Abstract
Background
To identify the risk factors associated with rebleeding in obscure gastrointestinal bleeding (OGIB) patients from southern China.
Methods
This retrospective study involved 229 patients who underwent small bowel endoscopy in our hospital between 1 January 2018 and 1 December 2020. The clinical characteristics and risk factors related to rebleeding were retrospectively evaluated.
Results
Rebleeding patients were significantly older than non-rebleeding patients (53.0 ± 15.9 vs. 46.2 ± 17.8 years), had lower hemoglobin concentrations (89.2 ± 28.1 vs. 126.2 ± 25.1 g/L), and higher blood urea nitrogen concentrations (5.4 ± 2.6 vs. 4.5 ± 2.2 µmol/L), respectively. A higher percentage of rebleeding patients had diabetes mellitus (13.9% vs. 2.9%) and overt bleeding (70.4% vs. 38.6%), and required blood transfusions (43.1% vs. 8.0%), compared with non-rebleeding patients, respectively. Multivariate logistic analysis indicated that drinking alcohol (odds ratio (OR): 9.27; 95% confidence interval (CI) = 1.35–63.78), anemia (OR: 17.38; 95% CI = 5.48–55.10), and blood transfusion (OR: 3.76; 95% CI = 1.04–13.56) increased the risk of rebleeding in OGIB patients.
Conclusion
Our data suggested that OGIB patients who drink alcohol, have anemia, and require blood transfusion have an increased risk of rebleeding.
Keywords
Introduction
Obscure gastrointestinal bleeding (OGIB) is defined as gastrointestinal bleeding of unknown origin with negative initial endoscopy (colonoscopy and esophagogastroduodenoscopy) results. 1 It has been estimated that OGIB accounts for approximately 5% of gastrointestinal (GI) bleeding cases. 2 Previous studies have suggested that the bleeding lesions in OGIB are usually located in the small bowel. 3 The advent of small bowel capsule endoscopy (CE) and balloon-assisted endoscopy (BAE) has made detecting small bowel bleeding (SBB) possible.4,5
OGIB is generally categorized into two subtypes according to the American Journal of Gastroenterology Clinical Guideline. One type is overt bleeding, constituting patients with melena or hematochezia, and the other is occult bleeding, constituting patients without visible bleeding but with positive fecal occult blood test results.6,7 Thanks to the availability of CE and BAE, the diagnosis and treatment of OGIB have improved greatly; however, rebleeding remains a major challenge. Lai et al. 8 reported that the rebleeding rate in OGIB patients with positive CE findings reached 48.4%. Endo et al. 9 found that rebleeding occurred in 9.5% of OGIB cases after therapeutic intervention, and in 40% of cases who did not undergo therapeutic intervention. However, although important, the risk factors associated with rebleeding rates in OGIB cases are not yet fully understood.
In the present study, we investigated the clinical characteristics of OGIB patients from southern China and compared the characteristics between rebleeding cases and non-rebleeding cases. The aim of this study was to identify the risk factors associated with rebleeding rates in OGIB cases to make a contribution to the management of OGIB.
Materials and methods
Patients
This was a retrospective study, and the reporting of this study conforms to the STROBE statement. 10 This study involved 229 patients who underwent endoscopy for small bowel bleeding in the Department of Gastroenterology, Meizhou People's Hospital (Huangtang Hospital) between 1 January 2018 and 1 December 2020. All of the participants had negative upper and lower GI endoscopy results; 142 of these patients were diagnosed as having OGIB. Patients with OGIB underwent repeat CE or BAE to evaluate their recovery and to identify rebleeding cases. Patients with failed CE examination owing to CE retention, incomplete small bowel transit, or poor bowel preparation were excluded. The patients’ data were de-identified before data analysis, for privacy. The protocol for this study was approved by the Ethics Committee of Meizhou People’s Hospital (No: MPH-HEC 2017-A-30). All patients provided written consent for treatment.
