Abstract
Objective
To evaluate the influence of insufficient bone cement distribution on outcomes following percutaneous vertebroplasty (PVP).
Methods
This retrospective matched-cohort study included patients 50–90 years of age who had undergone PVP for single level vertebral compression fractures (VCFs) from February 2015 to December 2018. Insufficient (Group A)/sufficient (Group B) distribution of bone cement in the fracture area was assessed from pre- and post-operative computed tomography (CT) images. Assessments were before, 3-days post-procedure, and at the last follow-up visit (≥12 months).
Result
Of the 270 eligible patients, there were 54 matched pairs. On post-operative day 3 and at the last follow-up visit, significantly greater visual analogue scale (VAS) pain scores and Oswestry Disability Index (ODI) scores were obtained in Group B over Group A, while kyphotic angles (KAs) and vertebral height (VH) loss were significantly larger in Group A compared with Group B. Incidence of asymptomatic cement leakage and re-collapse of cemented vertebrae were also greater in Group A compared with Group B.
Conclusions
Insufficient cement distribution may relate to less pain relief and result in progressive vertebral collapse and kyphotic deformity post-PVP.
Keywords
Introduction
Osteoporotic vertebral compression fractures (VCFs) are common in elderly patients and can result in chronic back pain, spinal deformity, decreased quality of life and increased mortality1,2 Conservative treatments, such as bed rest, analgesics, external bracing, and antiresorptive medications are generally considered primary therapy for acute VCFs.3,4 However, some patients fail to respond to conservative treatment and have persistent pain and progressive functional limitation.5,6 Over the past few decades, percutaneous vertebral augmentation (PVA) which includes percutaneous vertebroplasty (PVP) and percutaneous kyphoplasty (PK), has been widely accepted as a safe and effective procedure for the treatment of painful VCFs. By injecting bone cement into the fractured vertebrae, this technique can rapidly relieve pain, partially restore vertebral height (VH), and provide biomechanical stability.7–10 However, inadequate pain relief and re-collapse of cemented vertebrae are not uncommon after the procedure. Studies have suggested that absent or insufficient cement filling in the unstable fracture area of the vertebral body may be a risk factor for inadequate pain relief after the initial surgery.11,12 In addition, these studies demonstrated that bone cement distribution during unilateral or bilateral PVP was associated with recompression of the cemented vertebrae, loss of VH ratio and cement leakage, which ultimately affects treatment outcome. We undertook a retrospective matched-cohort study to investigate the influence of cement distribution in the fracture area on outcomes following PVP for acute VCFs.
Methods
Patients
This retrospective matched-cohort study included patients 50–90 years of age who had undergone PVP for a single level VCF at the First Affiliated Hospital of Guangzhou University of Chinese Medicine, from February 2015 to December 2018. These patients had experienced no apparent improvement of their VCFs following conservative medical treatment and physical therapy. Patients excluded from the analysis had the following: presence of pathologic compression fractures (i.e., spinal metastatic cancer, primary tumours, or infection); neurologic deficits or spinal cord compression syndrome; burst fracture or fracture areas involving at least two parts of the index vertebrae; pre-operative height loss of the fractured vertebra of more than two-thirds of the normal vertebral bodies in the adjacent levels; history of VCF surgery; index vertebra with indistinct magnetic resonance imaging (MRI); history of diabetes; severe VCF (i.e., vertebral body collapse <one-third of its original height).
Percutaneous vertebroplasty
Location of the vertebral fractured area was defined as the line-shape area with low signal intensity on both the T1-weighted and the T2-weighted sagittal plane MRI images (Figure 1b, c and d) and low signal intensity on Spin Echo with Triple Inversion Recovery (STIR) images (Figure 2d). Pre-operative sagittal and coronal computed tomography (CT) scans confirmed the compression fracture line; the line-shape cleft connected with the breach of vertebral cortex (Figure 2b and 2c).

