Abstract
The number of patients with heart failure with reduced ejection fraction (HFrEF) is increasing. These patients have a reduced cardiorespiratory reserve. Therefore, preoperative evaluation is essential to determine the best type of anaesthesia to use in patients with HFrEF. A 70-year-old man with HFrEF was scheduled to undergo debridement of skin necrosis due to thrombotic occlusion of the right common iliac artery. He had undergone wound dressing changes under local anaesthesia every other day for several months, and treatment for heart failure was on-going. A sciatic nerve and fascia iliaca compartment block was performed under ultrasound guidance because of the patient’s cardiopulmonary function. After confirming adequate sensory blockage, surgery was performed without any haemodynamic instability or complications. Thereafter, debridement was performed twice more using the same block technique, and a skin autograft was also successfully performed. We successfully performed an ultrasound-guided sciatic nerve and fascia iliaca compartment block in a patient with HFrEF who was scheduled to undergo lower limb surgery. Peripheral nerve block is an alternative option for patients with HFrEF.
Introduction
The prevalence of heart failure (HF) is increasing, 1 and anaesthesia for patients with HF is challenging because of the high risk of major adverse cardiovascular events. Patients with HF with reduced ejection fraction (HFrEF) have poor outcomes and high mortality owing to a reduced cardiorespiratory reserve. Therefore, risk assessment is required using preoperative serial measurement of B-type natriuretic peptide (BNP) concentrations and transthoracic echocardiography.1,2
Anaesthesiologists should conduct a pr-operative evaluation to ensure the patient’s safety, 2 and then the most appropriate anaesthetic technique should be used. The type of anaesthesia is chosen on the basis of these results, the patient’s condition, and the surgical site. An important factor is whether haemodynamics can be maintained. 3 Even modest sedation can cause haemodynamic and respiratory compromise in a patient with HFrEF. Therefore, careful dosing of sedatives or local anaesthetics is required during induction of general anaesthesia or neuraxial block. A neuraxial block in patients treated with anticoagulants also poses a risk of additional complications, such as haematomas. Several case reports have been published showing patients with cardiomyopathy or HFrEF in whom ultrasound-guided (USG) peripheral nerve block (PNB) can be safely performed for lower limb surgeries, providing haemodynamic stability and reducing complications.3–5
We successfully performed USG-guided PNB (sciatic nerve and fascia iliaca compartment block), while maintaining haemodynamic stability and preventing other complications in a patient with HFrEF who was scheduled to undergo lower limb surgery.
Case presentation
A 70-year-old man (170 cm, 48 kg, American Society of Anaesthesiologists status IV) had a history of HFrEF with dilated cardiomyopathy, diabetes mellitus, and chronic obstructive pulmonary disease. He was scheduled to undergo debridement of skin necrosis in the right leg. He had developed right leg weakness 4 months previously and was diagnosed with thrombotic occlusion of the right ilio-femoral artery. Skin necrosis appeared on the anterolateral side of the lower leg (Figure 1). While being treated for the skin lesion, his HF was treated with spironolactone, ivabradine, sacubitril/valsartan, and warfarin (1.5 mg) to optimise cardiopulmonary function. He had also received an implanted defibrillator 3 months previously.