Enteroscopy procedures
Patients with swallowing difficulties, suspected intestinal obstruction, cardiac pacemakers, or implantable electromedical devices were suggested to undergo balloon-assisted endoscopy (BAE) rather than CE. Patients undergoing either CE or BAE were required to fast overnight to clean the upper and lower GI tract. Four hours before the procedures, patients were required to take mannitol solution as standard bowel preparation.
CE was performed using a video capsule endoscopy device (PillCam SB2, or SB3; Given Imaging Ltd., Yokneam, Israel). Patients were instructed to swallow the CE capsule with dimethicone solution and wore the detection sensor and recording device for 8 hours. Images were analyzed with the RAPID Reader 6 software program on a RAPID 5 or 6.5 work station (Given Imaging Ltd.). The first recorded duodenal images and the first recorded cecal images were time-stamped, and the period between the two points was marked as small bowel transit time (SBTT). Lesion locations were reported by referring to the SBTT. In patients with positive findings during CE, BAE was used to confirm and possibly treat the lesions. BAE can be performed via oral and rectal approaches, depending on the CE findings. BAE was performed with a BAE system (Fujifilm, Saitama, Japan) using a Fujifilm EN-450T5, EN-530T, or EN-580T endoscope. Both CE and BAE were performed and analyzed by experienced gastroenterologists.
Endoscopic findings and diagnosis
The enteroscopic findings were divided into five groups: normal, diverticulum, tumors, vascular lesions, and ulcerative lesions. The endoscopic diagnosis was assessed by two experienced endoscopists.
Clinical characteristics
The patients’ clinical characteristics were obtained by reviewing their medical records, and the patients’ data were de-identified before analysis, for privacy. Clinical information constituted age, sex, smoking, drinking, hypertension, diabetes mellitus, blood transfusion, hemoglobin concentration, platelet count, blood urea nitrogen (BUN) and creatinine (CREA) concentrations, and comorbidities. Smoking was defined as one pack of cigarettes (20 cigarettes) per day or more; drinking was defined as alcohol consumption of ≥100 mL per day; hypertension was defined as systolic blood pressure/diastolic blood pressure (SBP/DBP) >140/90 mmHg; and diabetes was defined as fasting blood glucose ≥6.11 mmol/L and hemoglobin A1c (HbA1c) concentration ≥6.5%.
Definition of small bowel bleeding and rebleeding
OGIB was defined according to the following criteria: i) melena, hematochezia, or a positive fecal occult blood test result, and ii) negative upper and lower GI endoscopy results. In this study, OGIB manifesting as melena or hematochezia was considered overt bleeding, while OGIB manifesting as a positive fecal occult blood test results was considered occult bleeding.
Rebleeding was defined as recurrence of visible GI bleeding (hematochezia or melena) after endoscopy or medical treatment. OGIB cases without rebleeding during the study period served as controls.
Statistical analysis
Statistical analyses were performed using SPSS software, version 22.0 (IBM Corp., Armonk, NY, USA). Continuous variables were expressed as mean ± standard deviation (SD), while categorical variables were expressed as number (%). The Kolmogorov–Smirnov test was used to examine the normality of the distribution. Continuous variables were analyzed using Student’s t-test, and categorical variables were analyzed using the chi-square (χ2) test or Fisher’s exact test. The associations between the clinical variables and rebleeding were evaluated by logistic regression analysis. Odds ratios (ORs) were calculated by adjusting for variables that were distributed differently between patients with and without rebleeding. All tests were two-sided, and a P-value of <0.05 was considered statistically significant.
