Abstract
Development of a huge intrahepatic biloma after radiofrequency ablation (RFA) is a rare complication. We report a patient with hepatocellular carcinoma (HCC) who had been treated by RFA and was complicated by a huge biloma. The biloma was cured by percutaneous catheter drainage and endoscopic retrograde cholangiopancreatography. A plastic stent was placed from the duodenal ampulla to the common bile duct to lower the pressure. The catheter and the stent were removed within 1 month after the biloma had disappeared. There was no recurrence of the biloma and HCC lesions with a follow-up time of 2 years. The present case is one of the best reported outcomes after development of a huge biloma.
Keywords
Introduction
Biloma was first reported in 1979 to describe abnormal bile accumulation outside the biliary tree. 1 Biloma is considered to result from abdominal trauma, biliary surgery, endoscopic retrograde cholangiopancreatography (ERCP), and laparoscopic cholecystectomy,2–4 and it can occur spontaneously. 5 Percutaneous radiological procedures, such as transcatheter arterial chemoembolization, 4 percutaneous ethanol injection, 4 microwave ablation, 6 and percutaneous biliary drainage, 7 can also be complicated by biloma. We report here a patient with hepatocellular carcinoma (HCC) who was treated by radiofrequency ablation (RFA) and complicated by a huge biloma. However, after treatment of approximately 1 month, his biloma was completely released. In the ensuing 2 years, the patient has been free from recurrence of the biloma and HCC. We also discuss our experience about the treatment process of the biloma and HCC.
Case report
This study was approved by the Ethics Committee of Peking University First Hospital. Written informed consent for all therapeutic procedures that were performed was obtained from the patient before the procedures.
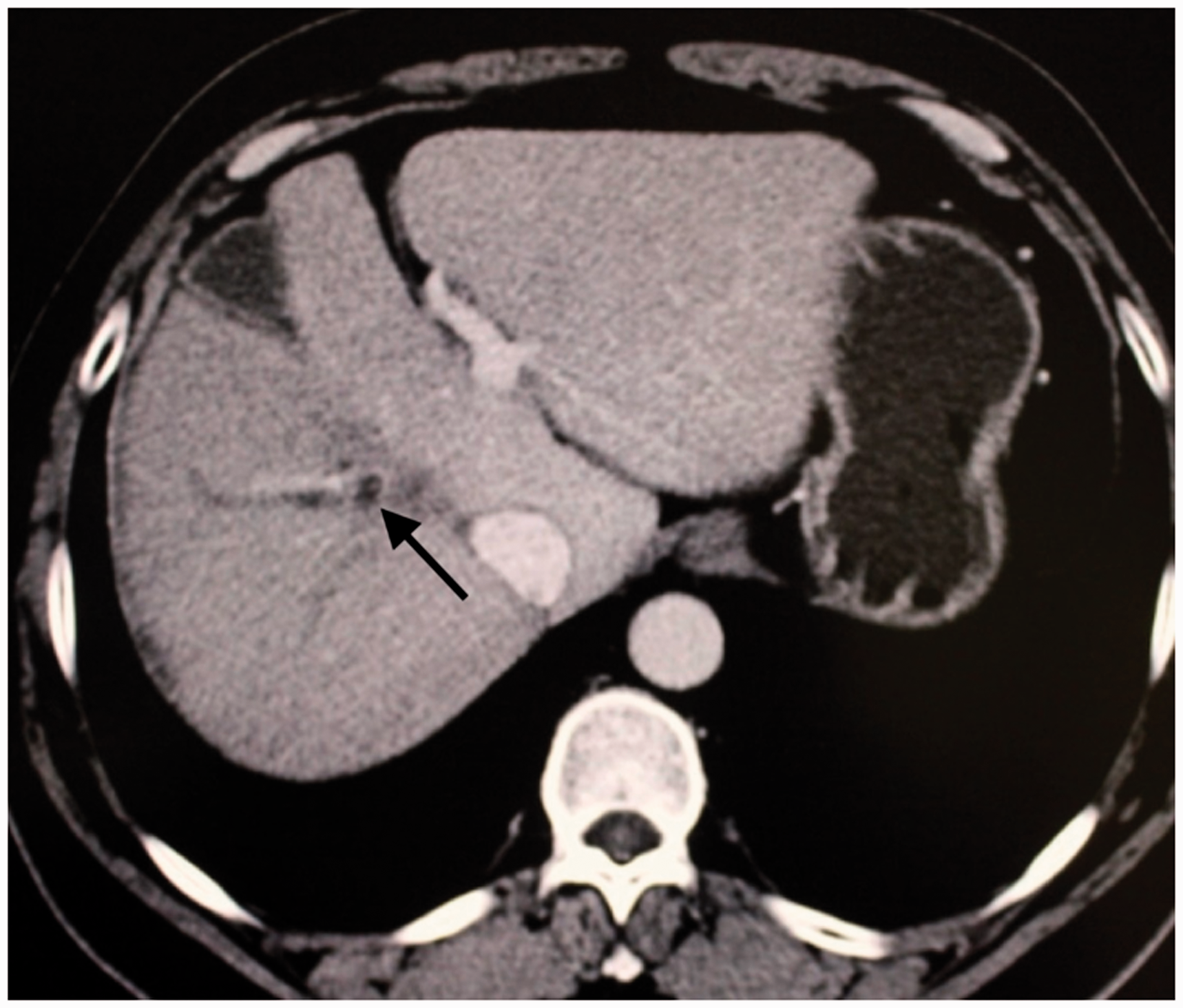
A 50-year-old man with two confirmed small HCC nodules was admitted to our department (Figure 1). The two lesions could not be operated on through one puncture. The patient developed intolerable pain during RFA. He received RFA two times for curative treatment of the HCC lesions. The first day after the second RFA, the patient suffered from fever, chills, and abdominal pain. A computed tomography (CT) scan showed low-attenuated areas under the liver capsule (Figure 2). Hemostatic measures were provided according to the imaging finding and a simultaneous drop in the hemoglobin level. One week later, his symptoms were relieved and he was discharged from our hospital.

