Abstract
Objective
This study aimed to investigate the application of an artificial neural network (ANN) in optimizing the Osteoporosis Self-Assessment Tool for Asians (OSTA) score.
Methods
OSTA score was calculated for each female participant that underwent dual-energy X-ray absorptiometry examination in two hospitals (one in each of two Chinese cities, Harbin and Ningbo). An ANN model was built using age and weight as input and femoral neck T-score as output. Osteoporosis risk screening by joint application of ANN and OSTA score was evaluated by receiver operating characteristic curve analysis.
Results
Nearly 90% of women with dual-energy X-ray absorptiometry-determined femoral neck osteoporosis were ≥60 years old. The ANN with age and weight as input and OSTA score both identified osteoporosis, with respective accuracy rates of 78.8% and 78.3%. However, both methods failed to identify osteoporosis in women < 60 years old. Compared with OSTA score alone, combined use of the two tools increased the rate of osteoporosis recognition among women > 80 years old.
Conclusions
OSTA score-mediated osteoporosis risk screening should be restricted to women ≥60 years old. Joint application of ANN and OSTA improved osteoporosis risk screening among Chinese women > 80 years old.
Keywords
Introduction
The human lifespan is continuously increasing, 1 which has resulted in the emergence of an aging society. 2 A high density of aged individuals increases the health and social burden on society, such that there is an urgent need for better understanding of age-related pathological changes and interventions to achieve successful aging. Older adult individuals may experience altered body composition, including bone and muscle loss. 3 Dysfunctional crosstalk among tissues may lead to accelerated aging of bone, which can adversely affect other tissues and organs. 4 Bone therefore comprises both a protective structural tissue and an active endocrine organ that is vital for maintenance of an individual’s overall health status, 5 particularly among older adults.
Bone is in a dynamic state of continuous tissue remodeling. In humans, there are three types of cells involved in this process. 6 Osteoblasts contribute to bone formation, whereas osteoclasts promote bone resorption. Osteoblastic bone formation and osteoclastic bone resorption are regulated by osteocytes, which secrete growth factors. Importantly, an imbalance in osteoblast function may result in reduced formation of bone mass and impaired microarchitecture. Continuous decline in bone mineral density (BMD) leads to osteoporosis, which increases fracture risk in older adults. 7 A reduction of BMD by one standard deviation, as measured by dual-energy X-ray absorptiometry (DXA), reportedly doubles the risk of fracture. 8 Numerous factors can trigger continuous decline in bone mass; these increase the risk of death and reduce autonomy.9,10
Low BMD increases future fracture risk, but BMD alone cannot adequately predict future fracture risk. 11 Fracture risk assessment indices can be used to identify individuals who are at risk for fractures. 12 However, such screening and subsequent recommendations may cause overdiagnosis and overuse of current pharmaceutical resources. 13 Osteoporosis is the main cause of fracture. 14 The Osteoporosis Self-Assessment Tool for Asians (OSTA) is commonly used for osteoporosis risk assessment. 15 Although OSTA only uses age and body weight as variables, it can effectively identify DXA-determined osteoporosis in a Chinese population. 16 Recently, artificial intelligence technology has been explored for osteoporosis risk screening; 17 an artificial intelligence model could identify osteoporosis more accurately than traditional methods by using > 10 quantitative indicators. 18 These additional indicators improve the risk identification accuracy, but reduce the applicability of the tools. Here, using data from women in two Chinese cities, Harbin and Ningbo, we investigated whether an artificial intelligence model—an artificial neural network (ANN)—could enhance the function of OSTA without the use of new indicators.
Materials and methods
Ethical statement
This study was approved by the Ethics Committee of the Second Affiliated Hospital of Harbin Medical University (Approval number: KY2018-131) and the Ethics Committee of Ningbo Health Career Technical College; it was carried out in accordance with the tenets of the Declaration of Helsinki.