Results
Comparison of clinical characteristics between non-OGIB and OGIB patients
Of the 229 patients included in the present study, 142 were diagnosed with OGIB, and 87 were classified as non-OGIB. The clinical characteristics of the OGIB and non-OGIB patients are shown in Table 1. The average age of the OGIB patients was higher than for the non-OGIB patients (49.6 ± 17.1 vs. 44.9 ± 13.3 years, respectively; P < 0.01). The proportion of patients presenting with hypertension (21.8% vs. 6.9%; P < 0.01) or diabetes mellitus (8.5% vs. 0%; P = 0.006), or requiring blood transfusion (21.8% vs. 8.0%; P < 0.01) was significantly higher in the OGIB vs. non-OGIB groups, respectively. Comorbidities constituted cardiovascular disease, chronic kidney disease (CKD), liver cirrhosis, malignant tumors, and hematologic diseases. Greater percentages of OGIB patients suffered cardiovascular disease (11.3% vs. 2.3%; P = 0.02), malignant tumors (11.3% vs. 3.4%; P = 0.047), and hematologic diseases (21.1% vs. 6.9%; P < 0.01) vs. non-OGIB patients, respectively. Furthermore, OGIB patients had significantly lower hemoglobin concentrations vs. non-OGIB patients (107.3 ± 32.4 vs. 130.9 ± 19.2 g/L, respectively; P < 0.01).
Clinical characteristics between patients with non-OGIB and OGIB.

OGIB, obscure gastrointestinal bleeding; SD, standard deviation; BUN, blood urea nitrogen; CREA, creatinine.
The endoscopic findings for the 229 patients were analyzed and are shown in Table 2. Twenty-nine of 142 (20.4%) OGIB patients had normal endoscopy results, which was significantly lower than that in non-OGIB patients (P < 0.01). Ulcerative lesions were the most frequent endoscopic finding in both OGIB and non-OGIB patients, followed by tumors. Compared with non-OGIB patients, OGIB patients had a higher proportion of vascular lesions (8.5% vs. 1.1%, respectively; P = 0.02).
Endoscopic findings in OGIB cases.

OGIB, obscure gastrointestinal bleeding.
Rebleeding in OGIB patients
Rebleeding was observed in 72 OGIB patients (50.7%) after a 6-month follow-up. Table 3 shows a comparison of the characteristics between non-rebleeding and rebleeding patients. Rebleeding cases were significantly older than non-rebleeding cases (53.0 ± 15.9 vs. 46.2 ± 17.8 years; P = 0.017), had lower hemoglobin concentrations (89.2 ± 28.1 vs. 126.2 ± 25.1 g/L; P < 0.01), and higher BUN concentrations (5.4 ± 2.6 vs. 4.5 ± 2.2 mmol/L; P = 0.039), respectively. A higher percentage of rebleeding patients suffered diabetes mellitus (13.9% vs. 2.9%; P = 0.031) and overt bleeding (70.4% vs. 38.6%; P < 0.01), and required blood transfusion (43.1% vs. 8.0%; P < 0.01) compared with non-rebleeding cases, respectively. Notably, there was no significant difference in the endoscopic findings between non-rebleeding and rebleeding patients.
Risk factors for rebleeding in OGIB patients.