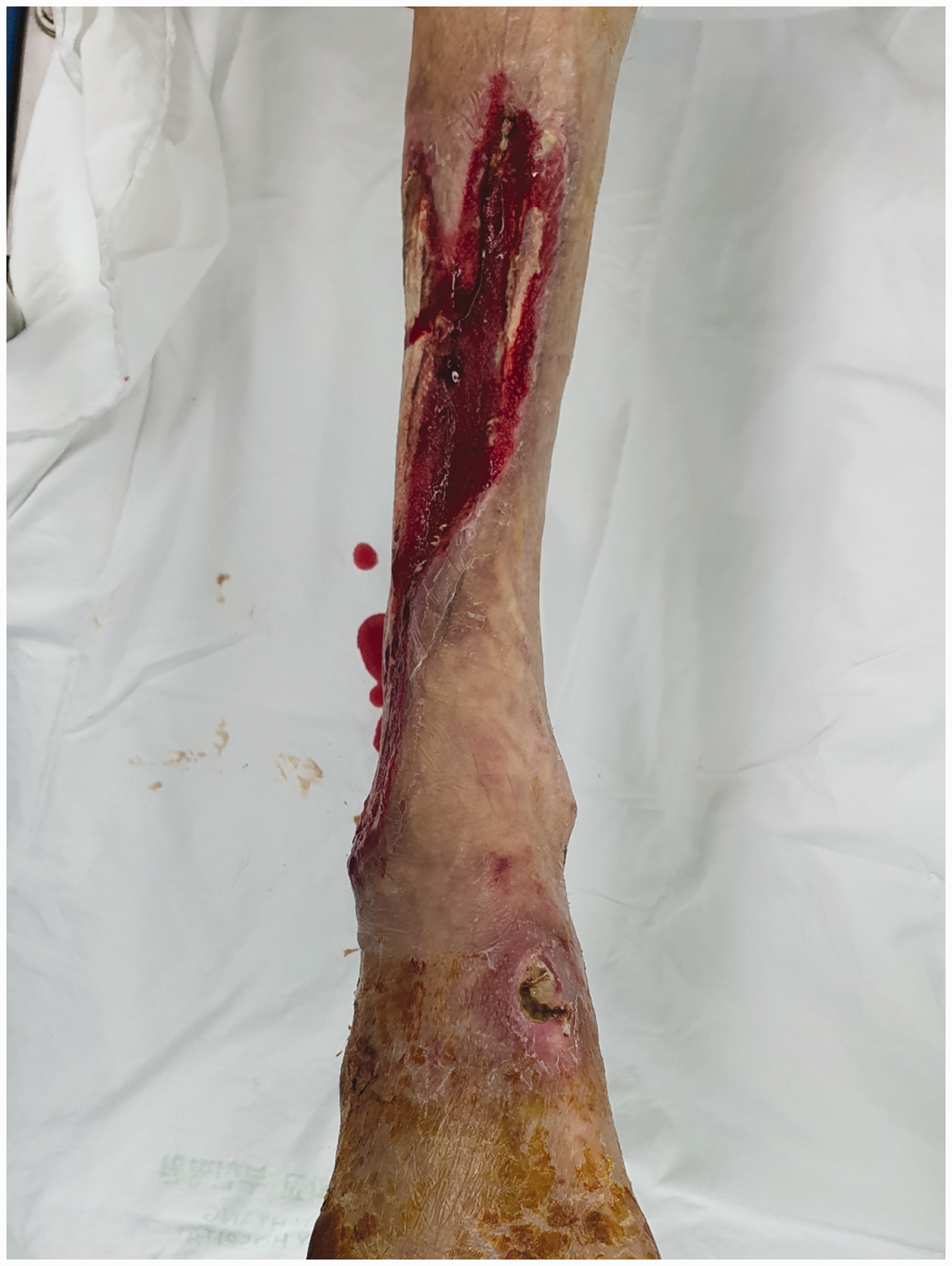
Photograph of skin lesions. Skin defects due to thrombotic occlusion of the right ilio-femoral artery can be seen on the right leg.
Despite inotropic administration, the patient’s systolic and diastolic blood pressure was 70 and 40 mmHg, respectively. His coagulation profile showed that the activated prothrombin time was 49.4 s and the prothrombin time/international normalised ratio was 1.63. However, anticoagulation therapy was continued because of the high risk of thromboembolism. The initial BNP level was 837 pg/mL, which decreased to 216 pg/mL just before surgery after treating the HF. Chest radiography showed pneumonic infiltration in the right lung (mainly in the right lower lobe) and diffuse emphysematous changes in both lungs (Figure 2). Preoperative transthoracic echocardiography revealed global hypokinesia with severe left ventricular dysfunction, an ejection fraction of 11%, an enlarged left atrium and ventricular chamber, and grade II diastolic dysfunction.
