Abstract
Gestational gigantomastia (GGM) is a rare complication of pregnancy. The etiology of GGM is yet to be fully established. Treatment methods for GGM include medical therapy and surgery. If medical treatment is unsuccessful, surgery may be required. Currently available surgical interventions are either breast reduction or mastectomy with delayed reconstruction. We report a case of a 25-year-old woman (G1P1) who presented with massive enlargement of both breasts during puerperium. Because of the limited effect of medical therapy, surgical intervention was considered to be the first choice. Bilateral mastectomies with grafting of the nipple–areola complex and immediate bilateral tissue expander implantation were performed. Reconstruction was fully completed 8 months after the initial procedure by replacing tissue expanders with definitive implants. Despite being a benign condition, GGM can turn into a serious problem. GGM can be successfully reconstructed by mastectomy with delayed reconstruction and grafting of the nipple–areola complex.
Keywords
Introduction
Gestational gigantomastia (GGM) is a rare clinical condition, which is characterized by rapid and disproportionate enlargement of the breasts during pregnancy. 1 The etiology of GGM is still uncertain with many proposed theories. GGM has been reported to be associated with a response of breast receptors to gestational hormones and with hyperprolactinemia. 2 GGM can cause physical and psychological problems that severely affect the patient’s quality of life.
Current procedures used in the treatment of this rare disease are still controversial. Available therapeutic options include conservative hormonal therapy, reduction mammoplasty, and mastectomy. In recent years with the advancement of surgical and anesthetic techniques, a surgical approach, especially mastectomies with reconstruction, is preferred for achieving better clinical and psychological outcomes for the patient. 1 Nevertheless, choosing the optimal therapeutic procedure should be based on the individual’s conditions and requirements.
We report here a rare case of GGM, which was successfully treated with bilateral mastectomies, free areola–nipple graft implantation, and delayed breast reconstruction.
Case report
A 25-year-old woman (G1P1) with macromastia visited our hospital for corrective surgery in 2017 during puerperium. She complained of marked enlargement of both breasts with no palpable masses. She also had severe pain and discomfort in her neck and back with severe limitation of movement that greatly affected her quality of life. She had been diagnosed with polycystic ovarian syndrome 3 years previously and was taking Diane-35 for treatment. She mentioned that her breasts had gradually increased in size since this time. She was pregnant for the first time in November 2016. During the initial stages of her pregnancy, her condition became severe. She noticed more rapid enlargement of both breasts accompanied by bilateral periareolar ulceration. Enlargement of the breasts persistently progressed until she delivered a live male newborn. Bromocriptine treatment was administrated within the time of puerperium. Enlargement of the breasts ceased and skin ulceration went into remission. However, considerable regression of the enlarged breasts was not expected. There was no other noteworthy personal medical or family history for breast pathologies.
On examination, both of the patient’s breasts reached below the umbilicus while in the standing position (Figure 1) and showed Grade III breast ptosis (according to Regnault’s classification). Additionally, the left breast was slightly larger than the right. The skin covering the breasts showed marked hyperpigmentation, dilated veins, and multiple healing ulcerations around the areola. Axillary accessory breast tissue was detected on bilateral axillary sides and the right axillary accessory breast was larger (10 × 5 cm). Ultrasonography of the breast showed no obvious lumps. All laboratory investigations were normal, except for an elevated prolactin level (50.7 ng/mL). Additionally, the results of immunological assays were negative.

Preoperative views of the patient. There is massive enlargement of both breasts and bilateral axillary accessory breasts.
Because conservative treatment of bromocriptine was ineffective, surgical intervention was chosen to obtain better results. Breast reduction was thought to be unsuitable for the patient because she was young and planned to be pregnant in the future. Additionally, the risk of recurrence was high. Consequently, bilateral mastectomy with delayed reconstruction was provided as the most ideal treatment option.
After anesthesia, bilateral mastectomy was performed by removing the breast tissue. We refashioned the skin of the breast, excised wide areas, including the devitalized and ulcerated areas, and left the healthy proximal skin intact. After the skin incision, the dermal flap from the inferior pole of the breast was de-epithelialized. Instead of implants, tissue expanders were chosen in the first stage to avoid infection resulting from a skin ulcer. Because the subcutaneous layer of the breast is <1 cm, 300-mL tissue expanders were placed in a subpectoral pocket. This was followed by suturing of a de-epithelized dermal flap to the superior border of the pectoralis muscle for lower pole prosthetic coverage. This method has been shown to effectively reduce the infection rate, and decrease the likelihood of palpability and exposure of the tissue expanders. Bilateral implantation of a free areola–nipple graft was performed (Figure 2). The removed right breast weighed 3975 g and the left weighed 4728 g. Bilateral axillary accessory breasts were also resected. The patient had a smooth postoperative course, except for necrosis of the left areolar–nipple graft.

