Abstract
A 21-year-old man underwent wedge resection for treatment of pneumothorax. This patient had been diagnosed with Charcot-Marie-Tooth disease (CMTD) and had a history of surgical treatment of scoliosis, pneumothorax, foot deformity, and arm dislocation. Additionally, the patient showed signs of muscle weakness and atrophy in the upper and lower extremities.
CMTD is genetically associated with motor and sensory neuropathy and reportedly has an association with malignant hyperthermia or a delayed muscle relaxation mechanism. In the present case, total intravenous anesthesia was performed with a combination of propofol and remifentanil, and rocuronium was administered as a neuromuscular blocking agent. Surgery was performed without delayed muscle relaxation or any other specific intraoperative adverse events.
Keywords
Introduction
Charcot-Marie-Tooth disease (CMTD) is the most common inherited neuromuscular disorder. It is characterized by weakness and sensory impairment of the distal limbs accompanied by contracture, deformity, and a decrease or loss of deep tendon reflexes. 1 CMTD tends to show autosomal dominant inheritance, but it may also be autosomal recessive or X-linked. Various genes are responsible for the clinical heterogeneity of CMTD. The upper extremities become involved as the disease progresses, and severe cases may be characterized by muscular atrophy of the respiratory muscles, diaphragm, and vocal cords. 2 With regard to anesthesia, a delayed onset of action of muscle relaxant drugs has been reported in patients with CMTD. 3 The possibility of malignant hyperthermia (MH) and inadequate respiratory function due to postoperative respiratory muscle weakness must be taken into consideration.
The present case report describes a patient with CMTD with a chest deformity who underwent total intravenous anesthesia (TIVA) with rocuronium. The relevant literature is also reviewed.
Case report
A 21-year-old man (height, 158 cm; weight, 40 kg) was scheduled for wedge resection with video-assisted thoracoscopic surgery for treatment of pneumothorax. The patient had visited our hospital because of sudden chest discomfort the day before admission. He had been diagnosed with CMTD 14 years previously. Surgical treatment of scoliosis had been performed 6 years previously, and chest tube insertion for treatment of right pneumothorax had been performed 3 years previously. The patient had also undergone surgery for CMTD-related bilateral foot deformities and arm dislocation. He reported that the surgery and anesthesia were uneventful at that time. Although the operations for the scoliosis, foot deformities, and arm dislocation had been conducted under general anesthesia, no other information was available because the operation had been performed in another hospital. The patient had muscle weakness in both upper extremities (manual muscle testing grade 2−), and only smartphone manipulation was possible using finger movements. Atrophy and deformation of both feet were noted (Figure 1), and the patient was unable to stand up on his own. His condition was so severe that even using a wheelchair was not possible. Neck movements were normal, and physical examination showed atrophy of the peroneal muscles of both lower extremities (manual muscle testing grade 1) with normal sensory function. The tendon reflexes were decreased in the knees and ankles. Additionally, atrophy was present in the upper extremities.

Deformity of the lower extremity.
The patient’s mouth opening width was normal, thyromandibular length was >5 cm, Mallampati classification was class II, and American Society of Anesthesiology physical status was grade III. Preoperative laboratory studies showed no abnormal findings. Chest radiographs showed right chest tube insertion for treatment of right pneumothorax accompanied by fixation of the thoracolumbar spine with scoliosis (Figures 2, 3). Electrocardiography (ECG) revealed signs of left anterior fascicular block, and the patient’s vital signs were as follows: blood pressure (BP), 120/60 mmHg; heart rate (HR), 64 beats/minute; body temperature (BT), 36.6°C; oxygen saturation, 100%; and respiratory rate (RR), 20 breaths/minute.

Chest tube insertion state.
