Abstract
Background
We performed a systematic review and meta-analysis to evaluate the efficacy and safety of minimally invasive radical cystectomy (MIRC) versus open radical cystectomy (ORC) for bladder cancer.
Methods
We searched the EMBASE and MEDLINE databases to identify randomized controlled trials (RCTs) of MIRC versus ORC in the treatment of bladder cancer.
Results
Eight articles describing nine RCTs (803 patients) were analyzed. No significant differences were found between MIRC and ORC in two oncologic outcomes: the recurrence rate and mortality. Additionally, no significant differences were found in three pathologic outcomes: lymph node yield, positive lymph nodes, and positive surgical margins. With respect to perioperative outcomes, however, MIRC showed a significantly longer operating time, less estimated blood loss, lower blood transfusion rate, shorter time to regular diet, and shorter length of hospital stay than ORC. The incidence of complications was similar between the two techniques. We found no statistically significant differences in the above outcomes between robot-assisted radical cystectomy and ORC or between laparoscopic radical cystectomy and ORC with the exception of the complication rate.
Conclusions
MIRC is an effective and safe surgical approach in the treatment of bladder cancer. However, a large-scale multicenter RCT is needed to confirm these findings.
Keywords
Introduction
Bladder cancer (BCa) is a common malignancy worldwide that is associated with age and smoking and that seriously affects the health of the advanced-age population. 1 BCa is also the most common urological malignancy in China, where it has a high incidence and recurrence rate; among individuals aged >75 years, the incidence is 69.7/100,000 population. 2 For patients with muscle-invasive BCa or high-risk non-muscle-invasive BCa, open radical cystectomy (ORC) is the gold standard surgical treatment. 3 With the development of surgical techniques, minimally invasive radical cystectomy (MIRC) has become more widely used in recent years. MIRC techniques include laparoscopic radical cystectomy (LRC) and robot-assisted radical cystectomy (RARC), both of which are associated with lower morbidity than conventional surgery.4,5 Many studies have compared the advantages and disadvantages between MIRC (LRC or RARC) and ORC.6–15 For example, Tang K et al. 14 performed a meta-analysis and found that RARC seems to be a safer and less invasive treatment than ORC. Tang JQ et al. 15 also performed a meta-analysis that suggested that RARC is a more minimally invasive treatment than ORC for BCa and has the advantage of reducing bleeding. However, these meta-analyses lacked enough randomized controlled trials (RCTs) to prove their findings. In recent years, increasingly more RCTs have been performed to compare MIRC and ORC in terms of oncologic, perioperative, and pathologic variables and complications. Therefore, the aim of our meta-analysis was to evaluate the efficacy and safety of MIRC and ORC in the treatment of BCa.
Materials and methods
Search strategy
We searched the EMBASE and MEDLINE databases to identify all RCTs that focused on the use of MIRC and ORC in the treatment of BCa. We also searched the references of the retrieved articles. The following search terms were used: “open radical cystectomy,” “laparoscopic radical cystectomy,” “robot-assisted radical cystectomy,” and “randomized controlled trials.”
Inclusion criteria and trial selection
All identified articles were screened by two independent reviewers, and a third reviewer was involved if there was a discrepancy. The inclusion criteria for RCTs were as follows: (i) The study included MIRC and ORC for the treatment of BCa; (ii) accurate data were available and could be analyzed, including the total number of patients and the values of each index; and (iii) the full text of the included study was available. When the same study was published in different journals or years, the most recent publication was used for the meta-analysis. If the same group of researchers conducted multiple experiments on a group of patients, each study was included. A flow chart of the selection process is shown in Figure 1.

