Abstract
A 54-year-old woman with hairy cell leukemia developed severe polymorphic erythema and blisters on the trunk and limbs after injection of interferon (IFN) α-2b. Skin biopsy revealed lymphocytic exocytosis and perivascular lymphocytic infiltrate in the dermis, and the lesions improved after methylprednisolone pulse therapy. Although injection-site reactions have been observed after injection of IFNα-2b, this is the first report of a widespread cutaneous reaction to IFNα-2b.
Introduction
Cladribine and pentostatin are the first-line treatments for classic hairy cell leukemia (HCL). Interferon (IFN)-α is no longer a recommended therapy because of its low complete remission rate.1,2 If the infection cannot be controlled and anti-leukemia therapy is needed, the clinician must decide whether to use either a purine analog or IFN-α as primary therapy. 1 IFN-α has been recommended for the treatment of HCL in pregnant women, who show good tolerance, an uncomplicated pregnancy and delivery, and normal child development. 2 However, IFN treatment is selected by many patients in developing countries such as India and China because of their family’s economic condition. Specifically, IFN-α can alleviate the symptoms of HCL and improve the quality of life of patients who cannot afford purine analogs. We herein report the first known case of a patient who developed severe polymorphic erythema and blisters after application of IFNα-2b to treat HCL. This case is being reported to help doctors treat patients with HCL in developing countries such as India and China and to raise awareness of the risk of widespread cutaneous reactions caused by IFN-α.
Case report
A 54-year-old woman diagnosed with HCL was treated with intramuscular injection of IFNα-2b (iH, QOD, 15000 U/time). The patient denied any history of rheumatism or dermatosis. She developed a rash and erythema without pruritus, fever, panic, chest tightness, or other symptoms after the first injection of IFN; a rash on the neck after the second injection; and gradually appearing diffuse erythema, rashes, and blisters after the third injection. The blisters were distributed in the form of strips that were mainly concentrated on the forearm and were accompanied by itching and pain (Figure 1). After consultation with a doctor, the patient was instructed to smear her whole body with calamine lotion (Figure 2), but a poor effect was attained. She was thereafter referred to the hematology department in our hospital because of widespread erythema, rashes, and blisters. Histopathological examination of a skin biopsy indicated lymphocytic exocytosis and a perivascular lymphocytic infiltrate in the upper dermis (Figure 3). Laboratory examination results showed that the C-reactive protein level was high at 44.60 mg/L, while all rheumatic factors were normal, including anti-streptolysin O, rheumatoid factor, anti-deoxyribonuclease, and serum amyloid A. Moreover, no abnormality was detected in the autoantibodies SSA, SSB, and anti-nuclear antibody. Methylprednisolone (120 mg) was given on days 1 and 2, and new blisters still appeared on day 3. After a dermatology consultation, the patient was diagnosed with a severe polymorphic erythema drug eruption; thus, methylprednisolone pulse therapy (500 mg) was given on days 3, 4, and 5, and no new blisters appeared thereafter. On day 6, the patient’s hormone levels were reduced by 50% daily until the withdrawal of hormone therapy. On day 10, the blisters, rashes, and erythema had receded and the patient was discharged from the hospital. The patient provided written informed consent. This case report was approved by the ethics committee of the Affiliated Hospital of Qinghai University.