64-year-old female patient was diagnosed with a T12 osteoporotic vertebral compression fracture (VCF) after a fall. (a) Pre-operative lateral X-ray of the lumbar spine showing compression of the T12 vertebral body. (b-d) Sagittal T1WI, T2WI, STIR magnetic resonance imaging (MRI) scans of the lumbar spine shows a line region with low signal located below the superior plate of the T12 vertebral body; this was considered as the vacuum cleft after reduction of the compression fracture. (e) T12 Percutaneous vertebroplasty (PV) was performed; the lateral film of the thoracolumbar X-ray shows the height and Cobb angle of the vertebra had improved. (f and g) Post-operative computed tomography (CT) scan shows bone cement insufficiently diffused in the fracture line with a partial vacuum cleft in the vertebral body. (h) Vertebra collapse 13 months post-operation and the index vertebra can be seen to be worse than pre-surgery; this could be defined as progressive kyphosis deformity of the thoracolumbar spine.

73-year-old female patient was diagnosed with an L1 osteoporotic vertebral compression fracture (VCF). (a) Pre-operative lateral X-ray of the lumbar spine showing that compression of the L1 vertebral body. (b and c) Pre-operative sagittal and coronal computed tomography (CT) scans show a compression fracture line with denser bone located below the endplate of L1 and linked to the disrupted site of the anterior and lateral vertebral cortex (red arrow). (d) Sagittal Spin Echo with Triple Inversion Recovery (STIR) and magnetic resonance imaging (MRI) scans of the lumbar spine showing a bone compression zone with low signal located in the corresponding site on CT (red arrow). (e) Lateral X-ray of the lumbar spine three days post-operation showing that the bone cement is adequately distributed in the vertebral body and the height and Cobb angle of the vertebrae has improved. (f and g) Post-operative CT scan showing that the bone cement is well dispersed within the fracture lines. (h) A CT scan taken 15 months post-surgery showing that there is no progressive collapse in the index vertebrae.
The PVP procedure was performed with patients in an extended prone posture through bilateral pedicle approach according to an established standard procedure. 13 Local anaesthetic (0.5%–1% lidocaine) was injected into a lumbar facet joint. Thereafter, a 13–gauge bone biopsy needle (Kyphon Kurve, Medtronic Plc, Dublin, Ireland) was inserted into the fractured vertebral body. Bone cement (Mendec Spine PMMA; Tecres SPA, Verona, Italy) was injected under fluoroscopic guidance using a simple syringe in the lateral and anterior-posterior planes. The cement injection started in the anterior third or quarter of the vertebral body and was completed when the cement reached the posterior quarter of the vertebral body. Vital signs (i.e., electrocardiogram [ECG], blood pressure [BP], and oxygen saturation [SpO2]) were monitored during the procedure. Patients were encouraged to walk as soon as possible and were treated with calcium and vitamin D supplements.
Outcome Assessments
Patient data were extracted from the hospital’s electronic medical records system. Pre-operative evaluations included: physical examination; conventional radiography (Figures 1a and 2a); multi-planar reconstruction of CT scans; MRI; bone mineral density (BMD) evaluations. Post-operative evaluations included: X-rays (Figures 1e and 2e); multi-planar reconstruction of CT scans (Figures 1f, 1g, 2f and 2g).
Pre-operation, 3-days post-operation, and at the last follow-up visit, clinical and radiographic outcomes were evaluated using: visual analogue scale (VAS) pain scores on a 0–10 scale (0 represents no pain, 10 represents worst pain); Oswestry Disability Index (ODI) score (0 [minimum]–100%[(maximum]); kyphotic angle (KA, the angle between the superior end plate one level above and the inferior end plate one level below the injured segment); 14 vertebral body height (VH, this was taken from a standing lateral radiograph and was the endplate-to-endplate distance measured in cm from the anterior aspect of the injured vertebral body. 15 Complications related to the PVP procedures (i.e., PVP cement leakage, adjacent vertebral fracture, re-collapse of cemented vertebrae) were also recorded.
Maldistribution of bone cement in the fracture area was assessed by three independent spinal surgeons from the pre- and post-operative CT images. Any ambiguity was resolved by consensus. As previously described, 16 insufficient bone cement distribution in the fracture area of the index vertebra was recorded when the distribution was less than half of the fracture area observed on post-operative coronal or sagittal CT scans (Figures 1f and 1g). By contrast, sufficient bone cement distribution in the fracture area of the index vertebra was confirmed when the distribution was more than half of fracture area observed on post-operative coronal and sagittal CT scans (Figures 2f and 2g). According to the relationship between bone cement and fracture area on post-operative CT scans, eligible patients were separated into two groups: Group A (insufficient cement distribution) and Group B (sufficient cement distribution). Similar to a previous study, 17 Group A patients were matched one-to-one with Group B patients. The matches were made using Excel software (version 2007; Microsoft Corp., Redmond, WA, USA) by one of the investigators (S.L.) who was blinded to the radiological status of the patients. Matching characteristics included: age (within 1 year); sex; weight (within 5kg); severity of osteoporosis (BMD within 0.5 standard deviation); duration of pain (within 7 days); major curve magnitude (Cobb angle within 10°); pre-operative VAS scores, KA, and VH (within 5cm).
