Abstract
Background
Sinonasal teratocarcinosarcoma (SNTCS) is a highly invasive malignant tumor most frequently found in the nasal cavity and paranasal sinuses. As a result, it can be confused with other sinonasal tumors. In addition, SNTCS progresses rapidly and often infiltrates other tissues or organs in the early phase, resulting in poor patient prognosis. The objective of this article was to report the case of a patient with SNTCS and discuss the management strategy. Furthermore, we conducted a literature review for SNTCS and summarized the findings from 107 cases.
Conclusions
As SNTCS progresses rapidly, early diagnosis and surgical treatment combined with radiochemotherapy can improve patient survival.
Keywords
Introduction
Sinonasal teratocarcinosarcoma (SNTCS) is a highly invasive malignant tumor that often arises in paranasal sinuses. Because it is not easy to identify by appearance, the gold standard diagnostic criteria are based on pathologies, such as malignant epithelial and mesenchymal components, including smooth muscle and cartilage.1–3 Treatment of this carcinoma is mainly through surgery, radiation, and chemotherapy, but the overall survival of patients remains unsatisfactory. Improving clinical outcomes is challenging owing to the aggressive and rapid progression, recurrence, and intracranial extension of SNTCSs. In this study, we report a case of SNTCS and conduct a literature review to discuss the diagnosis and treatment of this tumor.
Case presentation
Clinical history
In 2014, a 47-year-old man with a 2-month history of recurrent right nasal hemorrhage and obstruction was admitted to our hospital. He was first diagnosed with olfactory neuroblastoma by local biopsy at a previous hospital (the details were unclear). He then visited our hospital for further evaluation and treatment.
Imaging
A preoperative computed tomography (CT) scan revealed that the right frontal, maxillary, ethmoid, and sphenoid sinuses and nasal cavity were filled with soft tissue, and the right turbinates were obstructed. In addition, the bony wall between the maxillary and ethmoid sinuses was thin (Figure 1a–d). Chest CT revealed no evidence of metastasis.

a–d: Preoperative computed tomography scan of a 47-year-old male patient with sinonasal teratocarcinosarcoma. Analysis of the coronal section of the nasal cavity and sinuses revealed a soft tissue lesion (indicated by the red arrowhead) in the right ethmoid sinus (a, b), part of the frontal sinus, sphenoid sinus, maxillary sinus, and right nasal cavity (c, d). The orbit, cribriform plate, and nasal septum appeared normal (a, c), except for thinning of the bone of the right ethmoid and maxillary sinus. e–h: Postoperative magnetic resonance imaging scan showing minimal inflammatory edema in the right maxillary sinus (e, f), and operative regions showed no sign of recurrence (g, h).
Nasal endoscopy
Preoperative endoscopy revealed no abnormalities in the left nasal cavity (Figure 2a). The right nasal cavity was fully obstructed by a large purple-red neoplasm, and other anatomical structures were obscured (Figure 2b).
