Abstract
Objective
The present study aimed to evaluate the diagnostic accuracy of three-dimensional transvaginal ultrasonography (3D-TVS) for intrauterine adhesions (IUA).
Methods
We performed a retrospective cohort study. A total of 500 women aged 19 to 46 years with uterine lesions who received treatment from the Department of Obstetrics and Gynecology were enrolled. Endometrial 3D imaging was conducted to obtain the display plane and 3D-TVS parameters. Patients also underwent hysteroscopy for a definitive diagnosis.
Results
For diagnosing IUA, the sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), and overall accuracy of 3D-TVS were 98.8%, 90.8%, 91.4%, 98.7%, and 94.8%, respectively. For diagnosing a submucosal myoma, the sensitivity, specificity, PPV, NPV, and overall accuracy of 3D-TVS were 88.2%, 97.9%, 88.2%, 97.9%, and 96.4%, respectively. For diagnosing endometrial polyps, the sensitivity, specificity, PPV, NPV, and overall accuracy of 3D-TVS were 94.7%, 96.8%, 92.9%, 97.7%, and 96.2%, respectively.
Conclusions
Before hysteroscopy, 3D-TVS, as a method of screening, has great value for comparing differences before and after treatment, and for evaluating therapeutic effects.
Keywords
Introduction
In the normal menstrual cycle, the endometrium has periodic processes of exfoliation, proliferation, differentiation, and re-exfoliation. These processes maintain a high plasticity, dynamic regeneration, and differentiation of the endometrium, and prepare for embryo implantation. However, after intrauterine surgery or severe infection, the endometrium can be damaged by some serious injury, leading to secondary adhesions, which result in partial or complete closure of the uterine cavity. Intrauterine adhesions (IUA) are a disease that is common and frequently occurs in gynecology. The clinical manifestations of IUA include abdominal pain, secondary amenorrhea, infertility, and repeated abortion.1,2 Epidemiological surveys have shown that the incidence of IUA in patients has increased in recent years, especially in patients who receive treatment of uterine aspiration and curettage, where the incidence is as high as 25%.2,3 Without timely diagnosis and treatment, IUA induce deformation in the uterine cavity or lead to blockage of the fallopian tube, causing abortion or infertility.
Hysteroscopy (HS) is the gold standard for diagnosing IUA, and the degree, scope, and involved parts of adhesion can be visually and accurately displayed. However, HS is not widely used in clinical practice because it is an invasive examination with a complex operation and high cost. Hysterosalpingography is a common and effective method for determining IUA, and it is simple and easy to perform. However, hysterosalpingography is also an invasive examination, which is easily affected by other uterine lesions, and has poor repeatability. Two-dimensional transvaginal ultrasonography (2D-TVS) is noninvasive, relatively economical, and readily available. However, the sensitivity and specificity of 2D-TVS for diagnosing IUA are not good enough for clinical application. 3 As a non-invasive diagnostic method, 3D-TVS has been reported to compensate for the deficiencies of 2D-TVS, to detect pathological changes, and to assess the degree of IUA. 4 Therefore, this study aimed to evaluate the diagnostic accuracy of 3D-TVS in IUA, and to provide a basis for its selection in clinical diagnosis.
Materials and methods
Study population
This retrospective cohort study was conducted from June 2018 to October 2020 at the Department of Ultrasound. Consecutive patients, who were admitted to the Department of Obstetrics and Gynecology, were recruited when they met the following inclusion criteria: (1) patients were diagnosed with suspected IUA and had fertility requirements; (2) patients had a clear diagnosis by HS before ultrasonography; (3) patients who were willing to be followed up; (4) patients aged ≥18 years and between 22 and 45 years; and (5) patients who signed written informed consent voluntarily. The exclusion criteria were as follows: (1) patients were diagnosed with severe endometriosis and treated with a gonadotropin-releasing hormone agonist; (2) patients with a congenital uterine malformation; (3) patients with a previous history of pelvic tumor or radiotherapy; (4) patients with breast cancer or estrogen-dependent endometrial hyperplasia of a malignant tumor (bilateral endometrial thickness of 5 mm); (5) patients with uncontrolled hypertension and diabetes due to thromboembolic diseases, which were complications of severe liver and kidney diseases; and (6) patients who had ultrasound examination-associated contraindications.
