Abstract
Ovarian vein thrombosis (OVT) is a rare medical disorder, which is most often found in the immediate postpartum period. OVT is rarely considered idiopathic. We report a case of idiopathic OVT with pulmonary embolism in a 33-year-old woman who presented with abdominal pain. Computed tomography and postoperative pathology confirmed the diagnosis of idiopathic OVT. To date, only 12 cases of idiopathic OVT have been reported. In this case report, we present a summary of these cases and a review of literature regarding management of idiopathic OVT.
Keywords
Introduction
Ovarian vein thrombosis (OVT) is a relatively rare, but serious disease, which commonly occurs in postpartum women. OVT is usually associated with some other diseases, such as pelvic inflammatory disease, malignant tumors, sepsis, enteritis, and recent pelvic or abdominal surgery. 1 The incidence of idiopathic OVT is extremely rare. Only a few cases of idiopathic OVT have been reported to date in healthy patients with unknown etiology. Earlier diagnosis and anticoagulant therapy are required to prevent potential complications and adverse sequelae of OVT. 2 , 3 We report a case of idiopathic OVT with pulmonary embolism in a 33-year-old woman who presented with abdominal pain. This case demonstrates the risk of pulmonary embolism in patients with idiopathic OVT.
Case presentation
We report a case of a 33-year-old woman who presented to our outpatient department complaining of abdominal pain. The patient had suffered from pain in the right lower quadrant for approximately 2 years, and it occurred once or twice a month without precipitating factors. The abdominal pain lasted for approximately 30 minutes and was relieved without special treatment every time. She presented to our outpatient department because the abdominal pain had worsened and occurred weekly for 1 month. Her symptoms were not related to meals, bowel movements, or her menstrual cycle, which was normal. No oral contraceptives or other medical history, recent pregnancy, or abdominal surgical history was noted, and she had a normal vaginal delivery 9 years previously. She had no identifiable pelvic inflammatory disease risk factors and no personal or family history of coagulation system related diseases. Her vital signs were stable. A physical examination showed mild tenderness on palpation of the right lower quadrant. No obvious mass was found and bowel sounds were present. A gynecological examination was unremarkable.
Laboratory tests, including liver, kidney, and pancreatic function, were normal. The urine β-human chorionic gonadotropin level was negative. An electrocardiogram, and chest and abdominal X-ray showed no considerable changes. A routine blood test showed moderate anemia (hemoglobin: 89 g/L), and white blood cell and platelet counts were normal. The fibrin degradation product level was 12 mg/L and the D-dimer level was 4.4 mg/L in a coagulation test. Abdominal computed tomography (CT) was performed, which suggested a right ovarian vein mass and pulmonary embolism (Figures 1 and 2). Contrast-enhanced ultrasound showed a mass in the right ovarian vein, without blood flow into the right renal vein. Serum tumor markers were detected to exclude malignant lesion, including carcinoembryonic antigen, carbohydrate antigen 19-9, carbohydrate antigen 125, and alpha-fetoprotein. The results of these markers were all negative. Other laboratory tests were performed to exclude coagulation disorders, including protein C, protein S, lupus anticoagulant, factor V Leiden mutations, and antithrombin III, and these were also negative.