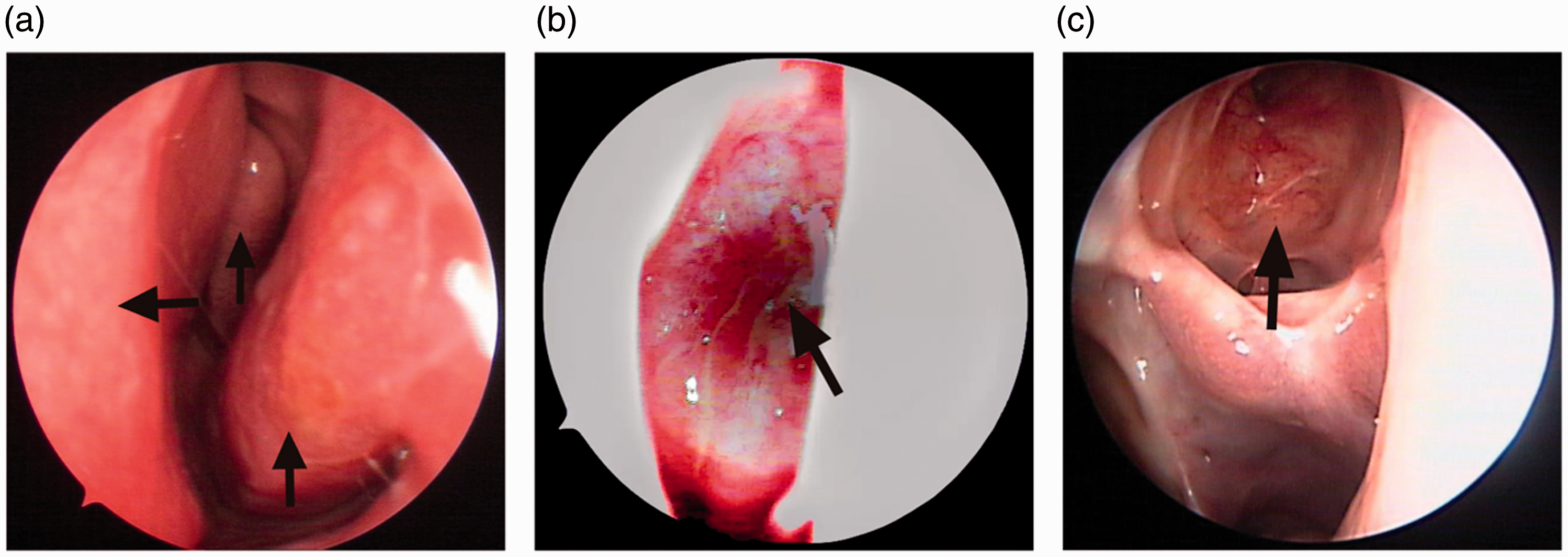
Preoperative and postoperative endoscopic results in a 47-year-old male patient with sinonasal teratocarcinosarcoma. a: the normal left nasal cavity with inferior and middle turbinal and nasal septum (black arrows). b: the right nasal cavity was fully obstructed by a large purple-red neoplasm (black arrow), and other anatomical structures were obscured. c: The latest follow-up revealed that the right sinuses recovered well with no sign of recurrence (black arrow).
Treatment strategy
After a systematic assessment, radical endoscopic sinus surgery was suggested to the patient. Under general anesthesia, the soft tumor in the right nasal cavity was completely resected (∼2.3 cm × 1.0 cm × 0.5 cm). Because of extensive tumor invasion (involved the right maxillary, ethmoid, and sphenoid sinus), extended maxillary sinus ostium resection was performed to completely remove the tumor. Finally, the patient was diagnosed with SNTCS (T2N0M0) according to the pathological results and preoperative CT scan. One month following the surgery, he received concurrent radiochemotherapy consisting of two cycles of radiotherapy [the first cycle: TOMO GTV DT 5,100 cGy/17 F, 300 cGy quaque day (qd); the second cycle: TOMO DT 9,000 cGy/30 F, 300 cGy, qd] and four cycles of chemotherapy (cisplatin and etoposide).
Pathological examination
The results of an endoscopic biopsy performed at the previous hospital suggested a diagnosis of olfactory neuroblastoma. However, after we resected the entire tumor, the pathological findings revealed ciliated columnar and non-keratinized squamous epithelia on the tumor surface and immature squamous cell nests containing clear cells in the core. Mature and cancerous glands and poorly differentiated adenocarcinomic structures with nested cords were also evident. Furthermore, multifocal, poorly differentiated sarcoma-like areas around the adenocarcinoma and mature brain and smooth muscle- and tumor-like hyperplastic fibrous tissues were observed in some areas (Figure 3a–b).