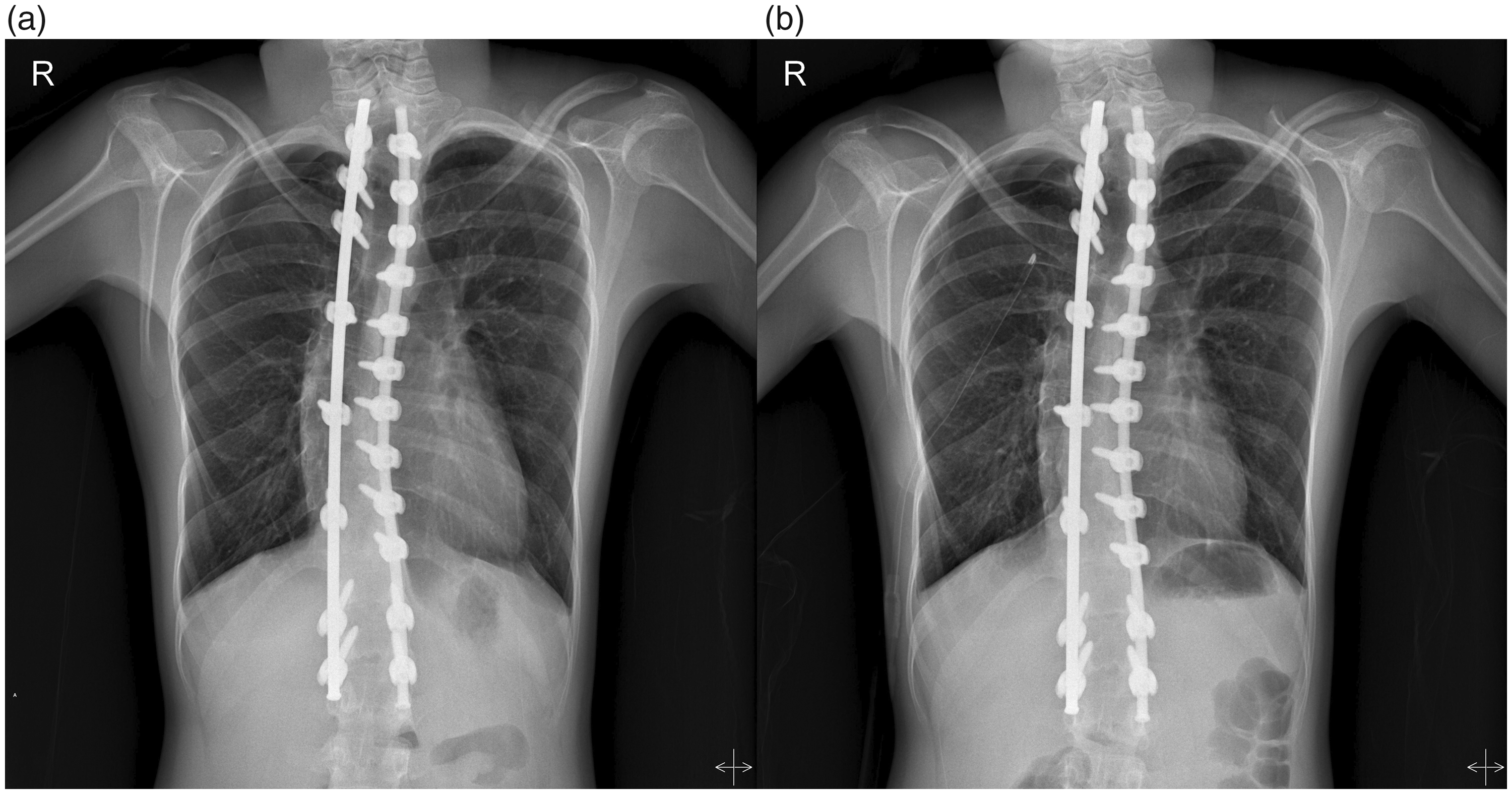
Preoperative chest radiograph. (a) Before chest tube insertion. (b) After chest tube insertion.
Premedication was not given because the patient had CMTD with pneumothorax. The patient was transferred to the operating room and underwent noninvasive BP, ECG, pulse oximetry, and bispectral index monitoring. Additionally, a neuromuscular monitoring (NMT) module (IntelliVue NMT module, Model 865383; Philips, Amsterdam, Netherlands) was set up. Before induction, the patient’s vital signs were as follows: BP, 116/63 mmHg; HR, 84 beats/minute; BT, 36.4°C; oxygen saturation, 100%; and RR, 12 breaths/minute.
Anesthesia was induced with 2% propofol (Fresofol 2%; Fresenius Kabi, Bad Homburg, Germany) and remifentanil (Ultiva; GlaxoSmithKline, Brentford, UK) administered at an effect-site concentration of 2.5 μg/mL and 2 ng/mL, respectively, using a target-controlled infusion pump (Orchestra Base Primea; Fresenius Vial, Brezins, France) under 100% oxygen inhalation (6 L/min). A neuromuscular block was achieved using intravenous injection of 15 mg of rocuronium. However, as the patient’s respiration continued, 5 mg of rocuronium was administered again after 2 minutes.
A 35-Fr left-sided double-lumen tube was inserted without difficulty. Anesthesia was maintained with 2% propofol at 1.5 to 2.5 μg/mL and remifentanil at 1 to 2 ng/mL (effect-site concentration) using a target-controlled infusion pump for TIVA, with 1 L/minute of oxygen and 2 L/minute of air.
