Abstract
Robert’s uterus is an asymmetric septate uterus with a noncommunicating cavity and is a rare Müllerian anomaly. We present a rare case of pregnancy in a blind cavity and the first report of ipsilateral renal agenesis. A 23-year-old primigravida woman presented to our hospital at 7 weeks and 3 days of gestation after an abortion had failed. Three-dimensional ultrasound and magnetic resonance imaging showed pregnancy in a blind hemi-cavity of Robert’s uterus with an ipsilateral renal anomaly. Surgery was performed by hysteroscopy with laparoscopic and ultrasound guidance. The pregnancy was removed and the asymmetric septum was resected. A single normal uterine cavity with bilateral tubal ostium remained. The treatment was considered to be satisfactory. Menstruation ceased to be painful and the uterus was not scarred. Robert’s uterus can be well evaluated by an experienced ultrasound physician and magnetic resonance imaging. Such patients may have renal agenesis and the urinary system must be simultaneously evaluated. Pregnancy in a blind hemi-cavity is extremely rare and easily ignored by gynecologists and sonographers. Timely and accurate diagnosis of this condition is essential to obtain minimally invasive treatment.
Introduction
Robert’s uterus is an asymmetric septate uterus characterized by a uterine septum dividing the uterine cavity into a blind hemi-cavity and a contralateral nonobstructing hemi-cavity that is connected normally to the cervix. The blind cavity obstructs menstrual flow and permits partial reflux of retained menstruation into the peritoneal cavity, 1 resulting in hematometra, dysmenorrhea, hematosalpinx, and even endometriosis. Endometriosis includes ovarian and deep infiltrating endometriosis, which is accurately detected by transvaginal ultrasound, but superficial endometriosis needs to be detected by laparoscopy. 2 There are three main clinical types of Robert’s uterus as follows: (i) with a large hematometra, (ii) without hematometra, and (iii) with a small hematometra in a blind hemi-cavity. 3 Another type of Robert’s uterus with a small hematometra or without hematometra can occur, as in our case, before pregnancy. To date, only a few cases have been reported in the literature with pregnancy in the noncommunicating cavity. 4 These were finally confirmed as pregnancy in one blind cavity of Robert’s uterus due to recurrent failed attempts at terminating the fetus in middle and late pregnancy. These cases underwent laparotomy and had a permanent scar in the uterus.
We report a rare case of pregnancy in a blind cavity of Robert’s uterus. This is the first case of early pregnancy treated by hysteroscopy with laparoscopic and transabdominal ultrasound guidance. We discuss the importance of early and accurate diagnosis for guiding appropriate surgery. Our case is also unique because of its atypical presentation as ipsilateral renal agenesis.
Case report
A 23-year-old woman, gravida 1, para 0, presented to our hospital at 7 weeks and 3 days of gestation after a failed abortion. She attained menarche at 12 years old with moderate dysmenorrhea and normal menstruation. Her menstrual cycles were regular at a 30-day interval for 7 days. Pain started at the first 3 day of cycles and bloating presented at the last 4 days of menstruation, without progressing to chronic pelvic pain. The intensity of symptoms had not progressively increased since menarche. There was no historical treatment for dysmenorrhea. A gynecological examination indicated an anatomically normal vulva, vagina, and cervix. The gravid uterus was the size of 8 weeks’ gestation and the right corpus was slightly larger than the left. Two-dimensional ultrasound showed that the uterus was anterior (6.2 × 5.2 × 8.6 cm) and the uterine cavity had a unicornuate left uterus. A muscle mass (4.3 × 4.3 × 3.9 cm) was detected on the right middle upper side of the unicornuate uterus, which showed a rudimentary right uterus. The fetal sac (2.2 × 1.2 × 1.2 cm) with a small embryo and primitive cardiac beat were observed inside the uterus (Figure 1A). Three-dimensional (3D) ultrasound by an experienced ultrasound physician clearly showed Robert’s uterus. An asymmetric septum completely divided the uterine cavity into an obstructed hemi-cavity in the right side and a contralateral nonobstructing hemi-cavity in the left side was connected normally to the cervix. The pregnancy was in the right blind cavity and there was adenomyosis (Figure 2A). She was further evaluated by magnetic resonance imaging (MRI) (Figure 3), which showed the same results as 3D ultrasound. The patient’s urinary system was also evaluated. Renal imaging studies showed that the right kidney was absent and there was an ectatic left kidney (Figure 1B).