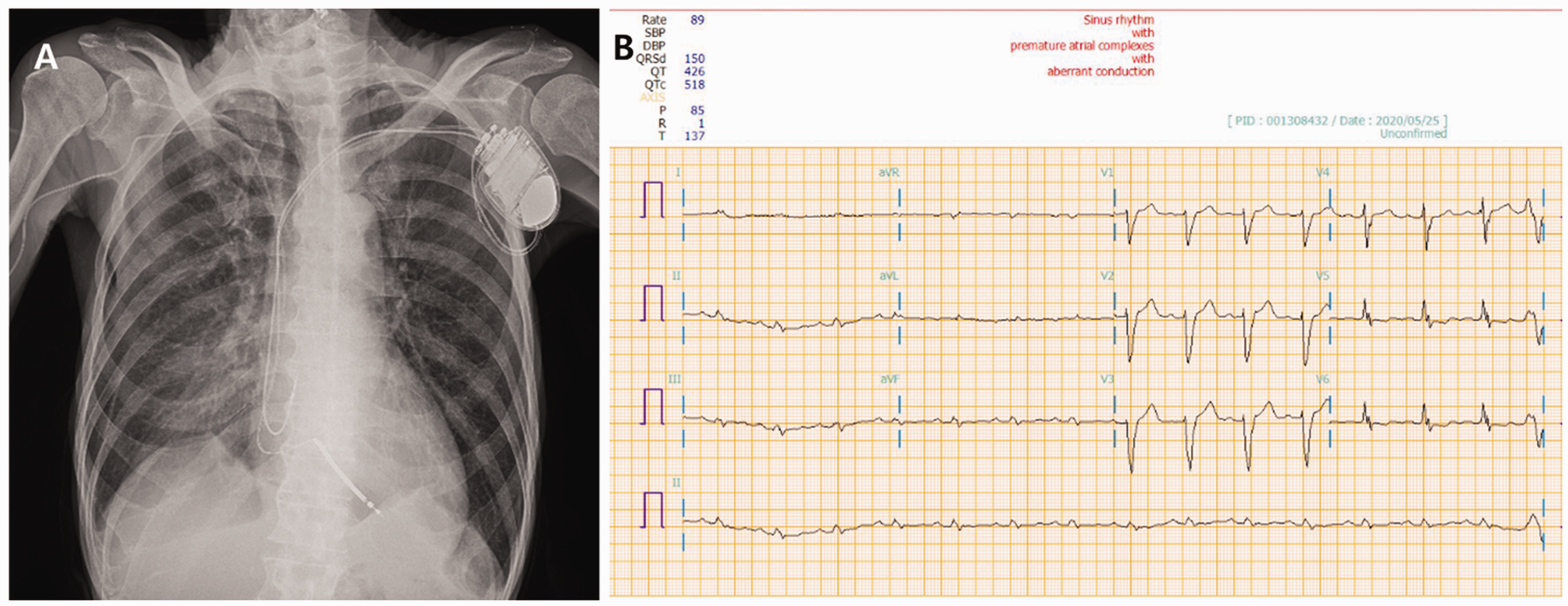
Preoperative chest radiographic image and an electrocardiogram. (a) Posteroanterior chest radiograph after receiving an implantable cardioverter-defibrillator. (b) Electrocardiogram before surgery.
Regional anaesthesia was considered safer than general anaesthesia because of the patient’s unstable cardiopulmonary function, but a neuraxial block was contraindicated owing to anticoagulation therapy. Therefore, we used a USG sciatic nerve and fascia iliaca compartment block to cover the operative field and avoid haemodynamic instability. However, the scheduled operation was postponed because the patient strongly requested only general anaesthesia and refused regional anaesthesia using a PNB. He had previously undergone wound dressing changes with local anaesthesia, and suffered from excruciating pain. Because of this previous experience, he was afraid that he might feel severe pain during the operation because of failure of the nerve block. Several counselling sessions were held to provide sufficient information to the patient, along with emotional support to overcome his fear and optimise the anaesthesia.