a. Intraoperative view of tissue expander coverage and suturing of the dermal flap to the inferior border of the pectoralis muscle. b. Postoperative view immediately after nipple–areola graft implantation.
Five months later, because of the thin subcutaneous layer of the breast, the patient received bilateral autologous augmentation of the breasts by filling them with fat combined with liposuction of the left accessory breast. Eight months later, the second phase of reconstruction was undertaken. The tissue expanders of both breasts were removed and definitive silicone implants were placed in the same subpectoral pockets. The right accessory breast was corrected with removal of surplus fat and skin in the axilla at the same time (Figure 3). Follow-up of the patient 1 year postoperatively showed no recurrence or major complications. Because all treatments were routinely performed according to established guidelines and no clinical trial was performed, no approval by an ethics committee or institutional review board was required. Written informed consent was obtained from the patient for publication of this case report and photographs.
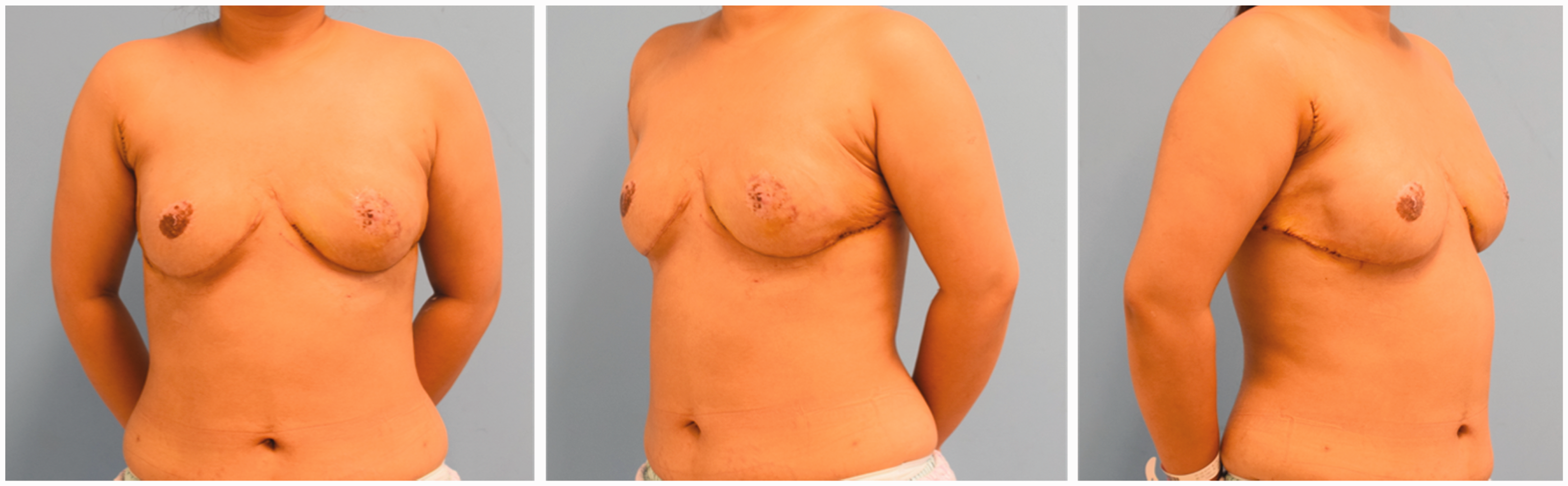
Postoperative views showing the final outcome of the reconstruction procedure.
Discussion
GGM was first described in 1684 and fewer than 100 cases have been reported in the literature since this time. 3 The incidence of GGM varies from 1/28,000 to 1/100,000 pregnancies. 4 Patients with GGM present with massive enlargement of the breasts accompanied by possible thinning of the skin, tissue necrosis, infection, and hemorrhage. This disease can also lead to movement and respiratory difficulties and emotional, social, and psychological disorders.
The etiology of GGM remains unknown, but various theories have been proposed, including hormonal imbalance, autoimmunity, and association with malignancy. 1 In most cases, rapid enlargement of the breast occurred at the end of early pregnancy, with overlap of the period of peak gonadotropin production, which may support the hypothesis of hormonal association. However, GGM can also affect patients with normal hormone levels or even after medical suppression. In our case, both breasts began to enlarge when oral Diane-35 was prescribed, and this was exacerbated during pregnancy. At admission, the prolactin level was slightly elevated in our patient, which may have played a role in the development of breast hypertrophy. These findings indicate that hormonal alteration may have been the triggering cause for this patient.