Two-dimensional ultrasound images. (A) Right rudimentary uterine horn pregnancy (black arrow) and left unicornuate uterus (white arrows). (B) Absent right kidney (white arrows) and an ectatic left kidney

Three-dimensional ultrasound images. (A) Pregnancy (black arrow) in the right blind cavity and left cavity is connected to the cervix preoperatively. (B) The shape of the uterine cavity is closer to normal without a uterine septum and intrauterine adhesions postoperatively
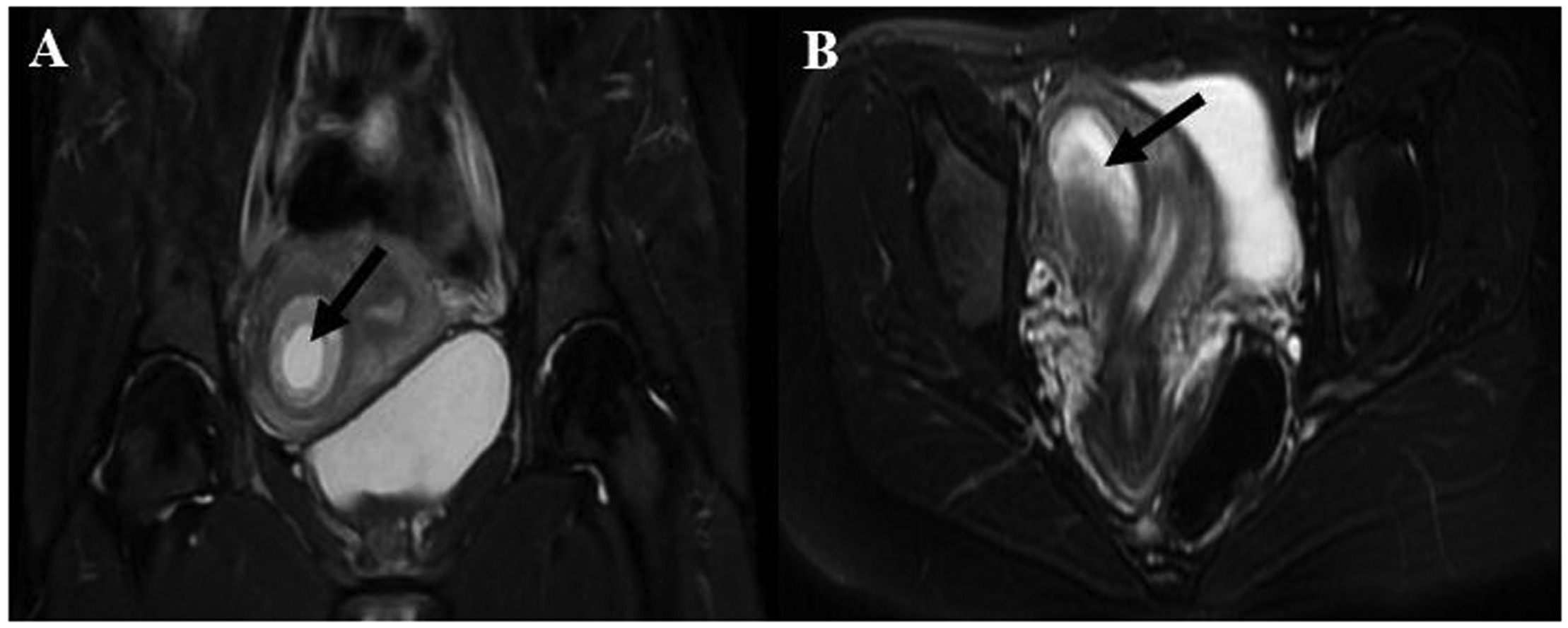
Magnetic resonance images. Axial (A) and coronal (B) images show pregnancy (black arrows) in the right blind cavity
We performed hysteroscopic electrotomy with laparoscopy and transabdominal ultrasound guidance under general anesthesia. In laparoscopy, the finding of a previous gynecological examination of a slightly enlarged uterus on the right side was confirmed (Figure 4). The external shape of the uterine fundus was normal. Violet blue nodules were observed on the surface of the right uterus and uterosacral ligament. Both ovaries and fallopian tubes were normal. The right kidney and ipsilateral ureter were absent. We excised the violet blue nodules and a histological report was compatible with the diagnosis of endometriosis. In hysteroscopy, the left tubal ostium was observed. On the right side, there was an asymmetrical uterine septum, which obstructed the right uterine cavity, so that the pregnancy and right tubal ostium were not visualized (Figure 5). Robert’s uterus with pregnancy in a blind hemi-cavity was verified again. Transabdominal ultrasound and laparoscopic-guided hysteroscopy using a needle electrode and micro-scissors were used to resect the asymmetrical uterine septum. During the first hysteroscopy, the septum between the communicating and blinded hemi-cavity was incised, and the incision was sustained to access the observed right endometrial cavity (Figure 5) and remove the pregnancy. We performed 3D ultrasound 2 weeks after surgery, which showed pregnancy tissue residue. We repeated the procedure with hysteroscopy with guidance by transabdominal ultrasound. After