator (minimally invasive puncture kit), dilated to 18 F and left in a 16 F working sheath. Intraoperatively in the prone position, the right renal upper calyces were punctured under the guidance of ultrasound in the local hospital. A massive hemorrhage was found when a working channel was established. There was not much bleeding at the time of puncture, but bleeding occurred after dilatation. The calyces and pelvic channels were not observed after entering along the working channel with a rigid scope to view them, and the field of view was blurred with more bleeding. The local doctor urgently required indwelling of a 16 F double-lumen catheter (used as a renal fistula) in the percutaneous renal puncture channel. A bladder balloon was injected with approximately 11 mL to compress the wound. No active bleeding was observed after the injection, and therefore, the operation was aborted. Postoperatively, a small amount of bloody fluid remained from the fistula. After the operation, the patient had repeated fever and abdominal distension. After conservative treatment for 2 days, no major improvement was observed. Therefore, she was urgently transferred to our department.
The patient had no history of hypertension, diabetes, or coronary heart disease. A physical examination at the time of admission to our department showed the following: a temperature of 38.7°C, abdominal swelling, soft abdominal muscle, no tenderness, rebound pain, and no bilateral lower extremity edema. A 16 F double-lumen catheter was inserted into the right kidney area and no fluid outflow was observed.
After admission to our department, a plain computed tomography (CT) scan (Figure 1) and CT venography (Figure 2) were performed. These scans suggested that thrombosis had occurred in the inferior vena cava and bilateral common iliac vein, and the right renal catheter penetrated the inferior vena cava. The result of an electrocardiogram was normal. An emergency in-hospital consultation was then performed. According to the results of this consultation, the main considerations for admission to our department were injury of the inferior vena cava by a foreign body (right renal fistula), bleeding, and infection after right PCNL. Empirical antimicrobial treatment, anticoagulation, and symptomatic supportive treatment by fluid replacement were performed. We closely observed whether there was recurrent blood, coagulation function, and other conditions, and paid attention to the fixation of the fistula to avoid traction and displacement caused by new injuries. After this treatment, the patient had no fever and the abdominal distension was relieved.

Plain computed tomographic scan shows a renal fistula penetrating the renal parenchyma through the dorsal skin.
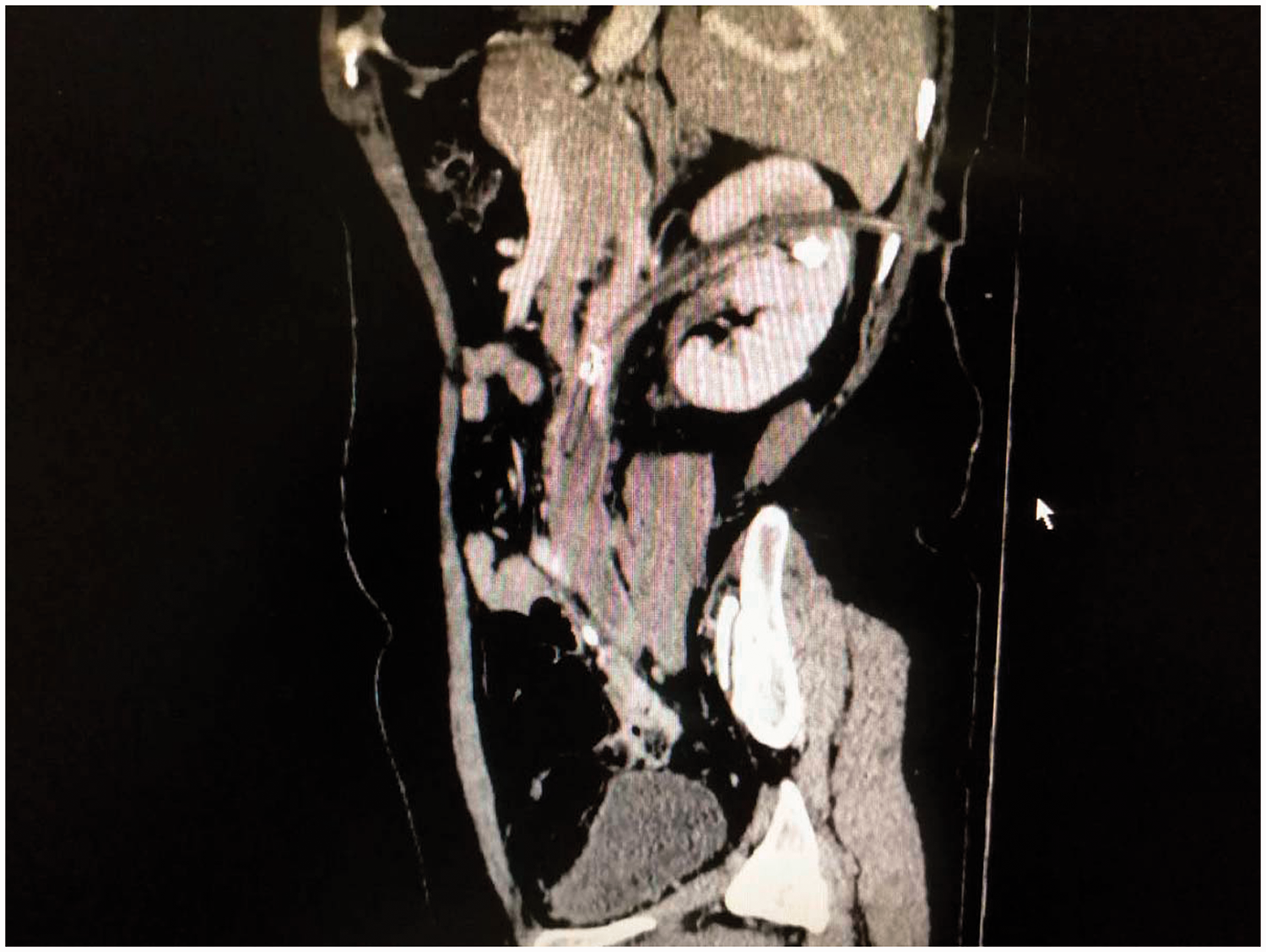
Computed tomographic three-dimensional reconstruction shows a fistula (ureter) through the renal parenchyma into the inferior vena cava with a thrombus around the balloon.
