Abstract
Objectives
Interleukin-37 (IL-37) has been identified as a potent inhibitor of the immune response. This study aimed to examine IL-37 expression in patients with chronic active hepatitis B (CAHB), and explore its possible regulatory role during inflammation.
Methods
Peripheral blood mononuclear cells (PBMCs) were collected from control (n = 20) and CAHB patients (n = 30) before and after treatment with entecavir (EVT) for 24 weeks. The PBMCs were cultured with lipopolysaccharide and IL-37 expression was determined by real-time polymerase chain reaction and flow cytometry. The mRNA and protein concentrations of IL-1β, IL-6, and tumor necrosis factor-alpha (TNF-α) in PBMCs were also measured.
Results
Levels of IL-37, IL-1β, IL-6, and TNF-α were significantly increased in the supernatant of PBMCs from patients with CAHB. IL-37 significantly reduced the expression of IL-1β, IL-6, and TNF-α. EVT resulted in regression of intraocular inflammation in patients with CAHB, associated with decreased production of IL-37.
Conclusion
These results suggest that increased expression of IL-37 was associated with the suppression of the inflammatory response in patients with CAHB. Furthermore, EVT treatment of CAHB was also correlated with downregulation of IL-37, indicating that EVT may partially alleviate the immune response by modulating IL-37 production.
Background
Chronic hepatitis B virus (HBV) infection is one of the most severe public health problems, affecting approximately 250 million people worldwide. People with chronic HBV infection are at higher risks of developing hepatocellular carcinoma and cirrhosis.1,2 Recent evidence showed that dynamic interactions among inflammatory chemokines/cytokines were associated with the process of chronic liver damage, implying an important role for adaptive immune cells in the pathogenesis of hepatic inflammation. 3
Interleukin (IL)-37 (previously known as IL-1 family member 7) is produced by various types of cells, including epithelial cells, peripheral blood mononuclear cells (PBMCs), and macrophages. 4 Recent studies revealed that IL-37 abrogated a wide spectrum of inflammatory responses.5,6 Human PBMCs and various tissues can express IL-37 at low levels, induced by inflammatory stimulation, such as via Toll-like receptor agonists. IL-37 improved the histological indices of colitis and attenuated the clinical signs by reducing the production of inflammatory cytokines in a mouse colitis model. 7 These findings indicate that IL-37 is involved in the inflammatory feedback loop. Previous studies have considered the inflammatory role of IL-37 in HBV. One clinical study reported that patients with HBV had significantly higher serum levels of IL-37 than normal subjects, and that serum IL-37 concentrations were positively correlated with the virus concentration and alanine aminotransferase (ALT) levels, suggesting a regulatory effect of IL-37 in immune tolerance to chronic HBV infection.3,8
Entecavir (ETV) is a nucleoside analogue that has been widely used to treat chronic active hepatitis B (CAHB). EVT acts as a selective inhibitor of hepadnaviral DNA polymerase by competing with the corresponding deoxyribonucleoside triphosphate for incorporation in nascent DNA, and by functioning as a chain terminator post-incorporation. 9 ETV has also been reported to be transported into cells by pyrimidine nucleoside transporters and to be activated by different sets of cellular enzymes. 10
Based on these previous results, we hypothesized that IL-37 might play a prominent role in the pathogenesis of CAHB by regulating the production of proinflammatory cytokines by activated immune cells. The present study investigated the role of IL-37 in CAHB, and determined if ETV could inhibit the production of IL-37 in patients with CAHB.
Methods
Study population
We recruited patients with CAHB who attended The First Affiliated Hospital of Chongqing Medical University, Chongqing, China, between November 2017 and January 2018 in this study. The diagnostic and treatment criteria were in accordance with the European Association for the Study of the Liver (EASL), the 2017 clinical practice guidelines for the management of chronic hepatitis B, 11 and the Asian-Pacific consensus statement on the management of chronic hepatitis 2012 update. 12 The inclusion criteria were as follows: serum hepatitis B surface antigen (HBsAg)-positive for at least 6 months; ALT above twice the normal level (<72 IU), and log HBV DNA >4 or <7; and no anti-viral or other related drugs for at least 24 weeks before recruitment. The exclusion criteria were as follows: acute hepatitis A or B, human immunodeficiency virus (HIV), hepatitis D or C virus (HDV, HCV) co-infection, or drug-induced acute hepatitis; hepatic decompensation, renal failure, or psychiatric disorders; marrow or organ transplants, or nephrotoxic or hepatotoxic immunosuppressive medications within 2 months of enrollment; and central nervous system disease, such as epilepsy. Healthy individuals of the same ethnic group, with confirmed absence of HBsAg, were enrolled as controls over the same time period. The protocol was approved by the Clinical Research Ethics Committee of the First Affiliated Hospital of Chongqing Medical University, and each participant provided written informed consent in accordance with the Declaration of Helsinki. This study was registered by Ethics Committee of the First Affiliated Hospital of Chongqing Medical University.