The study was approved by the Ethics Committee of The First Affiliated Hospital of Guangzhou University of Chinese Medicine (No: 2017-057) and all patients provided written informed consent.
Statistical analyses
Data were analysed using the Statistical Package for Social Sciences (SPSS®) for Windows® release 17.0 (IBM Corp., Armonk, NY, USA). All tests were two-sided and a P-value <0.05 was considered to indicate statistical significance. Data were reported as mean ± standard deviation. Differences between groups were compared using the χ2 test for categorical variables. Continuous data were compared using Student t-tests for normally distributed variables. Comparison of pre-operative, post-operative, and follow-up VAS scores, ODI scores, KA and VH were analysed using Wilcoxon signed-rank test.
Results
From February 2015 to December 2018, 760 subjects were diagnosed with a single level VCF at our spinal surgery department. Of these, 270 patients (82 men, 188 women) underwent PVP of the thoracolumbar spine (T10-L2), had complete information pre- and post-surgery for at least 12 months (median follow-up, 24 months; range, 12–76 months) and were eligible for our study (Figure 3). According to the relationship between bone cement and fracture area on postoperative CT scans, 54 patients (8 men, 46 women) had maldistribution or insufficient distribution of bone cement in the fracture area and were allocated to Group A. By contrast, 216 patients had adequate or sufficient bone distribution. From these subjects, 54 individuals (8 men, 46 women) were selected based on matched demographic characteristics to Group A and were allocated to Group B.

Flow diagram of the patient selection process.
Baseline characteristics of Groups A and B are shown in Table 1. The selected 108 patients (16 men and 92 women) had a mean age of 71 years (range, 52–89 years) and average disease duration of 25 days (range 14–60 days). All patients had a confirmed diagnosis of osteoporosis, with an average BMD, T-score of −3.3 (range −2.5–−4.8. PVP procedures were successfully completed in all patients without severe complications.
Comparison of baseline characteristics between groups.

Values are shown as mean ± SD, or n (%).
Abbreviations: ns, not statistically significant