Pathological analysis of a sinonasal teratocarcinosarcoma resected from a 47-year-old male patient. Histopathological examination revealed the following (×300): a–b Ciliated columnar epithelium and non-keratinized squamous epithelium on the top of immature squamous cell nests (some marked with black arrows), clear cells (red circles), cancerous glands (red arrowheads), and poorly differentiated adenocarcinoma structures with nested cords. Immunohistochemical staining revealed the following results (×625): c–f mesothelial tissue positive for calretinin (c) and neuroepithelium positive for CD56, neuron-specific enolase (NSE), and synaptophysin (Syn) (d–f).
The immunohistochemical staining results revealed that the tumor and neural epithelia were positive for phosphoenolpyruvate carboxykinase and epithelial membrane antigen (EMA) but negative for carcinoembryonic antigen. The neuroepithelium stained positive for neuron-specific enolase (NSE), CD56 (also termed neural cell adhesion molecule 1), synaptophysin (Syn), and chromogranin A (CgA). The neuroepithelium and mesenchyme stained positive for desmin but negative for myogenin. The mesothelial tissue was positive for calretinin (Figure 3c–f). About 70% of the field and 15% of the mesenchymal component area were positive for the Ki-67 neuroepithelial component.
Follow-up
The patient responded well and made an uneventful recovery (regular follow-ups 1 month after surgery, 3–6 months after radiochemotherapy, and subsequently every year). One-month postoperative head-and-neck magnetic resonance imaging (MRI) only revealed inflammatory lesions caused by surgery (Figure 1e–f). Head-and-neck MRI after concurrent radiochemotherapy at the 5-month follow-up showed good response of the right nasal cavity and sinuses (Figure 1g–h). The nasal endoscopic examination at the 2-year follow-up visit demonstrated that the right sinuses recovered well with no sign of recurrence (Figure 2c). No evidence of recurrence has been observed for over 5 years.
Discussion
Teratocarcinosarcoma (TCS) is a rare and highly malignant tumor often consisting of components from all three germ layers, including a squamous epithelial mass of ectoderm, smooth muscle fibers exhibiting mesoderm tumor-like hyperplasia with cartilage and bone tissue in the mesoderm, and a mucous cell-rich, ciliated columnar epithelium arranged as a duct-like structure (reminiscent of digestive and respiratory tract epithelia) in the endoderm. 1 TCS was originally termed “teratoid carcinosarcoma”, 2 “teratocarcinosarcoma”, 3 “teratoma”, or “malignant teratoma”. The World Health Organization coined the formal term SNTCS in 2005. 4 TCSs are commonly found in the nasal cavity, sinus(es), 5 ovaries, or uterine cervix.6,7 The incidence is relatively low, with fewer than 150 cases reported worldwide and only ∼10 cases in China. We reviewed the literature from 1968 to 2020, and 107 SNTCS cases were identified during this period (Table 1)5,8–22.
Summary of documented clinical details in 107 SNTCS cases (1968–2020).

RCT: radiochemotherapy, NACT: neoadjuvant chemotherapy, IMRT: intensity-modulated radiation therapy; N/A: not available.
