Abstract
Objective
To present and discuss the clinical course, management, recurrence and survival of patients with thymoma at a single centre.
Methods
This prospective observational study included patients with confirmed thymoma who were diagnosed and managed over a 10-year period.
Results
The study included 89 patients (mean ± SD age, 48.53 ± 11.60 years). There were 46 (51.7%) males and 43 (48.3%) females. The mean duration of follow-up was 60 months (range, 2 months to 8 years). Stage II was the most common stage (37 [41.6%]), followed by stage I with 30 (33.7%) patients, stage IIIA with 11 (12.4%) patients, stage IVA with six (6.7%) patients and stage IIIB with five (5.6%) patients. Overall (actuarial) 5-year survival was achieved by 84 of 89 patients (94.4%). Stage-specific survival was as follows: 100% in stage I (30 of 30 patients), 100% in stage II (37 of 37 patients), 54.5% in stage IIIA (six of 11 patients), 80.0% in stage IIIB (four of five patients) and 50.0% in stage IVA (three of six patients).
Conclusion
Complete surgical resection is the main modality used for the definitive diagnosis, staging and surgical cure of thymoma.
Introduction
Thymoma, which is a neoplasm of the thymic epithelium, is the most frequent tumour occurring in the anterior mediastinum and is regarded as a low-grade malignant disease with relatively good clinical outcomes after total resection. 1 Thymoma has little potential to spread through lymphatic or blood vessels, however, it retains the capacity for local invasion and pleural seeding. 2
The most common clinical presentation of thymoma is symptoms and signs of myasthenia gravis (MG), which occur in approximately 45% of cases, followed by accidental finding (30%); other symptoms such as chest pain, shortness of breath, cough, weakness or weight loss can also be the first presenting symptoms. 3 Diagnosis can be achieved by excisional biopsy if the mass is resectable, as well as by chest computed tomography (CT)-guided fine needle aspiration, mediastinoscopy or thoracoscopy. Recently, endobronchial ultrasound-guided transbronchial needle aspiration has been used for the diagnosis of thymoma; however, in most cases, a tumour specimen is necessary to define the subtypes and determine the stage of the tumour.4,5
Classification of thymoma based on histological appearance has been previously discussed thoroughly and several systems have been proposed. 3 Recently, consensus based on recommendations by the International Committee of the World Health Organization (WHO) was established, which categorized thymomas into three main types: predominantly epithelial (type A); predominantly lymphocytic (type B); and mixed (type AB). 6 Although the prognostic significance of histological classification has not been confirmed, some studies have shown its relevance to survival.3–8
Resection of thymoma remains the main therapeutic strategy with a prominent impact on local recurrence-free long-term survival. 9 Many studies have shown the beneficial effect of postoperative radiotherapy on overall disease outcomes.10–12 In cases of advanced invasive thymoma, preoperative chemotherapy has been advocated by several authors.1,2,9
Unfortunately, the clinical course of thymomas is unpredictable as the presentations are variable, histopathological types are interchangeable and recurrence might occur long after successful resection.6,9 The aim of this present study was to present and discuss the clinical course, management, recurrence and survival of patients with thymoma at a single centre in Kurdistan /Iraq.
