Abstract
Atypical hemolytic uremic syndrome (aHUS) is an ultra-rare disease induced by many triggers, all of which produce a common end phenotype of microangiopathic hemolysis and thrombotic microangiopathy. We herein describe a 63-year-old woman with ongoing protein-losing enteropathy and frequent transudates caused by hypoalbuminemia. The patient was treated with eculizumab with a full hematologic and partial renal response. Protein-losing enteropathy is an inflammatory condition that has been linked with increased complement activation, which can trigger aHUS in patients with loss of CD55 expression. The patient in the present case had an increased estimated glomerular filtration rate but stage IV to V chronic kidney disease. One year later, she remains off dialysis with a stable estimated glomerular filtration rate. We herein report an unusual trigger of complement activation that in turn triggered aHUS in this patient.
Keywords
Introduction
Atypical hemolytic uremic syndrome (aHUS) is a rare disorder with a population incidence of 2/1,000,000. aHUS is a state of systemic thrombotic microangiopathy with continuous microangiopathic hemolysis that occurs as a result of complement overactivation and dysregulation. The actual incidence is likely to be slightly higher than that reported, and missed diagnosis probably accounts for a large volume of unrecognized cases. 1 The triggers for aHUS are diverse and unknown in about 31% of cases. However, infectious, inflammatory, malignant, and drug-induced complement-amplifying triggers are known etiologies that trigger the cascade of complement dysregulation. 2 Protein-losing enteropathy (PLE) is an unusual trigger for aHUS, and a molecular link was recently found to suggest a possible underlying association between the two conditions.3,4
We herein describe a 63-year-old woman who was diagnosed with aHUS and PLE. The aHUS was treated with C5 complement blockade with complete hematological remission and partial improvement in renal function. We herein report the association of PLE as an inflammatory condition that may serve as a potential trigger for complement activation in patients with aHUS.
Case report
This report describes a 63-year-old woman with a medical history of PLE with a baseline serum albumin level of 1.5 to 1.6 g/L and chronic transudative bilateral pleural effusion. The patient had first developed gastrointestinal symptoms in 2016, starting with chronic diarrhea. She had no history of proteinuria, cirrhosis, or congestive heart failure. The patient also had no family history of clotting events, pregnancy loss, or PLE. She required serial thoracentesis for the recurrent pleural effusion.
From May to July 2018, she began to develop gradually worsening anemia, with a decline in the hemoglobin concentration to 7.4 g/dL from a baseline of 10.0 to 11.6 g/dL. She also developed thrombocytopenia of 48 × 103 platelets/µL from a baseline of 129 to 193 × 103 platelets/µL. Additionally, her serum creatinine concentration increased to 4.2 mg/dL from a baseline of 0.8 to 1.3 mg/dL. Her coagulation indices were within normal limits (prothrombin time, 14.8 seconds; international normalized ratio, 1; and activated partial thromboplastin time, 37 s). A peripheral smear was positive for schistocytes, and the lactate dehydrogenase concentration was 500 IU/L.
Shiga toxin was undetected in the patient’s stool, and human immunodeficiency virus serology was negative. The patient had no evidence of lupus anticoagulant and had a negative anti-cardiolipin test (1.9 GPL units; reference range, 0.0–14.9 GPL units). The C3 level was 115 mg/dL, the C4 level was 40 mg/dL, and the total hemolytic complement level was 63 CAE units. No additional complement panel testing, soluble membrane attack complex testing in blood or urine, or genetic testing was performed because of insurance coverage and cost limitations.
The patient was started on plasmapheresis for presumed thrombotic thrombocytopenic purpura, which was stopped after a normal ADAMTS13 activity level of 48% was noted, and diagnosis of aHUS was made. She was started on eculizumab, and her serum creatinine concentration improved to 2.1 mg/dL (see Figure 1). She was treated with eculizumab at 900 mg weekly for 4 weeks and thereafter remained on the standard regimen of 1200 mg every other week.