Flow diagram of the study selection process. RCT, randomized controlled trial.
Quality assessment
The methodological quality of each RCT was assessed in terms of the means of patient allocation to various arms of the study, allocation concealment, blinding, and loss to follow-up. Additionally, the methodological quality of each cohort study was assessed in terms of the means of patient allocation to various arms of the study, exposure variables and covariates, sample size calculation, and propensity score matching. The patients were then classified qualitatively according to the guidelines published in the Cochrane Handbook for Systematic Reviews of Interventions 5.1.0. 16 According to the quality evaluation standard, each study was evaluated using one of the following quality categories: A, quality criteria were met adequately, and the study was deemed to have a “low” risk of bias; B, quality criteria were met only partially or were unclear, and the study was deemed to have a “moderate” risk of bias; and C, quality criteria were not met or not included, and the study was deemed to have a “high” risk of bias. Differences were resolved by discussion among the reviewers.
Data extraction
Data included in the study were extracted and cross-checked by two reviewers. Any differences were settled through discussion or by a third person. The following information was collected from reports of the original experiment: the name of the first author and the publication year, country in which the study was carried out, study design, participants’ age, number of participants, follow-up duration, surgical approach, and outcome measures. The main outcome was oncologic outcomes, and the secondary outcomes were perioperative and pathologic variables and complications.
Statistical analysis and meta-analysis
The meta-analysis was conducted using Review Manager (RevMan) 5.1.0 (The Nordic Cochrane Centre, The Cochrane Collaboration, Copenhagen, Denmark). The meta-analysis revealed no evidence of publication bias according to the results of a funnel plot. Continuous variables are presented as the mean difference (MD) with 95% confidence interval (CI). The odds ratio (OR) with 95% CI was computed for all dichotomous variables. A fixed-effects model was used if there was no conspicuous heterogeneity; otherwise, a random-effects statistical model was used. Tests for heterogeneity were conducted using the I2 statistic with the level of significance set at P < 0.05. Funnel plots were used to assess publication bias. Tests of the lowest quality were excluded. The individual outcome evaluation was performed using the Grading of Recommendations, Assessment, Development, and Evaluation (GRADE) guidelines, and the quality of individual outcomes was divided into four grades as follows: high, medium, low, and very low.
Ethics
Ethics approval was not necessary because all included studies had already obtained ethical approval from relevant institutions.
Results
Characteristics of the individual studies
Our database search revealed 215 articles that could have been included in our meta-analysis. After reading the title and abstract of each article and applying the inclusion and exclusion criteria, 194 articles were excluded. Thirteen articles lacked useful data and were not RCTs. Finally, eight articles reporting data from a total of nine RCTs (803 patients)17–24 were included in the meta-analysis: six RCTs compared RARC with ORC, and three RCTs compared LRC with ORC. The baseline characteristics of the studies included in our meta-analysis are listed in Table 1.
Main characteristic and quality assessment of eligible studies.

RARC, robot-assisted radical cystectomy; ORC, open radical cystectomy; LRC, laparoscopic radical cystectomy; RCT, randomized controlled trial; NA, data not available.
*Grade A: if all quality criteria were adequately met, the study was deemed to have a low risk of bias.
Quality of the individual studies
All nine RCTs were double-blinded, and all described the randomization processes that they had used. All included a power calculation to determine the optimal sample size. Each study was of quality level A (Table 1). A funnel plot was used to qualitatively estimate publication bias, and no evidence of bias was found (Figure 2). The risk of bias of the individual studies is shown in Table 2.

Funnel plot of the studies represented in this meta-analysis. OR, odds ratio; SE, standard error; RARC, robot-assisted radical cystectomy; ORC, open radical cystectomy; LRC, laparoscopic radical cystectomy.
Risk of bias of individual studies.

+, low risk of bias; ?, unclear risk of bias; −, high risk of bias.
Outcomes of oncologic variables
Recurrence rate and mortality
Five RCTs involving 565 patients (282 in the MIRC group and 283 in the ORC group) included data on the recurrence rate. We found no heterogeneity among the studies, and we used the OR to express the effect size for the meta-analysis. The pooled estimate of OR was 0.95 (95% CI, 0.66–1.37) (Figure 3). Five RCTs involving 553 patients (277 in the MIRC group and 276 in the ORC group) included data on mortality. We found no heterogeneity among the studies, and we used the OR to express the effect size for the meta-analysis. The pooled estimate of OR was 0.91 (95% CI, 0.60–1.37) (Figure 4). These results suggest that there was no significant difference in the postoperative recurrence rate or mortality between MIRC and ORC.

Forest plots showing the outcome of the recurrence rate. M-H, Mantel–Haenszel; CI, confidence interval; df, degrees of freedom.

Forest plots showing the outcome of mortality. M-H, Mantel–Haenszel; CI, confidence interval; df, degrees of freedom.
Outcome of pathologic variables
Lymph node yield, positive lymph nodes, and positive surgical margins
Eight RCTs involving 706 patients (354 in the MIRC group and 352 in the ORC group) included data on the lymph node yield. The pooled estimate of MD was −1.43 (95% CI, −3.75–0.89) (Figure 5).