Participant characteristics
All participants were women ≥20 years old. Written/verbal consent was obtained from each participant. The electronic medical record systems of the Second Affiliated Hospital of Harbin Medical University and the Affiliated Hospital of the Medical School of Ningbo University were used to access the participants’ medical records. Age, weight, height, and femoral neck T-score were recorded for use as raw data. Participants from the Second Affiliated Hospital of Harbin Medical University were randomly divided into two datasets, dataset I and dataset II. Participants from the Affiliated Hospital of the Medical School of Ningbo University were all grouped in dataset III. The three datasets (I, II, and III) were used for respective training, external validation, and external testing of the OSTA score and the ANN established in the present study. Femoral neck T-scores were obtained using two DXA scanners (Hologic Inc., Bedford, MA, USA). Moderate reduction in BMD or osteopenia was defined as a femoral neck T-score of ≤ −1.0 and > −2.5, while marked decline in BMD or osteoporosis was defined as a femoral neck T-score of ≤ −2.5. 19 For each participant, the OSTA score and body mass index (BMI) were also calculated according to the OSTA formula 15 of (weight (kg)-age (year))×0.2 and the BMI formula of weight (kg)/square of height (m2). 20
Integrating age and weight into an ANN model
The original age and weight values were used as ANN input and femoral neck T-scores were regarded as training model output with the software STATISTICA Neural Networks (SNN, Release 4.0E; Statsoft, Tulsa, OK, USA). Subsequently, the Intelligent Problem Solver (IPS) tool was used to divide all participants of dataset I into three subsets (training, verification, and testing) in a 2:1:1 ratio and automatically generate a radial basis function ANN.
Model validation
A holdout cross-validation method was built into the SNN software for internal validation of the ANN model. Respective correlation coefficients were calculated for the training (RTr) and testing (RTe) subsets; these measured the correlation between predicted and actual femoral neck T-scores. Similar RTr and RTe values indicated that the ANN model had good generalizability. 21 The 10-fold cross-validation method was applied to further validate the ANN model, as previously described. 21 Briefly, participants in dataset I were randomly divided into 10 mutually exclusive groups of nearly equal size. Then, nine groups were selected to establish an ANN, and the remaining group was used for model validation. This procedure was repeated 10 times to ensure that all 10 groups were independently validated. Datasets II and III were used for external validation and external testing of the ANN model, as well as to compare the efficiencies of the ANN model and OSTA score in identifying femoral neck osteoporosis. Receiver operating characteristic (ROC) curve analysis was performed to determine the sensitivity, specificity, and accuracy of the ANN output and OSTA score, with the optimal criteria. In addition, femoral neck osteoporosis recognition rates were calculated for participants in different age groups within datasets II and III. Recognition rates were defined as the proportions of participants with DXA-determined osteoporosis who were successfully identified by ANN output, OSTA score, or both, relative to the total number of participants in each age subgroup.
Statistical analysis
All data are expressed as mean ± standard deviation. Graphpad Prism software (version 6.0, GraphPad Software, Inc., La Jolla, CA, USA) was used to perform one-way analysis of variance and Dunnett's multiple comparisons test. ROC curve analysis was performed by using MedCalc version 18.2.1 (MedCalc, Mariakerke, Belgium). Differences with p <0.001 were considered to be statistically significant.
Results
The incidence of osteoporosis rapidly increased with age
In Harbin, a total of 1559 women were included in the study, among which 428 were diagnosed with DXA-determined femoral neck osteoporosis; these 1559 women were randomly divided into two datasets (datasets I and II; the two datasets did not significantly differ in the assessed demographic characteristics) (Table 1). In Ningbo, 502 women were included in the study, among which 115 were diagnosed with DXA-determined femoral neck osteoporosis (dataset III) (Table 1). The overall incidence of femoral neck osteoporosis in Ningbo was 22.9%, whereas it was 27.5% in Harbin. Notably, the incidence of femoral neck osteoporosis before 60 years old increased slowly with age; however, upon reaching 60 years old, the incidence began to rise rapidly with age (Figure 1). This tendency was observed in both Harbin and Ningbo; overall, however, women with femoral neck osteoporosis in Harbin were younger than those in Ningbo.

Incidence of osteoporosis in different age ranges in Harbin (a, datasets I and II) and Ningbo (b, dataset III). The incidence of osteoporosis is defined as the percentage of participants with dual-energy X-ray absorptiometry-determined femoral neck osteoporosis in a specific age range.
Participant characteristics.

Values are mean ± standard deviation. #p < 0.001, *p < 0.0001, compared with Dataset III.
