Abstract
Objective
This study was performed to determine the prevalence of triangular fibrocartilage complex (TFCC) injuries as shown by 3.0T magnetic resonance imaging (MRI) in patients with distal radius fractures.
Methods
In total, 57 patients with distal radius fractures underwent 3.0T MRI examinations to observe the incidence of TFCC injuries after manual reduction and cast fixation. The fracture type was categorized by the AO classification, and the TFCC injury pattern was evaluated using the Palmer classification. The correlation between the location of the TFCC injury and the distal radius fracture pattern, distal radioulnar joint instability, or ulnar styloid fracture was analyzed.
Results
Fifty-five TFCC injuries were diagnosed. There was no significant relationship between the TFCC injury pattern and the type of distal radius fracture, distal radioulnar joint instability, or ulnar styloid fracture.
Conclusions
This study revealed a high prevalence of TFCC injuries in patients with distal radius fractures. The 3.0T MRI examination helps to assess TFCC injuries in patients with distal radius fractures.
Clinical Trial Registration
ChiCTR1800017101.
Keywords
Introduction
Distal radius fractures commonly occur in adults and account for 18% of all fractures in the human skeleton. 1 Regardless of conservative or surgical treatment, adverse outcomes occur in 6% to 80% of distal radius fractures. 2 Previous studies3–5 have demonstrated that triangular fibrocartilage complex (TFCC) injury, which is associated with distal radius fractures, is a common cause of these adverse outcomes. The TFCC is an important soft tissue structure on the ulnar side of the wrist that plays a critical role in the stability of the distal radioulnar joint. 6 TFCC injuries can result in distal radioulnar joint instability, ulnar-sided pain, or decreased grip strength. According to recent studies,7,8 symptomatic traumatic TFCC injuries often require surgical intervention. Therefore, early diagnosis of TFCC injuries may help clinicians to develop a proper treatment strategy.
The diagnosis of TFCC injuries continues to be challenging because the TFCC is a small and complex structure. 9 Through direct visualization and probing of the TFCC, wrist arthroscopy is generally considered the best way to diagnose TFCC tears. However, arthroscopy is impossible to use in all patients because it is an invasive procedure. Furthermore, Park et al. 10 reported that wrist arthroscopy had poor interobserver reliability in identifying TFCC injuries. Recent advances in 3T high-resolution magnetic resonance imaging (MRI) have enabled precise detection and evaluation of morphological changes of the TFCC. 11 Several studies have documented excellent intraobserver and interobserver reliability of the diagnosis using 3.0T high-resolution MRI.12,13 On the basis of these findings, we used 3.0T MRI to identify TFCC injuries in patients with distal radius fractures.
To our knowledge, few studies have been performed to investigate the prevalence of TFCC injuries in patients with distal radius fractures. The purpose of this study was to determine the incidence and features of traumatic TFCC injuries in patients with distal radius fractures by 3.0T MRI examinations. We also evaluated the correlation between associated TFCC injury locations and the distal radius fracture pattern.
Materials and methods
This study was performed in our hospital from January 2017 to July 2018. Institutional board review approval was obtained before beginning the study, and informed consent was obtained from each patient. Consecutive patients with a distal fracture of the radius were enrolled in this prospective study. The exclusion criteria were an age of >70 years, open fractures, skeletal immaturity, relevant medical comorbidities affecting the wrist, and MRI examination contraindications. Each patient underwent a standard wrist X-ray examination in the emergency department with subsequent closed reduction and plaster cast fixation.
All patients underwent an MRI examination of the involved wrist using a 3.0T MRI scanner (Siemens, Berlin, Germany). To maintain the stability after closed reduction, the forearm plaster was not removed during the MRI examinations. The imaging protocol 9 consisted of both T1-weighted images [repetition time/echo time (TR/TE), 480/11; image matrix, 256 × 512] and T2-weighted images (4000/81, 256 × 512), coronal fat-suppressed (FS) proton density (PD) images (2000/42, 256 × 512), and coronal isotropic three-dimensional FS PD images (1300/39, 256 × 512). The interval from injury to the MRI examination ranged from 0 to 7 days (average, 4.5 days). The MRI examinations were free of cost to all patients.