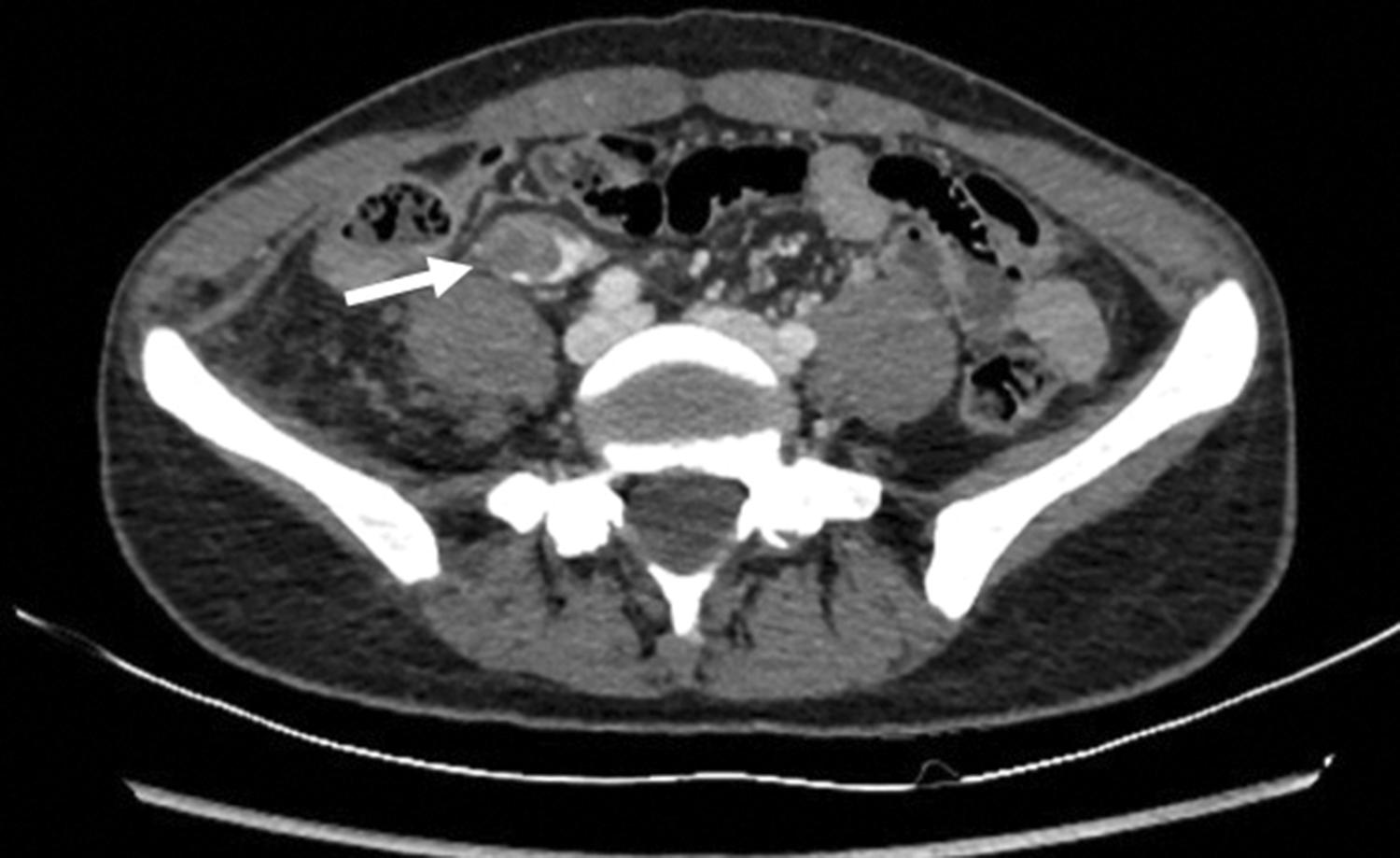
Computed tomography (cross-sectional view) of the abdomen and pelvis. The white arrow shows an ovarian vein mass.

Computed tomography (cross-sectional view) of the chest. The white arrow shows pulmonary embolism.
