Abstract
Objective
To evaluate the effect of thrombin (TM) injection via the cerebellomedullary cistern on cerebral vessels in rats with subarachnoid hemorrhage (SAH).
Methods
Eighteen rats were randomly divided into three groups. In the A1 group, physiological saline was injected via the cerebellomedullary cistern; in the A2 group, 3 U of TM was injected into the subarachnoid space; and in the A3 group, SAH models were established and 3 U of TM was injected with the first injection of whole blood. Three days later, basilar artery specimens were collected for pathological examination.
Results
The basilar arterial lumen cross-sectional area was significantly smaller in the A2 versus the A1 group, and proteinase-activated receptor (PAR)-1 and tumor necrosis factor (TNF)-α average optical densities were significantly higher (all P < 0.05). Basilar arterial lumen cross-sectional areas were significantly smaller in the A3 than the A2 group and average TNF-α optical densities were significantly lower (both P < 0.05), while those of PAR-1 did not differ significantly.
Conclusions
There was no significant difference in the extent of cerebral vasospasm between SAH and non-SAH model groups following TM injection into the subarachnoid space, so TM was considered to be an independent factor affecting cerebral vasospasm.
Keywords
Introduction
Subarachnoid hemorrhage (SAH) refers to a type of cerebral hemorrhage in which blood flows into the subarachnoid space after the rupture of intracranial blood vessels. Cerebral vascular spasm (CVS) is a common complication of SAH that occurs with an incidence rate of approximately 30% to 90%. 1 Consequently, it is important to assess, prevent, and treat CVS in SAH patients. The pathophysiological process of CVS includes reversible delayed vascular disease, impaired cerebrovascular auto-regulation, impaired cerebral perfusion caused by insufficient blood volume, 2 increased intracranial pressure, brain edema, and local brain tissue ischemia and hypoxia, eventually leading to neurological loss or even death. Following SAH, blood in the cerebrospinal fluid (CSF) and its metabolites contract through Ca2+-dependent or Ca2+-independent mechanisms, resulting in persistent CVS. 3 Intracranial hemorrhage releases more thrombin (TM) and impairs neurons, glial cells, and cerebral blood vessels for a long period. However, the specific mechanism of TM-induced CVS after SAH remains elusive.
TM exerts its biological action in a receptor-mediated manner. 4 The TM receptor is a proteinase-activated receptor (PAR), which is currently classified into PAR-1, PAR-3, and PAR-4 activated by TM and PAR-2 activated by pancreatin. 5 PAR-1 is a key receptor for TM that mediates intracellular Ca2+ release and protein phosphorylation during CVS. 6 Studies in a rabbit SAH model indicated that TM induces the up-regulation of PAR-1 expression, and that PAR-1 itself plays a pivotal role in this up-regulation and significantly enhances TM-induced CVS. 7 TM can construct a pro-inflammatory environment, especially for vascular endothelial cells and non-specific immune cells. 8 In mouse SAH models, suppressing TM alleviates the inflammatory response, which includes the actions of inflammatory cytokines such as tumor necrosis factor-α (TNF-α) and interleukin (IL)-8 in the incidence and development of CVS. 9
In this study, TM was injected into the rat subarachnoid space via the cerebellomedullary cistern to evaluate its effect on cerebrovascular damage and the underlying mechanism. We also investigated whether the impact of TM injection on cerebrovascular damage differed between SAH and non-SAH rat models, and evaluated the relationship between basilar arterial spasm and cerebrovascular damage.
Materials and methods
Animal selection and breeding conditions
Eighteen healthy male Sprague-Dawley rats, aged 7 weeks and weighing 280 to 330 g, were selected and fed in cages (rats and feed were provided by Changsha Tianqin Biotechnology Co., Ltd., Hunan, China). The animals had free access to food and water. The cages were replaced every 3 to 4 days. The rats were housed at 25°C with a humidity of 66%. Cages were disinfected by UV light on a regular basis. This study was approved by the Medical Ethics Committee of the Third People’s Hospital of Hainan Province.
Animal grouping
Animals were evenly divided into A1 (control), A2 (TM), and A3 (SAH + TM) groups using the random number table method. Ventricular perfusion was performed 3 days after surgery, and basilar artery specimens were collected to measure the cross-sectional area of the basilar arterial lumen and to quantitatively detect the expression levels of PAR-1 and TNF-α.