The study was performed in accordance with the principles of the Declaration of Helsinki. The protocol of the current study was approved by the ethics committee of Huazhong University of Science and Technology Union Shenzhen Hospital (approval number: LW-2021-004). The requirement for consent of patients for inclusion was waived owing to the retrospective nature of the study and we de-identified the details of all patients who were enrolled. This was an observational, retrospective study, which was conducted on the basis of the Strengthening and the Reporting of Observational Studies in Epidemiology guidelines of the Equator network. 5
Three-dimensional TVS
Patients with endometrial polyps received 3D-TVS 3 to 5 days after menstruation and patients with IUA or submucosal myomas received 3D-TVS 5 to 7 days before menstruation. The GE-Voluson E10 (GE Healthcare, Chicago, IL, USA), with a transvaginal probe (RIC5-9-D), frequency of 3.0 to 14.0 mHz, and cavity content integration probe, was used as the apparatus for 3D-TVS in our study. Before the examination, the patients were required to empty their bladder, assume the lithotomy position, lie flat on the bed for the examination, and put on a condom. The end of the vaginal probe was smeared with a coupling agent and then the vaginal probe was placed inside the vagina, close to the cervix and vaginal fornix, by the operator. Multi-section and multi-directional scanning was then conducted. The uterus and bilateral attachments were routinely examined to observe the position, size, and shape of the uterine cavity, and the intimal thickness, presence of lesions, and changes in blood flow in the basal and intimal layers were analyzed. The sagittal section of the long axis of the uterus was used as the starting plane until the contour of the uterus and the endometrium were clearly displayed. The probe was fixed at a frequency of 0.6 kHz and the volume of 3D sampling was adjusted. The angle for scanning with the probe was subsequently set at 60° after the uterine cavity was enveloped by the energy of the Doppler sampling frame. The patients were asked to hold their breath to prevent artifacts from movement of the abdominal wall or viscera during breathing. Sampling of endometrial 3D imaging was conducted to obtain the display plane (A, B, and C). The rotation angle for the adjacent section surface was adjusted to 30° on the basis of the 3D database volumetric mode. The endometrium was traced on display plane A, and the endometrial thickness (ED), endometrial volume (EV), vascular index (VI), blood flow index (FI), and Vascular-blood Flow Composite Index (VFI) were calculated by the diagnostic software provided with the instrument.
HS
HS was performed at approximately 1 week after the vaginal ultrasound examination. The pressure of dilatation was set at 13.3 kPa and the rate of the flow was 260 mL/minute. Routine disinfection was performed and the patients were subjected to local anesthesia with 2% lidocaine. A hysteroscopic probe was inserted into the uterus through the uterine tube for the examination. The thickness, texture, color, blood vessels within the endometrium, and the relation between the endometrium and the surrounding tissues was observed and determined. For patients with suspected intrauterine space occupation, the site, size, scope, and shape of the lesion were observed, and a suspicious lesion was collected for a pathological examination. Based on the diagnostic results of HS (the gold standard), the accuracy of 3D-TVS in diagnosing IUA in patients with abnormal infertility was examined and reviewed.
Statistical analysis
Statistical analyses were performed using IBM SPSS 22.0 software (IBM Corp., Armonk, NY, USA). Data are reported as mean (standard deviation) or number (%). Outcomes were compared between two groups with the two-sided t-test for continuous variables and the chi-square test for categorical variables. The sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), Jorden index, and relative operating characteristic curve (ROC) analysis of 3D-TVS were calculated on the basis of the gold standard of pathology. All tests were two-sided and P<0.05 was considered to be statistically significant.
Results
Comparison of the diagnostic results of 3D-TVS and HS in patients with uterine lesions
A total of 500 female patients with uterine lesions who were aged 19 to 46 years were included in the present study. Using HS, 249 patients were diagnosed with IUA, 152 were diagnosed with endometrial polyps, and 76 were diagnosed with submucosal myomas. Additionally, 269 patients were diagnosed with IUA, 155 were diagnosed with endometrial polyps, and 76 were diagnosed with submucosal myomas following application of 3D-TVS (Table 1).
Comparison of results between 3D-TVS and HS in all patients with uterine cavity lesions.

