Abstract
We report on a fetus with cardiomegaly and increased middle cerebral artery-peak systolic velocity at 25 weeks of gestation. Severe fetal anemia (hemoglobin (Hb) level 37 g/L) was confirmed by cordocentesis. Hb analysis showed that Hb Bart’s was 9% in cord blood. Molecular analysis of the proband’s family found that the mother was a carrier of Hb Quong Sze (Hb QS,
Keywords
Introduction
Fetal anemia is a serious condition with various possible causes, including maternal alloimmunization, virus infection, fetal aneuploidy, vascular tumors, arteriovenous malformations of the fetus or placenta, and inherited conditions such as hemoglobinopathies or genetic metabolic disorders.1,2 Hemoglobinopathies are the main cause of non-immune fetal anemia and hydrops fetalis (NIHF) in Southeast Asia.
1
Hemoglobin (Hb) Bart’s disease and some homozygous or compound heterozygote Hb variants, such as Hb Constant Spring (Hb CS) and Hb Quong Sze (Hb QS), which are relatively common in Asia, can also cause severe fetal anemia and hydrops fetalis.3–5 Hb Zurich-Albisrieden (Hb ZA) (α2 59(E8)Gly>Arg;
Case report
A 31-year-old pregnant woman from Guangzhou, Guangdong Province, and her 32-year-old husband from Zhangzhou, Fujian Province, presented at our center at 25+3 weeks of gestation. Prenatal ultrasound examination at 25 weeks of gestation indicated fetal anemia with cardiomegaly (cardiothoracic area ratio 0.45, cardiothoracic diameter ratio 0.67) (Figure 1a), an enlarged placenta (3.3 cm), and increased fetal middle cerebral artery peak systolic velocity (MCA-PSV) (49.7 cm/s) (Figure 1b). There were no other structural anomalies. This was their first pregnancy. The couple agreed to participate in our study and signed informed consent for treatment and for publication. This study was approved by the Ethics Committee of Guangdong Women and Children Hospital (approval no.: 201901085) and the study was reported in accordance with the CARE guidelines. 9

Prenatal ultrasound at 25 weeks’ gestation showing cardiomegaly (a) and increased fetal middle cerebral artery peak systolic velocity (b).
The mother’s blood group was A, Rhesus-positive. Tests for cytomegalovirus, rubella virus, parvovirus, and syphilis infections, glucose-6-phosphate dehydrogenase deficiency, red blood cell antibodies, and feto-maternal hemorrhage using the Kleihauer–Betke test were all negative. Thalassemia testing showed that the mother was heterozygous for Hb QS(αQSα/αα). Her husband had decreased mean corpuscular volume (70.7 fL), mean corpuscular Hb (25.1 pg), and HbA2 (2.6%), but was normal for both α- and β-thalassemia according to suspension-array system analysis, which detected the 23 most frequent deletions and mutations in southern China. Sanger sequencing and multiplex ligation-dependent probe amplification were carried out to check the husband’s thalassemia status. Sanger sequencing identified a heterozygous G > C mutation at the first base of codon 59 of the
After genetic counseling, the couple decided to undergo umbilical cord blood puncture to determine the cause of the fetal anemia and prepared for fetal intrauterine transfusion (IUT). Routine fetal blood examination showed severe fetal anemia (Hb 29 g/L) and Hb electrophoresis showed significantly elevated Hb Bart’s (9.4%) (Figure 2). Suspension-array analysis and Sanger sequencing indicated that the fetus was compound heterozygous for Hb ZA and Hb QS. The hematological data and genotypes of the family are summarized in Table 1 and Figure 3. Fetal aneuploidies were excluded by chromosome karyotyping and chromosome microarray analysis. Screening for rubella virus and cytomegalovirus in the amniotic fluid and IgM antibody detection of rubella virus, cytomegalovirus, and parvovirus in umbilical cord blood were all negative. Whole-exome sequencing (WES) revealed no other genetic causes of fetal anemia. The fetal Hb pre-IUT was 29 g/L and the MCA-PSV pre-IUT was 49.7 cm/s. Infusion of 57 mL of concentrated washed red blood cells via the umbilical vein increased the post-IUT Hb and MCA-PSV to 91 g/L and 26.6 cm/s, respectively. Subsequent ultrasonography was performed every 2 weeks to monitor fetal development and anemia. Ultrasound examination at 35 weeks of pregnancy showed oligohydramnios (amniotic fluid index 42 mm), fetal growth retardation, cardiomegaly with cardiothoracic diameter ratio of 0.65 and cardiothoracic area ratio of 0.43, an enlarged placenta (48 mm), and increased MCA-PSV (84 cm/s). Fetal hemoglobin was 65 g/L, confirmed by cordocentesis. After counseling, the decision was made to terminate the pregnancy. Postmortem autopsy indicated fetal hydrops with cardiomegaly, ascites, bilateral pleural effusion, and right foot varus.