Cell isolation and cell culture
PBMCs were isolated from heparinized blood samples using Ficoll–Hypaque density-gradient centrifugation with Lymphocyte Separation Medium (MD Pacific, Tianjin, China).13,14 Cells were cultured in RPMI 1640 (HyClone, Thermo Fisher Scientific, Logan, UT, USA) supplemented with 10% fetal calf serum (Hangzhou Sijiqing Biological Engineering Materials, Hangzhou, Zhejiang, China) and plated into 24-well plates at 1 × 106 cells/mL. To assess the effects of IL-37 on cytokine production by PBMCs from CAHB patients and healthy participants, PBMCs were seeded at 1 × 106 cells/mL and treated with 100 ng/mL of lipopolysaccharide (LPS; Sigma, Saint Louis, MI, USA) with or without 100 ng/mL recombinant IL-37 (rIL-37; R&D Systems, Minneapolis, MN, USA) for 72 hours. Cytokines in the supernatants were then analyzed by enzyme-linked immunosorbent assay (ELISA) as detailed below. Control samples were stimulated with the same volume of sterile phosphate-buffered saline alone.
To examine the mechanism by which IL-37 regulates the production of cytokines in more details, PBMCs from healthy subjects were seeded at 1 × 106/mL and treated with LPS (100 ng/mL) together with rIL-37 at 0,50,100, or 200 ng/mL for 72 hours. Then culture supernatants and cells were collected for mRNA and protein analyses using real-time polymerase chain reaction (RT-PCR) and ELISA, respectively.
Real-time quantitative RT-PCR
Total RNAs were extracted from rIL-37-stimulated PBMCs from CAHB patients and healthy subjects using an RNAeasy Mini Kit (Qiagen, Hilden, Germany) according to the manufacturer’s instructions. cDNA was then synthesized using a Superscript III Reverse Transcriptase system (Invitrogen, Carlsbad, CA, USA). mRNA expression levels of IL-37, IL-1β, IL-6, IL-10, tumor necrosis factor-alpha (TNF-α), and β-actin were detected using SYBR Premix Ex TaqII (TaKaRa, Japan) on a RocheZ480 Real-Time PCR System (Roche Molecular Diagnostics, Switzerland). The primers used are given in Table 1. The IL-37 and β-actin primers were purchased from Qiagen. Relative mRNA expression levels were normalized to β-actin using the 2−ΔΔct method.
Primer sequences of cytokines.
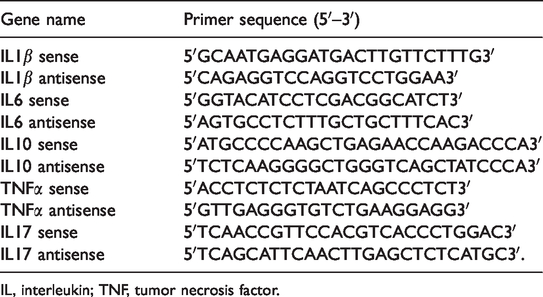
IL, interleukin; TNF, tumor necrosis factor.
ELISA
Peripheral blood samples from CAHB patients and healthy participants were obtained and stored in endotoxin- and pyrogen-free tubes. Serum levels of IL-37 were determined using a commercially available ELISA kit (AdipoGen, Sweden), with a detection limit of 0.016 to 1 ng/mL.
The concentrations of IL-1β, IL-6, and TNF-α in the culture supernatants of PBMCs were measured using kits (R&D Systems, Minneapolis, MN, USA), in accordance with the manufacturer’s instructions. The detection limits for IL-1β, IL-6, and TNF-α were 0.008, 0.015, and 0.031 ng/mL, respectively. The absorbance of the plates was read at 450 nm using an automated absorbance microplate reader (Sunrise, Tecan Inc., Austria).