3D-TVS, three-dimensional transvaginal ultrasonography; HS, hysteroscopy; IUA, intrauterine adhesions; EP, endometrial polyps; SM, submucosal myoma.
In the diagnosis of IUA, 3D-TVS showed that the normal shape of the inverted triangle uterine cavity was lost on the coronal surface of the uterus, along with disparity of the endometrial echo, which presented with different degrees of defects. Furthermore, a low-echo adhesion zone and rough edge were observed in the uterine cavity, and an angular side wall was found in severe cases in addition to “T”-shaped changes (Figures 1–3). The sensitivity, specificity, PPV, and NPV of 3D-TVS were 98.8%, 90.8%, 91.4%, and 98.7%, respectively. The overall accuracy was 94.8%.

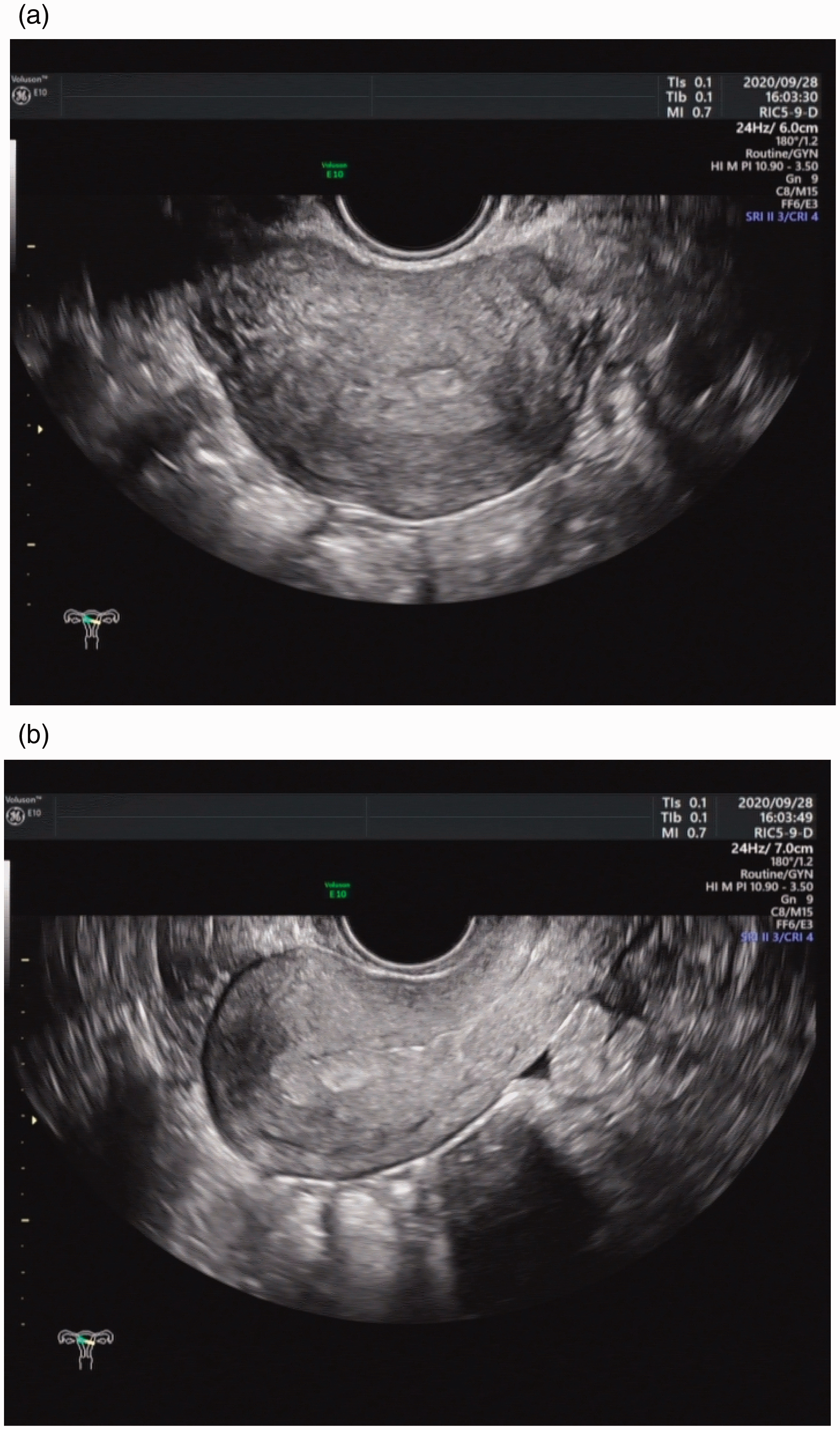
(a and b) Three-dimensional transvaginal ultrasonographic images of mild intrauterine adhesions.