Forest plots showing the outcome of the lymph node yield. SD, standard deviation; IV, inverse variance; CI, confidence interval; df, degrees of freedom.
Four RCTs involving 284 patients (144 in the MIRC group and 140 in the ORC group) included data on positive lymph nodes. The pooled estimate of MD was 0.97 (95% CI, 0.53–1.75) (Figure 6).

Forest plots showing the outcome of positive lymph nodes. M-H, Mantel–Haenszel; CI, confidence interval; df, degrees of freedom.
Eight RCTs involving 708 patients (354 in the MIRC group and 354 in the ORC group) included data on the positive surgical margins. The pooled estimate of MD was 1.00 (95% CI, 0.50–2.03) (Figure 7). These results suggest that there were no significant differences in the lymph node yield, positive lymph nodes, or positive surgical margins between MIRC and ORC.
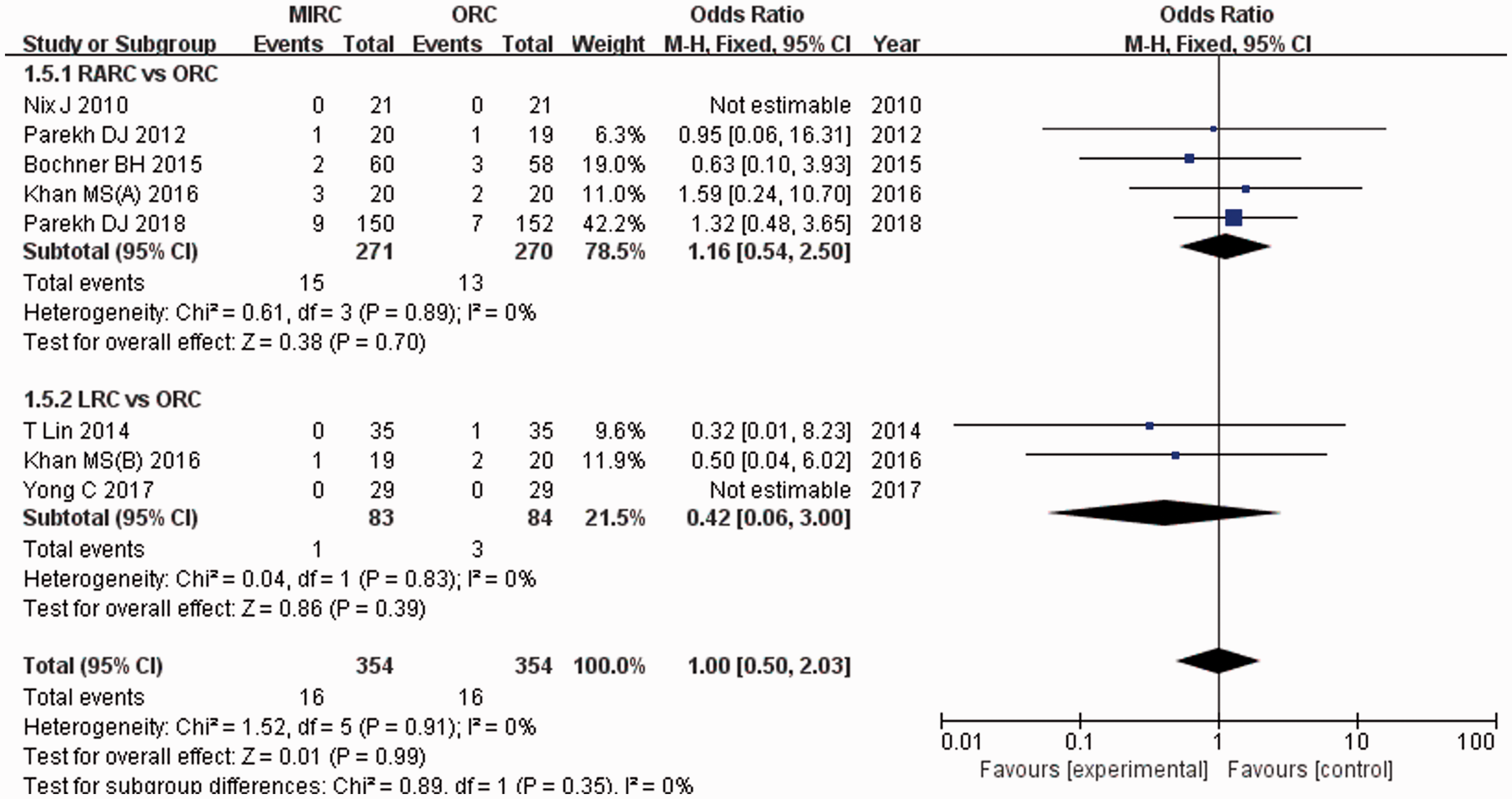
Forest plots showing the outcome of positive surgical margins. M-H, Mantel–Haenszel; CI, confidence interval; df, degrees of freedom.
Outcomes of perioperative variables
Operating time, estimated blood loss, blood transfusion rate, time to regular diet, and length of hospital stay