ANN was effective as a tool for femoral neck osteoporosis identification
A radial basis function ANN with a 2-4-1 architecture was successfully constructed by applying the IPS tool that was built into the SNN software. The RTr and RTe values were 0.359 and 0.437. ROC curve analysis indicated that the ANN successfully identified femoral neck osteoporosis among participants in dataset II with an area under the ROC curve (AUC) of 0.829. Ten-fold cross-validation suggested that the model had stable recognition ability (AUC = 0.828). By using an optimal criterion of ANN output > 0.511, the ANN provided highly specific identification of femoral neck osteoporosis with a moderate accuracy rate (Table 2). The specificity and accuracy rate of the OSTA score for identifying femoral neck osteoporosis were comparable to those of the ANN when using an optimal criterion of an OSTA score of 3.
Comparison of receiver operating characteristic curve analysis parameters between the Osteoporosis Self-Assessment Tool for Asians and the artificial neural network.
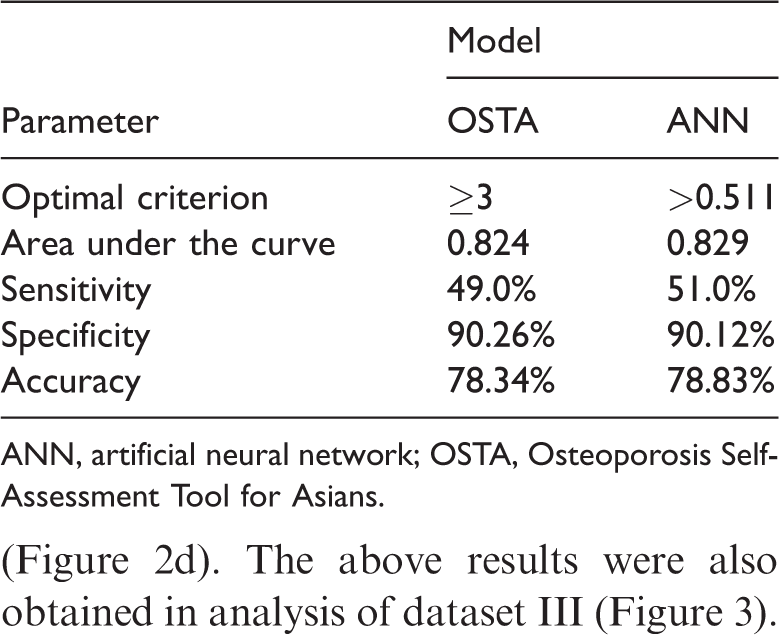
ANN, artificial neural network; OSTA, Osteoporosis Self-Assessment Tool for Asians.
ANN enhanced femoral neck osteoporosis recognition by the OSTA among women ≥80 years old
In dataset II, 195 participants (37.5%) were < 60 years old. Among them, only 14 had DXA-determined femoral neck osteoporosis. Nearly 90% of women with femoral neck osteoporosis in the present study were ≥60 years old. The OSTA failed to identify femoral neck osteoporosis among women < 60 years old (Figure 2a). Addition of the ANN (i.e., co-application of the OSTA and ANN) did not improve the effectiveness of femoral neck osteoporosis identification in this low age subgroup (Figures 2b and c). Comparatively, co-application of the OSTA and ANN increased the recognition rate of femoral neck osteoporosis in women > 80 years old, from 30.0% to 42.9% (Figure 2d). The above results were also obtained in analysis of dataset III (Figure 3).