All imaging findings were evaluated by two attending orthopedic surgeons in a blind manner using a picture archiving and communication system. After their discussion, the final diagnosis was reached. The surgeons re-examined all images after a 2-month interval to test intraobserver and interobserver reliability. All distal radius fractures, including associated ulnar styloid fractures and/or distal radioulnar joint (DRUJ) instability, were categorized according to the AO classification system. Acute DRUJ instability was diagnosed when the following criteria were met: dislocation of the DRUJ accompanied the distal radius fracture, a significant increase in the DRUJ gap distance was seen on the posteroanterior radiograph, 14 DRUJ instability was diagnosed during open surgery, and >5-mm proximal displacement of the distal part of the radius was present. 15 Acute DRUJ instability was assessed using X-ray or computed tomography according to previous reports.16,17 A manual stress test was also performed for diagnosis during open surgery. We defined a TFCC injury as the presence of increased signal intensity that extended through the entire thickness of the TFCC or a high signal of the local ligament structure. 12 The MRI features of traumatic TFCC injuries were analyzed using the Palmer classification. 18 A central lesion (Palmer 1A) was defined as a tear or perforation of the horizontal portion of the TFCC. Palmer 1B was defined as ulnar avulsion with or without an ulnar styloid fracture. Palmer 1C was defined as distal avulsion, and Palmer 1D was defined as radial avulsion with or without sigmoid notch fractures. Figure 1 shows representative traumatic TFCC images.
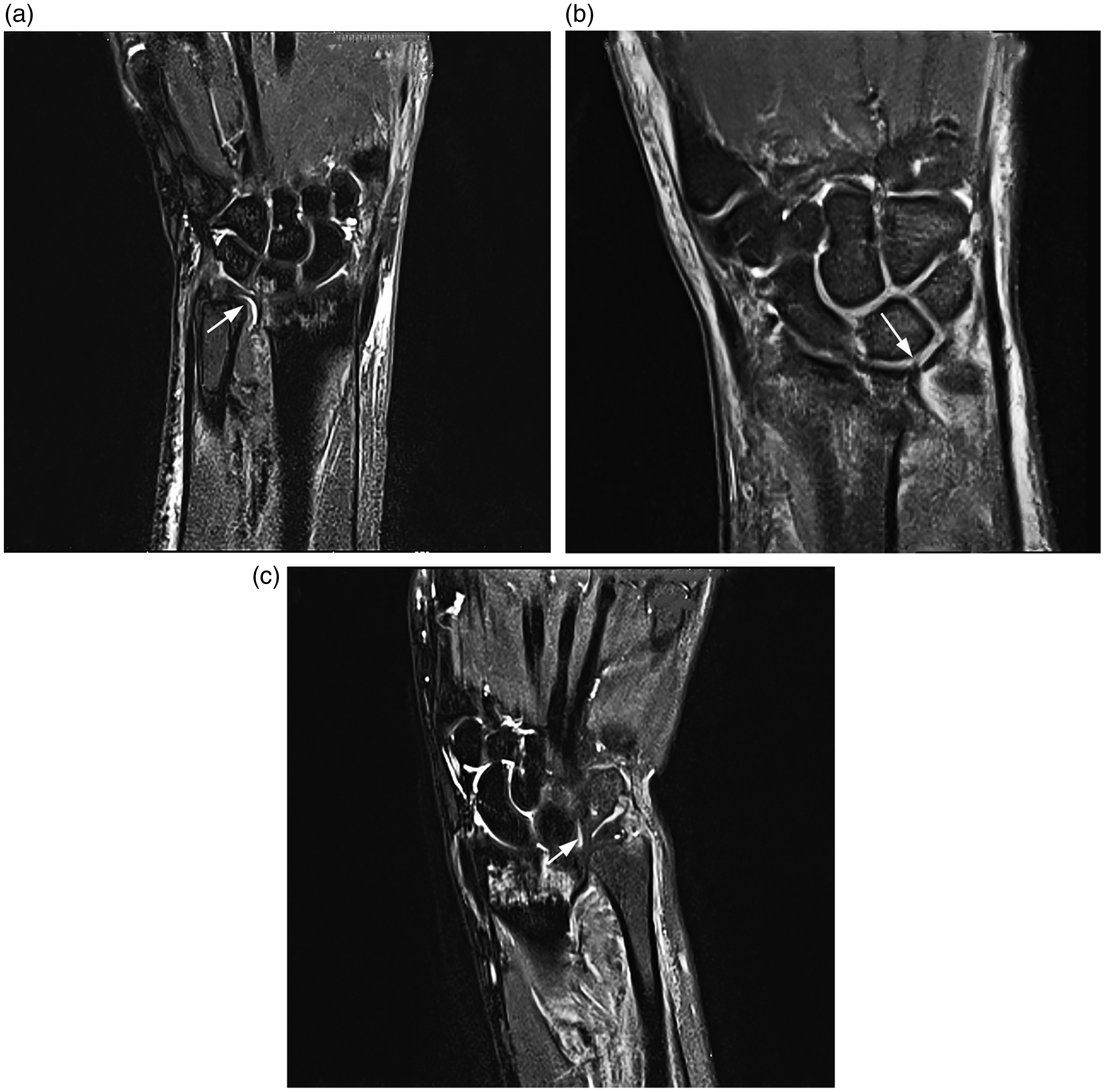
(a) Coronal proton density (PD) fat-suppressed (FS) image showing a normal triangular fibrocartilage complex (TFCC) (white arrow). (b) Coronal PD image showing a full-thickness tear (type 1A) of the central portion of the TFCC (white arrow). (c) Coronal PD FS image showing an injury (type 1B), but no tear, of the ulnar attachment of the TFCC. The ulnotriquetral ligament and the ulnolunate ligament are normal (white arrow).