For one-lung ventilation, the pressure-controlled ventilation–volume guaranteed mode was used with a tidal volume of 250 mL, RR of 14 breaths/minute, and peak airway pressure of 25 cmH2O. The patient was switched to the left lateral decubitus position for the video-assisted thoracoscopic surgery. However, the patient’s muscle relaxation was insufficient, and there was a collision between the ventilator and self-respiration. Therefore, 5 mg of rocuronium was administered again.
No adverse events occurred during the surgery, and 0.4 mg of glycopyrrolate and 15 mg of pyridostigmine were administered to reverse the neuromuscular block. The endotracheal double-lumen tube was removed after confirming that the patient had recovered spontaneous breathing and consciousness.
The total duration of anesthesia was 55 minutes, and that of the surgery was 25 minutes. The patient was transferred to the post-anesthesia care unit, and his vital signs were as follows: BP, 112/78 mmHg; HR, 68 beats/minute; BT, 36.5°C; oxygen saturation, 100%; and RR, 24 breaths/minute. After the patient was monitored for about 1 hour in the post-anesthesia care unit, he was transferred to the ward.
No abnormalities were found on the postoperative laboratory studies, chest radiographs or ECG or with the patient’s movement and respiration. The patient was discharged on postoperative day 3.
This study was approved by the institutional review board of Eulji University Medical Center and was performed in compliance with the EQUATOR Network guidelines. Written informed consent for publication was obtained from the patient and his parents.
Discussion
CMTD, the most common form of inherited neuropathy, is more common in women than in men. 4 As the disease becomes severe, respiratory dysfunction may develop and become restrictive in nature. 1 An important consideration in patients with CMTD is the risk of MH, the dosage of neuromuscular blocking agents, hyperkalemia, and respiratory complications. Because most inhalational anesthetics act as predisposing factors for the development of MH, caution is advised. However, an association with MH has not been demonstrated in previous studies. In the present case, TIVA was performed with propofol and remifentanil to minimize the possibility of MH despite the convenience of inhalational anesthesia.
When using inhalational anesthetics, the clinician should remember that the neuromuscular blocking effect is prolonged in patients with CMTD. This condition increases the neuromuscular blocking effect of the inhalational anesthetic itself; the neuromuscular blocking agent also has a synergistic effect.
The prolongation of the muscle relaxant effects in patients with CMTD is theoretically implied by a loss of motor units resulting in muscle weakness and atrophy, 5 up-regulation of acetylcholine receptors in the neuromuscular junction, and increased sensitivity to non-depolarizing neuromuscular blocking agents. However, up-regulation may increase the number of cholinergic receptors, resulting in normal or moderate resistance to non-depolarizing neuromuscular blocking agents. Hence, prolongation of muscle relaxation by non-depolarizing neuromuscular blocking agents may not occur. 6 Pogson et al. 3 reported prolonged neuromuscular blockade of vecuronium, whereas Baraka 6 reported a normal response with the use of vecuronium despite generalized areflexia and muscle weakness. Ortiz-Gómez et al. 7 reported that a prolonged effect was not observed with rocuronium use, and Schmitt et al. 8 reported that the use of mivacurium did not show any difference in normal individuals. We performed double-lumen tube insertion after intravenous injection of 15 mg of rocuronium in the present case, but because the patient’s spontaneous respiration remained, we administered 0.6 mg/kg of rocuronium, which is generally used during induction.
Patients with CMTD are in a chronic denervation state. Although hyperkalemia can reportedly be caused by muscle relaxants, particularly succinylcholine, some authors have insisted that this is not particularly problematic. 5 Caution is needed when managing patients with CMTD who develop hyperkalemia; these patients must be monitored by measurement of the preoperative and perioperative potassium levels and performance of ECG examination. In the present case, rocuronium was used to avoid the possibility of succinylcholine-induced hyperkalemia, and because the preoperative potassium level was within the normal range of 4.0 mEq/L, no clinical problems occurred. In addition, the NMT module was prepared for neuromuscular function monitoring, but it was not used because the patient exhibited no signs of prolonged muscle relaxation, the surgery was relatively short, and additional rocuronium administration beyond 0.6 mg/kg did not seem necessary.