Establishment of SAH models
The SAH rat model was established using secondary blood injection via the cerebellomedullary cistern. 10 After anesthesia, the rats were placed in a prone position and the skin was cut longitudinally at the occipital protuberance (approximately 1 cm). The tissues were bluntly separated until the occipital fascia was exposed, then the right side of the lower limb was exposed, and the approximate position along the vessel was longitudinally cut to 1.5 cm. The femoral artery was separated under the visual field and the distal end of the vessel was ligated to block the arterial blood flow. The tip of the surgical blade cut the vascular wall at an angle of 45°, and the arterial catheter was inserted into the femoral artery in the direction of the centripetal direction of approximately 0.7 cm. Immediately, autologous arterial blood was extracted by a 1-ml syringe through an intra-arterial catheter and injected it into the subarachnoid space of experimental rats to simulate SAH. The femoral artery was ligated proximally. Rats were fixed in a prone position and hemostatic forceps were used to separate bilateral cervical muscles to expose the temporal occipital fascia. The 1-mL syringe needle was placed at a 30° angle to the neck of the rats and held against the occipital condylar fascia. Next, 0.05 mL cerebrospinal fluid was extracted using a needle about 2 mm below the atlanto-occipital fascia, then 0.25 ml of autologous non-anticoagulant arterial blood was slowly injected (over about 1 minute) into the cerebellomedullary cistern; skin incisions were then sutured. Rats were fixed in a prone position with their heads at an angle of 30° for 30 minutes to facilitate blood distribution in the subarachnoid space and basilar arteries. The same procedures were performed in the left femoral artery 48 hours later.
Establishment of controls and TM models
Femoral arterial blood was not collected. Some of the procedures were the same as the establishment of whole blood models. Upon the first injection, 0.3 mL physiological saline at 37°C or an equivalent quantity of TM (3 U mouse thrombin; Sigma-Aldrich, St Louis, MO, USA) was injected via the cerebellomedullary cistern. After 48 hours, repeated surgery was performed by the injection of 0.3 mL physiological saline through the cerebellomedullary cistern.
Establishment of SAH + TM (3 U) models
Upon the first blood injection, 0.25 mL of autologous fresh arterial blood was injected with TM (3 U) into the cerebellomedullary cistern, and the surgical incisions were sutured. Pre-experiments were carried out with three doses of TM (1 U, 3 U, and 5 U). The rats were then fixed in a prone position with the head at an angle of 30° for 30 minutes to facilitate blood distribution in the subarachnoid space and basilar arteries. The second injection of whole blood was performed 48 hours later (Figure 1).

Model establishment procedures. (a) anesthesia. (b) exposure of the temporal occipital fascia. (c) exposure of the isolated femoral artery. (d) femoral artery blood. (e) injection of autologous blood via the cerebellar medullary cistern. (f), head lowering by 30° for 30 minutes.
Specimen collection
On day 3 after model establishment, 10% chloral hydrate was administered to the abdominal cavity as anesthesia. The abdomen was cut under the xiphoid process, and the chest was opened in a “V” shape to expose the heart. The heart was then cut and the syringe cut at the approximate apex. The needle was used to penetrate the ventricle, and the right atrial appendage was excised. The left ventricle was perfused with normal saline until the right atrial appendage effluent was clear and the limbs became white. Then, approximately 250 mL of 4°C neutral paraformaldehyde was continuously perfused into the rat limbs until all body muscles strongly convulsed. The entire perfusion process lasted for approximately 30 minutes after which the rat body became rigid. The brain was immediately opened for craniotomy and the basilar artery was preserved in neutral paraformaldehyde at 4°C for 24 hours (Figure 2).

The procedures of perfusion and brain tissue collection. (a) rats were sacrificed via perfusion. (b) craniotomy. (c) bottom view in the A1 group. (d) bottom view in the A2 group. (e) bottom view in the A3 group.
Pathological examination
Tissues were soaked in 80% ethanol then 95% ethanol for 3 hours each, then in anhydrous ethanol for 30 minutes, and xylene for 20 minutes twice. Paraffin blocks were frozen at –20°C for 30 minutes, then paraffin sections were cut into thicknesses of 3 to 4 μm, incubated at 65°C for 3 hours, then dewaxed in xylene (I) and xylene (II) for 15 minutes each. They were then rinsed in 95% alcohol twice for 5 minutes each and in 80% alcohol for 1 minute, washed with distilled water for 5 minutes, and stained with hematoxylin for 5 minutes. Finally, they were rinsed in 1% hydrochloric acid-ethanol for 2 seconds, in running water for 15 minutes, then in distilled water for 2 minutes, and stained with 0.5% eosin for 2 minutes.