Statistical analysis
The Kruskal–Wallis test was used to evaluate the correlation between associated lesions of the TFCC and the distal radius fracture pattern. The Mann–Whitney exact test was performed to evaluate the relationships between associated lesions of the TFCC and DRUJ instability or ulnar styloid fractures. A P-value of <0.05 was considered significant. Cohen’s kappa was used to evaluate interobserver and intraobserver reliability of the MRI findings of TFCC injuries. The following ratings were used for kappa: poor (<0.40), moderate (0.40–0.59), good (0.60–0.80), and excellent (>0.80). 11 Statistical analysis of the data was performed using IBM SPSS Statistics for Windows, Version 24.0 (IBM Corp., Armonk, NY, USA).
Results
Sixty-two consecutive patients with a distal radius fracture were initially evaluated. After application of the exclusion criteria, 57 patients were enrolled in the study (35 women, 22 men; mean age, 41.4 years; range, 17 to 69 years). The AO classification data showed A2 fractures in 8 patients, A3 fractures in 13 patients, B1 fractures in 3 patients, a B3 fracture in 1 patient, C1 fractures in 11 patients, C2 fractures in 15 patients, and C3 fractures in 6 patients. Eleven of the 57 patients had DRUJ instability on X-ray and physical examinations. Ulnar styloid fractures were observed in 34 patients. TFCC injury was present in 55 (96.5%) patients. The frequencies of fracture types and TFCC injuries are summarized in Table 1. There was no significant difference between associated lesions of the TFCC and the distal radial fracture patterns. We also found no correlation between the TFCC injury pattern and ulnar styloid fractures or DRUJ instability (Table 2). Both interobserver and intraobserver agreement for diagnosing TFCC tears by MRI was considered good (inter k = 0.662, intra k = 0.729).
Frequencies of triangular fibrocartilage complex injury according to fracture type.

Frequencies of triangular fibrocartilage complex injury according to ulnar styloid fracture or DRUJ instability.

DRUJ, distal radioulnar joint.