the second operation, remnant pregnancy tissue was completely removed and the two cavities were perfectly connected (Figure 5). A larger normal uterine cavity with bilateral tubal ostium was finally obtained. Postoperatively, the patient had 3D ultrasound performed at 3 months, which clearly showed that the uterine cavity shape was almost normal without intrauterine adhesions (Figure 2B). Moreover, the patient reported that menstruation ceased to be painful and there was no bloating at 12 months of follow-up.

Photograph of laparoscopy. The uterus is slightly enlarged on the right side, the external fundal shape is normal, and the right uterine surface shows endometriosis (black arrows)
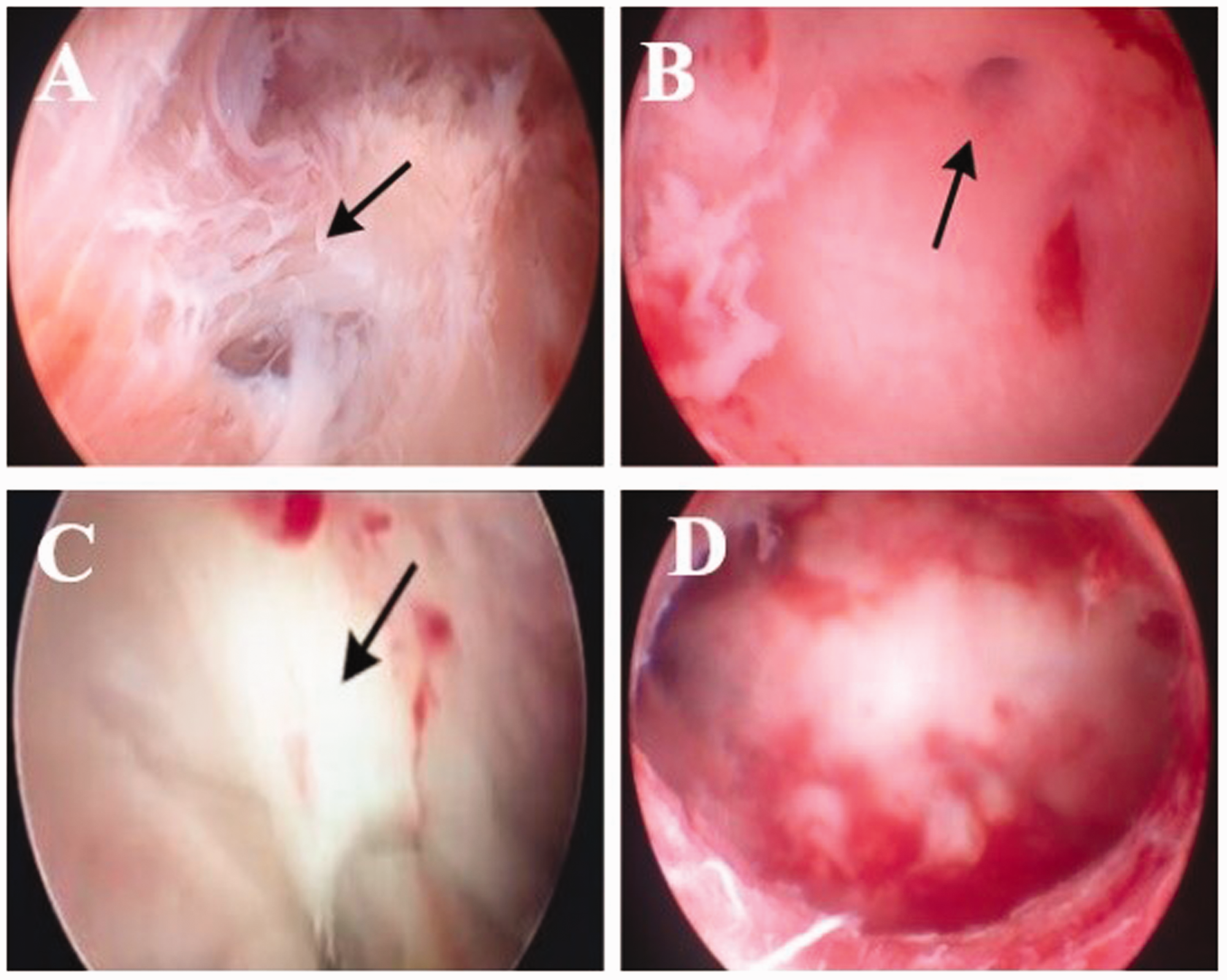
Images of hysteroscopy. (A) The right cavity has an asymmetrical uterine septum (black arrow). (B) In the left cavity, a left tubal ostium (black arrow) can be seen. (C) In the right cavity, there is pregnancy tissue (black arrow). (D) The two cavities were connected in the second operation
The study was approved by Fujian Provincial Maternity and Children’s Hospital, Affiliated Hospital of Fujian Medical University, Fuzhou, Fujian, China. Written informed consent was obtained from the patient for publication of this case report.
Discussion
Müllerian anomalies have been reported in 2% to 3% of women. 5 Robert’s uterus is an uncommon congenital Müllerian anomaly that was first described by Robert in 1970, and only a few cases have been reported.1,2 The characteristics of Robert’s uterus are as follows: (1) primary dysmenorrhea; (2) discordance between a normal laparoscopic appearance and a hysterographic appearance of an unicornuate uterus; and (3) the absence of anomalies of the urinary system. 9 One blind hemi-cavity with a functional endometrium causes menstrual retention, leading to unilateral hematometra, hematosalpinx, and endometriosis. These phenomena are associated with the severity of abdominal pain and dysmenorrhea.1,6 Non-communicating rudimentary horns are characterized by a blind cavity that does not appear to communicate with the fallopian tube. This leads to primary dysmenorrhea and abdominal pain with a progressive course. 