Eight RCTs involving 706 patients (354 in the MIRC group and 352 in the ORC group) included data on the operating time. The pooled estimate of MD was 62.90, (95% CI, 36.02–89.78; P < 0.00001) (Figure 8). Eight RCTs involving 706 participants (354 in the MIRC group and 352 in the ORC group) included data on the estimated blood loss. The pooled estimate of MD was −338.78 (95% CI, −422.22 to −255.33; P < 0.00001) (Figure 9). Four RCTs involving 468 patients (234 in the MIRC group and 234 in the ORC group) included data on the blood transfusion rate. The pooled estimate of OR was 0.46 (95% CI, 0.30–0.70; P = 0.0002) (Figure 10). Six RCTs involving 286 patients (144 in the MIRC group and 142 in the ORC group) included data on the time to regular diet. The pooled estimate of MD was −0.70 (95% CI, −0.93 to −0.46; P < 0.00001) (Figure 11). Eight RCTs involving 705 patients (354 in the MIRC group and 351 in the ORC group) included data on the length of hospital stay. The pooled estimate of MD was −0.93 (95% CI, −1.32 to −0.54; P < 0.00001) (Figure 12). These results suggest that MIRC had a significantly longer operating time, less blood loss, lower blood transfusion rate, shorter time to regular diet, and shorter length of hospital stay than ORC.
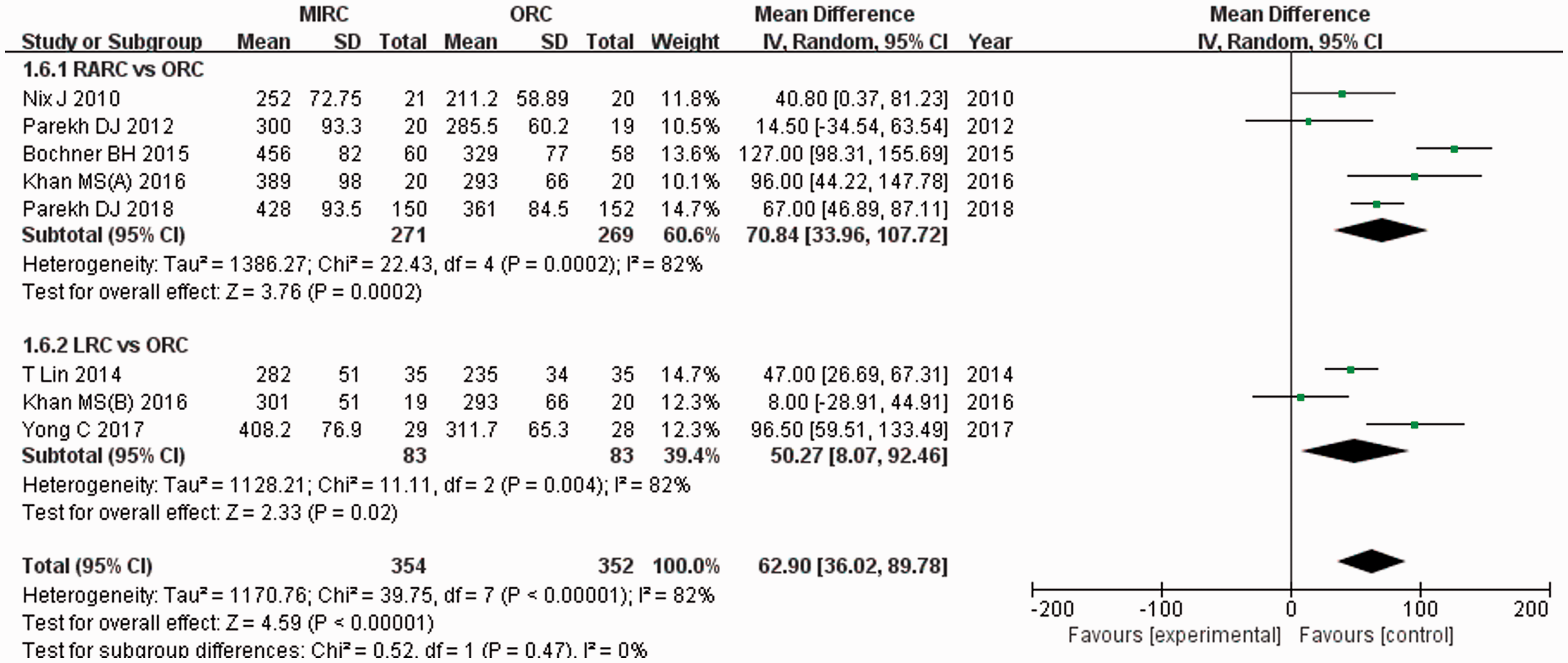
Forest plots showing the outcome of the operating time. SD, standard deviation; IV, inverse variance; CI, confidence interval; df, degrees of freedom.