(a and b) Three-dimensional transvaginal ultrasonographic images of moderate intrauterine adhesions.

(a and b) Three-dimensional transvaginal ultrasonographic images of severe intrauterine adhesions.
In the diagnosis of submucosal myomas, 3D-TVS showed protrusion of hypoechoic masses from the uterine wall to the functional cavity, with an oval or irregular shape. The basal part originated from the myometrium and protruded from the myometrium to the uterine cavity. On the basis of the relationship of the submucosal myoma with the myometrium, the submucosal myoma was divided into the following three types. Type 0 fibroids were defined as pedicled submucosal myoma, which did not expand to the myometrium. Type I fibroids were defined as submucosal myomas that expanded to the muscular layer, and coverage of the expansion was less than half of the myometrium. Type II fibroids were defined as submucosal myomas that expanded to the muscular layer, and coverage of the expansion was greater than half of the myometrium (Figure 4). The sensitivity, specificity, PPV, and NPV of 3D-TVS were 88.2%, 97.9%, 88.2%, and 97.9%, respectively. The overall accuracy was 96.4%.

(a and b) Three-dimensional transvaginal ultrasonographic images of submucosal myomas.
In the diagnosis of endometrial polyps, a single mass or multiple hyperechoic masses in the uterine cavity was displayed in 3D-TVS. The mass originated from the endometrial surface, varied in size, and usually had an elliptic shape. There was a clear boundary between the edge of the hyperechoic mass and the endometrium, with no interruption of the endometrial basement membrane and a visible separation gap in the uterine cavity (Figure 5). The sensitivity, specificity, PPV, and NPV of 3D-TVS were 94.7%, 96.8%, 92.9%, and 97.7%, respectively. The overall accuracy was 96.2%.
(a and b) Three-dimensional transvaginal ultrasonographic images of endometrial polyps.
Comparison of the diagnostic results of 3D-TVS and HS in patients with IUA
Sixty-eight patients were diagnosed with mild IUA, 81 were diagnosed with moderate IUA, and 97 were diagnosed with severe IUA by application of HS. Application of 3D-TVS showed that 71 patients were diagnosed with mild IUA, 82 were diagnosed with moderate IUA, and 93 were diagnosed with severe IUA (Table 2). Comparison of classification results between 3D-TVS and HS is shown in Table 3. For the diagnosis of mild, moderate, and severe IUA, the sensitivity, specificity, PPV, and NPV of 3D-TVS are shown in Table 4.
Comparison of severity of results between 3D-TVS and HS for intrauterine adhesions.

3D-TVS, three-dimensional transvaginal ultrasonography; HS, hysteroscopy.
Comparison of classification results between 3D-TVS and HS for intrauterine adhesions.

3D-TVS, three-dimensional transvaginal ultrasonography; HS, hysteroscopy.
Diagnostic efficacy of 3D-TVS for the severity of uterine cavity lesions.

3D-TVS, three-dimensional transvaginal ultrasonography; HS, hysteroscopy; PPV, positive predictive value; NPV, negative predictive value.
Three-dimensional TVS parameters of patients with IUA
There were significant differences in the ED, EV, VI, FI, and VFI among the four groups (all P<0.001). The ED, EV, VI, and VFI were significantly lower in the three IUA groups compared with the normal group (all P<0.05, except for the mild IUA group vs the normal group for the FI). The ED and EV in the moderate IUA and severe IUA groups were significantly lower compared with those in the mild IUA group (all P<0.05). The VI, FI and VFI in the severe IUA group were significantly lower compared with those in the mild IUA and moderate IUA groups (all P<0.05) (Table 5).
Comparison of three-dimensional transvaginal ultrasonographic parameters between patients with no IUA and patients with different severities of IUA.