Patients and methods
Study design and protocol
This prospective observational study included patients with thymoma diagnosed and managed over 10 years between January 2008 and January 2018 from a group of patients with mediastinal masses treated at the Department of Cardiovascular and Thoracic Surgery, School of Medicine, Faculty of Medical Sciences, University of Sulaimani, Al Sulaymaniyah, Kurdistan/Iraq. The study was registered at the Research Registry (www.researchregistry.com; registration number: researchregistry4967). All patients underwent surgery in the same public hospital (Sulaimani Surgery Teaching Hospital, Al Sulaymaniyah, Kurdistan/Iraq). The procedure was performed by the same surgeon with 15 years of experience as a thoracic surgeon (A.B.) and his team. All patients with confirmed thymoma were included in this study. Any patients with no histological proof of thymoma were excluded from this study. Written informed consent was obtained from all patients for both research purposes and publication of the confidential data. This study was approved by the Institutional Review Board of the Kurdistan Board for Medical Specializations (both scientific content and ethic committee. The work has been reported in accordance with the 2007 STROBE criteria checklist. 13
The duration of the data collection extended for over 10 years while some patients were followed-up for shorter periods of time. All patients had a regular monthly follow-up visit scheduled for the first 3 months postoperatively, followed by three additional visits for the first year and then annually after the first year. Chest X-rays (Figure 1) and chest CT scans (Figure 2) were undertaken for all patients. When other diseases such as lymphoma were suspected, fine needle aspiration cytology (FNAC) under CT guidance and/or mini-anterior mediastinotomy (Chamberlain procedure) was performed to obtain tissue diagnosis. After optimization of the general condition, under general anaesthesia, median sternotomy (or ministernotomy if the lesion was small and well capsulated) was performed for complete surgical resection (Figure 3). Thoracoscopic resections were not done due to the lack of appropriate facilities in our centre. Patients were staged according to the eighth edition of the TNM classification. 14
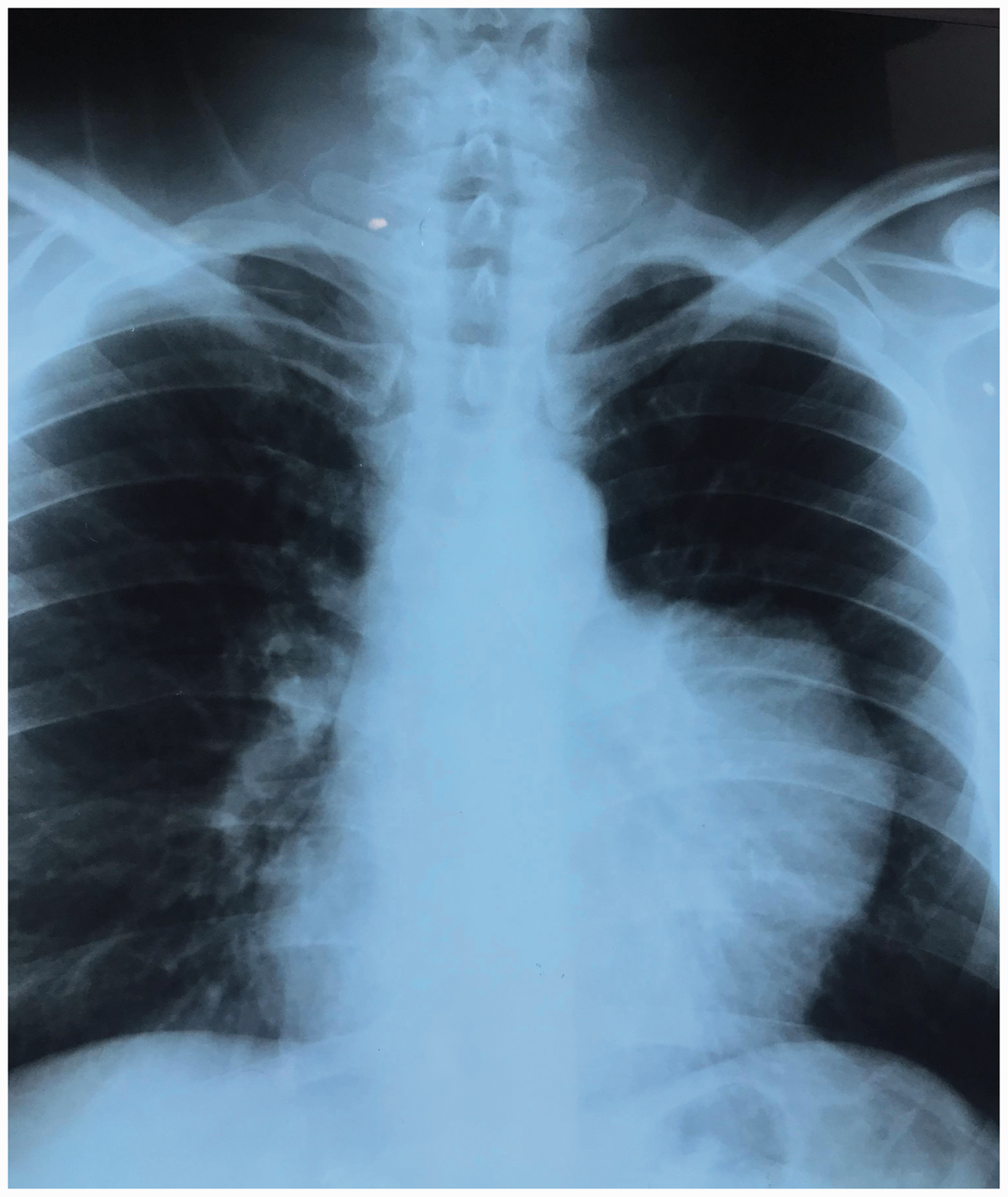
Representative posteroanterior chest X-ray of a patient with thymoma showing a large mediastinal mass.
