Abstract
Objective
This study was performed to investigate whether a definite correlation exists between alteration of blood biochemical parameters and immunosuppressive therapies in patients with inflammatory bowel disease (IBD).
Methods
A comprehensive search of PubMed, EMBASE, MEDLINE, and the Cochrane Library was conducted. Data on alterations in white blood cells, platelets, hemoglobin, serum creatinine, and liver enzymes in patients with IBD treated with immunomodulators were extracted.
Results
Data from 1141 patients were included. The relative risk (RR) of leukopenia was significantly higher in the immunosuppressive therapies group than in the placebo group (RR, 12.91; 95% confidence interval [CI], 5.28–31.57). A statistically significant risk of leukocytosis during immunosuppressive therapies was observed (RR, 1.53; 95% CI, 1.05–2.23). Patients taking immunomodulators had increased risks of serum creatinine elevation (RR, 10.68; 95% CI, 2.07–55.12) and serum aminotransferase elevation (RR, 3.18; 95% CI, 1.24–8.17).
Conclusion
Immunosuppressive therapies might have an impact on variations in blood biochemical parameters in patients with IBD. Although the conclusion regarding leukopenia was reliable in this study, some confounding factors might reduce the reliability of the conclusions about leukocytosis, creatinine elevation, and aminotransferase elevation. Close monitoring is recommended during immunosuppressive therapies for IBD.
Keywords
Introduction
Inflammatory bowel disease (IBD) is a chronic relapsing and remitting intestinal inflammatory disorder consisting mainly of ulcerative colitis (UC) and Crohn’s disease (CD).1,2 However, the etiology remains unclear. Environmental, genetic, and immune factors are generally considered to contribute to IBD in a complicated network system.3–5 Current conventional therapies for IBD, including aminosalicylates, corticosteroids, and immunosuppressants, play an important role in most developing countries.6,7
Immunosuppressants, especially azathioprine (AZA) and its active metabolite 6-mercaptoprine (6-MP), have been extensively used in maintenance therapy for IBD.8–10 These drugs are also widely used to induce remission in moderate to severe IBD, IBD with steroid dependence or steroid resistance, and fistulizing CD.10,11 The recent European Crohn’s and Colitis Organization consensus on the management of IBD emphasizes the importance of immunosuppressive therapy based on cost-efficiency.12,13 AZA treatment could produce up to 50% mucosal healing in patients with IBD. 14 Furthermore, clinical trials and evidence-based reviews demonstrated that the efficacy of infliximab in the early stages increased with combination therapy involving immunomodulators.15–18
Despite considerable evidence regarding the efficacy and safety of immunosuppressants for patients with IBD, these agents may be associated with some uncommon adverse events, including bone marrow suppression, 19 opportunistic infection,20–21 lymphoma,22–24 and pancreatitis.19,25 Prolonged immunosuppressive treatment may increase the risk of sepsis and lead to compromised healing, resulting in the formation of abscesses from internal fistulas. 13
Emerging evidence suggests that blood biochemical parameters are altered in patients with IBD who are receiving immunosuppressive therapies.26–48 These alterations, including changes in the erythrocyte, leukocyte, and platelet counts and the serum creatinine and aminotransferase concentrations, may imply greater risks of infection, coagulation disorders, and hepatic and renal toxicity. However, no comprehensive meta-analysis has focused on this issue to date.
Given the lack of a conclusive association between immunosuppressive therapies and alterations in blood biochemical parameters, we performed the first systematic review and meta-analysis based on the accumulation of data in published studies. The primary aim was to determine the relationship between immunosuppressive therapies and blood biochemical parameters. If an association was found, we planned to investigate which blood biochemical parameter was most frequently and substantially modified after immunosuppressive treatment. We further sought to determine whether different types of immunosuppressive agents had different effects on blood chemistries.