Post-operative values for VAS scores, ODI scores, KA, and VH taken 3-days post-surgery improved in both groups compared with pre-operative values (Table 2). In addition, VAS and ODI scores in each group improved markedly from 3-days post-surgery to the last follow-up visit.
Comparison of outcome measures between groups.
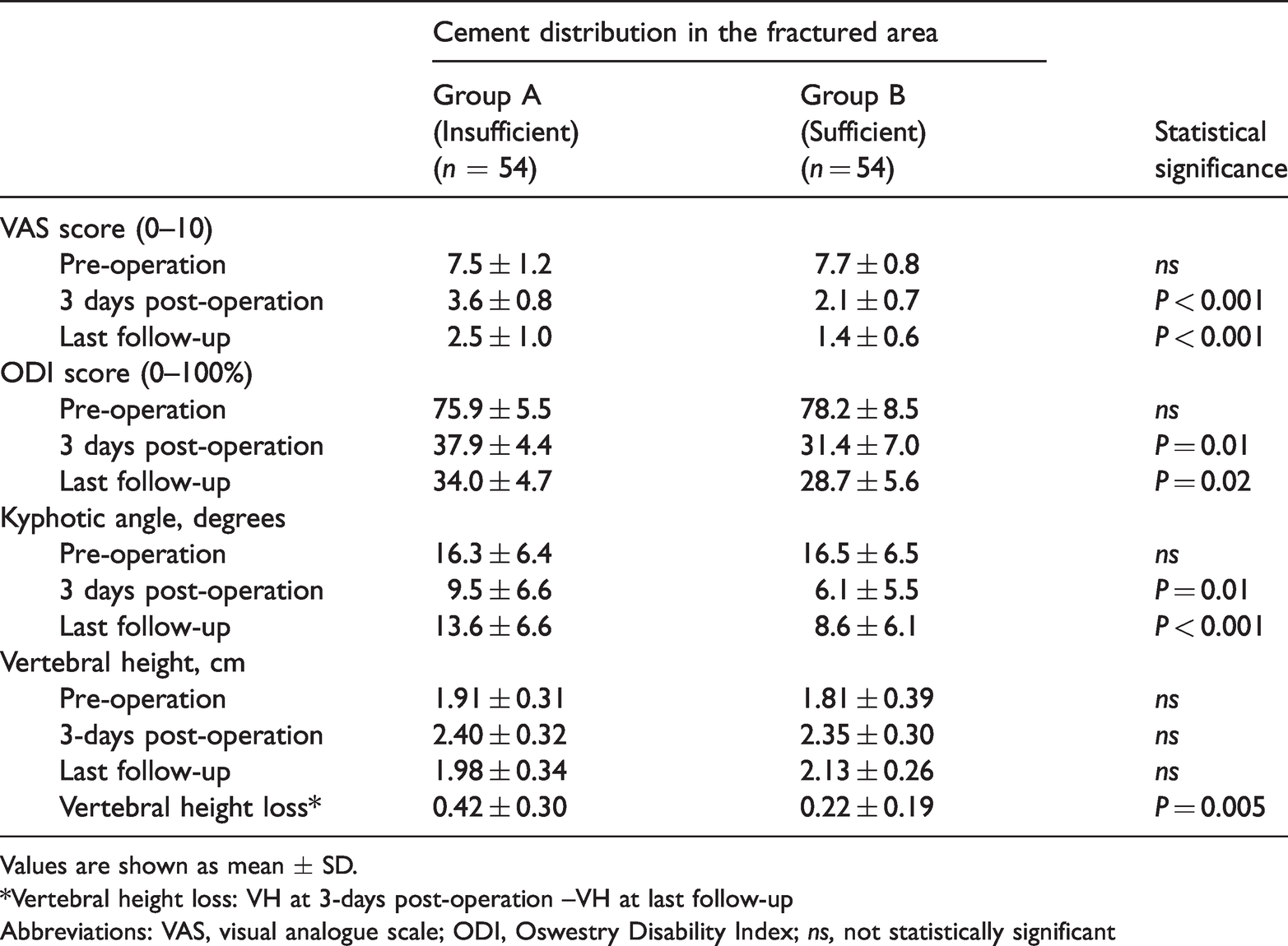
Values are shown as mean ± SD.
*Vertebral height loss: VH at 3-days post-operation –VH at last follow-up
Abbreviations: VAS, visual analogue scale; ODI, Oswestry Disability Index; ns, not statistically significant
Significantly better VAS scores were observed 3-days post-surgery and at the follow up visit in Group B compared with Group A (P < 0.001). In addition, significantly better ODI scores were observed 3-days post-surgery and at follow up visit in Group B compared with Group A (P = 0.01 and P = 0.02, respectively).
Following the PVP procedure, KA was significantly greater in Group A compared with Group B at 3-days post-operation and the last follow-up visit (P = 0.01, P < 0.001, respectively). Although there was no difference between groups in VH at 3-days post-operation and the last follow-up visit, VH loss (i.e., VH at 3 days -VH at follow up) was greater in Group A than in Group B (P = 0.005).
Based on pre-operative sagittal and coronal CT scans, all fracture areas in Group A and Group B were below the superior endplate. The average volume of cement injected was 4.9 ml (range, 2.5–9 ml) and more cement was injected in Group B than in Group A (P = 0.03, Table 3).
Comparison of bone cement implantations and complications between groups.

Values are shown as mean ± SD, or n (%).
Abbreviations: ns, not statistically significant
The incidence of bone cement leakage and re-collapse of cemented vertebrae was significantly greater in Group A compared with Group B (P = 0.044 and P = 0.01, respectively) (Table 3). However, there was no difference between Groups in the incidence of adjacent vertebral fractures (15% vs 9%) (Table 3).
Discussion
Although VH restoration and prompt relief of pain should be expected after PVP, re-collapse of augmented vertebrae, persistent back pain due to augmented VH ratio, osteonecrosis, intravertebral cleft, non-cement-endplate-contact, and enhanced pre-operative KA have been observed following the surgical procedure.15,18–21 However, it remains unclear if persistent or worsening pain and re-collapse of augmented vertebrae are procedural-related or part of the natural course of osteoporosis.
