Abstract
Objective
To compare modified expansive laminoplasty and fusion (MELF) with anterior cervical corpectomy and fusion (ACCF), and anterior cervical discectomy and fusion (ACDF), in treating four-level cervical spondylotic myelopathy (CSM).
Methods
This retrospective study included patients with four-level CSM who had undergone surgery at the Affiliated Hospital of Qingdao University between January 2013 and May 2015. D-values, Cobb’s angle, Japanese Orthopaedic Association (JOA) score and quality of life (SF-36 scores) were compared between patients treated with ACCF/ACDF versus MELF.
Results
Twenty-six patients who underwent ACCF/ACDF and 26 who underwent MELF were included, and all showed bone fusion following treatment. The most common complications were dysphasia (12/26) in the ACCF/ACDF group and axial neck pain (7/26) in the MELF group. C5 nerve root palsy was not observed in either group. D value and Cobb’s angle changes showed that ACDF/ACCF was more effective in curve correction than MELF. Postoperative improvements in JOA and SF-36 scores were noted in both groups, with no statistically significant between-group differences.
Conclusion
Anterior and posterior approaches may produce similar clinical outcomes in the surgical management of four-level CSM. MELF may avoid known complications of the posterior approach.
Keywords
Introduction
Cervical spondylotic myelopathy (CSM) is the most severe consequence of cervical intervertebral disk degeneration. 1 The onset of CSM is insidious and is observed at around 50–60 years of age.1–3 Based on the anatomical aetiology of CSM, surgical treatment may vary between anterior, posterior, or combined approaches to decompress the pathological area. The choice of approach depends on several factors including sagittal alignment, location and characterization of the compressive lesion, presence of preoperative symptoms, and longitudinal extent of the compression. 4 For single or two-level CSM, anterior cervical corpectomy and fusion (ACCF), anterior cervical discectomy and fusion (ACDF), or cervical disc replacement tend to be the first choice, except when a large osteophyte is identified. 5
For multi-level symptomatic CSM, controversy remains regarding the selection of surgical procedure. Historically, in cases involving a pathological area that extended for more than three vertebral segments, a posterior approach with laminoplasty or laminectomy was preferred over ACDF and/or ACCF. These posterior techniques, though avoiding the risk of pseudo-fusion, are known to have several prominent drawbacks such as higher frequency of C5 nerve root palsy, indirect decompression, limited correction, and postoperative pain. 6 Thus, the present authors developed an innovative, modified laminoplasty technique to minimize the risk of C5 motor root palsy.
The goal of the present study was to retrospectively compare the clinical effects of ACCF and ACDF with the novel laminoplasty technique with fusion for the treatment of four-level CSM.
Patients and methods
Study population and design
This retrospective study included patients with four-level CSM who had undergone surgery at the Department of Spine Surgery, Affiliated Hospital of Qingdao University, between January 2013 and May 2015, and who had at least 1 year of follow-up records. CSM was diagnosed according to previously published criteria. 1 The study inclusion criteria were: (1) diagnosis of CSM; (2) disc herniation at more than three levels; (3) had received ACDF, ACCF or modified expansive laminoplasty and fusion (MELF) treatment; and (4) had ≥1-year detailed follow-up. Patients with trauma as the aetiological factor for CSM were excluded.
The study protocol was approved by the Ethics Committees of the Affiliated Hospital of Qingdao University, and all participants provided written informed consent.
Criteria for selecting surgery type
All surgeries were performed by the same surgeon (XLC) who had 30 years of experience. All patients had straight or kyphotic cervical spine curvature, and all had undergone anteroposterior and lateral radiography, flexion-extension lateral radiography, computed tomography (CT), and magnetic resonance imaging (MRI). Indications for ACDF were as follows: straightened or reversed curvature of the cervical spine; soft tissues or discontinuous osteophytes as the main compressive factors; no development of severe canal stenosis; and numbness and weakness of four limbs combined with radiating pain on one side of the upper limb as the chief complaint. In cases that met the criteria for ACDF, but in which the osteophyte was considered too large and too long, ACCF would be selected as a safer decompression method. A posterior approach comprising MELF was selected when curvature of the cervical spine was appropriate and in the presence of continuous bone compression.