Flow cytometry
PBMCs were fixed in BD Cytofix/Fixation Buffer (BD Biosciences, San Jose, CA, USA) for 10 minutes at 37°C, and permeabilized using BD Phosflow Perm Buffer III (BD Biosciences) for 30 minutes at 4°C. The cells were subsequently incubated with IL-37 antibody (Abcam, MA, USA) for 30 minutes at 22°C followed by incubating with a phycoerythrin-secondary goat anti-mouse Ig antibody (4A Biotech, Beijing, China) for 30 minutes at 22°C. Fluorescence-activated cell sorting analysis was conducted using a FACS Canton II and FACS Diva software (BD Company, Franklin Lakes, NJ, USA). Data were shown as increments relative to an isotypic control (IC) using the following formula: [MFI of sample – MFI of IC]/MFI of IC.
Statistical analysis
Data were presented as mean ± standard deviation. Differences between groups were analyzed by Mann–Whitney tests for unpaired comparisons and Wilcoxon’s signed rank tests for paired comparisons using SPSS for Windows, Version 18.0 (SPSS Inc., Chicago, IL, USA). Correlations between variables were calculated using Spearman’s rank correlation test. A value of P < 0.05 was considered statistically significant.
Results
Patient characteristics
Thirty patients with CAHB and 20 healthy controls were enrolled in this study (Table 2). Most participants were from different regions of Southwest China. No patient had evidence of concomitant HCV, hepatocellular carcinoma, HIV, or HDV infection, or autoimmune or metastatic liver disease. The CAHB patients received oral EVT 0.5 mg/day for 24 weeks. There were no significant differences in sex or age proportions between the patients and controls.
Demographic and clinical characteristics of the study subjects.

NA, not assessed; CAHB, chronic active hepatitis B; ALT, alanine aminotransferase; HBsAg, hepatitis B surface antigen; HBeAg, hepatitis B e antigen.
Increased expression of IL-37 in PBMCs obtained from CAHB patients
Serum levels of IL-37 were significantly higher in CAHB patients compared with healthy participants (P = 0.0025), as demonstrated by ELISA (Figure 1a). IL-37 mRNA levels were also significantly higher in PBMCs from CAHB patients compared with the controls, according to qRT-PCR (Figure 1b). Consistent with the mRNA expression levels, IL-37 protein levels in PBMCs were also significantly higher in CAHB patients than in healthy controls (Figure 1c). IL-10 mRNA levels were also significantly higher in CAHB patients compared with healthy controls, as shown by qRT-PCR (Figure 1d). Moreover, IL-37 expression levels were positively correlated with serum ALT in CAHB patients (Figure 2).