Forest plots showing the outcome of estimated blood loss. SD, standard deviation; IV, inverse variance; CI, confidence interval; df, degrees of freedom.

Forest plots showing the outcome of the blood transfusion rate. M-H, Mantel–Haenszel; CI, confidence interval; df, degrees of freedom.

Forest plots showing the outcome of the time to regular diet. SD, standard deviation; IV, inverse variance; CI, confidence interval; df, degrees of freedom.

Forest plots showing the outcome of the length of hospital stay. SD, standard deviation; IV, inverse variance; CI, confidence interval; df, degrees of freedom.
Outcomes of complications
Eight RCTs involving 707 patients (354 in the MIRC group and 353 in the ORC group) included data on the complication rate. We found no heterogeneity among the studies, and we used the OR to express the effect size for the meta-analysis. The pooled estimate of OR was 0.75 (95% CI, 0.54–1.03; P = 0.07) (Figure 13). This result suggests that the complication rate was similar between MIRC and ORC.

Forest plots showing the outcome of the complication rate. M-H, Mantel–Haenszel; CI, confidence interval; df, degrees of freedom.
Subgroup analysis and GRADE assessment of individual outcomes
The surgical approaches in the MIRC group were RARC and LRC (Table 1). We therefore divided the included studies into two groups: RARC and LRC. Again, we conducted subgroup analyses for the outcomes of oncologic, perioperative, pathologic and variables and complications (Figures 3–13). We found no statistically significant difference in the recurrence rate (I2 = 0%), mortality (I2 = 0%), lymph node yield (I2 = 0%), positive lymph nodes (I2 = 0%), positive surgical margins (I2 = 0%), operating time (I2 = 0%), estimated blood loss (I2 = 6.3%), blood transfusion rate (I2 = 14%), time to regular diet (I2 = 0.3%), or length of hospital stay (I2 = 0%) between RARC versus ORC or LRC versus ORC. The data suggested that the LRC group had fewer complications than the ORC group (OR, 0.5; P = 0.03). However, the performance of RARC did not significantly reduce the complications compared with ORC (OR, 0.86). The results of the GRADE assessment of individual outcomes are shown in Table 3.
GRADE assessment of individual outcomes.