ACDF/ACCF
Following routine general anaesthesia, the patient was placed in the supine position with the head slightly tilted back. C-arm radiography (GE Healthcare, Wauwatosa, WI, USA) was used to localize the middle segment of the fusion level. The modified Smith-Robinson approach on the right side was used to perform anterior cervical exposure, as previously described.7,8 An avascular plane medial to the sternocleidomastoid muscle was identified and dissection was carried down to the anterior longitudinal ligament. Anterior distraction devices were placed and the discs or vertebral bodies were removed one by one to perform extensive decompression. Endplates were prepared for arthrodesis. A titanium fusion cage (DePuy Synthes, Raynham, MA, USA) was filled with allograft bone (DePuy Synthes) and inserted. A suitable titanium plate (DePuy Synthes) was fixed to the vertebral bodies. Four patients underwent ACDF/ACCF and one underwent subtotal vertebral body resection due to a large osteophyte. No autogenous iliac bone grafts were used. Fluoroscopy was employed to ensure adequate placement of the cage(s) and the plate in the mid-line, and to ensure that the length of the plate was not too long to affect the adjacent segments. The incision was closed using absorbable sutures. The prevertebral drain was removed at 24 h following surgery and patients were advised to wear a hard cervical collar for ≥3 months. Representative images are shown in Figure 1.

Representative cervical spine images from preoperative and postoperative X-ray, computed tomography, and magnetic resonance imaging in a patient with four-level cervical spondylotic myelopathy. The lesion levels were at C3/4, C5/6, and C6/7 with disc herniation and osteophyte, and C4/5 was normal (left-hand images). After four-level anterior cervical discectomy and fusion, the cervical curve was in normal physiological condition with complete decompression (right-hand images).
