Abstract
Objective
This study was performed to summarize our experience in applying choledochofiberscopy to the treatment of anastomotic stricture after cholangiojejunostomy.
Methods
We retrospectively analyzed patients who underwent choledochofiberscopy for the treatment of anastomotic stricture via balloon dilatation and were followed up for at least 6 to 12 months.
Results
A 6- to 12-month follow-up was performed in the above-mentioned 30 patients after trans-choledochofiberscopic balloon dilation and stone removal. Among these patients, 19 did not develop recurrent fever or abdominal pain, and the serum levels of direct bilirubin, aspartate aminotransferase, γ-glutamyl transpeptidase, and alkaline phosphatase returned to normal or near normal, with a total success rate of 63%. Eleven patients developed restenosis and recurrence of intrahepatic stones, with a stenosis rate of 37%. Among these 11 patients, 6 underwent trans-choledochofiberscopic balloon dilatation for stone removal, and they recovered uneventfully; the remaining 5 patients were transferred for surgical reoperations for treatment of stenosis following repeated dilatation, with a failure rate of 17%.
Conclusion
Choledochofiberscopy for the treatment of anastomotic stricture after cholangiojejunostomy has the following advantages: minimal trauma, minimal pain, rapid effect, low risk, repeatable treatment procedures, and no serious complications. This is a safe and effective method of treatment.
Keywords
Introduction
Cholangiojejunostomy is an effective approach to resolve a variety of clinical benign and malignant biliary strictures, iatrogenic bile duct injuries, and congenital choledochal cysts. However, the development of bilioenteric anastomotic strictures is a common complication after cholangiojejunostomy because of the complexity and operative difficulty of this procedure and the poor prognosis associated with reoperation. These are challenges that hepatobiliary surgeons must face. If not treated promptly, patients often develop septic shock, liver and kidney failure, biliary cirrhosis, and other potentially life-threatening conditions. 1 In the present study, we evaluated patients with bilioenteric anastomotic stricture who underwent choledochofiberscopic therapy at our hospital with good results. Bilioenteric anastomotic stricture formation is especially problematic among patients in whom the anastomosis has been made at a high position because the necessity of reoperation in such patients can be very difficult to determine. Therefore, we performed the present study to share our experience regarding safe and effective treatment.
Data and methods
This study was conducted in accordance with the principles of the Declaration of Helsinki and with approval from the ethics committee of our hospital. Written informed consent was obtained from all participants.
General information
We retrospectively analyzed patients with bilioenteric anastomotic stricture who underwent choledochofiberscopic therapy in our hospital from October 2007 to July 2011. The patients’ conditions included multiple stones in the intrahepatic bile duct, a congenital cystic duct, iatrogenic bile duct injury, and benign stenosis. All patients presented with inflammatory stricture or anastomotic contracture after cholangiojejunostomy (Figure 1(a)) as diagnosed by color Doppler ultrasound examination, computed tomography, magnetic resonance cholangiopancreatography, and other tests.

Dilation of the bilioenteric anastomosis. (a) Bilioenteric anastomosis with absolute stenosis. (b) Placement of drainage tube or guide wire in intestinal tract via the anastomosis by percutaneous transhepatic cholangial drainage. (c) Balloon dilatation of bilioenteric anastomosis. (d) Image of bilioenteric anastomosis after balloon dilatation.
Treatment
Endoscopic channels were established for use of a fibercholedochoscope (CHF-P60; Olympus, Tokyo, Japan). For this purpose, patients without a retained subcutaneous intestinal loop underwent jejunostomy at a site 10 cm from the bilioenteric anastomosis. In contrast, patients with a retained subcutaneous intestinal loop only underwent incision of the retained intestinal loop for performance of jejunostomy under local anesthesia. 2 After the sinus tract was established by one of these two methods, a T tube was placed in the jejunal loop for drainage for 2 to 4 weeks. The choledochoscopic examination was then carried out.
The choledochoscopic examination and treatment were performed as follows. The choledochoscope was advanced into the jejunal loop through the sinus tract to locate the anastomosis. If the leakage was located in the intestinal input loop, the cecum of the jejunum was identified and the bilioenteric anastomosis was then located in the output loop. If the leakage was located in the jejunal output loop, the bilioenteric anastomosis was found retrogradely along the direction of the input loop. After identification of the anastomosis, the anastomotic stricture was evaluated and the dilation pressure and time were confirmed according to the degree of stenosis. After evaluation of the anastomotic stricture, a guide wire was placed via the anastomosis, and a biliary dilatation balloon catheter was advanced inside along the guide wire. The narrow anastomosis was dilated under the assistance of anesthesia with a balloon pressure of 10 to 15 atm, effective diameter of 0.8 cm, and dilation time of 10 to 20 minutes. Difficulty was encountered in finding the anastomosis in four patients; thus, a drainage tube was placed or a guide wire was advanced into the intestinal tract via the anastomosis by percutaneous transhepatic cholangial drainage (PTCD), and the balloon dilatation was then carried out (Figure 1(b)–(d)).