Methods
Literature retrieval and study selection
A medical literature search of PubMed, EMBASE, MEDLINE, and the Cochrane Library (up to April 2016) was conducted. The selection criteria were as follows:
Double-blind, randomized controlled trials (RCTs) Adults (>90% of patients aged >16 years) with a clinical diagnosis of IBD Comparison of placebo versus any types of immunosuppressive agents (e.g., 6-MP, AZA, methotrexate [MTX], cyclosporine, or tacrolimus) administered orally, intramuscularly, or intravenously Minimum therapy duration of 14 days Reporting of adverse effects of immunosuppressive agents on blood biochemical parameters (leukocytes, blood platelets, hemoglobin, serum creatinine, or hepatic enzymes) based on quantitative laboratory analyses
When necessary, the first and senior authors of the studies were contacted to provide additional information on individual trials.
To identify potentially eligible studies, literature searches were conducted using the terms CD, IBD, colitis, ileitis, or UC as Medical Subject Headings (MeSH) and as free-text terms, or CD and regional enteritis as free-text terms. These searches were combined using the set operator AND; studies were identified with the terms immunosuppressor or immunosuppressant (as MeSH terms and free-text terms) or the following free-text terms: MTX, AZA, 6-MP, thiopurine analog, Imuran, cyclosporine, tacrolimus, immunosuppressive, and antimetabolites.
The literature search was conducted with no language restrictions. The lead investigator independently evaluated the abstracts of papers identified in the initial search for appropriateness to the study question. All potentially relevant articles were obtained and evaluated in detail. The articles published in non-English or non-Chinese languages were translated when necessary. Two investigators independently assessed articles using predesigned eligibility forms according to the predefined inclusion criteria. Any disagreement between the investigators was resolved by discussion with a third investigator.
Data extraction
All data were extracted independently by two investigators. We assessed the therapy-induced changes in laboratory parameters, including quantitative changes in white blood cells (WBCs), platelets, hemoglobin, serum creatinine, and liver enzymes. The following clinical data were collected for each trial: number of study centers, country of origin, disease type (UC or CD) and distribution, patients’ demographic data, type of immunosuppressants, duration of therapy, and concomitant medications allowed.
Quality assessment
Risk of bias was assessed using the criteria described in the Jadad scale 49 and the Cochrane Handbook, which was updated to the latest version. The assessments included the method used to generate the randomization schedule, the method used to hide allocation, whether a double-blind method was adopted, the proportion of patients who completed follow-up, whether an intention-to-treat analysis was extractable, and whether evidence of selective reporting of outcomes existed. This process was performed independently by two investigators. Studies were considered to have a “low risk of bias” when a quality score of >3 had been achieved. Any disagreement between investigators was resolved by reconciliation and/or discussion with a third investigator.
Statistical analysis and publication bias
The outcomes of the above-mentioned blood biochemical parameters were selected separately to conduct a meta-analysis of the studies that met the inclusion criteria and the requirements of quality assessment.
Review Manager (RevMan) version 5.1 (The Nordic Cochrane Centre, The Cochrane Collaboration, Copenhagen, Denmark) was employed to generate forest plots of pooled relative risks (RRs) with 95% confidence intervals (CIs) as well as the results of heterogeneity tests. Pooled RRs were calculated by the Mantel–Haenszel method for all analyses by combining the RR of the individual studies into a global RR. Heterogeneity tests were performed to assess whether the variation across trials was due to true heterogeneity or chance. This quantity was termed I2, and a value of ≤25% combined with a P value of >0.1 for the heterogeneity test was arbitrarily chosen to represent low levels of heterogeneity. When significant heterogeneity was present, a random-effects model was used for combinatorial effects; otherwise, a fixed-effects model was adopted.
Funnel plots were also performed to evaluate the publication bias. The funnel plots were estimated by observing whether the distribution of the funnel plots was symmetrical. If the number of studies was too low to draw a funnel plot, Egger’s test was performed via Stata 12.0 (StataCorp, College Station, TX, USA), with a P value of >0.05 indicating no publication bias. When possible, we also performed a subgroup analysis based on the type of immunosuppressants or subtypes of IBD.
Ethics
Ethics committee approval was not required because this study was a meta-analysis, which focuses on published data, not living individuals.
Results
Literature retrieval and characteristics of included studies
The broad search strategy identified 4325 citations, of which 4302 were excluded after examining the title and abstract. Twenty-three articles reporting on the adverse effects of immunosuppressive therapies in IBD were retrieved and evaluated in more detail.26–48 Seven studies were disqualified for miscellaneous reasons (Figure 1), leaving 16 articles with 17 RCTs eligible for inclusion. Of these, 10 articles reported leukopenia caused by immunosuppressive drugs compared with placebo in IBD,26–35 2 reported leukocytosis,36,37 2 reported increased platelet counts,28,36 2 reported serum creatinine elevation,37,38 and 3 reported serum aminotransferase elevation.39–41 The study outcomes are summarized in Tables 1 and 2.