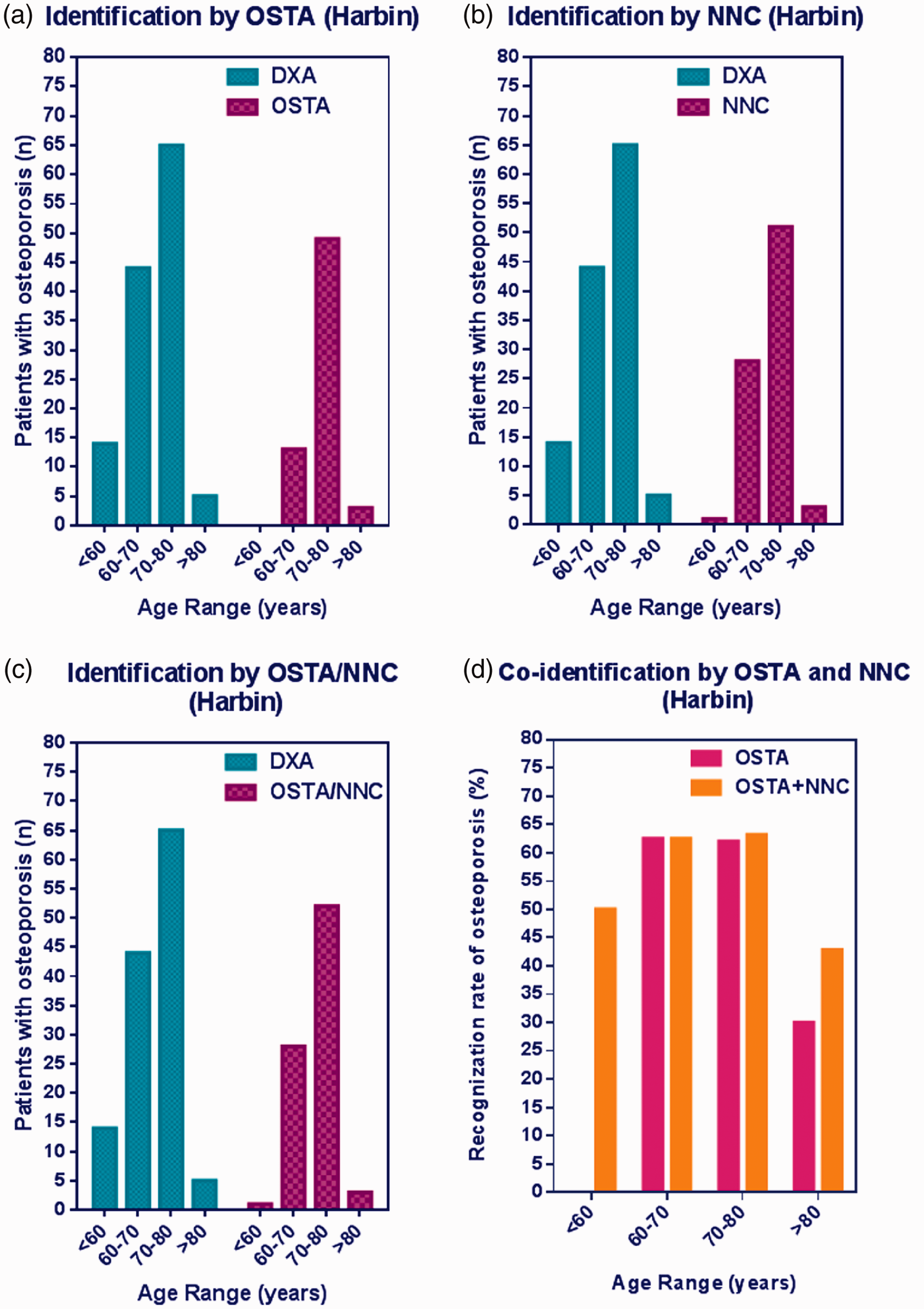
Validation of the Osteoporosis Self-Assessment Tool for Asians and the artificial neural network for identifying osteoporosis in dataset II. (a–c) Respective applications of OSTA, ANN, and OSTA/ANN for osteoporosis identification with the gold standard dual-energy X-ray absorptiometry as reference. (d) Recognition rates of osteoporosis by both OSTA and ANN.
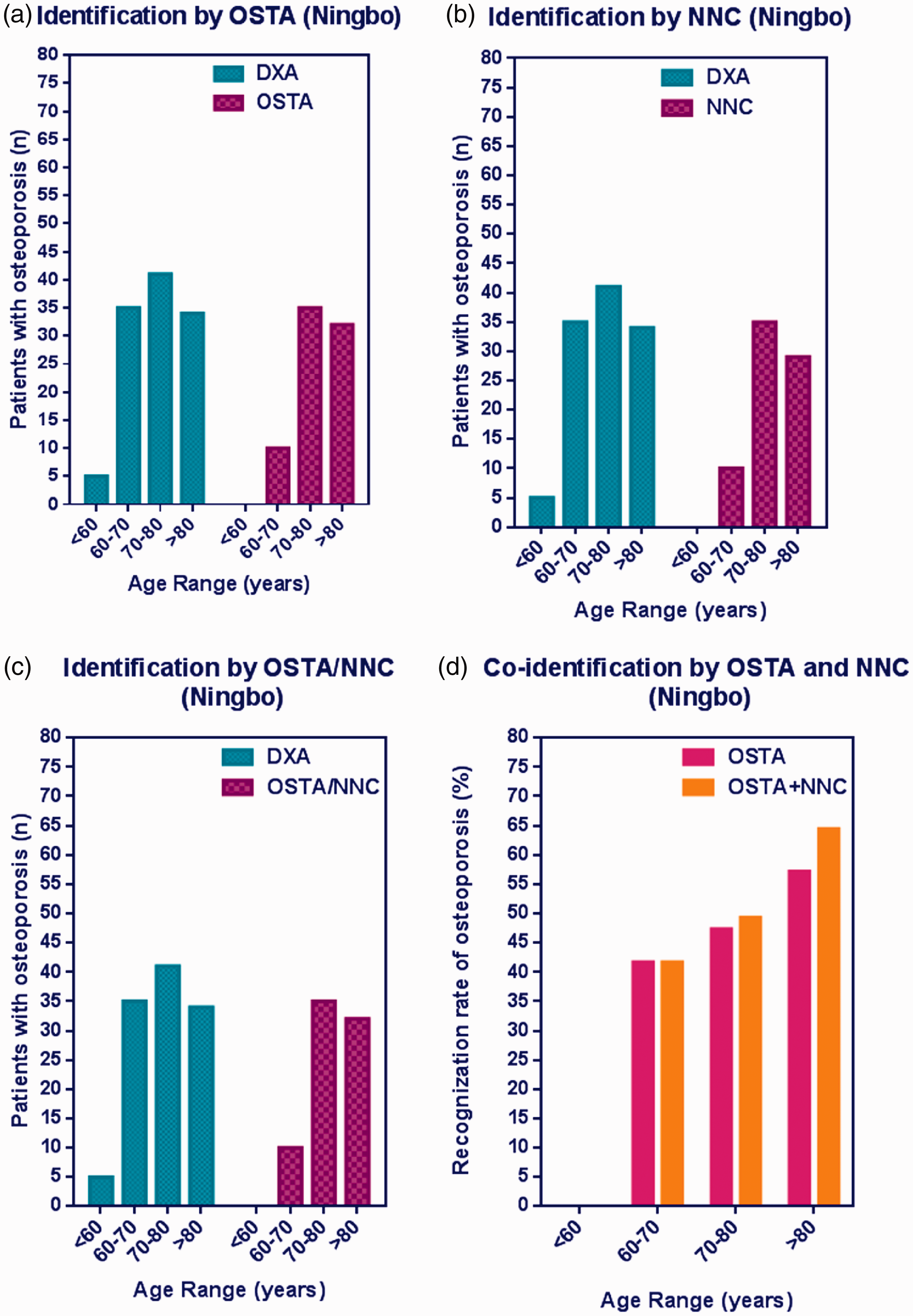
External testing of the Osteoporosis Self-Assessment Tool for Asians and the artificial neural network for identifying osteoporosis in dataset III. (a–c) Respective applications of OSTA, ANN, and OSTA/ANN for osteoporosis identification with the gold standard dual-energy X-ray absorptiometry as reference. (d) Recognition rates of osteoporosis by both OSTA and ANN.
Increased height of younger women caused the OSTA to fail in identification of femoral neck osteoporosis
Three body indicators—weight, height, and BMI—were investigated to explore the inability of OSTA to effectively identify women <60 years old with femoral neck osteoporosis. Generally, a taller individual has higher weight than a shorter individual. 22 In datasets I and II, compared with women who were >80 years old, those who were <60 years old had significantly greater height and weight (Dunnett's multiple comparisons test, q for height = 6.247, q for weight = 3.757, degrees of freedom = 1555, p < 0.001, effect size for height (difference between group means) = 0.05 m, effect size for weight = 6.1 kg, Figures 4a and b). However, the mean BMI of women < 60 years old was 23.78, which was only slightly higher than the mean BMI of 22.87 of the women > 80 years old; the difference was not statistically significant (Figure 4c). Because of the inverse relationship between body weight and age in the OSTA formula, the increased height of the younger women explained the inability of the OSTA to identify femoral neck osteoporosis in this subgroup. The results obtained in dataset III were consistent with the observations in datasets I and II (Figures 4d–f).

Comparisons of weight, height, and body mass index in different age ranges in Harbin (a–c, datasets I and II) and Ningbo (d–f, dataset III). #p < 0.001, *p < 0.0001, compared with > 80 years old.