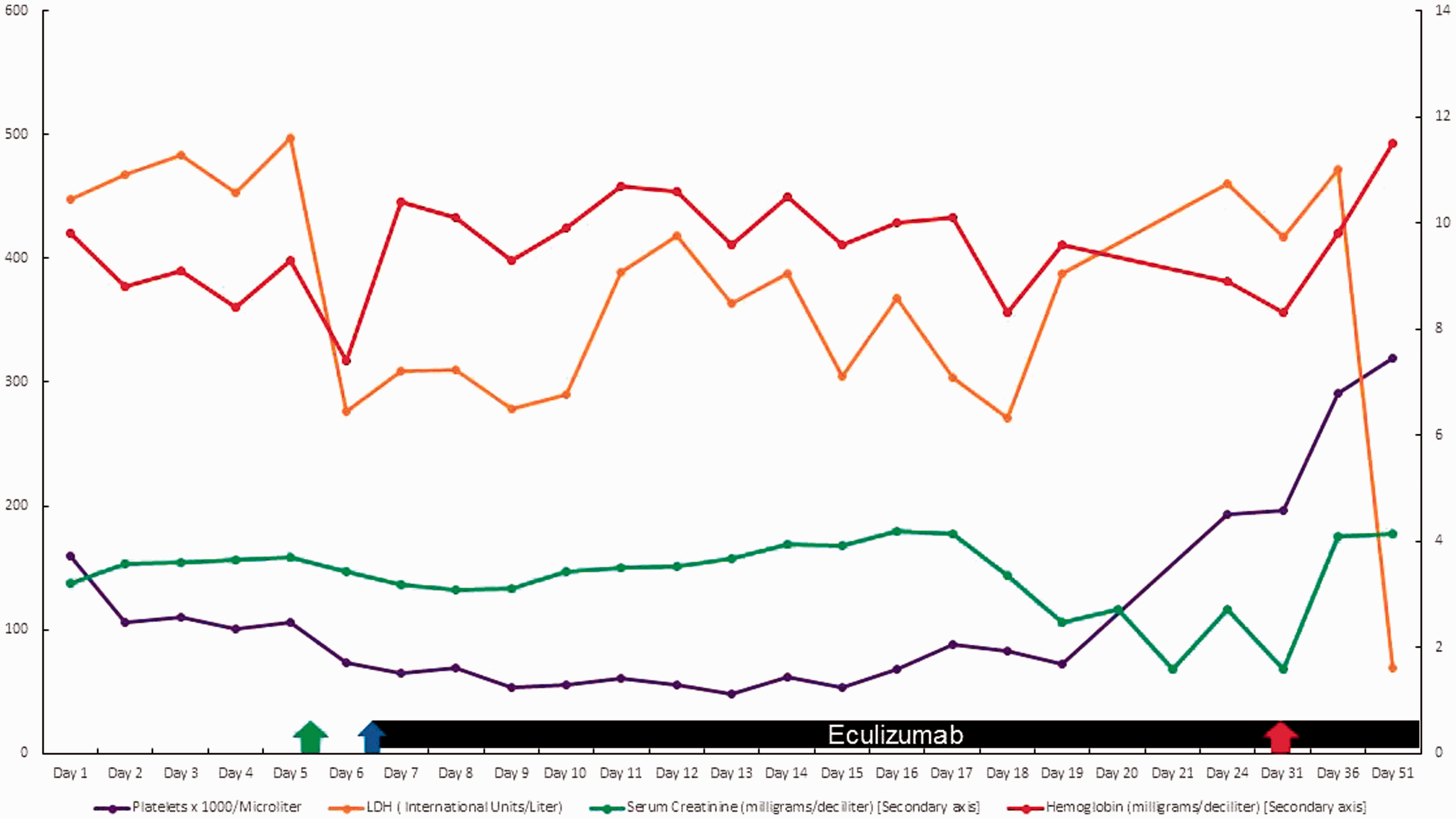
Trends of platelets (×1000//Microliter), serum LDH (IU/L), serum creatinine (mg/dL) (on secondary axis), and hemoglobin (mg/dL) (on secondary axis) Blue arrow = start of eculizumab, green arrow = start of dialysis, and red arrow = stopping of dialysis. LDH, lactate dehydrogenase
The patient was started on dialysis on 5 July 2018 (day 5) and continued until her serum creatinine nadir reached 1.6 mg/dL on 30 July 2018 (day 30). Her serum creatinine concentration increased after the discontinuation of dialysis in late July 2018 and remained at 3 to 4 mg/dL, with an estimated glomerular filtration rate of 20 m/minute, and she was asked to prepare for starting peritoneal dialysis at another institution. She presented to the UCLA Health System to obtain a second opinion and inquire about the availability of other agents for the treatment of aHUS besides eculizumab, which at the time of treatment was not commercially available or approved by the United States Food and Drug Administration (US FDA). Her symptoms of PLE persisted, but her serum albumin concentration improved to 1.9 to 3.1 g/dL.