Flow diagram of assessment of studies identified in the systematic review. RCTs, randomized controlled trials; IBD, inflammatory bowel disease.
Eligible RCTs of immunosuppressive medications in patients with CD.

*Cross-over trial.
#Average age of patients in immunosuppressive agents group and placebo group, respectively.
RCTs, randomized controlled trials; WBCs, white blood cells; Hb, hemoglobin; AZA, azathioprine; 6-MP, 6-mercaptopurine; MTX, methotrexate; CS, corticosteroids; PSL, prednisolone; PS, prednisone; 5-ASA, 5-aminosalicylic acid; SSZ, sulfasalazine; ABS, antibiotics; ADR, antidiarrheals; CD, Crohn’s disease.
Eligible RCTs of immunosuppressive medications in patients with UC.

*Average age of patients in immunosuppressive agents group and placebo group, respectively.
RCTs, randomized controlled trials; WBCs, white blood cells; Hb, hemoglobin; AZA, azathioprine; 6-MP, 6-mercaptopurine; MTX, methotrexate; HCS, hydrocortisone; PSL, prednisolone; PS, prednisone; SSZ, sulfasalazine; UC, ulcerative colitis.
Risk of leukopenia with immunosuppressive therapies versus placebo in IBD
We identified 10 eligible RCTs reporting leukopenia in 542 patients with IBD.26–35 Of these patients, 273 (50.4%) were randomized to receive immunosuppressive therapies and 269 were randomized to receive placebo. Sixty-two patients had leukopenia among all patients receiving immunosuppressive therapies, but no patients had leukopenia among those receiving placebo. The RR of leukopenia was significantly higher with immunosuppressive therapies than with placebo (RR, 12.91; 95% CI, 5.28–31.57; P < 0.05) (Figure 2), with no statistically significant heterogeneity detected between studies (I2 = 0%). However, statistically significant funnel plot asymmetry was present (Egger test, P = 0.004), suggesting the existence of publication bias.
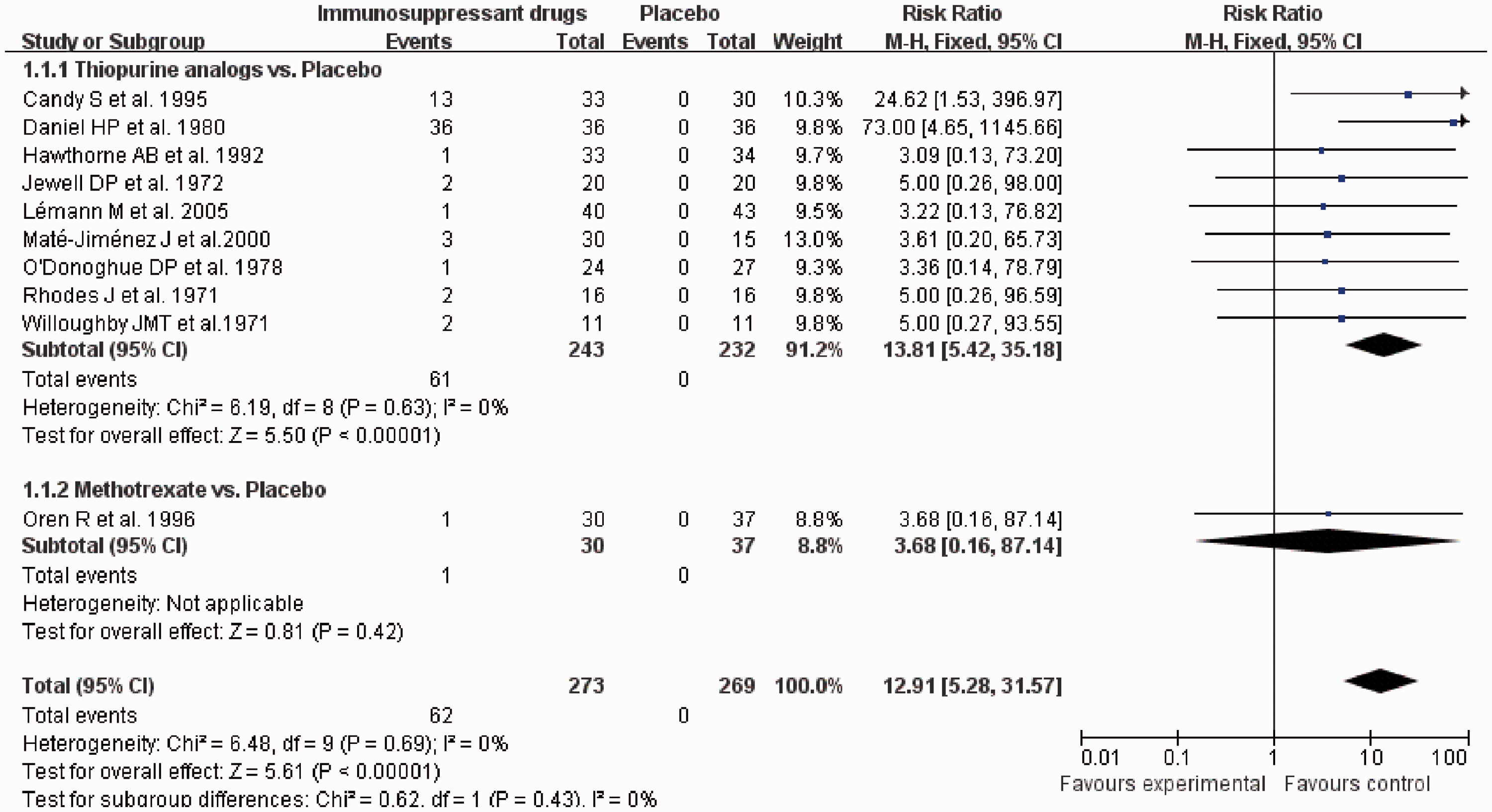
Forest plot for overall analysis of controlled trials evaluating leukopenia among randomized controlled trials of immunosuppressive agents versus placebo in inflammatory bowel disease. Results are expressed as mean difference versus control arms and 95% CI using the M-H method. Subgroup analysis was conducted between thiopurine analogs and methotrexate. M-H, Mantel–Haenszel; CI, confidence interval.
