Abstract
A 52-year-old man was admitted to our hospital because of abdominal pain, nausea, and vomiting. On arrival, his body temperature was <35°C. Although his other vital signs and electrocardiographic findings were normal, his white blood cell count and C-reactive protein concentration were elevated. He was diagnosed with severe infectious disease and treated with intravenous antibiotics and rewarming therapy. Two hours later, his body temperature had increased to 38.4°C, but his abdominal pain persisted. A repeat electrocardiographic examination showed an elevated ST-segment in leads II, III, and aVF. He was then diagnosed with ST-elevation myocardial infarction. Coronary angiography showed occlusion of the right coronary artery, and he underwent implantation of two stents. His symptoms were relieved soon thereafter, and his body temperature returned to normal without antibiotics.
Keywords
Introduction
Acute myocardial infarction (AMI) is a common disease with high mortality. In most cases, AMI is easily diagnosed based on an elevated troponin level, abnormal electrocardiography findings, and typical symptoms such as exertional chest pain. However, the diagnosis may be more challenging if the symptoms are atypical or obscured by other clinical conditions. 1 We herein introduce a case in which the patient initially presented with hypothermia but was finally diagnosed with AMI.
Case report
A 52-year-old Chinese man presented to our hospital with an approximately 30-min history of mid-upper abdominal pain, nausea, and vomiting that had begun several minutes after supper (steamed fish and rice) in June. He had a history of pancreatitis 10 years previously and had been treated for hypertension for 2 years with valsartan; his blood pressure was well controlled. He reported no other vascular risk factors or family history. On arrival, his ear temperature was low (left, 34.9°C; right, 34.8°C) and he had mild upper abdominal tenderness. His blood pressure was 115/79 mmHg, and his heart rate was 79 bpm. An electrocardiographic examination performed upon arrival showed sinus rhythm with an Osborn wave on leads II, III, and aVF without obvious ST–T changes (Figure 1). Laboratory examination showed a white blood cell count of 13.9 × 109/L with 82% neutrophils, C-reactive protein concentration of 26.8 mg/L, and serum potassium concentration of 3.4 mmol/L; his serum amylase, creatine kinase MB isoenzyme, and high-sensitivity troponin-T concentrations and blood sugar level were all normal. He was suspected to have severe infection and underwent treatment with intravenous fluid and antibiotics in a warm room with a blanket. Half an hour later, his ear temperature had increased to 36.0°C with relief of his symptoms. However, 2 hours after arrival, he developed chills and shivering with an increased body temperature of 38.4°C, and his abdominal pain and nausea had become aggravated again. A repeat electrocardiographic examination showed an elevated ST-segment in leads II, III, and aVF and ST depression in leads I, aVL, V1, and V2 (Figure 2). Emergency coronary angiography was performed after another blood sample was taken and showed occlusion of the right coronary artery (Figure 3). After thrombus inspiration, two stents were implanted and the patient’s abdominal pain was relieved soon thereafter. During the process of coronary angiography, the blood test results were obtained and showed that the troponin-T concentration was 1.24 ng/mL, further supporting the diagnosis of myocardial infarction. After the angioplasty, we ceased the administration of antibiotics. The troponin-T concentration peaked at 6.29 ng/mL on the second day of hospitalization. Two days later, the patient’s body temperature returned to normal. An abdominal computed tomography scan was also performed during hospitalization and showed no obvious abnormality. The results of a blood culture (sampled from the vessels of both arms) and urine culture during hospitalization were negative.