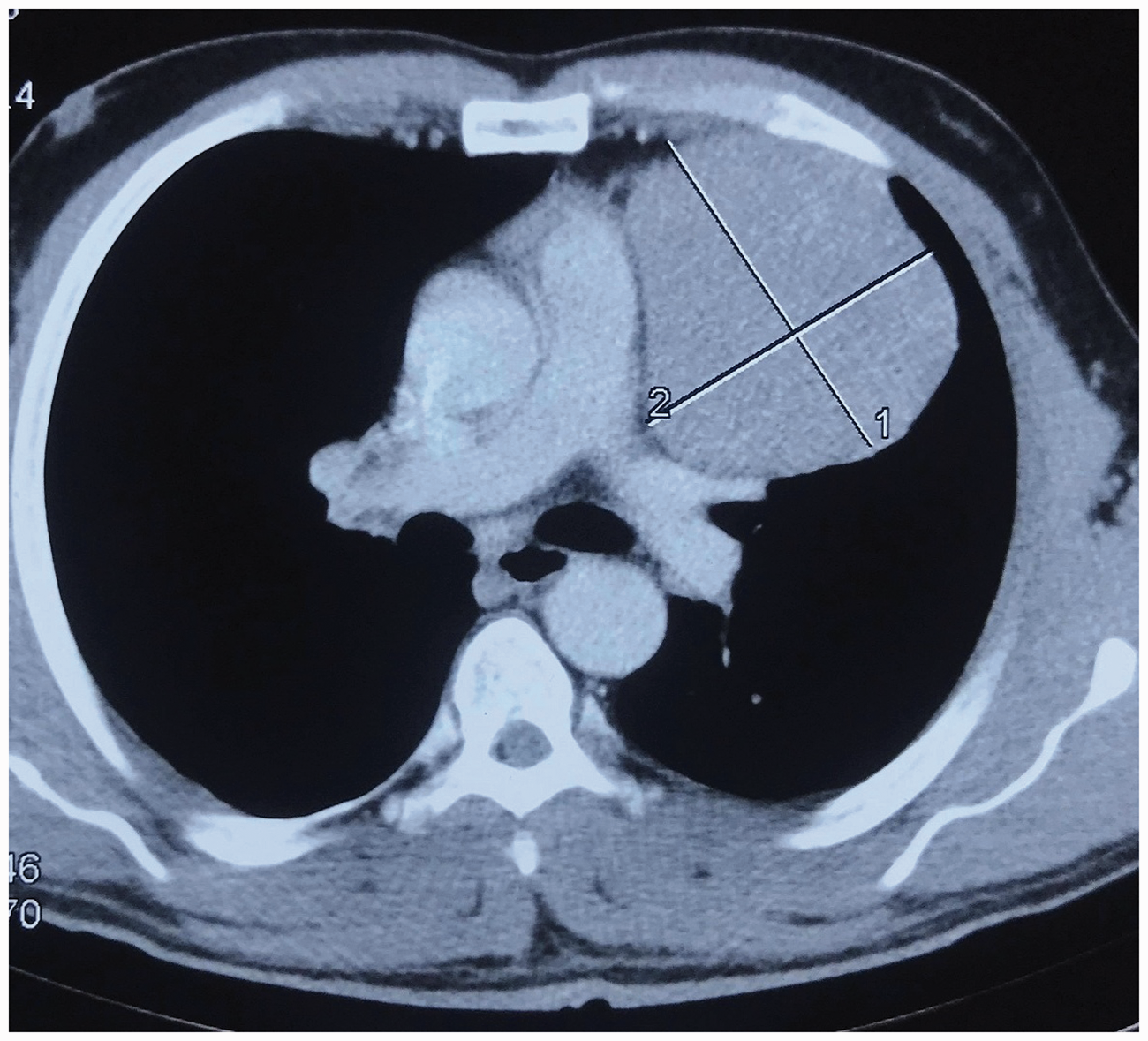
Representative chest computed tomography scan of a patient with thymoma showing a large anterior mediastinal mass.

Representative photograph showing a median sternotomy for radical resection of an anterior mediastinal mass in a typical patient with thymoma.
Postoperative radiotherapy was used in patients with stages II, IIIA, IIIB and IVA; adjuvant chemotherapy was also administered in patients with stage IVB if their general condition was reasonable.
Clinical data collection
For each patient, data regarding sex, age, past medical history, quantitative history of smoking, presentations, features of MG, investigations, stage of the disease, concomitant malignant diseases, management strategy and complete follow-up were obtained from the hospital medical records. Only patients who had confirmed thymoma were included in this study; patients with all other suspicious histopathologies were excluded.
Statistical analyses
Data entry and coding were done using Microsoft Excel 2010 (Microsoft, Redmond, WA, USA). Then the data were transferred to and analysed using IBM SPSS Statistics for Windows, Version 24.0. (IBM Corp., Armonk, NY, USA). Descriptive statistics (mean ± SD; n [%]) were used to present socio-demographic and clinical data. χ2-test was used to compare categorical data. Kaplan–Meier plots were used to produce cumulative survival curves according to different staging and histological types. The graphs were compared using log-rank tests. Patients with other concomitant malignant diseases were excluded from the analysis during survival calculations in order to alleviate confounding effects. Any P-value ≤ 0.05 was considered statistically significant.