To prevent and cure the thrombus from falling off, we consulted with specialists at the Vascular Surgery, Interventional Medicine, and Hematology departments again. On the basis of this consultation, before the fistula was pulled out, a filter was placed, and the fluid in the bladder of the urinary duct was discharged to restore blood flow. Therefore, after actively improving preoperative preparation, inferior vena cava angiography plus vascular filter implantation and venous thrombosis plus balloon fluid extraction of the inferior vena cava foreign body (16 F urethral catheter) were performed under local anesthesia. A small amount of thrombus remained during the operation because of the large number of thrombi, and CT venography was performed after the operation (Figure 3). There was no postoperative bleeding. No major abnormalities were found in related indices, such as improved coagulation function and the international normalized ratio. Anticoagulation, and prevention and treatment of infection and other treatments were continued, and the catheter was gradually withdrawn. The catheter was completely withdrawn in 1 week. No bleeding was observed in the patient. During the treatment, renal function was normal and serum creatinine concentrations did not change.

Computed tomographic venography shows the insertion of an inferior vena cava filter with a small thrombus near the renal fistula (ureter) and its wall.
The patient was discharged from the hospital and continued to take rivaroxaban tablets for anticoagulation by oral administration. Coagulation function and other related indicators were rechecked regularly. If there was any discomfort, such as hematuria, the patient was instructed to return to the hospital for re-examination immediately. Three months later, she returned to the hospital for re-examination, and the thrombus had completely absorbed. After re-admission, the inferior vena cava filter was pulled out and the treatment ended. The patient was followed up for 2 years without any discomfort, such as hematuria, lumbago, and renal infection. An inferior vena cava ultrasound was performed (Figure 4). The ultrasound showed good filling of the venous lumen with no obvious abnormal reflux and no obvious thrombosis.

Inferior vena cava ultrasound after 2 years of follow-up shows good filling of the venous lumen with no obvious abnormal reflux and no obvious thrombosis. (a) Bilateral common iliac vein lumens were well filled with blood, no abnormal reflux was observed, and no abnormality was observed in a frequency spectrum. (b) There is no blood flow in the lumen of this segment of the vein. The right internal and external iliac veins are permeable, with smooth walls and no obvious thrombus. (c) The right internal and external iliac veins are filled with blood. The external iliac vein is red in the centripetal direction, and at the bifurcation, it turns to the internal iliac vein and is blue in the centrifugal direction.
Discussion
PCNL is still an important method for the treatment of upper urinary calculi. A previous study reported the complications of PCNL. 1 However, there have been few reports on renal vein vascular injury, especially inferior vena cava injury, and there are even fewer cases of recurrent thrombosis.2,3 However, regardless of whether the procedure of PCNL is endovascular or open, the current recommendations are that an inferior vena cava filter should be placed first to prevent dislodgement of thrombus. At the same time as the filter is placed, the thrombus can then be aspirated using endovascular luminal aspiration, and vibration is used to break up the thrombus and then aspirate it. An advantage of this method is that it is minimally invasive, but a disadvantage is that it is difficult to remove the thrombus when it is large or even growing. There is also another option of open surgery to remove the thrombus. An advantage of open surgery is that it is intuitive and can remove the thrombus more thoroughly, but a disadvantage is that it is more invasive.
Kotb and colleagues 3 reported a case of inadvertent insertion of a nephrostomy tube into the renal vein following PCNL. Finally, the nephrostomy catheter was pulled back into the renal pelvis under fluoroscopic visualization, but thrombosis formed. Resorlu et al. 5 only reported one case of misplacement of an ephrostomy tube into the inferior vena cava. Because of discovery of this insertion within 24 hours after surgery, the patient re-entered the operating room in a timely manner, and the catheter was successfully withdrawn under close monitoring, without obvious massive hemorrhage and thrombosis.