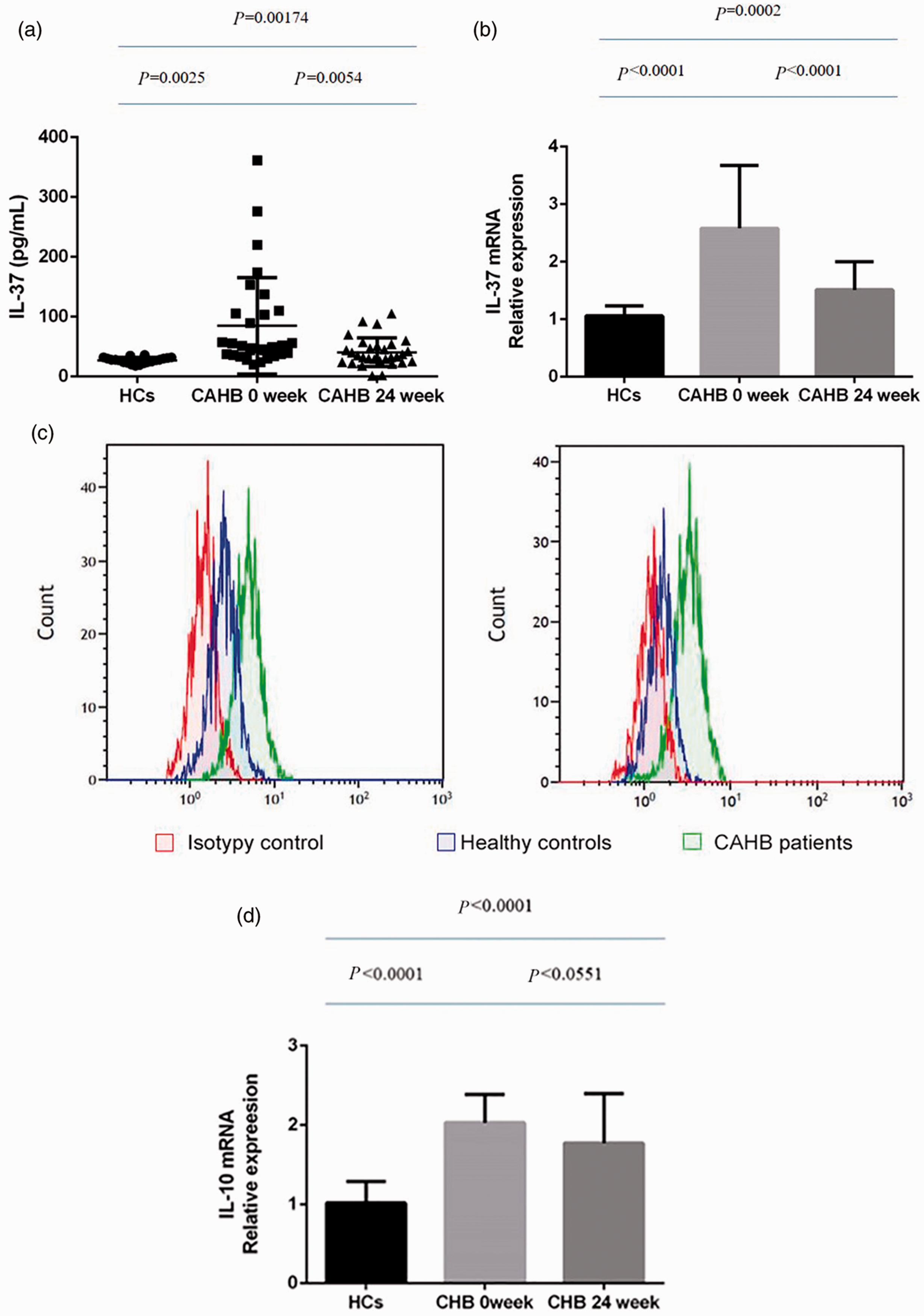
IL-37 levels were increased in patients with CAHB compared with healthy controls, and were decreased after 24 weeks of ETV treatment. (a) IL-37 concentrations in supernatants of PBMCs from patients with CAHB before and after treatment (n=30) and healthy controls (n=20) assayed by ELISA. (b) IL-37 mRNA levels in PBMCs from CAHB patients before and after treatment (n=30) and healthy controls (n=20) assayed by RT-PCR. Levels were normalized to β-actin. (c) Representative histograms showing results for one patient and one healthy participant, based on flow cytometry. IL-37 protein levels were in line with the mRNA expression levels. (d) mRNA expression of IL-10 in PBMCs from 30 CAHB patients before and after 24 weeks of the EVT treatment compared with 20 healthy controls. CAHB, chronic active hepatitis B; IL-37, interleukin-37; PBMC, peripheral blood mononuclear cell; ETV, entecavir.

Correlation between IL-37 levels and serum ALT in CAHB patients. IL-37, interleukin-37; ALT, alanine aminotransferase.
IL-37 expression in CAHB patients decreased after 24 weeks of treatment with EVT
EVT is commonly used to treat CAHB. We therefore examined IL-37 mRNA expression levels in PBMCs from 30 CAHB patients before and after 24 weeks of EVT treatment, compared with levels in 20 healthy controls. IL-37 mRNA expression was significantly up-regulated before EVT treatment, compared with controls, but was significantly decreased after treatment, indicating that EVT significantly decreased IL-37 mRNA expression in PBMCs (Figure 1b).
IL-37 suppressed proinflammatory cytokine production by PBMCs in CAHB patients and healthy subjects
We examined the regulatory effect of IL-37 on the production of proinflammatory cytokines, and determined if PBMCs from patients with CAHB and controls responded differently to IL-37. rIL-37 100 and 200 ng/mL down-regulated IL-1β, IL-6, and TNF-α mRNA expression levels in PBMCs, consistent with the results of ELISA.