Assessment of cerebral basilar artery spasm
The extent of basilar artery spasm was measured by the diameter and cross-sectional area of the basilar arterial lumen. A cross-sectional slice was obtained at a point 0.2 mm below the cerebellar artery. 11 Hematoxylin and eosin (HE) staining was performed, and basal arterial morphological changes and the cross-sectional area of the basilar arterial lumen in each slice were measured under an optical microscope and statistically analyzed with Image-Pro Plus software v. 6.0 (Media Cybernetics, Rockville, MD, USA). 12
Assessment of neurological function
Neurological function was scored on a scale from 1 to 4 according to the neurological function score of Endo et al. 13 with 1: normal, without any neurological dysfunction; 2: mild or suspected neurological deficits; 3: moderate neurological deficits without abnormal activity; and 4: severe neurological deficits in limbs. Body paralysis.
Immunohistochemical staining of TNF-α and PAR-1
Slices were placed in xylene for 10 minutes twice, followed by 100%, 95%, 85%, and 75% ethanol for 5 minutes each. They were then rinsed with distilled water for 5 minutes, immersed in 0.01 M citrate buffer (pH 6.0), washed three times in 0.01 M phosphate-buffered saline (PBS; pH 7.2–7.6) for 3 minutes each, then in 3% H2O2 at room temperature for 10 minutes to inactivate endogenous enzymes. Next, they were rinsed three times in PBS for 3 minutes each, incubated with rabbit or mouse primary antibody at 37°C for 1 to 2 hours or overnight at 4°C, washed three times in PBS for 5 minutes each, and incubated with 50 to 100 μL of anti-rabbit/mouse horseradish peroxidase-labeled secondary antibody at 37°C for 30 minutes. Then, they were again washed three times with PBS for 5 minutes each, incubated with 50 to 100 μL of DBA working solution (Zhongshan Jinqiao Biotechnology Co., Beijing, China) for 1 to 5 minutes at room temperature, washed with distilled water, counterstained with hematoxylin for 5 to 10 minutes, then in PBS, xylene (I), xylene (II), and xylene (III) for 2 minutes each, dehydrated in an alcohol gradient (60%–100%) for 5 minutes each, placed in xylene for 10 minutes twice, and covered by neutral gel.
Evaluation of PAR-1 and TNF-α immunohistochemistry
Immunohistochemical staining of basal artery PAR-1 and TNF-α was assessed in a constant visual field (40 × 10) under a light microscope. Five visual fields were randomly chosen for each slice. The positive reaction was based on mean optical density values. The average optical density value of each slice was statistically analyzed.
Statistical analysis
All data were statistically analyzed using the SPSS 17.0 statistical software package (SPSS Inc., Chicago, IL, USA). Measurement data were described using the mean ± standard deviation (means ± s). Comparisons between two groups were analyzed by the independent samples t-test. A P value < 0.05 was considered statistically significant.
Results
Postoperative score of rat behavior
Pre-experiments revealed that 5 U of TM caused brain edema and rapid deterioration of nerve function, sometimes resulting in animal death, while 1 U caused no vascular damage. Therefore, a dose of 3 U was selected. Within 24 hours of SAH model establishment, the rats became mentally fatigued, with greatly reduced activity and reduced intake of water and feed. The sensitivity to external stimuli was also lowered, and limb spasms occurred in a minority of rats. At 1 day after the second blood injection, the above-mentioned symptoms were gradually mitigated and only existed in a few rats until they were sacrificed. After 24 hours, all rats in the A1 group were graded as 1 point. In the A2 group, three rats were graded as 2 points (50%) and three as 3 points (50%). In the A3 group, four rats were graded as 2 points (66.7%) and two as 3 points (33.3%). Twenty-four hours after surgery, the neurological deficits in rats were alleviated.
Histological changes of basilar artery
In the brain of the SAH rat model, a large number of blood clots were diffusely distributed in the subarachnoid space, mainly in the basilar artery and surrounding the Wills ring. In the A1 group, the basilar artery lumen was round or oval with a smooth inner wall. The wall of the artery was thin, the intima was smooth with no wrinkling or bulging, and normal vascular lumen morphology was present. In the A2 group, the basilar artery lumen was narrow with a slightly thickened wall and endothelial folding. In the A3 group, the basilar artery lumen was round or oval with thickening of the vessel wall. In both A2 and A3 groups, a large number of inflammatory cells, mainly neutrophils, and red blood cells had infiltrated around the basilar artery. There was no significant difference in inflammatory cell infiltration between the A2 and A3 groups (Figure 3).