Values are mean ±standard deviation.
aP<0.05, compared with the normal group; bP<0.05, compared with the mild group; cP<0.05, compared with the moderate group.
IUA, intrauterine adhesions; ED, endometrial thickness; EV, endometrial volume; VI, vascular index; FI, blood flow index; VFI Vascular-blood Flow Composite Index.
Discussion
IUA, which are also known as Asherman syndrome, are a common disease of gynecology. IUA affect the reproductive health in women and are defined as full or partial closure of cervical fibrous adhesions from various causes, such as trauma, infection, and uterine cavity or endometrial injury. This condition causes a series of clinical symptoms, such as a decrease in menstrual volume, amenorrhea, periodic abdominal pain, recurrent miscarriage, and secondary infertility, with serious effects on the function of menstruation and fertility in women of childbearing age. The pathological mechanism of IUA is mainly damage to the basal layer of the endometrium and the connection of non-vascular fibrous tissue to each wall of the uterus. Both of these types of damage result in an obstructed endometrium, amenorrhea, infertility, and other symptoms.4,6,7 The diagnosis of IUA is mainly based on the medical history, clinical manifestations, and an auxiliary examination. The medical history of IUA involves a history of a uterine operation, uterine infection, uterine artery embolization, or pelvic radiotherapy. Examinations of B-ultrasound, HS, and ultrasonography are used as auxiliary examinations for diagnosing IUA.8–10
HS is regarded as the gold standard for diagnosing IUA. However, the invasive nature and limited times for repetition of HS have resulted in an urgent need to develop some more non-invasive and simpler methods for screening. The value of intrauterine 3D-TVS has been determined in the diagnosis of IUA.
In 2015, according to the Consensus on intrauterine adhesions by Chinese experts from the gynecology and obstetrics branch of The Chinese Medical Association, an ultrasonic examination is the recommended method for screening IUA. In this study, the results of HS were considered as the gold standard. Additionally, the quality of ultrasound examinations was controlled by the physicians and conditions during the ultrasound examination and continuous dynamic observations. Three-dimensional TVS was applied to analyze various ultrasonic parameters to screen IUA and to evaluate the accuracy and scope of the intrauterine environment. 11
The utility of 3D-TVS in classifying the severity of IUA was successfully reported by Kim et al.'s study. 4 These authors found that the sensitivity of identifying IUA by using 3D-TVS was 98.8%, which is similar to previous reports.4,12 We also confirmed the accuracy of 3D-TVS for diagnosing endometrial polyps and submucosal myoma. On the basis of findings from 3D-TVS, IUA were classified into mild, moderate, and severe IUA; these findings were not fully consistent with the diagnostic results from HS. Among all patients who were enrolled in the current study, the accuracy of diagnosing IUA using 3D-TVS under HS was >90%, which is consistent with a previous report. 4 Additionally, on the basis of 3D-TVS results, we also classified several forms of IUA, including simple cervical or uterine adhesions or complex cervical and uterine adhesions. This classification was in agreement with HS findings. In this study, we also showed significant differences in parameters of endometrial flow in the diagnosis of IUA with clinical application of 3D-TVS. Our results suggest that 3D-TVS is a useful and accurate tool for predicting classification and diagnosis of IUA. Application of 3D-TVS can provide a vivid 3D perspective of the endometrial cavity, suggesting that 3D-TVS is a rapid and noninvasive modality for diagnosing IUA.
This study has some limitations. Endometrial biopsies in patients who received a normal HS and 3D-TVS were not collected for histological evaluation. There was an inherent bias for selection, which could have occurred because this retrospective study was performed at a single institution. Additionally, the operators of HS were not blinded to the outcomes of detection on 3D-TVS.
Conclusion
Our study shows agreement between HS and 3D-TVS for detecting uterine pathologies in patients. Although the features of ultrasound are not currently described in any system for classification of IUA, ultrasound may provide comprehensive information on various aspects of IUA, including intrauterine occlusion and obstruction, and endometrial functional status. Before performing HS, 3D-TVS, as a screening method, may have great value for comparing differences before and after treatment, and for evaluating therapeutic effects.