Statistical analysis
Statistical analysis was performed using SPSS v.13.0 software (SPSS Inc., Chicago, IL, USA). Welch’s t test was used when one-way analysis of variance was unequal; otherwise, Student’s t test was used. Bonferroni’s adjustment was used for multiple comparisons. A P value of <0.05 indicated statistical significance. All data are presented as mean ± standard error of the mean.
Results
Patients
Thirty patients with bilioenteric anastomotic stricture underwent choledochofiberscopic therapy in our institution from October 2007 to July 2011, and all 30 patients [18 (60%) male, 12 (40%) female] were retrospectively analyzed. Among the 30 patients, 12 (40.0%) had multiple stones in the intrahepatic bile duct, 7 (23.3%) had a congenital cystic duct, 8 (26.7%) had iatrogenic bile duct injury, and 3 (10.0%) had benign stenosis. The patients’ median age was 46 years (range, 25–70 years).
Improvement in symptoms after cholecystoscopic balloon dilatation
All 30 patients underwent cholecystoscopic balloon dilatation. On the third postoperative day, 4 patients had abdominal pain, 11 had jaundice, and 6 had a fever. On the fifth postoperative day, no patients had abdominal pain, four patients had jaundice, and three had a fever. On the seventh postoperative day, no patients had abdominal pain, one had jaundice, and one still had an intermittent fever. Under consideration of a postoperative infection, symptomatic treatment with anti-infective therapy was administered and resulted in gradual improvement (Figure 2).

The patients’ symptoms gradually disappeared after the balloon dilatation.
Improvement of liver function after cholecystoscopic balloon dilatation
On the third day after surgery, 11 patients had an elevated serum direct bilirubin (DBIL) level, 10 had an elevated aspartate aminotransferase (AST) level, and 9 had an elevated alkaline phosphatase (ALP) level. Until the fifth day postoperatively, three patients had an elevated serum DBIL level, two had an elevated AST level, and five had an elevated ALP level. All laboratory test parameters gradually returned to normal in all patients up to postoperative day 7 (Figure 3).