A prolonged block can be observed in CMTD-affected tibial, ulnar, and facial nerves as assessed by neuromuscular function monitoring. Therefore, neuromuscular function in patients with CMTD should be monitored via the corrugator supercilii muscle rather than the adductor pollicis muscle because of clinical evidence for involvement of the extremities 3 and the ease of neuromuscular blocking agent titration and identification of adequate reversal signs via effective nerve monitoring. The correlation of corrugator supercilii muscle relaxation to diaphragm relaxation is another factor that supports monitoring of the corrugator supercilii muscle. 9
The cardiac manifestations of CMTD may include long QT syndrome, 10 paroxysmal atrial flutter, cardiomyopathy, and complete atrioventricular block. 11 However, more research is required to identify any increases in the incidence of these conditions compared with the normal population. In the present case, ECG showed a left anterior fascicular block preoperatively, but no special findings were noted intraoperatively. Propofol may be safely used in patients with arrhythmia-associated CMTD because it does not affect the patient’s cardiac conduction system. Hence, TIVA with a combination of propofol and remifentanil was chosen for this case.
CMTD may also be associated with respiratory complications, and 30% of patients with respiratory symptoms may experience a reduction in their total lung capacity, forced vital capacity, maximal expiratory pressure, and maximal inspiratory pressure to lower than 80%, 80%, 35%, and 25% of the predicted values, respectively. Such abnormal lung function is more common in patients with proximal upper extremity involvement and even more common in patients of advanced age. However, reports show no correlation with sex, height, age at onset, or duration of disease. 2
Spine deformity is also associated with lung volume reduction, and most affected patients show scoliosis or kyphoscoliosis. When the above-mentioned abnormalities in lung function are seen in patients with CMTD, noninvasive positive-pressure ventilation is reportedly helpful (i.e., when any one of the following criteria is met: forced vital capacity of <50% predicted, nocturnal desaturation of <88% for >5 consecutive minutes during sleep, maximal expiratory pressure of <60 cmH2O, or awake PaCO2 of >45 mmHg). 2
In the present case, we could not perform pulmonary function tests because the patient’s chief complaint was chest discomfort, and chest tube insertion was performed because pneumothorax was present without abnormal parenchymal findings on the chest radiograph. Although the patient had no apparent respiratory problems, a respiratory problem could have developed if the duration of administration of the neuromuscular blocking agent had been prolonged; thus, NMT monitoring was set up for this reason. However, the initial administration of 15 mg of rocuronium (60% of the 0.6-mg/kg dose generally used for induction) resulted in insufficient muscle relaxation during the first attempt at induction, and an additional 5 mg was administered within 2 minutes. However, only after adding another 5 mg had been administered (total administration of 25 mg) could the operation begin. Therefore, problems caused by prolongation of muscle relaxation could be minimized.
Sugammadex is a modified gamma-cyclodextrin that reverses the neuromuscular blocking action of rocuronium more rapidly than neostigmine. Gold and Haper 12 compared the effects of neostigmine and sugammadex and reported that in the reversal of deep blockade (post-tetanic count of 1–2), the time required for return of neuromuscular function (train-of-four ratio of >0.9) was 2.9 minutes with sugammadex and 50.4 minutes with neostigmine. This finding demonstrates that sugammadex is more suitable for deep blockade reversal. In addition, sugammadex is reportedly safe and effective in diseases such as myasthenia gravis 13 and Duchenne muscular dystrophy. 14 However, it should be used with caution because some reports have described QT prolongation and atrioventricular block after sugammadex administration. 15
In the present case, use of sugammadex was considered before induction of anesthesia because the total duration of anesthesia was 55 minutes and that of the surgery was 25 minutes. However, sugammadex was not used because the patient’s response to rocuronium was not different from that of normal individuals, and reversal was achieved with 0.4 mg of glycopyrrolate and 15 mg of pyridostigmine.
In conclusion, in patients with CMTD, clinicians should be fully aware of the possibility of hyperkalemia, MH, prolongation of muscle relaxation, and respiratory failure. It is important to determine the methods of anesthesia and the type and dosage of anesthetics as well as to consider the use of monitoring devices such as NMT so that a prompt response is assured. Additionally, the use of monitoring devices such as NMT should be considered. In particular, the patient in this case study had a higher likelihood of respiratory dysfunction from the upper extremity involvement and postoperative respiratory dysfunction because of the chest deformity and pneumothorax. With consideration of the above-mentioned factors, our patient underwent neuromuscular blockade with TIVA using a combination of propofol and remifentanil as well as rocuronium, which has no reports of prolonged muscle relaxation, and anesthesia was performed with no complications.
Supplemental Material
IMR881239 Supplemental Material - Supplemental material for Anesthesia in a patient with Charcot-Marie-Tooth disease with pneumothorax: a case report
Supplemental material, IMR881239 Supplemental Material for Anesthesia in a patient with Charcot-Marie-Tooth disease with pneumothorax: a case report by Jae Won Kim, Goo Kim, Tae Woo Kim, Woong Han, Jin Hyun Maeng, Chang Young Jeong, Jin Ho Choi and Dong Ho Park in Journal of International Medical Research
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