In our case, the surgeon failed to detect the lesion in the inferior vena cava early enough in the local hospital. The patient was transferred to our hospital 2 days after the operation. Because retention of the foreign body in the inferior vena cava was for a relatively long time, the catheter was inserted deeply, the bladder balloon was injected, and the blood circulation was affected, which resulted in thrombosis. After careful analysis of the causes of the thrombosis in this case, we speculate that the surgeon might have observed bleeding during the operation and tried to place a renal fistula through conventional methods 6 to stop the bleeding by compression. To achieve a better effect of hemostasis, a catheter was chosen for the renal fistula and compressed by a balloon of the inserted catheter. At that time, the location of the lesion was not clearly identified and the lesions were not monitored under ultrasound or X-ray before catheter placement. This led to the blind placement of the catheter in the inferior vena cava without knowledge of this location at the time. Filling the balloon with water at the same time caused further damage to the inferior vena cava. This caused difficulty regarding how to deal with safely removing the fistula. Our operation was slightly different from that used in three cases reported by Chen and his colleagues, 6 who used the one-step or two-step regression method. However, we agree with their opinion that withdrawal of the catheter depends on the penetration depth of the casing and whether there is considerable bleeding. In our case, because of the concern that the thrombus would fall off when the catheter was withdrawn, and because of the delay in time, the water-filled balloon could not eliminate adhesion in the inferior vena cava. Therefore, there should be active consideration for anticoagulation and temporary filter placement. 2 These treatments are important for the prevention and treatment of severe complications of pulmonary embolism caused by thromboembolism. During the anticoagulation process, short-acting heparin anticoagulation should be selected and the coagulation function should be monitored. Heparin should be stopped immediately if a bleeding tendency is found. A vascular strainer should be inserted as soon as possible to prevent and cure thrombosis. At the same time, most of the thrombus should be sucked out. Residual thrombus is absorbed by anticoagulant methods. In this case, unlike the one reported by Ge et al., 2 the inferior vena cava filter was removed 10 days after placement. In preparation for open surgery, we released the fluid out of the balloon. The catheter was removed to the calyces 2 days later, and the renal fistula was completely removed 1 week later. The three-step catheter was then completely removed. We chose to perform ultrasonic monitoring when exiting the fistula. If hemorrhage had been found, the open operation would have been changed immediately. After the above-mentioned comprehensive treatment, the fistula was removed smoothly, and no bleeding or emboli shedding complications were found. After the fistula was removed, anticoagulant therapy was continued. The thrombosis had completely absorbed as shown by a re-examination 3 months after discharge from hospital. The strainer was removed and the stent was removed. After follow-up, the patient was satisfied with the absence of thrombotic complications and the avoidance of open surgical catheter removal. Notably, not all patients are able to have their fistulas removed by the step-by-step method. In this case, open surgery to remove the tube and remove the remaining stones may be considered if the patient agrees. Fu and colleagues 7 reported two cases of intravenous misplacement of a nephrostomy catheter that were treated by open surgery and good results were achieved.
Conclusions
On the basis of our experience about the diagnosis and treatment of this patient, we suggest the following. First, after injury, patients should be treated as soon as possible, and CT or renal vein angiography should be performed. If thrombosis occurs, active intervention, multidisciplinary expert consultation, and joint diagnosis and treatment should be conducted. If there is no obvious active bleeding, anticoagulation should be carried out as early as possible. In the case of thrombosis, filter mesh should be placed as early as possible to prevent and treat pulmonary embolism and other complications. Second, when the intraoperative channel is unknown, the renal fistula should not be replaced with a urinary tube, and balloon compression should not be performed to stop bleeding. As in this case, where the catheter was placed in the inferior vena cava by mistake, injection of an air sac will only cause more damage. With regard to treatment, surgeons should be prepared for open surgery and prepare for bleeding. During the operation, the catheter can be withdrawn under ultrasonic or CT monitoring.
Supplemental Material
sj-pdf-1-imr-10.1177_03000605211058868 - Supplemental material for Management of inferior vena cava injury and secondary thrombosis after percutaneous nephrolithotomy: a case report
Supplemental material, sj-pdf-1-imr-10.1177_03000605211058868 for Management of inferior vena cava injury and secondary thrombosis after percutaneous nephrolithotomy: a case report by Pan Li, Dengjiu Mao, Jie Zhou and Hongmei Sun in Journal of International Medical Research
Footnotes
Acknowledgements
Ethical approval was provided by the First Affiliated Hospital of Hunan University of Medicine. We thank the patient for giving us permission to use her medical information for this publication. The authors would like to thank the entire operating team of the Clinic of Urology.
Author contributions
All authors read and approved the final manuscript.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Ethics statement
Written and signed consent to publish the case was obtained from the patient.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