Laparotomy was performed with an initial diagnosis of an ovarian vein mass and possible intravenous leiomyomatosis of the right ovarian vein. During the operation, we observed a right varicose ovarian vein without obvious dilation (Figure 3). Therefore, the varicose ovarian vein was totally removed, and thrombus was found in the ovarian vein. The thrombus started from the distal end of the right ovarian vein, and spread to two thirds of the total length of the right ovarian vein. A frozen pathological examination showed smooth muscle hyperplasia in the vessel wall, small focal degeneration, and necrosis with calcium deposition. No malignant sign was found. At this point, the diagnosis of this patient was clear. Paraffin pathology showed vascular tissue with internal thrombus formation, focal hyperplasia of smooth muscle tissue with focal mucus degeneration, and no tumorous lesions. No abdominal pain occurred after the operation, and she was discharged 1 week later on therapeutic anticoagulation with rivaroxaban for 3 months. She was followed up regularly for 1 year with no symptom of abdominal pain.

Photograph during surgery. The white arrow shows a right varicose ovarian vein.
Literature review
A comprehensive bibliographic search of PubMed was performed using the following Search MeSH terms: [((idiopathic) OR (nonpregnant)) AND ((“ovary, vein thrombosis”[MeSH Terms] OR (“ovarian”[All Fields] AND “vein thrombosis”[All Fields]) OR “ovarian vein thrombosis”[All Fields] OR “gonadal vein thrombosis”[All Fields] OR (“vein thrombosis”[All Fields] AND “ovarian”[All Fields])))]. The search was limited to articles published from January 2005 to November 2020. All citations identified were selected for abstract review. Abstracts that did not relate to case report/series or those with themes not related to idiopathic OVT were excluded. The remaining publications were selected for full-text evaluation and those considered relevant were included for final review. After the first cycle of review, cross-reference searches were performed until all relevant publications were reviewed.
Relevant data were then extracted from case descriptions. Clinical/patients’ characteristics included abdominal pain, fever, and other symptoms, such as vomiting and nausea. Diagnostic data included oral contraceptives or other medical history, recent pregnancy, abdominal surgical history, Doppler ultrasound images, abdominal CT scans, and thrombophilia tests. Additionally, the type of therapeutic intervention and outcomes were collected.
The flowchart results from our search are shown in Figure 4. Fifteen relevant citations from January 2005 to November 2020 were retrieved from PubMed. All abstracts were evaluated and 11 were selected for full-text review. Four records were excluded after abstract review because they were not based on idiopathic OVT. The 11 identified studies were retrieved in full and cross-reference searches were performed, which identified a further study that reported idiopathic OVT. Thirteen cases were related to idiopathic OVT, including our case, and were reviewed. The demographics and clinical information of these 13 cases, including our case, are shown in Table 1.2,4,6–15 The ages of these 13 patients ranged from 27 to 67 years, with a mean age of 41.7±15.8 years.

Flowchart of the literature search on November 2020.
Documented cases of idiopathic ovarian vein thrombosis.

Discussion
Idiopathic OVT is an extremely rare condition that mainly occurs in postpartum women and may have serious complications. We experienced idiopathic OVT with pulmonary embolism in a 33-year-old woman who presented with abdominal pain. To the best of our knowledge, 12 cases of idiopathic OVT have been reported in the PubMed database in the past 15 years (Figure 4). OVT is an uncommon occurrence that mainly affects women in the puerperium state, especially early postpartum. 3 There is an unequal incidence of OVT in women with vaginal delivery (0.18%) and cesarean section (2%) in their postpartum period. 4 OVT is also associated with gynecological malignancies, recent abdominal and pelvic surgeries (especially hysterectomy and salpingo-oophorectomy), pelvic inflammatory disease, and other thrombosis. 3 Diagnosis of Idiopathic OVT should exclude conditions, such as postpartum, malignancy, pelvic inflammatory disease, recent surgery, and any other risk factors that can easily lead to a hypercoagulable state. 1
All of the 13 patients with idiopathic OVT found in a literature search had the symptom of abdominal pain, 5/13 had symptoms and signs involving the digestive system, such as nausea and vomiting, 1/13 had a low fever, and 1/13 had an abdominal mass.2,4,6–15 These results indicate that abdominal pain may be the primary symptom of idiopathic OVT. In patients with other types of OVT, their clinical symptoms are usually fever, pelvic pain, and a right abdominal mass. 5
Identification of OVT relies on a prompt and thorough examination. Although results of Doppler ultrasound were missing in four previous patients with idiopathic OVT, most patients who had Doppler ultrasound showed some positive findings (7/9). These findings included an echogenic nodular structure within a dilated vein or a tubular hypoechoic lesion in the flank area. Therefore, we suggest that Doppler ultrasound may be used as the first screening technique for idiopathic OVT because it is a convenient, non-invasive, and economical method. However, in most cases, Doppler ultrasound was not able to examine the entire length of the ovarian vein, which requires further examination such as a CT scan. Diagnosis and the range of thrombus were confirmed by CT in all previous patients with idiopathic OVT, except for one in whom a CT scan was not performed. We believe that an abdominal CT scan can provide reliable evidence for the diagnosis of idiopathic OVT.