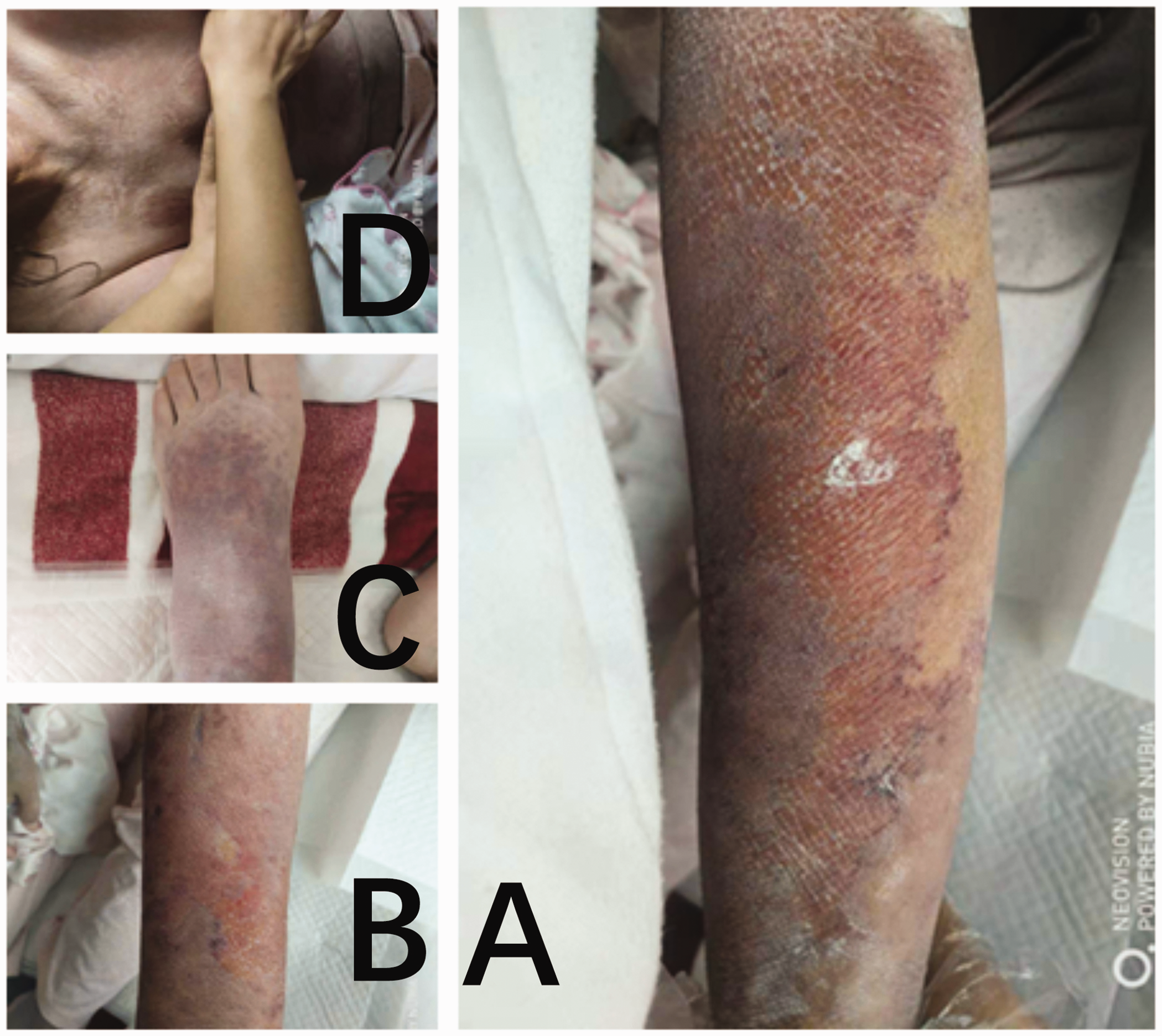
Photographs of patient’s limbs and chest. The patient developed a rash on the neck after the second injection. (a) Left forearms. (b) Right forearms. (c) Left foot. (d) Chest.

Photographs of treatment with calamine lotion. The patient was instructed to smear the whole body with calamine lotion. (a) Legs. (b) Chest. (c) Abdomen. (d) Left forearms.

Skin biopsy. Lymphocytic exocytosis and perivascular lymphocytic infiltration were present in the upper dermis.
Discussion
HCL is a rare inert B cell leukemia that accounts for about 2% of all cases of lymphocytic leukemia. The long-term efficacy of this drug shows that persistent disease control can be achieved. 3 IFNα has historically been the first-line therapy and shows efficacy in both induction and maintenance therapy for HCL. The reported generalized reactions induced by the use of IFN include oral erosive lichen planus, 4 alopecia universalis, 5 sarcoidosis, 6 Meyerson nevi, 7 and cutaneous polyarteritis nodosa. 8 The reported localized reactions include hyperpigmentation of the tongue 9 and facial erythema. 10 The drug manufacturer indicates that the incidence of common rashes is 2%; however, no cases of severe polymorphic erythema resulting from the application of IFN to treat HCL have been previously reported, although some reports have described a severe polymorphic erythematous drug rash induced by IFN in the treatment of hepatitis type C 11 and multiple sclerosis. 12 In the present case, the patient finally developed a severe erythematoid rash after the application of IFN, and the rash obviously improved after withdrawal of IFN and administration of symptomatic treatment. Therefore, we consider that IFN resulted in the drug-induced rash. IFN can mediate the immune response through stimulation of lymphocytes, which might account for the pathogenetic mechanism of the severe erythematous rash. The increased number of lymphocytes seen in the skin biopsies also supports this. However, the possibility of a drug rash caused by polyethylene glycol excipients cannot be excluded.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