Immunohistochemistry of the basal artery. (a) A1 group (HE 10 × 10). (b) A2 group (HE 10 × 10). (c) A3 group (HE 10 × 10). (d) inflammatory cell infiltration surrounding the basilar artery (HE 10 × 40). HE, hematoxylin and eosin.
Immunohistochemical staining of PAR-1
Under the light microscope, positive PAR-1 expression appeared as a brown or brownish-yellow color. In the A1 group, no positive expression of PAR-1 was evident in basilar artery tissues. In the A2 group, PAR-1 expression was higher in the vascular wall compared with the A1 group (Figure 4).

Immunohistochemistry of PAR-1 in the basilar artery. (a) A1 group (HE 40 × 10). (b) A2 group (HE 40 × 10). (c) A3 group (HE 40 × 10). HE, hematoxylin and eosin.
Immunohistochemical staining of TNF-α
Under the light microscope, positive TNF-α expression appeared as a brown or brownish-yellow color. In the A1 group, no significant positive expression of TNF-α was observed in the basilar artery wall. However, TNF-α expression in the vascular wall was up-regulated in the A2 group compared with the A1 group (Figure 5).
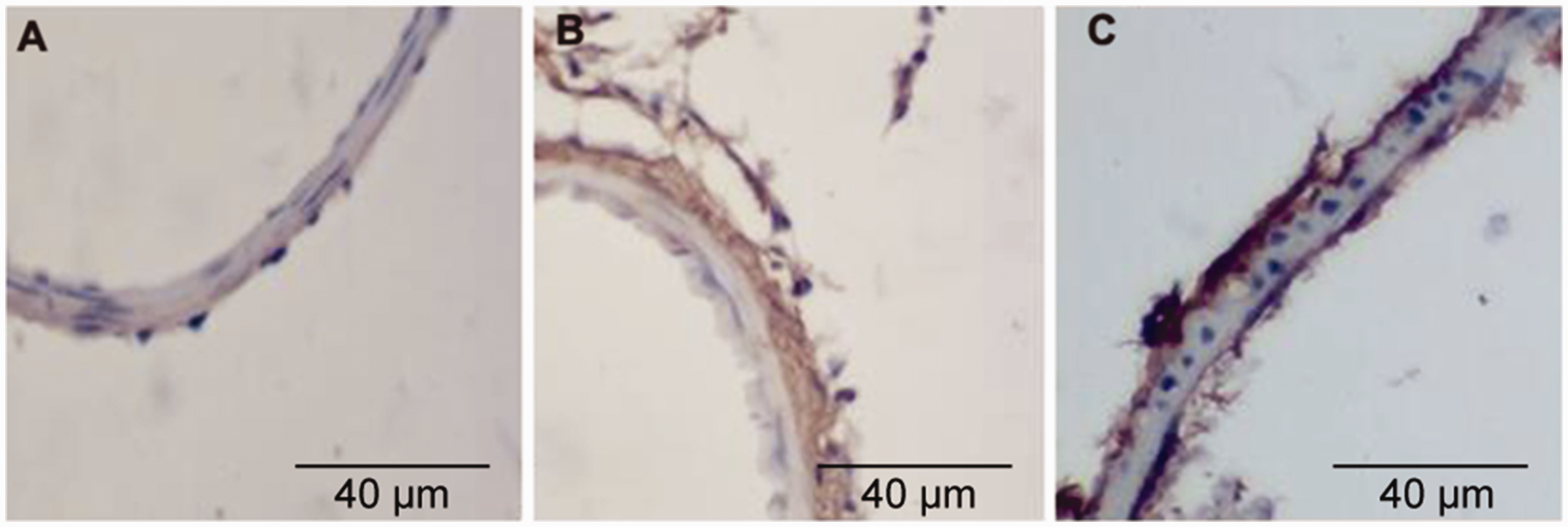
Immunohistochemistry of TNF-α in the basilar artery. (a) A1 group (HE 40 × 10). (b) A2 group (HE 40 × 10). (c) A3 group (HE 40 × 10). HE, hematoxylin and eosin.