SNTCS is a complex and malignant nasal sinus tumor exhibiting characteristics of both a teratoma and carcinosarcoma. It may arise from embryonic tissue or pluripotent stem cells in the upper airway during development. A typical tumor exhibits both benign and malignant epithelia, mesenchymal tissue, and neural components. SNTCS is more common in adults (average age 54.7 years) and male patients (male:female ratio of approximately 7:1–8:1) than in children/adolescents and female patients. 5 Adolescent cases are rare, 5 with only seven reported cases in patients under 20 years old, which includes one 27-day-old newborn. The most common clinical symptoms are nasal obstruction and recurrent epistaxis. When the tumor invades the surrounding tissues, patients present with facial swelling, proptosis, optic atrophy, and headaches. 23 The course of the disease generally ranges from weeks to 2 years. The nasal cavity and sinuses are the most commonly involved sites, followed by the nasopharynx, pharyngeal sidewall, and anterior skull base. 8 Nasal endoscopy detects most nasal lesions, and endoscopic examination of an SNTCS typically shows a solid tumor that is grayish-white to dark red in color, irregularly shaped, brittle, bleeds easily, and exhibits localized surface necrosis. 24
SNTCS usually lacks specific CT and MRI features; the images are similar to those of common malignant sinus tumors. In our case, CT revealed a non-distinctive neoplasm. Pathological examinations were required for diagnosis as local tissue biopsy alone is inadequate, given the histological diversity of SNTCSs. 17 Postoperative pathology (microscopy) revealed ciliated columnar and non-keratinized squamous epithelia, immature squamous clear cell nests in the core, mature glands, and poorly differentiated adenocarcinomic structures, all of which are characteristic of teratomas. It was previously reported that immunohistochemical results are helpful for the diagnosis of SNTCS. These included positive staining for epithelial markers (cytokeratin and EMA), the undifferentiated shuttle sarcoma/smooth muscle marker vimentin, undifferentiated or primary tumor component markers (CD99 and NSE), Syn, and CgA (weakly positive) and negative staining for smooth muscle actin and desmin. 25 These staining patterns are consistent with the immunohistochemical findings in our case.
Given the rarity of SNTCS, it is easy to misdiagnose this carcinoma as other nasal sinus tumors, such as olfactory neuroblastomas, small cell carcinomas, immature teratomas, malignant transformations of teratomas, carcinosarcomas, or adenocarcinomas. 26 Our present case was initially misdiagnosed with olfactory neuroblastoma for the following reasons: the biopsy sample size was inadequate, the tumor was heterogeneous, and the morphologies of olfactory neuroblastoma and SNTCS are relatively similar. Therefore, a comprehensive pathological examination is essential.
Many SNTCS cases are diagnosed at an advanced stage, and the average 2- to 3-year survival rates range from 45% to 60%.5,27 In previous studies, 87.2% of patients with SNTCS underwent surgical resection, 59.3% underwent radiation therapy, and 18.6% were treated with chemotherapy. The highest survival rate (88.8%) and lowest recurrence rate (22.2%) were found in the group that underwent surgery with adjuvant focused radiation and chemotherapy.5,20 Currently, surgery plus radiochemotherapy is considered to be the optimal treatment strategy.1,27–30 Given the anatomical complexity of the nasal sinuses, surgery alone cannot guarantee complete tumor resection.13–22,26–29 Recently, neoadjuvant chemotherapy prior to operation has been suggested. 31 The local recurrence rate ranges from 25% to 55%.5,27–29,32,33 Thus, follow-up nasal endoscopy and/or positron-emission tomography-CT is essential to screen for early recurrence. Our patient received surgery combined with chemoradiotherapy and was followed-up regularly for 5 years without any recurrence or metastasis.
Conclusion
SNTCS is a morphologically and histologically heterogeneous malignant tumor, and the prognosis is poor. Early detection and surgery combined with adjuvant treatments will improve patient prognosis.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Ethics statement
We obtained a signed consent form from the patient to publish this article and explained to this patient that all of his identity information would be de-identified.
Funding
The authors disclose the following financial support received for this research: This work was supported by a 1·3·5 project for disciplines of excellence–Clinical Research Incubation Project, West China Hospital, Sichuan University [Grant No. 2019HXFH003]; Key Research and Development Support Programs of Chengdu Science and Technology Bureau: 2019-YF05-00461-SN; Fundamental Research Funds for the Central Universities: 20ZDYF3010 and 2019HXBH079; Scientific and Technological Projects of Sichuan Province: 20ZDYF0266, 20GJHZ0193, and 2018ZR0342; a Science and Technology Project of Sichuan Health and Health Commission: 20PJYY1597; the China Postdoctoral Science Foundation: 2020M673250; the National Natural Science Foundation of China: 82002868; The Foundation of National Clinical Research Center for Geriatrics: Z20201013; National Natural Youth Science Foundation of China: 30801280.