Hemoglobin analysis of fetal cord blood.
Hematological and genotypic data of the proband’s family.

TOP, pregnancy termination; Hb, hemoglobin; RBC, red blood cell count; HCT, hematocrit; MCV, mean corpuscular volume; MCH, mean corpuscular Hb; ZA, Zurich-Albisrieden; NA, not available
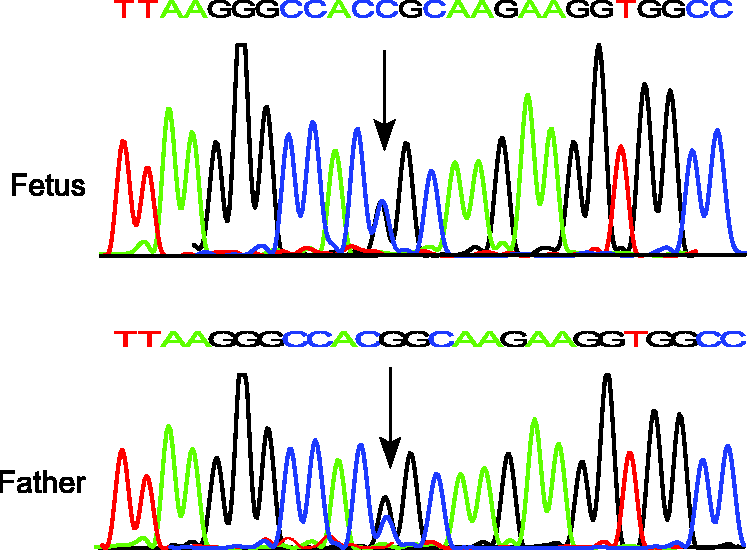
DNA sequencing of the
Discussion
Hemoglobinopathies are the most common inherited disorders worldwide. Hb variants caused by mutations in globin genes leading to structural changes in the Hb molecule are responsible for a group of hereditary Hb diseases, ranging from asymptomatic to severe clinical manifestations. Hb ZA is a highly unstable Hb variant, in which arginine replaces glycine at codon 59 in the
The common causes of fetal anemia and hydrops fetalis include maternal alloimmunization, parvovirus B19 infection, fetal aneuploidy, vascular tumors, arteriovenous malformations of the fetus or placenta, and inherited conditions such as α-thalassemia or genetic metabolic disorders. No aneuploidy was detected in the current fetus. Several monogenic disorders are also associated with fetal anemia, including dehydrated hereditary stomatocytosis, glucose-6-phosphate dehydrogenase deficiency, congenital erythrocyte membrane disorders, pyruvate kinase deficiency, lysosomal storage diseases, and Fanconi’s anemia. Further studies are needed to determine if high-throughput sequencing approaches such as WES are useful for the clinical management of hydrops fetalis. Given the large number of genes associated with NIHF, we propose that WES is necessary for the diagnosis of monogenic hydrops fetalis and may be required for the timely and efficient identification of monogenic NIHF.