Comparison of PAR-1 and TNF-α expression and the lumen area between A1 and A2 groups
Using the independent samples t-test, TNF-α and PAR-1 expression levels and the cross-sectional area of the basilar arterial lumen were shown to differ significantly between the A1 and A2 groups (all P < 0.05). Specifically, the cross-sectional area of the basilar arterial lumen in the A2 group was considerably smaller than in the A1 group, whereas the mean optical densities of TNF-α and PAR-1 in the A2 group were significantly higher compared with those in the A1 group (P < 0.05; Table 1).
Comparison of three parameters between A1 and A2 groups (n = 6).

PAR, proteinase-activated receptor; TNF, tumor necrosis factor.
Comparison of PAR-1 and TNF-α expression and the lumen area between A2 and A3 groups
Using the independent samples t-test, the cross-sectional area of the basilar arterial lumen and the average optical density of TNF-α differed significantly between A2 and A3 groups (both P < 0.05), whereas the average optical density of PAR-1 was not significantly different. The cross-sectional area of the basilar arterial lumen in the A3 group was smaller than in the A2 group, whereas the average optical density of TNF-α was also lower than in the A2 group (Table 2).
Comparison of three parameters between A2 and A3 groups (n = 6)

PAR, proteinase-activated receptor; TNF, tumor necrosis factor
Discussion
Three methods are commonly adopted to establish SAH models. 14 The first is intracranial vascular puncture, which uses different approaches to expose target vessels, then punctures the artery and allows blood to enter the subarachnoid space, leading to hemorrhage. 15 The second method is blood injection into the cerebral cistern. In this technique, fresh autologous arterial blood is collected and injected through the lateral ventricle, cerebellomedullary cistern, and optic chiasmatic cistern to induce SAH. 16 In the third method, craniotomy is performed to expose intracranial arteries, then fresh autologous arterial blood extracted from other sites is injected into the exposed intracranial arteries. 17 Secondary blood injection via the cerebellomedullary cistern has been frequently used, 18 and yields a high success rate and a low postoperative mortality rate. Therefore, this technique was employed in our experiment.
Fresh blood can be rapidly coagulated by TM, and 1 U of TM was reported to coagulate 1 mL of blood within 15 s. 19 In this study, we injected exogenous TM into the subarachnoid space of SAH models after the injection of autologous blood into the cerebellomedullary cistern. Subsequently, the rat heads were lowered by approximately 30° for several minutes to allow the blood to diffuse into the subarachnoid space and avoid the formation of blood clots. After the experiment, only a small number of blood clots were detected in the cerebellum medulla.
TM is a terminal serine protease present in the serum, which is produced by the catalytic lysis of prothrombin by the prothrombinase complex. It plays a vital role in the balance of coagulation–anticoagulation and hemostasis–fibrinolysis under the physiological state. TM can initiate the thrombin system and activate physiological hemostasis by regulating a cascade of coagulation events, leading to cerebral vascular injury. Approximately one-third of patients with aneurysmal SAH are reported to present with cerebral vascular spasm and ischemic brain dysfunction. Because these severe complications resulting from CVS are the main causes of neurological dysfunction and death, 2 it is extremely important to prevent and treat the incidence of CVS after SAH. In the present study, the cross-sectional area of the basilar arterial lumen was chosen to assess the extent of vascular contraction. A higher severity of vascular spasm correlated with a smaller lumen area.