Discussion
The TFCC is a small ligamentous complex on the ulnar side of the wrist with an average thickness of only 2 to 5 mm. 18 Evaluation of TFCC injuries requires special MRI scan sequences and extensive experience in reading MRI. To improve the accuracy of the diagnosis, the wrist must be continuously scanned in a 1-mm-layer thickness in coronal isotropic three-dimensional FS PD images. We once considered that hematomas and edema caused by distal radius fractures would affect the evaluation of TFCC injuries. In contrast, the present study showed that 3.0T MRI clearly reveals the small ligamentous structure of the TFCC. Because of the lack of equipment in our hospital, we were unable to perform wrist arthroscopy. Therefore, we referred to previous reports on the MRI criteria for diagnosing TFCC injury in this study. We were also unable to determine the sensitivity and specificity of MRI; we only evaluated the observers’ agreement of the MRI readings. Our results showed a high level of diagnostic agreement of MRI in TFCC injury (inter k = 0.662, intra k = 0.729), consistent with several recently published studies.11–13
Lindau et al. 19 found that the most frequent ligament tear was the TFCC (78%) in patients with distal radius fractures. In their study of 118 patients with distal radius fractures, Richards et al. 20 reported that 46 patients had TFCC tears. Ogawa et al. 21 showed that TFCC injury complicated by distal radius fractures was present in 59% of cases, irrespective of the fracture type. Kasapinova and Kamiloski 8 reported that exploratory arthroscopy revealed TFCC lesions in 45 patients (53%) with surgically treated distal radius fractures. The incidence of TFCC was variable and dependent upon on the definition of TFCC tears. In the present study, the prevalence of TFCC injuries in patients with distal radius fractures was as high as 96.5%, which is higher than in previous reports. We believe that the high incidence of TFCC injuries is mainly due to the anatomical and biomechanical characteristics of the TFCC. 18 However, in our study, the presence of increased signal intensity interpreted as TFCC injuries may have resulted in overestimation of the incidence.
Although the incidence of TFCC injury associated with distal radius fractures is high, only 11% to 19% of patients sustain symptomatic and clinically relevant problems. 6 Recommended treatments for TFCC tears are variable and depend on the features of the tear. The current consensus is that Palmer type 1A and 1D injuries are treated with debridement, and type 1B lesions require surgical repair. To our knowledge, few studies have focused on the location of TFCC lesions. 7 Blazar et al. 22 reported that the number of central, radial, and peripheral lesions in 51 wrists without fracture was 19, 4, and 12, respectively. Kasapinova and Kamiloski 23 evaluated 85 patients with distal radius fractures and found a type 1A lesion in 6 patients, a type 1B lesion in 9 patients, a type 1C lesion in 4 patients, and a type 1D lesion in 26 patients. Our results differ from these. In our study, 11 patients had Palmer type 1A TFCC injuries, 53 had type 1B (92.3%), 16 had type 1C (28.1%), and 10 had type 1D (17.5%). Our study also showed no correlation between associated lesions of the TFCC and specific fracture types, similar to previous reports. Perhaps the location of the TFCC tear is related to the injury mechanism. This remains unclear and requires further research.
The relationship between ulnar styloid fractures and TFCC injuries is controversial. As opposed to Lindau et al., 19 Richards et al. 20 found no relationship between ulnar styloid fractures and TFCC injuries. Our research supports the lack of a significant difference. Several studies have demonstrated that ulnar styloid fractures have no adverse effect on the functional recovery of distal radius fractures.24,25 These conclusions are not contradictory to our findings. Ulnar styloid fractures suggest a high risk of TFCC injury (100%), but not necessarily complete ligament rupture of the TFCC.
DRUJ stability is maintained by bony congruity, the TFCC, the interosseous membrane, the extensor retinaculum, and muscle–tendon units. 6 The TFCC is considered a major contributor to intrinsic stabilization. DRUJ instability accompanied by distal radius fractures suggests the presence of TFCC injury, a sigmoid notch fracture, or an ulnar styloid fracture. 26 However, Fujitani et al. 27 concluded that an increase in the DRUJ distance was only one risk factor for DRUJ instability in patients with distal radius fractures. Furthermore, according to Kasapinova and Kamiloski, 23 there was no positive correlation with any measured parameter and the presence or absence of TFCC tears. Likewise, our study showed that the presence of DRUJ instability in distal radius fractures was not correlated with the pattern of TFCC injuries.
Our research has several limitations. First, we had no criteria with which to determine the sensitivity or specificity of the MRI findings. In addition, we did not distinguish between partial and complete tears, which may have resulted in overestimation of the TFCC injuries. Another limitation of this study is the relatively small number of patients.
In conclusion, the present study indicates a high prevalence of TFCC injuries in patients with distal radius fractures, and the presence of ulnar styloid fractures suggests type 1B injuries. However, there was no statistical relationship between the location of the TFCC injury and the type of distal radius fracture (AO classification), DRUJ instability, or ulnar styloid fractures.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This study was supported by Jinshan Health Bureau, Shanghai, China (JSKJ-KTMS-2016-10).