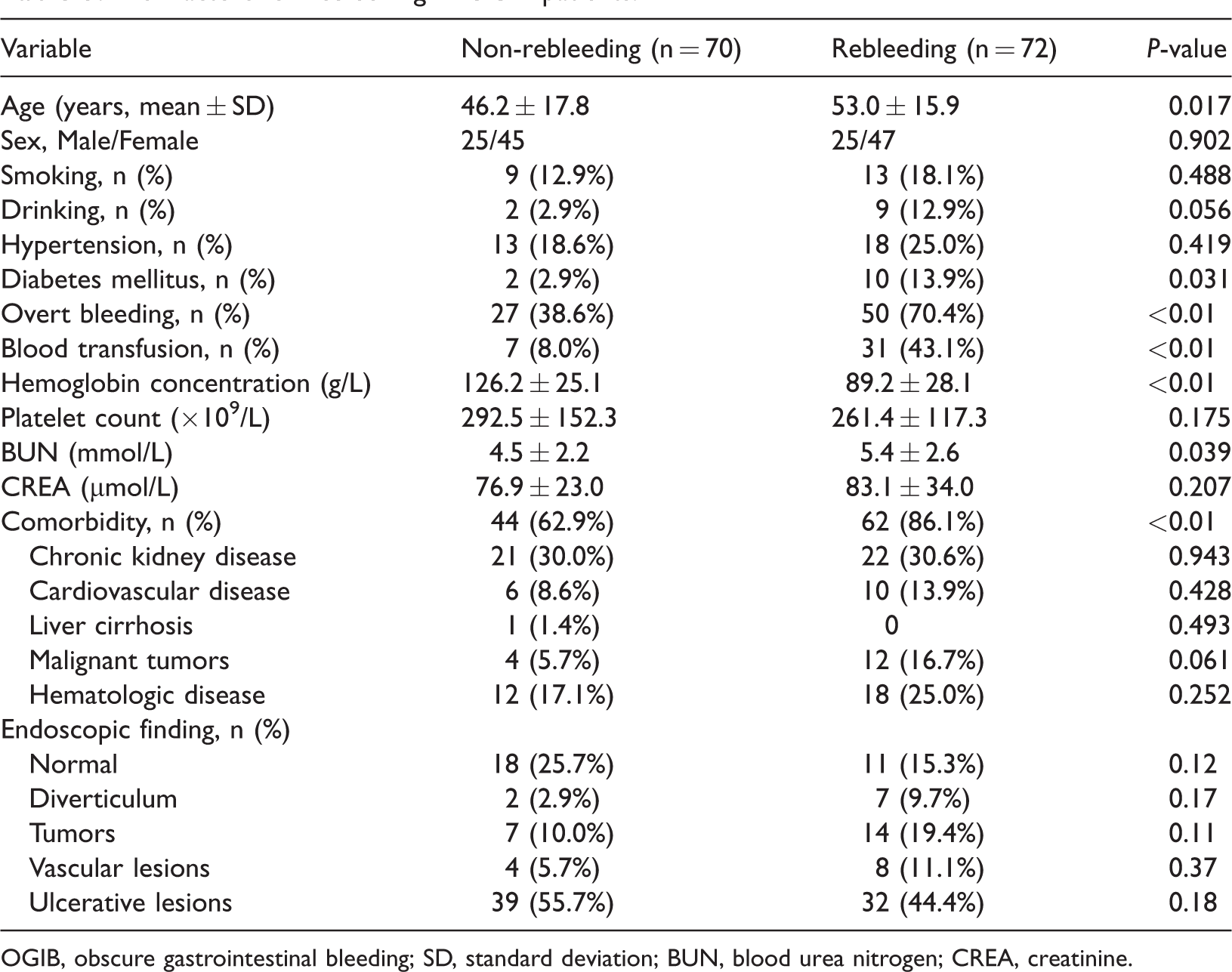
OGIB, obscure gastrointestinal bleeding; SD, standard deviation; BUN, blood urea nitrogen; CREA, creatinine.
Risk factors associated with rebleeding in OGIB patients
Logistic regression analysis was used to determine the risk factors for rebleeding in OGIB patients. Univariate analysis showed that drinking alcohol, diabetes mellitus, anemia, blood transfusion, and overt bleeding were significant risk factors for rebleeding. After adjusting for other factors, multivariate analysis indicated that drinking alcohol (odds ratio (OR): 9.27; 95% confidence interval (CI) = 1.35–63.78), anemia (OR: 17.38; 95% CI = 5.48–55.10), and blood transfusion (OR: 3.76; 95% CI = 1.04–13.56) increased the risk of rebleeding in OGIB patients (Table 4).
Predictors of rebleeding in patients with OGIB.

OGIB, obscure gastrointestinal bleeding; OR, odds ratio; CI, confidence interval.