We further investigated how IL-37 affected the expression of proinflammatory cytokines by treating PBMCs from CAHB patients and healthy subjects with LPS with or without 100 ng/mL rIL-37. IL-1β (Figure 3a), IL-6 (Figure 3b), and TNF-α (Figure 3c) levels were significantly elevated in the PBMC culture supernatant from untreated CAHB patients compared with healthy subjects. However, rIL-37 suppressed LPS-induced cytokine production in both CAHB patients and healthy participants. We previously reported that proinflammatory cytokine levels in culture supernatants from unstimulated PBMCs were very low, indicating the need for LPS treatment. We therefore did not include unstimulated controls in the current study.
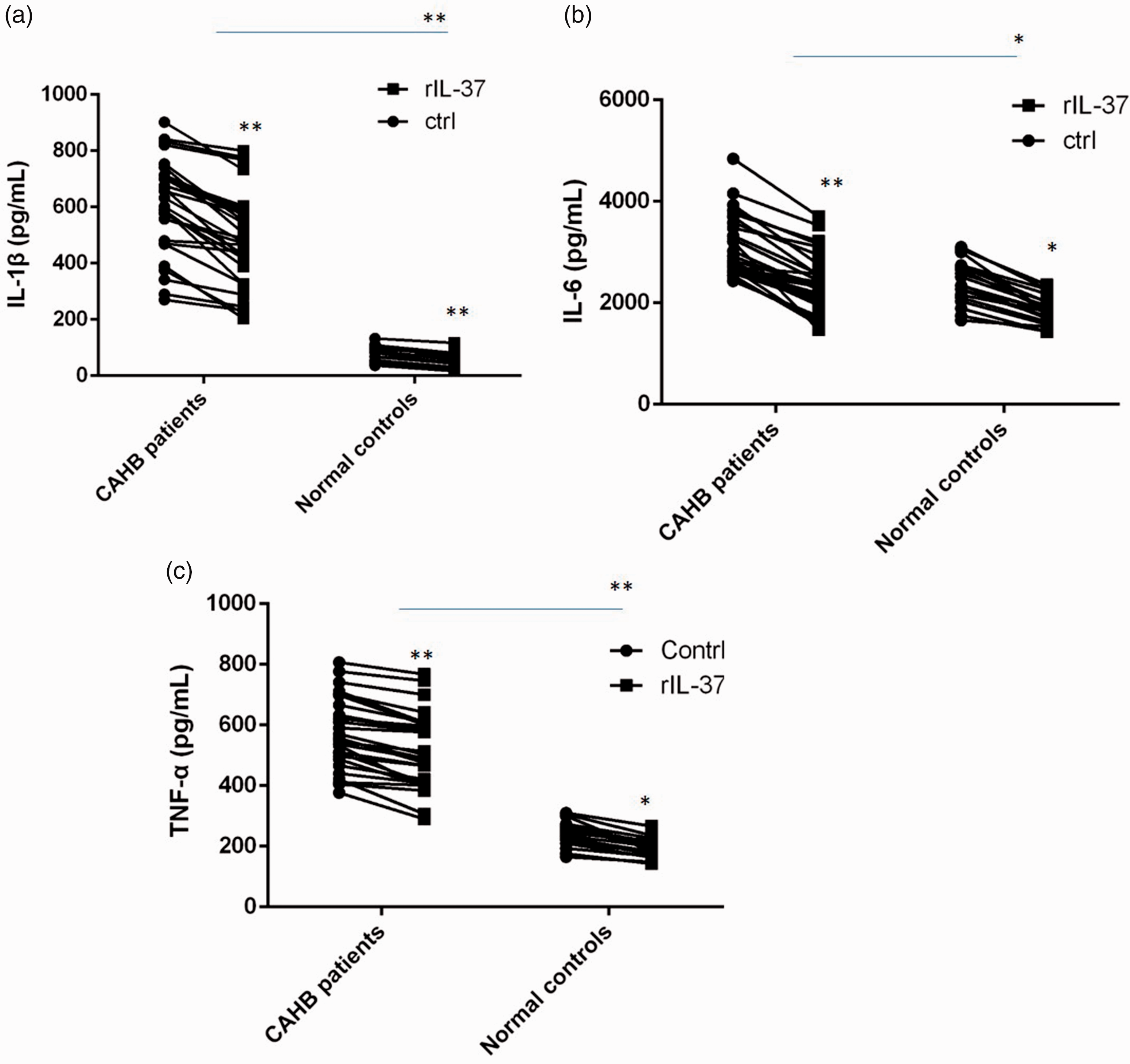
IL-37 suppressed the levels of proinflammatory cytokines in PBMCs from patients with CAHB and healthy participants. PBMCs from CAHB patients before treatment (n=30) and healthy participants (n=20) were treated with LPS plus rIL-37 or LPS alone for 72 hours. IL-1β, IL-6, and TNF-α levels in the supernatants were measured by ELISA. (a–c) Concentrations of cytokines were elevated in CAHB patients before treatment compared with healthy participants. IL-37 blocked the expressions of these cytokines in both CAHB patients and healthy participants. rIL-37, recombinant interleukin-37; IL- interleukin; TNF-α, tumor necrosis factor-alpha; ctrl, control. *P<0.05, **P<0.01.