We subsequently performed a subgroup analysis according to the types of immunosuppressive drugs in the eligible RCTs (AZA/6-MP vs. placebo; MTX vs. placebo). AZA/6-MP was more likely to induce leukopenia than placebo (RR, 13.81; 95% CI, 5.42–35.18; P < 0.05) (Figure 2). However, the difference in the RR between MTX and placebo was not statistically significant (RR, 3.68; 95% CI, 0.16–87.14).
Risk of leukocytosis with immunosuppressive therapies versus placebo in IBD
Three RCTs in two articles reported increased WBC counts with immunosuppressive drugs compared with placebo.36,37 No significant heterogeneity was present between the studies (I2 = 18%). A statistically significant benefit of placebo over immunosuppressive therapy was detected (RR, 1.53; 95% CI, 1.05–2.23; P < 0.05) (Figure 3). No funnel plot asymmetry was present, suggesting no evidence of publication bias or small study effects. However, with only three trials, the power of this test is limited.

Forest plot for overall analysis of controlled trials evaluating leukocytosis among randomized controlled trials of immunosuppressive agents versus placebo in inflammatory bowel disease. Results are expressed as mean difference versus control arms and 95% CI using the M-H method. Subgroup analysis was conducted between thiopurine analogs and methotrexate. M-H, Mantel–Haenszel; CI, confidence interval.
Risk of platelet count elevation with immunosuppressive therapies versus placebo in IBD
Three trials involving 117 patients with IBD reported platelet count elevation after immunosuppressive therapies compared with placebo.28,36 Significant heterogeneity was present between the studies (I2 = 67%, P = 0.05). Thus, a random-effects model was used to pool these RCTs. The RR of the increased platelet count compared with placebo was 0.79 (95% CI, 0.17–3.69) (Figure 4), with no statistically significant funnel plot asymmetry.