Discussion
The clinical features of OGIB patients in southern China have rarely been reported. To investigate the possible risk factors for OGIB, we compared the clinical features and endoscopic results between non-OGIB and OGIB patients in this region. Although the development of CE and deep enteroscopy has greatly improved the diagnosis and treatment of OGIB, rebleeding cases occur frequently and remain an unresolved threat. Thus, identifying the risk factors associated with rebleeding rates is very important and could offer practical help in managing OGIB cases. This case–control study compared the clinical characteristics between rebleeding and non-rebleeding OGIB cases. Multivariate analysis revealed that drinking alcohol, anemia, and blood transfusion were independent risk factors for rebleeding in OGIB.
Increasing evidence has established that most bleeding sites in OGIB cases are located in the small intestine.3,11 Advances in small bowel imaging represented by CE and BAE enable endoscopists to determine the etiology of small bowel bleeding sources in most OGIB cases.12,13 Previous studies have suggested that possible small bowel etiologies in OGIB are angioectasias, ulcerative lesions, diverticulae, tumors, or non-steroidal anti-inflammatory drug use.14,15 We compared the clinical features between OGIB cases and non-OGIB cases, in whom gastrointestinal diseases were suggestive but who showed no significant abnormalities in upper and lower GI endoscopy. Our data suggested that older patients were vulnerable to OGIB. Hypertension, diabetes mellitus, blood transfusion, and anemia rates were higher, and comorbidities were more prevalent, in OGIB patients. Vascular lesions are reported to be a major small bowel enteroscopy finding in OGIB patients. 16 Consistently, we found that significantly larger proportions of OGIB patients had vascular lesions compared with non-OGIB patients.
The rebleeding rate in OGIB cases has been assessed in different studies, but the data varied. A study by Pinho et al. 17 revealed that the global rebleeding rate after endoscopic intervention was approximately 40%. Two systematic reviews reported rebleeding rates of approximately 45% and 42.7%, respectively, in OGIB patients with different follow-up times.18,19 In the present study, we observed a rebleeding rate of 50.7%, which is higher than in most previous studies. A major reason for this difference may be that some of the OGIB cases did not undergo effective treatment after the first endoscopy. Some studies identified the risk factors for rebleeding as advanced age, number of vascular lesions, anticoagulant medication, overt bleeding, and chronic renal disease.20–23 In other studies, vascular lesions were a reported predictive factor for rebleeding in patients with OGIB.24,25 However, in the present study, OGIB and non-OGIB cases presented with significant differences in some clinical features, such as age, diabetes mellitus, overt bleeding, BUN concentration, and comorbidities. Multivariate logistic analysis indicated that only anemia, blood transfusion, and drinking were independent risk factors for rebleeding in patients with OGIB, in this study. The need for blood transfusion has been reported to increase the rebleeding rate, 26 but to our knowledge, few studies suggested that anemia and drinking increase the risk of rebleeding.
There are limitations in this study. First, the retrospective design made it impossible to obtain the patients’ medication information when they were diagnosed with OGIB for the first time, which may have compromised the study’s conclusions. Second, the follow-up times varied greatly, which may have influenced the rebleeding rate. Third, we failed to evaluate the therapeutic interventions for rebleeding. One reason was that patients usually underwent combined interventions consisting of surgery, endoscopic therapy, and medications.
In conclusion, this case–control study provided knowledge about the clinical features of OGIB cases, and identified the independent risk factors for rebleeding. Our data suggested that drinking alcohol, anemia, and blood transfusion increase the risk of rebleeding in OGIB patients. Our findings may have practical meaning for the management of OGIB patients and preventing rebleeding.
Footnotes
Acknowledgments
The authors would like to thank the doctors in the Department of Gastroenterology for their help with this research.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This study was supported by the Fund of the Guangdong Provincial Key Laboratory of Precision Medicine and Clinical Translational Research of Hakka Population (2018B030322003).
Author contributions
XG designed the study and reviewed the draft. BL reviewed the medical reports and wrote the draft. SW and FW performed the endoscopy; SL and PW collected and analyzed the clinical data.
Availability of data and material
The datasets used and analyzed during the current study will be provided by the corresponding author upon reasonable request.