6 In our patient, primary dysmenorrhea appeared without progression and pelvic endometriosis was identified by histology. This finding is probably due to a blind rudimentary uterine cavity being usually connected with the ipsilateral fallopian tube, which allows partial reflux of retained menstruation into the peritoneal cavity. 4 In contrast to the classical symptoms, other reported cases of Robert’s uterus occurred in patients who did not have any previous dysmenorrhea or other history related to hematometra. 7 This phenomenon can be considered to be associated with a progressive increase in the diameter of the distended blind cavity.
Robert’s uterus is an exceptionally rare variant of the complete septate uterus because of its asymmetry. Classification of Robert’s uterus is debatable. The European Society of Human Reproduction and the Embryology–European Society for Gynecological Endoscopy classification system describe Robert’s uterus as a rare anomaly under a complete septate uterus with unilateral cervical aplasia (class U2bC3V0), 8 without explaining the cause of unilateral cervical aplasia. 2 Therefore, Ludwin et al. 2 considered Robert’s uterus as class VB by the American Society of Reproductive Medicine classification and the basis of unilateral cervical aplasia may be segmental agenesis of the isthmus with a lack of reabsorption of the septum between upper regions of the Müllerian ducts. None of these classifications considered Robert’s uterus accompanied by urinary abnormalities. We experienced a case of Robert’s uterus with an ipsilateral renal anomaly that has not been previously reported in the literature. Our patient presented with different deformities to those in previous reports, 9 which presents further challenges to the classification and etiopathogenesis of Robert’s uterus. The urinary and reproductive systems generate from the same ureteric bud, which leads to Müllerian duct abnormalities at the same time as renal agenesis. 5 Therefore, patients with Robert’s uterus need to have the urinary system evaluated.