First electrocardiogram.
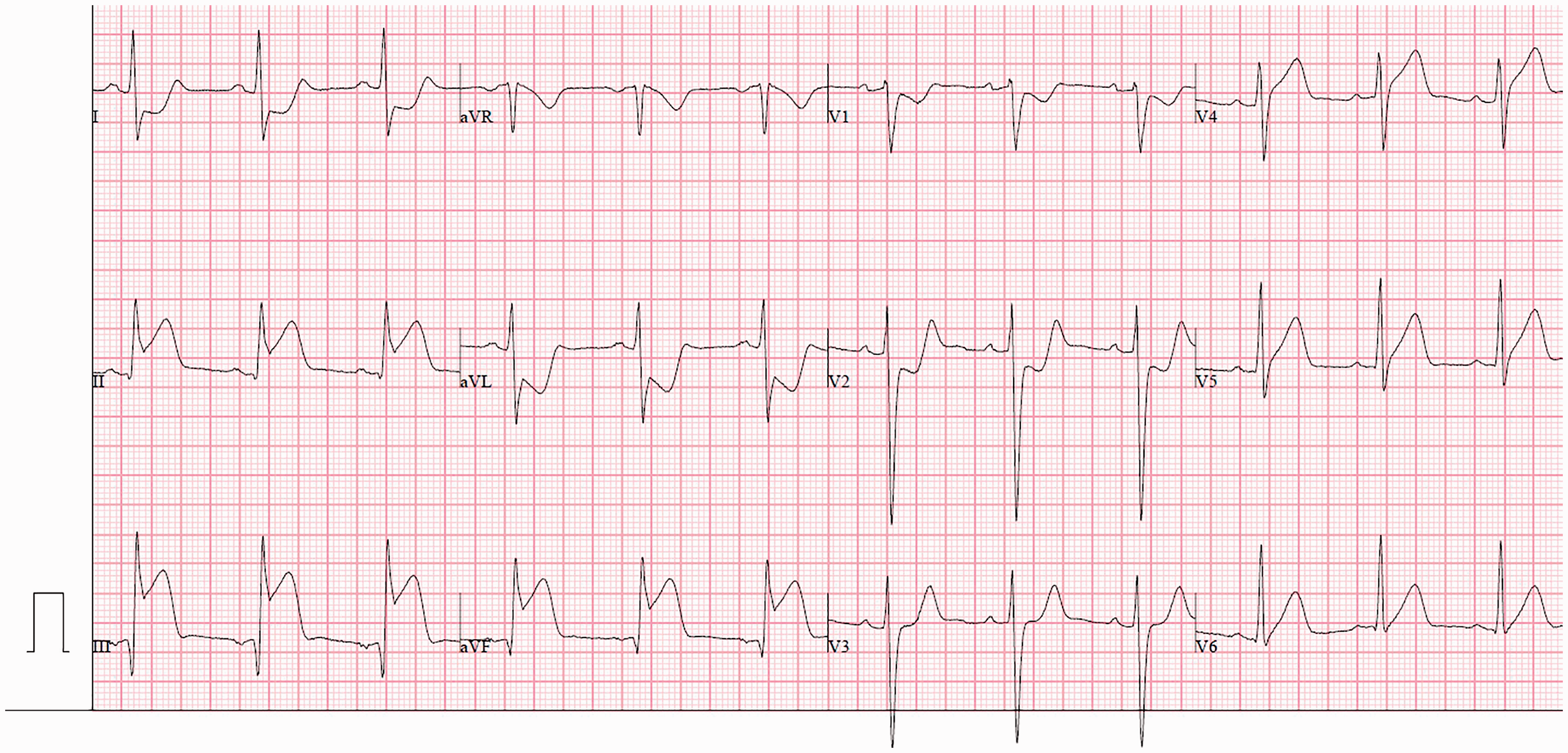
Second electrocardiogram.

Image of the right coronary artery. (a) The occluded right coronary artery. (b) The right coronary artery after wire-crossing and thrombus inspiration. (c) The stent-implanted artery.
Discussion
This was an atypical case of AMI. The patient presented with hypothermia, a rapid temperature change, and abdominal symptoms; the latter symptoms are sometimes atypical but not rare symptoms of AMI. 1 Based on the combination of hypothermia, symptom onset after dinner, and negative electrocardiogram findings, we first considered a gastrointestinal infectious disease or even sepsis. However, another electrocardiographic examination was performed because the patient’s symptoms were not relieved after the administration of antibiotics and fluid, and this examination prevented further misdiagnosis. The troponin-T concentration was first measured 2.5 hours after the onset of abdominal pain and was 1.24 ng/ml at that time. The electrocardiogram at that time also showed obvious ST-segment elevation in multiple leads. Thus, we considered that the onset of AMI might have been around 2 hours before presentation. The AMI was most likely triggered by an infection that first manifested as hypothermia. Infectious diseases, especially influenza, have been reported to be a trigger for AMI, possibly because of the effect of influenza on the inflammatory and coagulation pathways. 2 In the present case, the location of the infection might have been the gastrointestinal system based on the abdominal pain and symptom onset after a meal. Alternatively, the abdominal pain might have simply been a symptom of the AMI considering that it was relieved immediately after the percutaneous coronary intervention and the examinations performed to locate the infection site were all inconclusive. Another possible explanation is that the patient developed AMI, not infection, and that the hypothermia, fever, and abdominal pain were all manifestations of the AMI. Actually, fever after AMI is common, especially in patients who do not undergo reperfusion therapy. 3 Hypothermia is usually caused by exposure to cold, shock, or sepsis. Therapeutic hypothermia has been used as a cardioprotective approach in patients with AMI by reducing the infarct size and microvascular resistance. 4 Severe hypothermia may cause ST elevation and lead to misdiagnosis. 5 The hypothermia in the present case might have been a manifestation of hypoperfusion of the peripheral circulation or a pre-shock state caused by the right ventricular and inferior wall AMI, similar to the manifestation of hypovolemic shock. 6 After fluid administration, the hypoperfusion was corrected but the infarction progressed and induced hyperthermia. However, this explanation is based only on deduction without strong evidence. More studies are required to determine whether hypothermia can be caused by AMI and, if so, identify the underlying mechanism.
In conclusion, this was an atypical case of AMI that might have been secondary to the presence of infection. This case demonstrates the diversity of the manifestations of AMI. It is important for emergency physicians to consider AMI as a differential diagnosis of hypothermia in patients with epigastric systems.
Ethics and consent
This was an individual case report with no involvement in clinical or animal research. The requirement for ethical permission was waived according to the statements regarding the application of ethical permission by the Ethical Committee of the Fourth Affiliated Hospital of Zhejiang University School of Medicine. Written consent was obtained from the patient for publication of his medical data, including images.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research was supported by grants from the National Natural Science Foundation of China (No. 81600393) and the Zilong Mountain Young Talent Program of ZJU4H.