For this case report, we did not apply for institutional review board approval because such approval is not required for individual case reports in our institution (University of California Los Angeles). Written consent was retrospectively obtained from the patient and documented, on the condition that no identifiable data be published.
Discussion
The link between PLE and aHUS is not well recognized but has been reported in the literature. In 2017, Ozen et al. 3 evaluated a cohort of 11 patients with PLE and found increased complement deposition and loss of CD55 expression. The identification of a protein called complement decay-accelerating factor provides a direct link explaining why complement hyperactivation is present in patients with PLE. 3 The role of decay-accelerating factor in regulating complement has also been long known and studied. 4 Importantly, our patient had no family history of PLE and genetic testing for CD55 was not readily available at our institution.
Our patient’s diagnosis of aHUS was based on clinical and serological findings; she presented with laboratory data suggestive of aHUS rather than thrombotic thrombocytopenic purpura. The presentation of more severe renal failure and less severe thrombocytopenia is highly sensitive for aHUS versus thrombotic thrombocytopenic purpura as described by Coppo et al. 5 The patient did not require hemodialysis after initiation of eculizumab; this is congruent with the findings in the US FDA trials of eculizumab (specifically C-008-02 and C-008-03). 6 Recovery of kidney function was evident when complement blockade was started 1 week after her initial diagnosis. Unfortunately, she did not experience complete remission but rather partial recovery of her acute kidney injury. As such, she remained with stage IV to V chronic kidney disease. The data regarding eculizumab indicate that it improves renal function by an estimated glomerular filtration rate of 15 mL/minute in roughly 50% of patients and that 80% of patients who are started on eculizumab can stop dialysis. 7
Many patients with aHUS recover a high percentage of kidney function, but some have more modest renal recovery. Continuing eculizumab therapy was recommended in this case according to the data presented by Macia et al. 8 in 2017. These authors showed a 31% relapse rate of thrombotic microangiopathy upon stopping complement blockade. A newer study by Olson 9 showed that this high rate of relapse is the rule in all cases of aHUS, suggesting that some patients will do well with a shorter course of therapy. Studies that specifically focused on the rate of relapse after eculizumab discontinuation showed that 27% of patients relapsed off the drug but that the majority of those patients who relapsed had a genetic mutation.10–14 The risk of relapse remains clinically significant, and which subgroups of patients will do better with discontinuation of eculizumab remains controversial.13,14
Genetic testing for aHUS is recommended because only about 50% to 60% of patients have identifiable mutations, and finding new mutations will improve the accuracy of prognostication and advance the study of aHUS.15,16 However, genetic testing could not be performed in our case because of the high out-of-pocket cost. Figure 2 shows new and old genetic loci associated with aHUS, including vitronectin, which was recently described by Bu et al. 16 At the time of this writing, our patient’s aHUS was in hematologic remission and partial renal remission, and although she remained on eculizumab therapy, no other adjunctive agents were approved for use. C3 blockade is expected to be available in the US and Europe in the near future 17 and might be helpful in combination therapy or as a replacement for eculizumab or C5 blocking agent. These agents are pending approval until the results of US FDA clinical trials on their use in aHUS are available.

Genetics of atypical hemolytic uremic syndrome including newly described genetic mutations
Footnotes
Declaration of conflicting interest
Dr. Ramy M. Hanna and Dr. Richard Burwick are consultants and speakers for Alexion Pharmaceuticals and are part of the 2019 Speaker’s Bureau. However, this case report was not sponsored in any way.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