Discussion
Osteoporosis is characterized by reduced bone mass and deteriorating bone microarchitecture, and is prevalent in older adults, especially in postmenopausal women; consequently, osteoporosis increases the probability of fractures in older individuals. 23 Our retrospective analysis of two independent datasets confirmed the severity of this trend, in that nearly 90% of women in Harbin with femoral neck osteoporosis were ≥60 years old; similarly, approximately 96% of women in Ningbo with femoral neck osteoporosis were ≥60 years old. Among osteoporotic fractures, hip fracture is associated with the highest mortality. 24 Patients with hip fracture experience increased mortality, regardless of the time elapsed after fracture. 25 Femoral neck fracture comprises 53% of all fractures of the proximal femur, which is the hip region most vulnerable to fracture 26 and is one of the most common traumatic injuries in older individuals. 27 In this context, the findings of our study suggest that women ≥60 years old should be regarded as a population with an extremely high risk of femoral neck fracture because they exhibit a very high prevalence of femoral neck osteoporosis. Thus, current bone health screening policy should place greater emphasis on this population, with more specific osteoporosis risk assessments that are optimized for this population.
Thus far, there has been considerable effort to develop osteoporosis risk self-examination instruments for identification of individuals with osteoporosis in the overall population. The most common instruments include the OSTA score, the simple calculated osteoporosis risk estimation instrument, osteoporosis index of risk, and the osteoporosis risk assessment instrument. 28 Among these instruments, the OSTA score is the simplest method and showed the best performance in a large sample. 18 In the present study, we also confirmed that the OSTA score could identify femoral neck osteoporosis with high accuracy. In addition, osteoporosis has been associated with a variety of triggers.9,10 Consistent with these associations, a prior analysis showed that the integration of a package of 11 risk factors into a support vector machine model could improve the identification of osteoporosis in postmenopausal Korean women. 18 However, the authors of that study found that the inclusion of additional variables in the model reduced its applicability in practice because participants did not accurately provide exact values for some variables. Relative to other indicators, objective measurements of age and weight can be accurately obtained. This is an obvious advantage of the OSTA score over other osteoporosis risk assessment methods. Rather than incorporating an increasing number of potential indicators into a model, we allowed different models to complement each other with their existing indicators. Co-application of the OSTA with an ANN that was established by using age and weight as input was proven to increase the recognition rate of femoral neck osteoporosis in women > 80 years old, compared with use of the OSTA score alone. Our results suggest that this approach is effective and imply that other artificial intelligence algorithms may also be useful for optimizing age and weight models for osteoporosis screening in further studies.
Our study results also suggest that the OTSA score might not be effective for identifying DXA-determined femoral neck osteoporosis in Chinese women < 60 years old, with respect to epidemiological analysis. Generally, individuals with increased body height have greater weight. Our observations were consistent with this trend. Younger Chinese women were taller and heavier than those of the previous generation. In China, overweight and obesity have become a current epidemiological trend because of rapid economic development and the resulting altered dietary intake.29,30 According to the OSTA score formula, increased weight will reduce the risk of osteoporosis when age remains constant. Thus, our results suggest a reduced incidence of femoral neck osteoporosis in Chinese women < 60 years old. Therefore, it may be inappropriate to emphasize the risk of osteoporosis in this population. However, a broader epidemiological study of femoral neck osteoporosis in women should be performed to validate these findings. The OSTA score continues to effectively identify femoral neck osteoporosis in Chinese women ≥60 years old. Thus, its inability to identify osteoporosis among women < 60 years old indicates that a new risk identification method is needed for this younger population. Although our results indicated that increased height was associated with greater weight, and therefore with a reduced risk of femoral neck osteoporosis in younger Chinese women, height should not be regarded as a strong predictor of femoral neck osteoporosis. 31 Moreover, appropriate nutrition, rather than increased height and weight, should be emphasized in efforts to delay the occurrence of aging-related diseases, such as femoral neck osteoporosis. 32
Conclusions
We made two important findings with respect to risk assessment of femoral neck osteoporosis in Chinese women. First, co-application of the ANN and the OSTA score improved femoral neck osteoporosis risk identification, relative to that of the OSTA score alone, without the use of additional indicators that may not be objectively quantified. Second, the OSTA score is not an appropriate femoral neck osteoporosis risk assessment tool for young Chinese women because it may yield false negative predictions. However, careful consideration is needed prior to any alterations in the practical use of the OSTA score because of the limitations of the present study (i.e., limited geographical area and limited sample size). Finally, our study is important in that promotes the re-evaluation of conventional methods of osteoporosis risk assessment and screening, especially with respect to differences among women across multiple age groups.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This work was supported by the National Natural Fund Committee (grant number: 71774092).