Modified expansive laminoplasty and fusion
Patients under routine general anaesthesia were placed in the prone position. A posterior midline approach was used. After clear exposure of the lamina and lateral mass joints, lateral mass screws (DePuy Synthes) were placed from C3–C6 and pedicle screws (DePuy Synthes) at C2, C7, and T1. A high-speed drill was used to create an innovative type of hinge-door laminotomy. The aim was to localize the hinge and door at the medial margin of the lateral mass joint and drill part of the medial margin of the lateral mass, widening the open-door area by an average of 25 mm (Figures 2 and 3). Laminoplasty could then be easily performed without the need to open the door much wider, reducing the risk of possible fracture at the hinge, which could possibly lead to nerve compression. Moreover, this technique allowed direct compression of the ipsilateral nerve root canal.
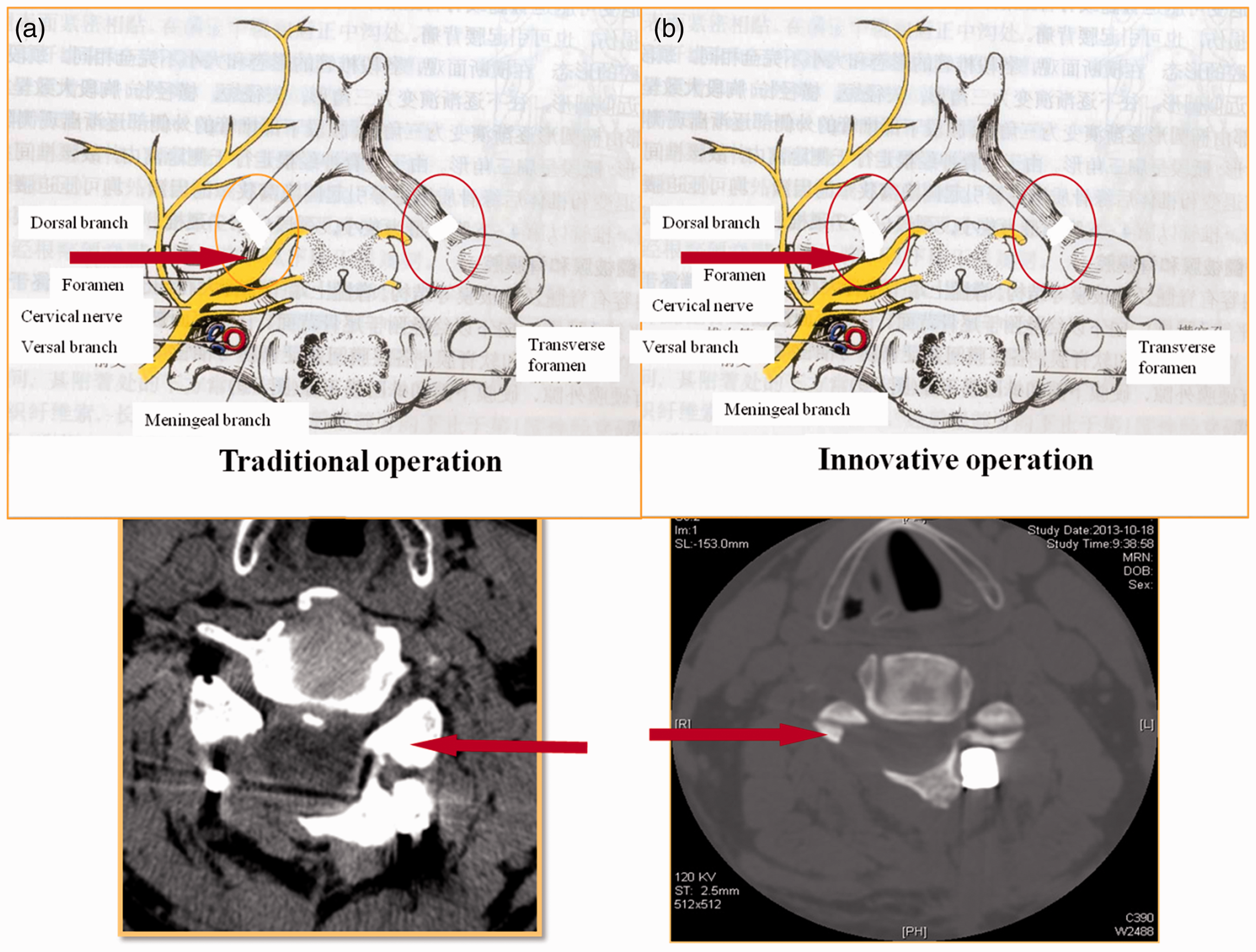
Representative images of posterior laminoplasty and fusion showing: (a) the traditional method with the hinge and door located at the lamina margin (red arrows). The residual integration of lamina and lateral mass will compress the nerve root; and (b) the modified method with the hinge and door at the medial margin of the lateral mass joint, at an average of 25 mm outward compared with the traditional approach (red arrows).
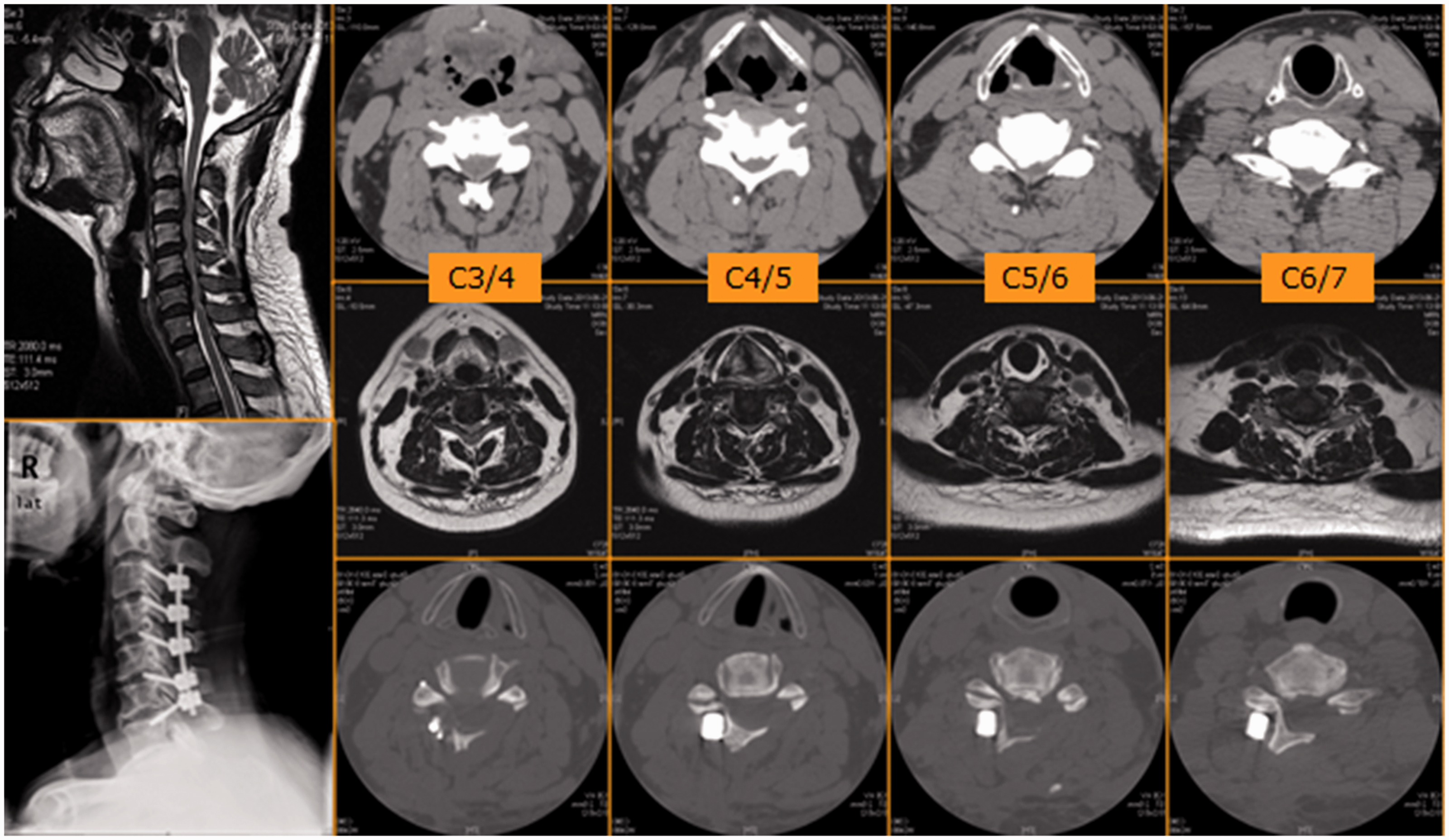