GRADE, Grading of Recommendations Assessment, Development, and Evaluation; OR, odds ratio; MD, mean difference; RARC, robot-assisted radical cystectomy; ORC, open radical cystectomy; LRC, laparoscopic radical cystectomy.
Discussion
BCa is a common malignancy of the urinary system. 25 ORC with pelvic lymphadenectomy is the gold standard treatment for high-risk BCa. Minimally invasive surgical approaches have been recommended for various surgical treatments of BCa with the hope of improving the complications and recovery. In recent years, several studies have demonstrated the potential benefits of LRC and RARC for the treatment of patients with BCa.26,27 One study showed that MIRC could shorten the length of stay and reduce the 90-day episode cost compared with ORC, but there was no significant difference in the readmission rate between MIRC and ORC. 28
Notably, most reports on MIRC are retrospective studies; prospective randomized trials are limited. The RCTs included in our meta-analysis were prospective randomized trials and more convincing. Tang K et al. 14 performed a meta-analysis to compare robotic surgery with ORC in the treatment of BCa. However, the study included in the meta-analysis was only one RCT and unpersuasive. Lauridsen et al. 6 also conducted a meta-analysis that included four RCTs, but the results were not comprehensive and only included complications and health-related quality of life. Tang JQ et al. 15 performed a meta-analysis that only focused on RARC versus ORC.
Our meta-analysis included nine prospective randomized trials, and the outcomes were comprehensive. We also performed a subgroup analysis to further compare RARC versus ORC and LRC versus ORC. The outcomes of our meta-analysis suggest that MIRC and ORC in the treatment of BCa were not significantly different with respect to oncologic variables (recurrence rate and mortality) or pathologic variables (lymph node yield, positive lymph nodes, and positive surgical margins). This indicates that MIRC is as effective as ORC, which is considered to be the gold standard in the treatment BCa. However, our assessment of the perioperative variables and complications suggested that MIRC has a longer operating time, less estimated blood loss, lower blood transfusion rate, shorter time to regular diet, shorter length of hospital stay, and similar complication rate compared with ORC. These findings indicate that MIRC has more advantages over ORC and is a more effective and safe surgical approach than ORC in the treatment of BCa.
Furthermore, the results of our subgroup analysis showed no statistically significant difference in the recurrence rate, mortality, lymph node yield, positive lymph nodes, positive surgical margins, operating time, estimated blood loss, blood transfusion rate, time to regular diet, or length of hospital stay between RARC versus ORC or LRC versus ORC. The data also suggested that LRC was associated with fewer complications than ORC. However, the performance of RARC did not significantly reduce the complications compared with ORC. Overall, the results of our meta-analysis show that MIRC (RARC and LRC) is a safe and effective surgical approach in the treatment of BCa.
All of the trials on robotic surgery were performed with an extracorporeal approach, which might have affected the results of our analysis. Future trials including the iROC 29 and the RAZOR 24 trials are currently recruiting patients for comparison of extracorporeal and intracorporeal diversions in RARC. When assessing MIRC procedures, it is important to specify the type of urinary diversion performed and whether it was performed intracorporeally or extracorporeally. This information is essential because it may have a major bearing on the outcome of perioperative variables such as the operation time, length of hospital stay, blood loss, and complication rate. Clinically, when assessing the feasibility of upcoming techniques and their oncologic outcomes, it is important to ensure that there is appropriate follow-up. In the present analysis, patients were followed up for BCa progression or death of any cause at 4 to 6 weeks, then every 3 to 6 months for a minimum of 2 years after cystectomy. The serum hemoglobin, creatinine, and albumin concentrations were measured at baseline and at 4 to 6 weeks and 3, 6, 12, 24, and 36 months postoperatively.
Although this meta-analysis included only prospective RCTs and the quality of the individual studies was conforming, there were some important limitations in our analysis. First, the sample sizes of the subgroups were small. Additionally, unpublished studies were excluded. These factors may have led to bias. Second, there were significant differences in the adequacy of the randomization process and blinding methodology. Third, the results may be measured in different ways, and the researchers involved were different; for example, the extent of pelvic lymph node dissection (standard or extended) was based on the patient’s condition, institutional preference, and level of operation, which would determine the lymph node yield. Finally, potential selection bias may have affected the homogeneity between groups, and the relatively small sample sizes limited the statistical power for identifying true associations. After considering the heterogeneity between individual studies, this meta-analysis remains important for assessing the efficacy and safety of MIRC in the treatment of BCa. We suggest that more high-quality randomized trials with larger samples are needed to learn more about MIRC versus ORC in the treatment of BCa.
Conclusion
This meta-analysis suggest that MIRC is a safe and effective surgical approach in the treatment of BCa. However, large-scale multicenter randomized controlled study is still needed to further confirm.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This work was supported by grants from the Natural Science Foundation of Ningxia (NZ17164, NZ17166).