Results
This prospective observational study identified 487 patients with mediastinal masses. Of these, 89 patients with a mean ± SD age of 48.53 ± 11.60 years (range, 26–79 years) that had confirmed thymoma were included in the study. There were 46 males (51.7%) and 43 females (48.3%). The mean duration of follow-up was 60 months (range, 2 months to 8 years). A total of 33 (37.1%) patients were current smokers; and six patients (6.7%) were former smokers. The most common past medical disease was hypertension, which was found in 29 (32.6%) patients, followed by type 2 diabetes mellitus in 17 (19.1%). The most common presentation was MG occurring in 22 (24.7%) patients. Table 1 shows the clinical presentations of the patients.
Clinical presentations of the patients with thymoma (n = 89) that were analysed in this prospective observational study.

Tumour sizes according to the CT scan findings demonstrated a mean ± SD diameter of 4.38 ± 1.72 cm (range, 1.6–9.0 cm). FNAC was performed in five (5.6%) patients and only positive for malignancies in two patients (40.0%) without defining the subtype and clinical stage. Anterior mediastinotomy was performed in three (3.4%) patients.
According to the WHO histological classification, type A thymomas were found in 30 (33.7%) patients, type B in 24 (27.0%) patients and type AB in 35 (39.3%) patients. Stage II was the most common stage (37 [41.6%]), followed by stage I with 30 (33.7%) patients, stage IIIA with 11 (12.4%) patients, stage IVA with six (6.7%) patients and stage IIIB with five (5.6%) patients.