Representative case images of a 52-year-old male patient with numbness of the extremities and pain in the left arm for 3 months prior to treatment. The affected cervical levels were from C3 to C7, and the compressive cause was large osteophytes. Modified laminoplasty with fusion was selected to decompress the spinal cord.
Data collection
The treating surgeon and the radiologist recorded the D value and Cobb’s angle, as previously described,9,10 preoperatively, at 1 week, 3 months and 6 months postoperatively, and at the final follow-up. D value was defined as the vertical distance between the inferior posterior margin of C4 to the connection line from the odontoid posterior margin to the inferior posterior margin of C7. Cobb’s angle was defined as the angle between the upper margin of the head-end vertebral body and the lower margin of the tail-end vertebral body within the fusion segment. Japanese Orthopaedic Association (JOA) score and quality of life (QoL; assessed using the 36-Item Short Form Health Survey [SF-36]) were evaluated preoperatively, at 1 week following surgery and at the final follow-up. Flexion and extension lateral radiography and/or CT scan were performed to determine bone fusion at 3 and 6 months, and at the final follow-up. In order to eliminate observer bias, all data were independently analysed by two experienced radiologists who were blinded to the treatment.
Statistical analyses
Statistical analyses were performed using SPSS software, version 16.0 (IBM, Armonk, NY, USA). Continuous data are presented as mean (range) or mean ± SD and between-group differences were analysed using Student’s t-test. Categorical data are presented as n prevalence and between-group differences were analysed using χ2-test. Two-sided P-values <0.05 were considered statistically significant.