Pregnancy in the non-communicating blind cavity is another rare event, which suggests that transperitoneal migration of sperm or zygote, via the contralateral cavity and fallopian tube, probably occurred in our case. To date, only a few cases of pregnancy in the non-communicating blind cavity of Robert’s uterus have been reported. 4 Our patient was finally diagnosed because of recurrent failed attempts at terminating the fetus. If one blind cavity of Robert’s uterus could have been found in early pregnancy in our patient, laparotomy and metroplasty might have been able to be avoided. Previous cases of Robert’s uterus showed misdiagnosis, which led to treatment failure, including our patient who underwent the first failed operation, and other previous patients suffered multiple unsuccessful operations. 10 To the best of our knowledge, this is the first case of Robert’s uterus with pregnancy in the blind cavity in a patient who underwent a minimally invasive operation. Our findings suggested that timely and accurate diagnosis was important and allowed us to successfully perform minimally invasive surgery. Three-dimensional ultrasound and MRI are useful for evaluating Robert’s uterus.8,11 Additionally, 3D ultrasound is cost-effective for diagnosis, planning surgery, guidance for hysteroscopy, and in postoperative assessment.2,3 Modern ultrasound techniques are useful for evaluating pre- and postoperative uterine volume and shape.3,11 In addition to the diagnostic methods described above, salpingography can be used for Robert’s uterus.
The goals of treatment for obstructive uterine malformations are unification of both uterine cavities by incising the septum, which drains the hematometra by maintaining the integrity of both unified uterine cavities and the cervix. There are many methods of surgery for Robert’s uterus according to the individual, such as the patient’s condition and the surgeon’s skill. Hysteroscopy and laparoscopy combined with ultrasound guidance is a good method for treating Robert’s uterus. 12 Laparoscopy facilitates observation of the uterine fundal contour, while assisting diagnosis for uterine malformation and simultaneous treating abdominal and pelvic adhesions. Hysteroscopic electrotomy is an effective and minimally invasive technique, and with ultrasound guidance, it can be more accurate and safer. We performed hysteroscopic electrotomy with laparoscopic and transabdominal ultrasound guidance instead of performing hemi-hysterectomy. Our technique averts any adverse effects on ovarian blood supply and injury to the myometrium of the unicornuate uterus. This technique is also minimally invasive, associated with easier recovery after surgery, and has no uterine scarring, with less implications for future fertility, which is particularly important because many patients’ desire to become pregnant.8,13 In our case, laparoscopy assisted diagnosis and was used for treating superficial endometriosis, which was not discovered by ultrasound or MRI. However, after treatment of obstructive anomalies, endometriosis commonly resolves spontaneously without abdominal laparoscopic surgery. Kiyak et al. 14 reported that laparoscopic excision of a blind endometrial cavity was a safe and effective surgical alternative in patients who did not consent to hysteroscopic surgery because of their virgin state and religious beliefs. Ludwin et al. 2 proposed that hysteroscopic metroplasty with ultrasound guidance by experienced surgeons was safe for patients. This technique reduces the need for more invasive operations, such as laparoscopy or laparotomy, which might miss treating superficial endometriosis. Additionally, Robert’s uterus can be treated by laparotomy and noncommunicating rudimentary uterine resection or endometrectomy of the blind cavity, 6 as well as abdominal metroplasty. 1 After surgical excision of the uterine septum of Robert’s uterus, occurrence of intrauterine adhesion might need to be prevented. There are various methods to prevent intrauterine adhesion, including hyaluronic acid gel, estrogen therapy, an intrauterine balloon or device, and insertion of a balloon by using short repeated sequences. 15
Robert’s uterus can have an elusive diagnosis, but is able to be evaluated by 3D ultrasound and MRI. Such patients who are accompanied by ipsilateral renal agenesis must have evaluation of the urinary system by imaging. Prompt early diagnosis, as well as proper surgical treatment, are important for this condition. Hysteroscopic electrotomy under laparoscopic and/or) ultrasound guidance is an effective and minimally invasive therapy, and also further confirms uterine abnormalities. The skill and experience of gynecologists and sonographers are also important for identifying and managing unusual uterine malformations.
Footnotes
Declaration of conflicting interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