Thrombus of most (10/13) patients with idiopathic OVT was located in the right ovarian vein, which is similar to patients with other types of OVT. This may be due to the long length of the right ovarian vein, right shift of the uterus, and relative insufficiency of the right ovarian vein valve. 7
OVT is at risk for pulmonary embolism, which occurs in 25% of patients with postpartum OVT and expansion of thrombus into the inferior vena cava and renal veins. 6 Pulmonary embolism occurred in a previous idiopathic OVT case 10 and the current case. One of these patients complained about chest pain after the diagnosis of OVT; therefore, a chest CT scan was performed and pulmonary embolism was found. Our patient had no symptoms of pulmonary embolism, but her abdominal CT scan showed subsegmental pulmonary embolism incidentally. Therefore, we suggest that, for patients with symptoms such as chest pain or other symptoms of pulmonary embolism, a chest CT scan should be performed after diagnosis of idiopathic OVT. Fortunately, the thrombus of these two patients was small, and caused no severe symptoms, such as hypoxemia.
At present, there is no guiding opinion for treatment of OVT. 2 Systemic anticoagulation for these patients may achieve a favorable outcome for resolution of symptoms and prevention of life-threatening complications. 1 All 13 previous patients with idiopathic OVT were provided anticoagulant therapy, ranging from 6 weeks to 6 months. Two patients used rivaroxaban and the rest were treated with warfarin. Most patients’ abdominal pain resolved after anticoagulation, and only one patient still had occasional pain. The imaging follow-up of some cases was missing. For the seven patients with follow-up information, thrombus completely resolved in one patient, one patient had partial resolution, and one patient had no change.4,6–8,11,12,14 In addition to pulmonary embolism, ovarian infarction, sepsis, and death are potential severe complications of OVT, but these complications did not occur in the group of patients with idiopathic OVT.14,15 Idiopathic OVT is not caused by pelvic inflammatory disease, malignant tumors, enteritis, recent pelvic or abdominal surgery, and other factors for OVT. Therefore, idiopathic OVT may have a slower disease progression and a lower risk of infection compared with OVT. This may explain why symptoms of fever and serious complications, such as ovarian infarction and sepsis, are unlikely to occur in idiopathic OVT.
Conclusion
Idiopathic OVT is at risk for pulmonary embolism, and it is usually characterized by abdominal pain and may not be accompanied by fever. For patients with sudden abdominal pain, but without risk factors for OVT, the possibility of idiopathic OVT should still be considered. To date, anticoagulant therapy is the primary treatment for idiopathic OVT.
Footnotes
Ethics statement
Case reports are exempt from the requirement of IRB approval in our institute. Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the Editor of this journal.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author contributions
WRL was involved in protocol/project development, data collection and management, data analysis, and manuscript writing. SSC was involved in project development, collection of images, data analysis, and manuscript writing. RMZ was involved in data collection and analysis, and review and editing of the manuscript. XMC was involved in project development, and review and editing of the manuscript. All authors have read and approved the manuscript.