Results
Patient demographic and clinical characteristics
Out of 64 patients who were initially identified as diagnosed with four-level CSM, a total of 52 patients met all of the study inclusion criteria, comprising the anterior treatment group (ACDF/ACCF; n = 26) and posterior treatment group (MELF; n = 26). In the anterior group, mean patient age was 54.2 years (range, 46–74 years), with 14 male and 12 female patients, and mean symptom duration was 11.7 months (range, 6–37 months). MRI analysis revealed 23 patients with C3–C7 lesions and three patients with C4–T1 cervical cord compression. There were 20 cases of myelopathy and six cases of myelopathy mixed with radiculopathy. In the posterior group, mean patient age was 56.7 years (range, 47–76 years), with 16 male and 10 female patients. Mean duration of symptoms was 11.1 months (range, 5–35 months). Clinical examination showed 21 patients with C3–C7 lesions and five patients with C2–C6 cervical cord compression. Thus, vertebrae were fused at C3–C7 or C2–C6. No statistically significant between-group differences were observed in terms of age, sex, mean duration of symptoms, duration of surgery or follow-up period (Table 1).
Demographic and clinical characteristics of patients with four-level cervical spondylotic myelopathy.

Data presented as n prevalence or mean (range).
ACDF, anterior cervical discectomy and fusion; ACCF, anterior cervical corpectomy and fusion; MELF, modified expansive laminoplasty and fusion.
NS, no statistically significant between-group difference (P > 0.05; Student’s t-test or χ2-test).
Surgery characteristics
In the anterior group, 22 patients underwent ACDF and four patients underwent ACDF plus ACCF. Mean duration of surgery was 145 min (range, 125–185 min) and mean blood loss was 45 ml (range, 10–150 ml). In the posterior group, innovative modified laminoplasty with fusion was performed in all patients in the posterior group, with a mean surgery duration of 131 min (range, 95–150 min) and mean blood loss of 160 ml (range, 100–800 ml; P < 0.05 versus anterior group; Table 1).
Follow-up
Mean follow-up for the anterior group was 15.6 months (range, 13–37 months; Table 1). Bone fusion was observed in all patients in this group at 6 months following surgery, shown by post-operative three-dimensional reconstructive CT. At a 36-month follow-up assessment for one patient, radiography revealed the titanium mesh to have mild subsidence without displacement of plate and screws. Mean follow-up in the posterior group was 16.2 months (range, 12–40 months; Table 1). All patients in this group displayed solid bony fusion of the hinge side at 3 months following surgery.
Complications
Complications associated with surgical treatment are summarised in Table 2. The most common complication associated with the anterior approach was dysphagia (12/26), and the most common complication associated with the modified posterior approach was axial neck pain (7/26). C5 nerve root palsy was not observed in either group.
Complications associated with anterior and posterior surgical approaches in patients with four-level cervical spondylotic myelopathy.

Data presented as n prevalence.
Outcomes
Changes in D value and Cobb’s angle showed that ACDF/ACCF was more effective in curve correction than MELF (P < 0.05; Table 3). Postoperative improvements in JOA and SF-36 scores were noted in both groups, with no statistically significant between-group differences (P > 0.05; Table 4).
Radiographic changes in D values and Cobb’s angles between anterior and posterior surgical approaches in patients with four-level cervical spondylotic myelopathy.

Data presented as mean ± SD.
P < 0.05, statistically significant between-group differences (Student’s t-test).
Comparison of preoperative and postoperative Japanese Orthopaedic Association (JOA) and 36-Item Short Form Health Survey (SF-36) scores between anterior and posterior surgical approaches in patients with four-level cervical spondylotic myelopathy

Data presented as mean ± SD.
NS, no statistically significant between-group differences (P > 0.05; Student’s t-test).