Several studies suggest that bone cement distribution in the fractured vertebrae may be a crucial factor in the pain relief following PVP.11,12,22 Although small and retrospective, one study in 15 patients reported that repeated PVP at the same vertebral level was effective in abating unrelieved pain following the initial procedure which may have been caused by absent or inadequate filling of cement. 11 Interestingly, a large retrospective study, involving 226 patients, suggested that the incidence of inadequate cement distribution was high in patients who had the fractured area located in the superior portion of the index vertebra. 16 However, it is difficult to evaluate dominant risk factors related to unsatisfactory outcomes following PVP because the specific mechanisms of pain relief from the procedure are unclear. While restoring strength, stiffness, stabilization of fractured vertebrae, and minimizing micro-motion of the endplates and trabecular bone are thought to be the main mechanisms for pain relief from PVP, damage to algesiroreceptors in or around the fractured vertebrae through chemical toxicity and thermal effects of the injected cement may adversely affect the treatment outcome.23–26
Data from our present, retrospective, matched-cohort study suggests that sufficient cement distribution in the fracture area does play a critical role in the outcome of PVP. Although pain scores decreased in all patients following PVP, our results indicated that insufficient cement distribution in the fracture area leads to inadequate pain relief in the short and mid-term post-operatively. It has been suggested that insufficient cement distribution could lead to a significant displacement of the fractured vertebrae which may result in notable micro-motion around the fracture and result in unrelieved pain. 27
We found that at the last follow-up visit, KA was significantly higher in Group A compared with Group B, and VH loss was greater in Group A compared with Group B. The importance of sufficient cement distribution in the fracture area to lessen the probability of unsatisfactory pain relief and vertebral re-collapse following PVP should be emphasised. We suggest that a targeted injection procedure could assist in ensuring sufficient cement distribution in the fracture area. To this end, the fracture area should be evaluated and located in pre-operative CT and MRI scans. From these images, the target of the cement injection should be identified. To enable the bone cement to permeate easily around the fracture area, the tip of the injection needle should be positioned beside the fracture area under the guidance of fluoroscopy. In addition, although the preferred surgical approach to PVP remains controversial, we suggest that bilateral PVP would provide a symmetrical distribution of bone cement in the fracture area. Furthermore, while this study showed no difference between Group A and Group B in BMD, we suggest that BMD may affect outcomes because osteoporosis of the fractured vertebrae may influence the distribution of the bone cement. Based on the pathology of osteoporosis, low bone density often correlates with large trabecular separation of the vertebral body, so the bone cement could have more room for “running,” which could lead to better diffusion of the cement.
Our results showed that a larger cement volume was used during the PVP procedures in Group B compared with Group A, and cement leakage, which alerted surgeons to stop the injection of bone cement intra-operatively, occurred more frequently in Group A than Group B. However, although adjacent vertebral fractures during follow-up were more common in Group A compared with Group B (15%vs. 9%) the difference was not statistically significant.
The study had several limitations. Firstly, although the two groups were comparable in baseline data, we compared the clinical outcomes these patients through a non-random retrospective method with a relatively small sample size and assessed short or mid-term outcomes. Other influencing factors, such as severity of VCF, were not considered. Secondly, approximate observations from post-operative CT scans were used to assess cement distribution because it was difficult to gain accurate measurements from planar images. Moreover, data from the CT scans may have been affected by the positioning of the patient which was not always consistent. Finally, it was difficult to distinguish between the fracture area and the area with bone oedema due to bone bruise seen in the MRI scans. Therefore, the definition of sufficient/insufficient cement distribution in the fracture area was subjective and based on ‘eyeballing’. Therefore, further research is needed on the long-term outcomes regarding cement distribution in the fracture area following PVP.
In conclusion, insufficient bone cement distribution in the fracture area following PVP is associated with less pain relief and may result in progressive vertebral collapse and kyphotic deformity.
Footnotes
Declaration of conflicting interests
The authors declare that there are no conflicts of interest.
Funding
This work was supported by Scientific Research Project of Guangdong Traditional Chinese Medicine Bureau (20172043), National Natural Science Foundation of China (81774338, 81503591) and Guangdong Province Health Bureau(2016A030313645).