The exact mechanism underlying TM-induced CVS remains elusive. A previous study demonstrated that 1 to 1000 U/mL of TM caused persistent vascular smooth muscle contraction, similar to endothelin. 20 The mechanism underlying TM-mediated vascular contraction is probably related to two signal transduction pathways. 21 One is the myosin light chain kinase (MLCK) signaling pathway in which blood and related metabolites increase intracellular Ca2+ concentrations and phosphorylate myosin light chain, resulting in the contraction of vascular smooth muscle. The other is the mitogen-activated protein kinase (MAPK) signaling pathway. Hemolysis-related products can provoke MAPK cascade reactions, leading to cerebral arterial contraction. 22 Studies of a rabbit SAH model demonstrated that TM released into the CSF promotes tyrosine phosphorylation of the growth factor receptor and activation of receptor tyrosine kinase, which activates MAPK cascade reactions to induce vascular contraction. 23 TM inhibitors, such as anti-thrombin III, can significantly mitigate CVS by inhibiting activation of the MAPK signaling pathway. 24
After SAH, vascular contraction is mainly contributed to in a Ca2+-dependent and Ca2+-independent manner. The occurrence of CVS may be associated with MLCK and MAPK signaling pathways. TM exerts a biological effect by binding to PAR and activating receptors PAR-1, PAR-3, and PAR-4. 25 PAR-1 is the most relevant to CVS, being expressed in the vessel system and also distributed in neurons, astrocytes, microglia, and oligodendrocytes. After SAH, the blood–brain barrier is destroyed and TM can enter the brain where it binds PAR-1 to provoke cerebral injury. 26 In SAH rabbit models, up-regulated PAR-1 expression significantly increased vascular contraction, while down-regulating PAR-1 expression mitigated vascular contraction. 27 The mechanism underlying TM-induced PAR-1 up-regulation was reported to be irreversible. When occurring in the rat hippocampus, it led to a rapid increase in intracellular Ca2+ concentrations and a slow decrease in cyclic adenosine monophosphate levels. 28 An increased Ca2+ concentration is an important mechanism in the contraction of vascular smooth muscle, suggesting that TM is closely correlated with PAR-1 up-regulation and vascular contraction. In our experiment, the effect of TM on vascular spasm was evaluated by detecting PAR-1 expression in the rat basilar arteries. The change in PAR-1 expression induced by TM was consistent with the worsening vasospasm. The alleviation of neurological deficits 24 hours after surgery likely reflected abundant cerebral vessel circulation.
Previous studies demonstrated that TM is not only an important substance in the coagulation system, but can also lead to the spread of inflammation, the proliferation of inflammatory cells, and the production of proinflammatory cytokines. These activate microglia in the brain, 27 which are pivotal immune cells that are intrinsic to the nervous system. Vecchione et al. 5 suggested that CVS is caused by oxidative stress and inflammation after SAH. TM induces the proliferation of inflammatory mediators, such as TNF-α, IL-6, IL-12, cytokine KC, and TNF-α receptors. 29 These inflammatory mediators aggravate the vascular spasm after cerebral hemorrhage, and TNF-α plays an important role in the occurrence and development of this spasm. 30 TNF-α is a potent pro-inflammatory cytokine that is highly expressed in human intracranial aneurysms. It amplifies the signaling pathways between cells, leading to increased inflammatory responses, apoptosis, and degenerative changes of nerve tissue. 31 Hanafy et al. confirmed that the level of TNF-α in the CSF 4 to 6 days after SAH is positively correlated with CVS. 9 As a natural antagonist of TM, anti-thrombin III (AT-III) reduces the post-hemorrhagic inflammatory response and regulates coagulation by reducing the production of pro-inflammatory cytokines such as TNF-α. 32 The topical administration of AT-III mitigates the severity of CVS after SAH and inhibits MAPK phosphorylation, suggesting that TM and its related signal transduction pathways function in the pathogenesis of CVS after SAH.
We quantitatively measured the expression level of TNF-α in the basilar artery to reflect the effect of TM upon the cerebral blood vessel injury. Because CVS occurred 3 days post-SAH, the rats were sacrificed on the third day of successful model establishment and specimens were harvested to observe the manifestations of cerebrovascular damage during the early stages of CVS. We observed that the expression of PAR-1 and TNF-α and the cross-sectional area of the basilar arterial lumen differed significantly between A1 and A2 groups. In the A2 group, the extent of basilar arterial contraction was more severe than in the A1 group, and PAR-1 and TNF-α expression levels in the basilar artery wall were significantly up-regulated. This suggested that subarachnoid injection of TM causes CVS in the presence of SAH and that TM impairs cerebral blood vessels. The cross-sectional area of the basilar arterial lumen and TNF-α levels differed significantly between A2 and A3 groups. In the A3 group, the lumen area was smaller than in the A2 group, and TNF-α expression was down-regulated. There was no significant difference in the expression of PAR-1, indicating that the extent of cerebral vascular contraction is enhanced by TM in SAH, whereas TNF-α expression was increased in the vascular wall and PAR-1 expression was unchanged. These results collectively reveal that the injection of TM into the subarachnoid space had no significant effect on cerebral vascular contraction irrespective of the presence or absence of SAH. Consequently, TM is considered to be an independent factor affecting CVS.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This study was funded by the Scientific Research Subject from the Health Department of Hainan Province (grant no. 2010-64).