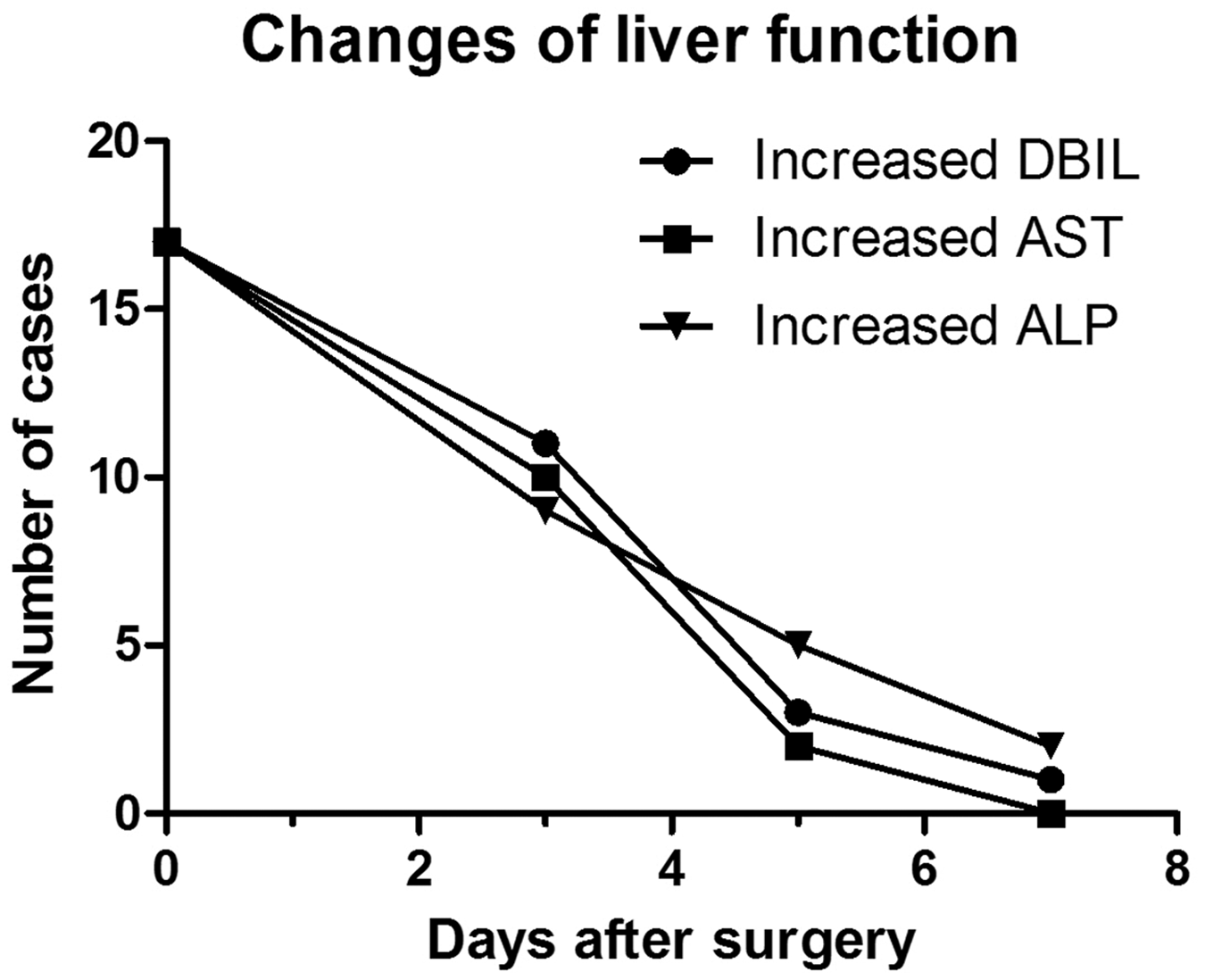
Cholecystoscopic balloon dilation resulted in gradual improvement of liver function. DBIL, direct bilirubin; AST, aspartate aminotransferase; ALP, alkaline phosphatase.
Short-term follow-up outcomes
All 30 patients were followed up for 6 to 12 months. The patients’ conditions were closely observed during this period. In 19 patients, the fever, jaundice, and abdominal pain did not recur, and the serum DBIL, AST, γ-glutamyl transpeptidase (GGT), and ALP levels returned to normal or near normal levels, with a total success rate of 63%. Eleven patients developed restricture and recurrence of intrahepatic stones, with a stricture rate of 37%. Among these 11 patients, 6 underwent cholangioscopic balloon dilatation for stone removal and recovered uneventfully, and 5 were transferred to the surgical department for reoperations to treat stenosis following repeated dilatation, with a failure rate of 17% (Figure 4).

Good short-term follow-up outcomes were obtained after cholecystoscopic balloon dilation.
Discussion
Cholangiojejunostomy is an effective means of treatment for a variety of clinical benign or malignant biliary strictures, choledochal iatrogenic bile duct injuries, and congenital common bile duct cysts. However, the development of bilioenteric anastomotic stricture is the main surgical complication associated with this procedure, with an incidence rate of approximately 21.6%; 3 one report indicated that this rate may be as high as 30.0%. 4 Diagnosis of bilioenteric anastomotic stricture mainly depends on the patient’s symptoms, serum biochemical test results, and abdominal magnetic resonance imaging findings. 5
Bilioenteric anastomotic stricture is a complex lesion that is prevalent in patients undergoing biliary tract surgery, and it is a challenge faced by surgeons in this field. Such strictures generally lead to failure of the operation and the need for reoperation.