Eighty-seven patients (97.8%) were managed with median sternotomy and wide local excision, and two patients (2.2%) underwent ministernotomy. The following neighbour structures were involved and resected in one patient for each structure (1.1%): right phrenic nerve; right upper lobe (wedge resection); segment of left brachiocephalic vein; pericardium; pleura; left upper lobe (wedge resection); middle lobe (wedge resection); and left aortopulmonary (lymph nodes). The mean ± SD duration of hospital stay was 3.98 ± 2.07 days (range, 2–12 days). Postoperative radiotherapy was administered in 18 (20.2%) patients and chemoradiotherapy was given in one case (1.1%). One patient (1.1%) received pre- and postoperative radiotherapy. Three patients (3.4%) with stage III did not receive adjuvant therapy as they did not consent to treatment.
No intraoperative complications were reported in 73 (82.0%) patients; delayed recovery ± intubation for < 72 h occurred in five (5.6%) patients and surgical site infections occurred in three patients (3.4%). Other complications reported in one patient each (1.1%) were minor pulmonary embolism, elevated left hemi-diaphragm, chest infection, inferior myocardial infarction, signs of cerebral oedema, prolonged air leak lasting for 12 days and inhalational pneumonitis. The latter was treated with 3 days of continuous positive air way pressure. There was a single operative mortality that occurred on the second postoperative day.
Local recurrence was reported in four (4.5%) patients: two patients with stage III, two patients with stage IVB progression despite free margins, and none from the other stages (P < 0.0001; intergroup comparison). Among the histological types, three patients were type A, none were type B and one was type AB. This type of recurrence in type A thymoma was extremely surprising, so the slide interpretation was independently verified by three different pathologists. Three patients were excluded from the survival analysis because of concomitant malignancies (colonic cancer, gastric cancer and lymphoma). Two patients experienced pulmonary recurrences.
Overall (actuarial) 5-year survival was achieved by 84 of 89 patients (94.4%). Stage-specific survival was as follows: 100% in stage I (30 of 30 patients), 100% in stage II (37 of 37 patients), 54.5% in stage IIIA (six of 11 patients), 80.0% in stage IIIB (four of five patients) and 50.0% in stage IVA (three of six patients) (Figure 4). Actuarial 5-year survival was also not significantly correlated with histological type: two patients were type A, one was type B and two were type AB (Figure 5).

Actuarial 5-year survival according to disease stage from the time of operation to death or the most recent follow-up in patients (n = 89) with thymoma The colour version of this figure is available at: http://imr.sagepub.com.

Actuarial 5-year survival according to histological type from the time of operation to death or the most recent follow-up in patients (n = 89) with thymoma. The colour version of this figure is available at: http://imr.sagepub.com.
Discussion
Myasthenia gravis is the most common clinical presentation of thymoma. 15 Approximately 10% of patients with MG have thymoma, while one-third to one-half of thymoma cases have MG.13,14 In this current study, features of MG were reported in less than one-quarter of patients. It remains to be determined if this difference is significant or not. Further studies are necessary to confirm and explain this deviation from the international data.15,16 There were no post-thymectomy crises in this current study.