Computed tomography shows two hepatocellular carcinoma nodules (arrow).
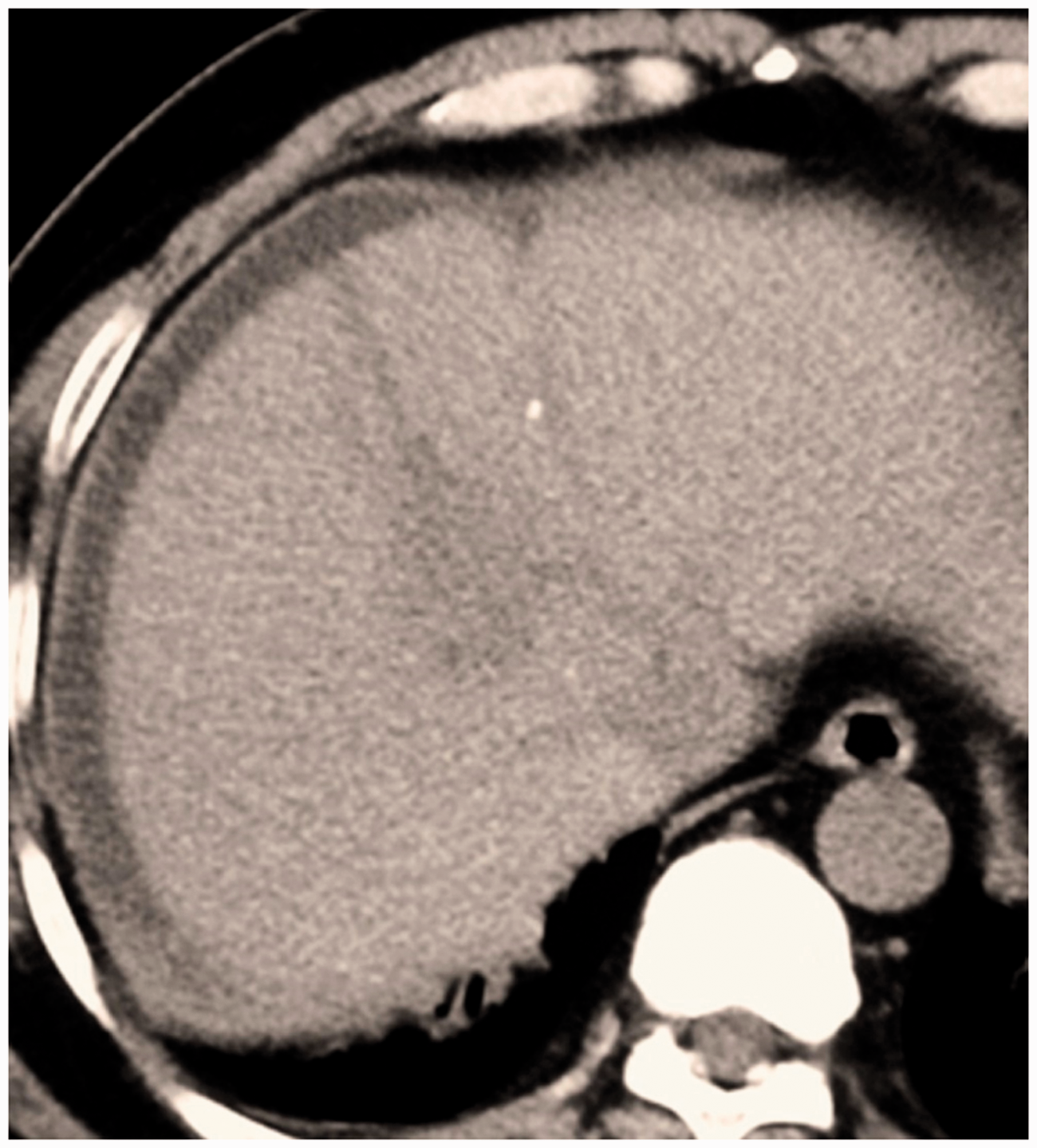
A computed tomography scan shows low-attenuated areas under the liver capsule
Two weeks after discharge, the patient had fever, chills, and abdominal pain again. A CT scan showed 18 × 13-cm fluid collection under the liver capsule (Figure 3). Percutaneous catheter drainage was performed with an 8-French catheter. The contents were bilious fluid (approximately 2000 mL). The bilirubin level in the fluid was 52.8 µmol/L. Drainage was continued with a volume of 600 to 800 mL of bile fluid per day, without any sign of reduction. Magnetic resonance cholangiopancreatography (MRCP) was performed and showed stenosis in the right hepatic bile duct (Figure 4). By contrast, ERCP showed no stenosis in the hepatic bile ducts. However, spasm of the duodenal ampulla was found to be persistent and a guidewire encountered resistance when passing through the duodenal ampulla and common bile duct. A plastic stent was placed from the duodenal ampulla to the common bile duct (Figure 5). A considerable decrease in bile drainage was encountered in the following days of the stent placement. The percutaneously placed drainage catheter was removed 1 week after the biloma had totally disappeared on a follow-up CT scan. The patient was discharged home with no more abdominal pain, but sometimes experienced a slight fever. Three weeks later, the plastic stent was removed. The patient did not feel any discomfort and entered the out-patient follow-up procedure. CT scans after 6 months, and 1 and 2 years showed no recurrence of the biloma and HCC lesions, while the distal branch of the right upper bile ducts was slightly distended (Figure 6).

Fluid collection of 18 × 13 cm was observed under the liver capsule

Magnetic resonance cholangiopancreatography shows stenosis in the right hepatic bile duct

(a) Spasm of the duodenal ampulla (arrow). (b) A plastic stent was placed from the duodenal ampulla to the common bile duct (arrow)
Computed tomography scan after 6 months shows no recurrence of the biloma and hepatocellular carcinoma lesions, while the distal branch of the right upper bile duct is slightly distended (arrow)
Discussion