Unlike the intestinal wall, the bile duct wall has neither muscle nor peristaltic motility; however, it has a layer of elastic fibers. When an obstruction is relieved, the passively dilated bile duct returns to its previous condition as the pressure drops, and the lumen therefore narrows. The extent of recovery is affected by the degree of biliary fibrosis, thickness, and stiffness; greater retraction will occur with non-inflammatory lesions. Kram et al. 6 noted that bile duct–jejunal anastomosis would be narrowed by 30% after 3 days; thus, stricture certainly occurs if the anastomosis is not large enough. If the incision is too small or the anastomosis is too tight, the anastomosis will be narrowed by scar tissue contraction. In addition, if the free proximal bile duct is long, blood flow at the stump is insufficient, which induces scar tissue contraction and anastomotic stricture. More scars and poor mucosal healing after the first operation increase the risk of postoperative stricture formation. Some scholars have considered that anastomotic stricture is caused by contraction of the inflammatory scar after the operation, oppression of the external cavity by the anastomotic or biliary anastomosis, bile leakage or development of an infection or abscess around the stoma, or biliary stenosis above the anastomosis that was not probed during the surgery. 7
Because of the complexity of anastomotic stricture, surgery is the main treatment. The basic goals of surgery are to re-establish the anastomosis and ensure smooth flow of bile. 8
However, because of the high difficulty of reoperation in some patients, surgeons are required to fully master the skills necessary for the procedure; additionally, the rate of anastomotic restricture is high. Especially for patients in whom the anastomosis has been made at a high position, whether reoperation is necessary can be very difficult to determine. With the development of endoscopic techniques and equipment, the use of endoscopic retrograde cholangiopancreatography (ERCP) or enteroscopy for treatment of anastomotic stricture has been reported.9–11 However, treatment with ERCP or enteroscopy necessitates creation of endoscopic channels with a complex distribution in the gastrointestinal tract and is associated with great operational difficulties, high cost, and low repeatability. Therefore, the establishment of gastrointestinal channels in advance to facilitate repeated treatments has also been reported. 12
Based on surgical balloon dilatation of bile duct stenosis, 13 the application of percutaneous choledochoscopy to treat postoperative anastomotic stricture has achieved satisfactory results. In the present study, the success rate was 80%, recurrence rate was 33%, and relapse rate was closely related to the degree of stricture. Furthermore, the patients could be treated after relapse. We believe that the quality of life of patients with repeat stone recurrence and long-term intubation can be significantly improved after treatment. Percutaneous choledochoscopy can be applied to the treatment of postoperative anastomotic stricture with the benefits of minimal trauma, a simple operation, low cost, high safety and reliability, and the absence of serious complications compared with ERCP and other endoscopic procedures. Furthermore, the operation can be repeated to effectively treat recurrence of anastomotic stricture. In addition, it can be used to remove intrahepatic stones left behind from re-laparotomy.
The following five points should be noted to achieve good therapeutic effects. First, specific criteria should be used to evaluate the degree of anastomotic stricture. Mild stricture is characterized by mild jaundice (serum total bilirubin level of 34.2–171.0 µmol/L), mild liver insufficiency, and a maximum anastomotic diameter of 2 to 3 mm (when the cholangioscope is close after the anastomosis, the maximum anastomotic diameter is less than 2/3 but greater than 1/2 of the diameter of the field of view of the cholangioscope). Severe stricture is characterized by moderate jaundice (serum bilirubin level of 34.2–171.0 µmol/L), moderate or severe liver dysfunction, and a maximum anastomotic diameter of <2 mm (when the cholangioscope is close after the anastomosis, the maximum anastomotic diameter is less than 1/2 of the diameter of the field of view). We did not include the GGT and ALP levels in the evaluation criteria for bilioenteric anastomosis stricture because we found that the GGT and ALP levels were only associated with biliary obstruction; the degree of elevation of GGT and ALP was not closely correlated with the degree of anastomotic stricture. Second, the surgeon must be able to skillfully use a choledochoscope with the assistance of anesthesiologists. Third, when locating the anastomosis is difficult, the cholangioscope should be moved forward under direct vision, and if yellow-white flocculent material or a large amount of bile is found nearby, then the opening of the bile duct is in the vicinity. Fourth, for patients with severe anastomotic stricture or patients in whom the biliary–enteric anastomosis is difficult to identify, percutaneous transhepatic cholangial drainage can first be performed. In this procedure, an antegrade guide wire or catheter drainage tube is placed through the stoma to the intestine, and under its guidance, balloon dilatation of the anastomotic stricture is performed. 13 Finally, attention must be given to the occasional occurrence of sinus perforation, anastomotic bleeding, cholangitis, and other complications.14,15 In the present study, we performed balloon expansion for 10 to 20 minutes to suppress hemostasis.
This study has several limitations. First, it was a retrospective study; a prospective cohort study design will provide more definitive results. Second, no control group was included for a comparative study. Third, the sample size was relatively small, and a longer follow-up period is needed for long-term observation. Finally, the factors leading to unfavorable treatment outcomes require further study.
In summary, great attention should be given to the operative skills necessary to prevent anastomotic stricture formation after the first cholangiojejunostomy procedure. 16 The surgeon must have a sense of prevention of the stricture, and specific conditions should be established during the first operation to facilitate the treatment of cholangiojejunostomy-induced stricture. We believe that the use of percutaneous choledochofiberscopy can allow for easy, safe, and effective diagnosis and treatment of cholangioenterostomy-induced stricture.17,18 Furthermore, the application of intervention-guided percutaneous choledochoscopic balloon dilatation can significantly improve the symptoms of patients with obstructive jaundice. In particular, this treatment would be safe and effective for patients in whom reoperation is difficult and the postoperative prognosis is poor.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