Wide local resection of thymoma is still regarded as the mainstay of thymoma management; it has been shown to have a remarkable impact on the overall survival. 17 Nonetheless, even after total removal of the neoplasm, recurrence may happen in 9–29% of patients.18,19 A 19% recurrence rate was reported in a series of 126 cases. 1 In the current study, the overall recurrence rate was 4.5%. The low recurrence rate observed in this current series may be explained by the short duration of the follow-up 60 months (range 2 months to 8 years) in comparison with other studies,18,19as it is well known that the recurrence of thymoma can occur many years (sometimes decades) after successful surgical resection.6,9 A problem associated with the long-term follow-up of patients that have undergone thymoma resection is that when they are asymptomatic, they no longer request medical consultations, which makes it hard to follow their progress. As a result, it is the surgeon’s job to contact these patients for further follow-up. A previous report described a case of thymoma that recurred 32 years after complete surgical resection. 20 Recurrence has been reported in all stages of thymoma. 18 In this current study, no recurrence was observed in stages I and II, which was in agreement with two previous studies.1,2 Although recurrence is usually constrained to the anterior mediastinum, intrathoracic pleural seeding may occur. 3 However, extrathoracic metastases are rare. 9 A previous study reported pulmonary and pleural recurrence in 14 cases out of 24 recurrences. 18 In addition, pericardial and pleural recurrences were found in two cases and spinal cord recurrence in one case out of seven recurrent patients. 3 Two patients experienced pulmonary recurrences in the current study.
There are considerable controversies regarding prognostic factors in thymoma.18,19 This can be explained by several reasons: thymoma is a rare disease, it is anatomically and clinically polymorphic and grows slowly, several classification systems have been proposed, and almost all published studies are retrospective.2,20 Some authors have confirmed that the only prognostic factor is the type of resection, with the complete resection offering the best chance of disease-free survival and subtotal resection increasing the risk of long-term recurrence and mortality. 1 Previous data have shown that MG in patients with thymoma is an unfavourable prognostic indicator, although this was challenged by recent data.15,16 In an analysis of 1089 patients with thymoma, a 6.4% recurrence rate was found in the group with MG compared with an 8.3% recurrence rate in the group without MG, but the difference was not statistically significant. 16 In a previous study of 797 patients (47% with MG), univariate analysis showed that MG had a significant beneficiary effect on actuarial survival. 17 In the current study, although statistically insignificant, recurrence was found in four (4.5%) cases and none of them had MG.
The histological type is another area of debate when one considers prognostic factors in thymoma.3,12,21–23 An analysis of a registry of 273 patients with thymoma over 40 years (18 with type A, 178 with type B, 77 type with AB) concluded that when histological classification was adopted, it reflected the oncological and clinical behaviour of the neoplasm. 6 The 20-year survival rates were best for type A (100%), followed by mixed type (87%), while type B was subdivided into three other subtypes with different survival rates (B1 91%, B2 59% and B3 36%). 6 However, multivariate analysis failed to show any significant effect of histological classification in a study that included 307 patients with a mean follow-up of eight years.18,23 In the present study, four patients experienced thymoma recurrence (three patients with type A, none with type B and one with type AB). Actuarial 5-year survival was also not significantly correlated with histological type (Figure 5): two patients were type A, one was type B and two were type AB.
In the present study, the overall (actuarial) 5-year survival was 94.4%. The stage-specific survival was as follows: 100% in stage I, 100% in stage II, 54.5% in stage IIIA, 80% in stage IIIB and 50% in stage IVA (Figure 4). Overall 5-year survival rate among the different stages in the current report agrees with other studies for some stages (stage I, stage II, stage III and stage IVB) and disagrees for other stages (stage IVA).8,14,16 This may be explained by the small sample size in the present study and the short duration of follow-up in some patients.
The current study had several important limitations. First, crucial data such as postoperative anti-MG medications and type B histological subtypes were missing. Secondly, the small sample size made some apparently significant comparisons became statistically insignificant. Thirdly, the short duration of follow-up was a limitation as the recurrence of thymoma may occur decades after complete surgical resection.
In conclusion, thymoma is the most common anterior mediastinal tumour. Thymoma may present with the signs and symptoms of MG or be found accidentally during work-up for other diseases. Complete surgical resection is the main modality of definitive diagnosis, staging and surgical cure. Long-term follow-up is mandatory as it has a tendency to recur long after complete surgical resection. Further studies are recommended, as controversies remain regarding its clinical pathology and the oncological behaviour of this disease.
Footnotes
Acknowledgement
The author acknowledges all personnel who assisted in serving their patients.
Declaration of conflicting interest
The author declares that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