Forest plot for overall analysis of controlled trials evaluating platelet count elevation among randomized controlled trials of immunosuppressive agents versus placebo in inflammatory bowel disease. M-H, Mantel–Haenszel; CI, confidence interval.
Risk of serum creatinine elevation with immunosuppressive therapies versus placebo in IBD
Only two trials provided extractable data of serum creatinine elevation in 228 patients.37,38 An increased serum creatinine concentration was reported in 14 of 110 patients receiving immunosuppressive drugs compared with 1 of 118 receiving placebo. Statistically significant differences in the serum creatinine elevation were detected during immunosuppressive therapy compared with placebo (RR, 10.68; 95% CI, 2.07–55.12; P < 0.05) (Figure 5). No statistically significant heterogeneity was present between the studies (I2 = 0%).

Forest plot for overall analysis of controlled trials evaluating serum creatinine elevation among randomized controlled trials of immunosuppressive agents versus placebo in inflammatory bowel disease. Results are expressed as mean difference versus control arms and 95% CI using the M-H method. Subgroup analysis was conducted between thiopurine analogs and methotrexate. M-H, Mantel–Haenszel; CI, confidence interval.
Risk of serum aminotransferase elevation with immunosuppressive therapies versus placebo in IBD
Three RCTs reported serum aminotransferase elevation in 224 patients with IBD.39–41 The serum aminotransferase concentration increased in 15 patients receiving immunosuppressive therapy and in 4 receiving placebo. No statistically significant heterogeneity was present between the studies (I2 = 0%). There was no evidence of funnel plot asymmetry. A statistically significant difference in the serum aminotransferase elevation was found with immunosuppressive therapy compared with placebo (RR, 3.18; 95% CI, 1.24–8.17; P < 0.05) (Figure 6).

Forest plot of overall analysis of controlled trials evaluating serum aminotransferase elevation among randomized controlled trials of immunosuppressive agents versus placebo in inflammatory bowel disease. Results are expressed as mean difference versus control arms and 95% CI using the M-H method. Subgroup analysis was conducted between thiopurine analogs and methotrexate. M-H, Mantel–Haenszel; CI, confidence interval.
We conducted a subgroup analysis according to the type of immunosuppressive agents (AZA/6-MP vs. placebo; MTX vs. placebo). MTX was more likely to induce a serum aminotransferase elevation than placebo (RR, 3.20; 95% CI, 1.19–8.60; P < 0.05) (Figure 6). However, the RR between AZA/6-MP and placebo was not statistically significant (RR, 3.00; 95% CI, 0.13–70.30) (Figure 6).
Discussion
To the best of our knowledge, this is the first comprehensive meta-analysis focusing on the relationship between immunosuppressive therapies and alteration of blood biochemical parameters in patients with IBD. Our meta-analysis included 17 RCTs with data from 1141 patients (875 with CD, 266 with UC).
Patients receiving immunosuppressive agents were at greater risk of leukopenia than patients receiving placebo (RR, 12.91; 95% CI, 5.28–31.57; P < 0.01). However, in the subgroup analysis, we observed no statistically significant differences in leukopenia between the MTX group and the placebo group, while AZA/6-MP treatment significantly increased the risk of leukopenia (RR, 13.81; P < 0.05). In our clinical impression, leukopenia occurred in some patients who had received MTX therapy, and the lack of a significant difference between the MTX group and placebo group was most probably because only one eligible RCT was included, leading to a very small sample size for the analysis. We also analyzed the adverse effects of immunosuppressant use on the WBC count by specifying the disease to CD and UC, and we found that immunosuppressive agent use significantly reduced the WBC count in patients with CD (P < 0.01) (Figure S1). Although there was no statistical significance for UC, a strong trend in the incidence of leukopenia was observed during immunosuppressive agent use compared with placebo in patients with UC (7/113 vs. 0/106, respectively) (Figure S1).