Standard monitoring, including non-invasive blood pressure monitoring, three-lead electrocardiography, and pulse oximetry, were applied before the nerve block, and the left brachial artery was cannulated for continuous blood pressure monitoring. Supplemental oxygen was administered through a facial mask at 5 L/minute. The patient was positioned laterally for the popliteal sciatic nerve block. A high-frequency linear transducer (HFL38x®; SonoSite, Bothell, WA, USA) was transversely placed on the posterior aspect of the popliteal fossa, and the sciatic nerve was located. Under real-time ultrasound (M-Turbo®; SonoSite) guidance, a 25 G needle was inserted 5 cm from the popliteal crease using the in-plane approach. Once the needle tip was near the distal sciatic nerve, 40 mL of 0.375% ropivacaine was injected around the sciatic nerve after confirming negative blood aspiration. Subsequently, the patient was placed in the supine position for the fascia iliaca compartment block. Using the same ultrasound transducer, the fascia lata and fascia iliaca were checked. A 20-mL aliquot of 0.25% ropivacaine was injected into the plane between the fascia iliaca and iliopsoas muscles after checking for negative aspiration (Figure 3). A loss of sensation was confirmed in the surgical area after 30 minutes. The surgery commenced after confirming adequate sensory block. During the operation, the patient did not require any analgesics or rescue block, and haemodynamic parameters were stable. The patient was transferred to the intensive care unit after surgery for close monitoring because of his severely compromised cardiopulmonary function. Haemodynamic stability was confirmed and he was transferred to the general ward the next day. Thereafter, the patient underwent wound debridement twice more and finally received a skin autograft at the defect site. All of these surgical procedures were successfully performed using the same PNB techniques. After the skin graft, the patient was discharged from the hospital without any symptoms, such as dyspnoea or surgical site pain.

(a) Ultrasound image of sciatic nerve block. (b) Ultrasound image of fascia iliaca compartment block.
The reporting of this study conforms to the CARE guidelines.
Discussion
Our patient had severely compromised cardiovascular function, and anticoagulation therapy was maintained during the perioperative period because the thromboembolic risk was too high. USG PNB was used for anaesthesia because of the patient’s physical status. Lesions were located on the lateral aspect of the distal leg and the medial aspect of the instep. We performed a USG popliteal block and fascia iliaca compartment block to cover all lesions. This procedure was successful during the intraoperative period and there were no complications. The patient did not complain of any pain or discomfort, and the haemodynamic parameters were stable.
When managing patients with severely compromised cardiovascular function, anaesthesiologists need to select an appropriate anaesthesia technique and carefully monitor vital signs to maintain haemodynamic stability during the perioperative period. Several studies have shown that PNB has many advantages compared with general anaesthesia, such as superior postoperative analgesia, improved postoperative mortality, intraoperative haemodynamic stability, and a reduced incidence of pulmonary complications.6,7 Additionally, PNB has several benefits compared with neuraxial anaesthesia. A previous study of patients who underwent diabetic foot surgery showed that the incidence of significant hypotension was higher in the spinal anaesthesia group than in the popliteal block group. 8 Therefore, anaesthesia using PNB may be a suitable choice to maintain haemodynamic stability and the analgesic effect.
The advantages of a USG nerve block over conventional approaches using a landmark, loss-of-resistance technique, or nerve stimulator are well known. Ultrasound guidance enables direct visualisation of anatomical structures, the needle pathway, and the distribution of local anaesthetics, and this visualisation accelerates the onset of blockade, increases accuracy, and reduces the dose of the local anaesthetic.9,10 However, potential complications of USG nerve block remain, including systemic toxicity of the local anaesthetic, direct nerve injury, vascular puncture, haematoma, block failure, and infection. 11
The patient’s physical status and any preoperative anxiety should be considered by anaesthesiologists. Preoperative anxiety is a common symptom during the perioperative period, and a preoperative visit from an anaesthesiologist can considerably assuage this concern, as in our case. 12 Mismanaged preoperative anxiety can negatively affect patients. 13 Therefore, a preoperative visit from an anaesthesiologist and counselling are recommended for patients who experience extreme anxiety. 14 These measures could be effective for reducing anxiety and promoting cooperation, through discussion of the current physical and psychological status of the patient, and the plan and options for anaesthesia. 14
In conclusion, a USG sciatic nerve and fascia iliaca compartment block was safely performed in a patient with HFrEF. USG PNB is a safe and useful anaesthetic method that should be considered for use in patients who are haemodynamically unstable and require continuous anticoagulation therapy.
Footnotes
Ethics statement
The study was approved by the institutional review board of Soonchunhyang University Bucheon Hospital (IRB approval no.: SCHBC 2020-07-042). Informed written consent was obtained from the patient for publication of this report and the accompanying images.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Soonchunyang University Research Fund.