Discussion
IL-37 has been shown to play an anti-inflammatory role inhibiting the immune response in various diseases. 15 Previous studies suggested that IL-37 was involved as an anti-inflammatory cytokine in autoimmune diseases by inhibiting both innate and adaptive immunity.16,17 IL-37 was reported to be up-regulated in immune-mediated inflammatory conditions, such as systemic lupus erythematosus (SLE). 18 In addition, IL-37 inhibited TNF and IL-1 family members in fibromyalgia. 19 However, the role of IL-37 in HBV infection remains unclear.
We aimed to clarify the role of IL-37 in the development of CAHB by comparing its expression levels between patients with CAHB and healthy subjects. The results revealed that IL-37 expression was significantly increased at both the mRNA and protein levels in PBMCs from CAHB patients.
Numerous studies have shown an apparent association between IL-37 expression and immune cells and cytokines.17,20,21 IL-37 was recently found to have anti-inflammatory effects on neuroinflammation. 22 In the present study, high levels of both proinflammatory and anti-inflammatory cytokines were produced in patients with CAHB. The elevated levels of IL-37 may be correlated with the HBV-specific immune responses in CAHB patients. Furthermore, the association between elevated IL-37 and CAHB supports an inflammatory mechanism of CAHB pathogenesis. The addition of rIL-37 largely decreased the expression levels of IL-1β, IL-6 and TNF-α in PBMCs. This suggests that proinflammatory cytokines in CAHB patients might enhance the production of IL-37, and that IL-37 might activate a negative feedback loop to downregulate the excessive production of proinflammatory cytokines. The upregulation of anti-inflammatory cytokines, including IL-37, might thus be a potential underlying mechanism for attenuating inflammation and alleviating disease symptoms. However, the concentrations of these anti-inflammatory cytokines may not be high enough to neutralize the detrimental impacts of proinflammatory cytokines in progressive CAHB.
EVT has been used extensively to treat patients with HBV. EVT therapy can suppress viral replication and improve liver function and the immune response in patients with CAHB. Our current results revealed that IL-37 levels were increased in CAHB patients, but both mRNA and protein levels of IL-37 were significantly decreased 24 weeks after EVT treatment, indicating suppression of intrahepatic inflammation in EVT-treated patients.
These findings are in agreement with the results in SLE patients, 18 which showed that IL-37 mRNA levels in PBMCs were decreased after prednisone treatment. However, whether there is a cause-and-effect relationship between IL-37 and these cytokines, or if the expression levels of both IL-37 and cytokines are increased during the development of CAHB without direct correlation, remains unclear.
We presumed that IL-37 might be involved in the immune response in CAHB patients, and that the increase in IL-37 production might be correlated with the development of CAHB. Previous data showed that IL-37 was expressed in natural killer cells and monocytes, including PBMCs, and was stimulated B cells.23,24 However, further investigations are needed to identify the subpopulations of cells involved. Furthermore, the source of IL-37-expressing cells in CAHB remains unclear, and the effect of IL-37 in the pathogenesis of CAHB remains unknown.
Conclusion
On the basis of the demonstrated a correlation between IL-37 expression and cytokines, we hypothesized that IL-37 may play a crucial role in CAHB. Further studies are needed to determine the potential molecular mechanisms involved, and to clarify the regulatory network of IL-37 in CAHB. Longitudinal studies are also required to explore the response of IL-37 in patients with CAHB after treatment, and to investigate the correlation between IL-37 levels and treatment response.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This project was supported by Chongqing Municipal Planning Commission of Science and Research Fund (No. 20142004). The authors thank all the patients and healthy participants in this study.