In addition to reducing the WBC counts, immunosuppressive agents were also reported in three RCTs to have possible underlying effects on leukocytosis. This result is contradictory to that mentioned above; however, leukopenia and leukocytosis were observed in different RCTs included in our research. After carefully reviewing these studies, we speculated that there may be two explanations for the contradictory results. First, moderate leukocytosis may be a result of cotreatment with corticosteroids, which were used in most of the included RCTs. Second, leukopenia occurred mainly during AZA/6-MP treatment, and leukocytosis was observed during administration of three kinds of immunosuppressive agents. The different magnitude of leukopenia and leukocytosis in our research might have been associated with the kinds of agents used. Thus, RCTs involving different immunosuppressive agents without corticosteroid cotreatment should be designed to clarify this issue. The RCTs were pooled as a result of significant heterogeneity in the analysis of the risk of changes in platelet counts during immunosuppressive therapies. The results suggested that there were no definite associations between elevated platelet counts and immunosuppressive therapies. Our previous research showed a significant elevation of platelet counts in patients with CD. 50 Platelets might play a role as a mediator between the innate and adaptive immune responses. Large amounts of proinflammatory substances are excreted by platelets when they are activated at sites of inflammation.51,52 The increases in the platelet counts in the RCTs might have been associated with the hypercoagulability and inflammation status in patients with IBD.
Notably, our meta-analysis also revealed that immunosuppressive therapy was significantly associated with serum creatinine and serum aminotransferase elevations. The expression level of serum creatinine in patients with IBD was upregulated by almost 10-fold with administration of immunosuppressive therapy. Such an increase was also observed in serum aminotransferase, with no significant heterogeneity. The risk of serum aminotransferase augmentation differed between MTX therapy (RR, 3.20; 95% CI, 1.19–8.60) and AZA/6-MP therapy (RR, 3.00; 95% CI, 0.13–70.30). These findings provide strong evidence that the administration of immunosuppressive drugs is a risk factor for alterations in liver- and renal-associated laboratory parameters in patients with IBD.
The immunosuppressive drugs involved in our studies included AZA/6-MP, MTX, tacrolimus, and cyclosporine. Only two RCTs reported patients taking tacrolimus (n = 46) and cyclosporine (n = 182); this number of studies was too few to obtain meaningful estimates of risk. 6-MP and its prodrug AZA are thiopurine analogs that competitively interfere with nucleic acid metabolism, thus reducing cell proliferation and having an immune-modulating effect.53,54 Thiopurine analogs may be involved in the inhibition of T-lymphocyte function. A decline in the activation of natural killer cells and cytotoxic T cells can be seen in patients with IBD after the first or second trimester of AZA therapy.39,55 Tacrolimus has been shown to interfere with the production of interleukin 2 by T-helper cells. 37 The different mechanisms of action of these immunosuppressants may contribute to their different effects on blood biochemistry parameters in patients with IBD.
The application of immunosuppressive drugs should be weighed against the potential adverse events, particularly the effects on blood chemistries. Bone marrow suppression is defined as a hemoglobin concentration of <7 g/dL, a WBC count of <3 × 109/L, or a platelet count of <100 × 109/L. Thus, the blood count might be a crucial indicator of severe complications (e.g., bone marrow suppression) accompanying immunosuppressive therapies for IBD. 31 Patients with lower lymphocyte counts have a greater risk of infections, suggesting that subtle myelosuppression mediated by active metabolites of AZA/6-MP is linked to the occurrence of opportunistic infections. The most frequent infections are caused by cytomegalovirus and varicella zoster virus. Immunosuppressive drugs, especially AZA/6-MP, can reportedly increase the risk of opportunistic infections about 2- to 3-fold; when combined with corticosteroids, the risk increases to about 15-fold.20,21