Treatment procedures for GGM are still controversial. Currently available treatment approaches for GGM are conservative hormonal therapy, breast reduction, and mastectomy. Treatment selection varies on a case-to-case basis. Most macromastia occurs when hormone levels drastically change. Therefore, these patients can be treated with hormone antagonists, such as bromocriptine, progesterone, tamoxifen, and danazol. 5 However, the results of medical treatment are uncertain and inconsistent. Conservative treatment can stop progression and cause regression, but most commonly, restoring the breasts to their original size is difficult. 6 Bromocriptine is the most widely used medical regimen, but effects are variable and usually temporary, and cannot restore breast volume to normal. Agarwal et al. 4 reported a case in which bromocriptine was successfully used as a monotherapeutic approach, avoiding the need for surgical intervention in a patient with a normal hormone profile. El-Boghdadly et al. 7 reported a case of GGM in a patient with an elevated serum prolactin level who did not respond to bromocriptine. Despite varying clinical results, use of bromocriptine as a monotherapeutic approach in some patients has proven effective, supporting its clinical use in an effort to avoid surgical interventions. In our case, bromocriptine was initiated, but unfortunately, minimal clinical improvement was observed.
When conservative treatment is ineffective for GGM or patients present with complications, such as cardiac failure, massive hemorrhage, ulceration, or breast necrosis, a surgical approach is indicated. Presently, two surgical methods are commonly used, including breast reduction and mastectomy with simultaneous or delayed reconstruction. Breast reduction can provide a one-step procedure and preservation of breastfeeding, which may be a possible advantage. However, breast reduction has a higher risk for hemorrhage and recurrence than mastectomy with delayed reconstruction, and the incisions are made through hypertrophied and hypervascularized tissue. Further, as long as breast tissue remains, it is likely to become more hypertrophic in subsequent pregnancies. In patients with GGM who undergo breast reduction, the risk of recurrence during subsequent pregnancy is 100%. 1
Bilateral mastectomy with delayed reconstruction has a lower risk of recurrence compared with breast reduction during subsequent pregnancy. This method can also be performed faster with less blood loss. Therefore, bilateral mastectomy with reconstruction appears to be the best therapeutic alternative for most patients with GGM, especially for women who desire pregnancies again. 8 Miller and Becker 9 first described reconstruction for mastectomy using an implant in 1979. Boyce et al. 10 reported the first use of tissue expanders followed by replacement and exchange by implants. Ben Meir et al. 11 described their experience of mastectomy and reconstruction using implants and a free nipple graft, with localization of the surgical scar at the meridian of the breast, which resulted in an inferior aesthetic result. Ohlsen et al. 12 reported breast reduction and banking of the nipples followed by mastectomy with delayed reconstruction, and the nipples were replaced in the same stage. In our patient, we chose to perform bilateral mastectomy with delayed breast reconstruction and a free nipple–areola complex graft. The first phase of reconstruction was undertaken by placement of subpectoral tissue expanders, which were wrapped by pectoralis major muscle and a de-epithelized dermal flap. This method provides good blood supply in the subcutaneous layer, reduces the incidence of infection, and decreases the likelihood of palpability and exposure of the tissue expanders. At the same time, fat grafting and exchange of implants offer a more natural breast contour. This procedure was accepted by the patient and the results were satisfactory.
According to the current literature, there is still controversy on the preferred procedure (breast reduction or mastectomy) or the timing of surgery (before or after partus) for GGM. However, bilateral mastectomy with delayed reconstruction can be the best option for a woman in hope of future pregnancies and a lower risk of recurrence. If future pregnancies are not expected, and the patient is clinically stable and accepts the risk of recurrence, then breast reduction can also be considered. Finally, surgery should be delayed until the fetus is viable if it is to be performed during pregnancy. Administration of steroids to promote fetal lung maturation in case of premature delivery is necessary and should be considered.
Conclusion
GGM is a rare disease. Despite being a benign condition, GGM can be physically and psychologically debilitating to the patient. Pharmacological management is usually ineffective for GGM, but remains the first-line therapy in the hope of avoiding surgery. Breast reduction and mastectomy are the currently available methods of treating GGM cases. In the present case, pharmacotherapy failed to alter clinical progression of the condition, and bilateral mastectomy with delayed breast reconstruction and a free nipple–areola complex graft was offered as a definitive treatment. This procedure provides the advantage of preserving the shape of the breast together with minimizing the risk of future recurrence.