Chang et al. 8 reported that 109 (3.3%) bilomas occurred in 3284 sessions of RFA. In other large groups of patients,9–11 symptomatic biloma occurred in 0.2% to 1.3% of them after RFA. Development of a large intrahepatic biloma after RFA, which is rare, was first reported in 2003. 12 In that case, the biloma was cured in more than 2 months after percutaneous catheter drainage for the biloma and ERCP stenting. However, the patient died 6 months later with the internal stent still in place. In our patient, the biloma was cured within only 1 month and the drainage catheter and ERCP stent were then removed. To the best of our knowledge, this is the shortest time for treatment among any patient who has suffered from a huge biloma after RFA.
Diagnosing and treating a biloma as early as possible are important for patients. Ultrasonography, CT, MRI, MRCP, and ERCP are useful for diagnosing a biloma. 13 If a lesion is observed is association with an injured biliary tree, or the contents are bilious fluid (the bilirubin level in the fluid must be must be much higher than that in the blood), a biloma can be confirmed. Hepatic subcapsular hemorrhage, which can also occur after RFA, is an important differential diagnosis.
Rupture of the bile duct is considered as the first important reason for formation of a biloma. 12 Additionally, increased intraductal pressure, which is usually caused by spasm of the sphincter of Oddi, obstruction by a tumor or stone, or necrosis of a portion of the bile duct wall, is another precondition for leaking bile accumulating in the cavity. 5,14–16 MRCP or ERCP can be used to observe stenosis or obstruction in the bile duct.
Percutaneous catheter drainage is preferred for treating a huge biloma, and this can promote the bile duct to heal. 17 However, in some cases, huge bilomas cannot be treated only by drainage. Although ERCP has been incriminated in the occurrence of biliary tract rupture, 18 endoscopic management can be simultaneously used to lower pressure in the biliary tree. Drainage and ERCP management are an effective method of treating bilomas.5,14,19 In our patient, ERCP showed spasm of the sphincter of Oddi, while MRCP showed that there may be stenosis in the right hepatic bile duct. Once a stent was placed in the common bile duct to lower the pressure, the amount of drainage was greatly reduced.
Our experience suggests that decompression treatment by both drainage and endoscopic means should be considered in patients with huge bilomas. Additionally, we consider that the ERCP stent should be removed in several weeks after complete resolution of a huge biloma.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