Serum creatinine and serum aminotransferase are two strong indicators of renal and liver function, respectively. Although symptoms and pathological lesions cannot be observed in the early stages of elevation of these two parameters, their elevation reflects a high risk of renal and liver toxicity and may act as a predictor of severe outcomes. Increases in serum creatinine in excess of 30% above baseline values, which are associated with an increasing risk of interstitial nephritis and nephrotic syndrome, could indicate the need to reduce or discontinue treatment with immunosuppressive agents.37,38 Few studies have reported the influence of AZA and 6-MP use on serum creatinine changes in patients with IBD, and in our clinical experience, AZA and 6-MP induce very little nephrotoxicity. In the present study, we found an increased risk of serum creatinine elevation when calcineurin inhibitors, including cyclosporine and tacrolimus, were used in patients with IBD. Two other studies also showed serum creatinine elevations in some patients with IBD who were receiving cyclosporine and tacrolimus therapy,56,57 but the extent of these increases was slight and the duration was usually temporary; the creatinine level can be restored by dose adjustment. MTX is also very safe in terms of nephrotoxicity in IBD therapy; only one small-sample study showed an increase in the serum creatinine concentration after addition of low-dose cyclosporine to MTX therapy. 58 Moreover, very few studies have revealed the associations between immunosuppressive agents and serum aminotransferase. When data from three RCTs were pooled together, our study showed a risk of serum aminotransferase elevation during immunosuppressive agent use in patients with IBD; however, MTX rather than thiopurine analogs was more likely to induce an increase in serum aminotransferase. In a recent study focusing on AZA-induced hepatotoxicity among 293 patients receiving AZA, only 8 patients (about 2.7%) were diagnosed with AZA-induced hepatotoxicity, and none developed liver failure or required liver transplantation. 59 AZA and its derivate 6-MP can reportedly cause a spectrum of liver injuries ranging from asymptomatic elevated liver enzymes to cholestasis and nodular regenerative hyperplasia in the clinical setting. 60 A recent clinical observation demonstrated that liver steatosis was a risk factor for hepatotoxicity in patients taking immunosuppressants for IBD. These patients were found to have prevalent elevations in liver enzymes. 61 In some patients, the hepatotoxicity was dose-independent.
To minimize the risk of hepatotoxicity and opportunistic infection based on abnormal laboratory parameters, several RCTs in the present study discontinued or reduced the dose of these agents.34,37,38 Adverse events led to withdrawal of the drug in up to 30% of patients. 44 IBD practice guidelines recommend monitoring for myelosuppression after initiation of immunomodulator medications. 62 Importantly, close monitoring of laboratory parameters will provide early, convenient, and economical guidelines for dose adjustments during immunosuppressive therapy, helping to prevent treatment-related impairment and complications in patients with IBD.
Our study has several limitations. We examined a limited number of laboratory parameters. C-reactive protein, creatinine clearance, uric acid, and bilirubin were not examined because of the insufficient numbers of RCTs that reported these values. Each type of immunosuppressive agent may have different impacts on certain blood biochemical parameters or subtypes of IBD. We failed to finish every subgroup analysis either because of insufficient numbers of studies about tacrolimus and cyclosporine or insufficient numbers of studies about UC.
In addition, the small RCTs and early studies were subject to publication bias. Dosages were administered differently, with AZA given at either at 2.0 or 2.5 mg/kg body weight per day.39,43 Moreover, the duration of immunosuppressive therapies varied from 2 to 18 months. 43 Finally, many of the studies failed to perform weekly or monthly follow-ups involving laboratory investigations during immunosuppressive therapies. Whether these parameters were transiently abnormal or would continue to deteriorate remains unknown. However, almost all of the trials included in this meta-analysis were randomized, double-blind, placebo-controlled, and prospective clinical trials, and most exhibited no heterogeneity. Thus, our study is more informative, extensive, and persuasive than any single RCT included in the analysis.
Taken together, the findings of this study indicate that immunosuppressive therapies might have an impact on variations in blood biochemical parameters in patients with IBD. However, although the conclusion regarding leukopenia was reliable in this study, some confounding factors might reduce the reliability of the conclusions about leukocytosis, creatinine elevation, and aminotransferase elevation. These factors include the small number of patients in the analysis, indeterminacy of concomitant drug use, and the different characteristics of the immunosuppressants. Close monitoring of laboratory parameters is recommended to adjust the dose of or discontinue immunosuppressive drugs for IBD therapy. Further well-designed prospective studies to confirm the causal relationship between immunosuppressive agents and variations in blood biochemical parameters are warranted.
Footnotes
Acknowledgements
We thank Ping Zhang for her statistical expertise. We also appreciate the help of Kathy Kyler, University of Oklahoma Health Sciences Center, for the language editing of this manuscript.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This work was supported by the National Natural Science Foundation of China (grant Nos. 81600437, 81470823) and the Natural Science Foundation of Hubei Province (grant No. 2013CFB304).