Discussion
In general, surgical management for CSM tends to have better prognosis than surgery for thoracic or lumbar degenerative disease, regardless of the number of levels involved, or whether anterior or posterior approaches were used. 11 Nevertheless, posterior surgical approaches for CSM are associated with drawbacks such as the risk of C5 nerve root palsy. 6 An innovative posterior approach was therefore designed in an attempt to improve outcomes and risks. The results of the present retrospective study suggest that for the surgical management of four-level CSM, both anterior and posterior approaches may result in similar clinical outcomes, but fewer complications may be associated with the modified posterior approach.
Anterior approaches have been rarely applied in the past due to disadvantages such as lower fusion rates and higher rates of adjacent segment degeneration following long segment fixation, dysphasia and dysphagia, and poor cosmetic results from the required large oblique straight incision on the anterior aspect of the neck. 12 However, the effects of ACDF or hybrid techniques in treating multilevel cervical spondylosis have been verified experimentally and clinically. 13 To improve fusion rates, attention has been given to dealing with the superior and inferior vertebral endplates, and processed allografts are widely used to replace autogenous iliac bone grafts. Due to economic constraints (such as medical insurance), however, bone morphogenic proteins are not a readily available treatment option.
In the present study, patients in the anterior group showed solid fusion at approximately 6 months following surgery, suggesting that a hard-cervical collar should be worn for longer than 3 months in this patient population. ACDF is an effective surgical procedure that has been widely used to replace ACCF to restore the physiological curve and improve fusion rates. 14 Nevertheless, if the compressive lesions are large osteophytes and localized ossification of the posterior longitudinal ligament, ACCF may be necessary. 15 Wang et al. 16 commented that ACDF using a stand-alone anchored cage showed similar clinical results to laminectomy with fusion for the treatment of four-level CSM, with better lordosis correction and less blood loss, however, ACDF was associated with increased loss of lordosis and a higher rate of non-unions following surgery.
Dysphagia, defined as solid or dry food getting stuck in the process of swallowing due to constant traction on the trachea and oesophagus, is a common complication associated with the anterior approach, and is common in four-level CSM. 17 In the present study, there were twelve cases of dysphagia in the anterior group and one in the posterior group.
Laminectomy and laminoplasty with or without fusion allows relatively safe decompression and avoids complications such as cerebrospinal fluid leak.18,19 Nevertheless, these surgical techniques have been associated with axial neck pain, C5 nerve root palsy, and significant trauma to the paraspinal muscles and ligaments. 20 Palsy of the C5 nerve root is an obvious potential complication of laminoplasty with reported rates of 0–30%.21,22 In patients with cervical canal stenosis combined with myelopathy or continuous ossification of the posterior longitudinal ligament, laminectomy and laminoplasty with or without fusion provides adequate decompression and prevents progressive neurological deterioration. In the present study, the cervical anatomy was analysed and the surgical laminoplasty technique was modified, resulting in no postoperative C5 nerve root palsy. From the present results, it can be surmised that locating the ‘door’ at an average of 25 mm outward compared with the traditional approach allows adequate decompression of both the nerve root and spinal cord. The authors conclude that C5 nerve root palsy was not observed in the present series as a result of the modified approach.
In general, laminoplasty without fusion results in clinical improvement, although it is usually accompanied by loss of cervical lordosis in cases of CSM with osteophytes or ossification of the posterior longitudinal ligament, which may worsen after surgery. Cervical laminoplasty for ossification of the posterior longitudinal ligament may improve radiculo-myelopathy, but it has been demonstrated to increase the probability of cervical kyphotic alignment.23,24 A previous study showed that range of motion of the cervical spine decreased by 30.5% following laminoplasty, and kyphosis developed in 10.6% of the patients. 25 In the present study, all patients who underwent the posterior approach had straight or kyphotic cervical curvature, which would have been the main reason for axial neck pain.
The results of the present study are limited by a number of factors. First, there is a selection bias that is inherent to the retrospective nature of the study. Secondly, the study is limited by the relatively small number of patients, however, the prevalence of patients with four-level CSM requiring surgery is generally low and the involved surgeon selects the procedure of choice. Thirdly, all surgeries in the present series were performed by a single surgeon at a single centre, and this may affect the generalisability of the results. A prospective, multicentre, randomized study would be ideal to validate the present results. The authors would like to note that postoperative axial neck pain was observed in some patients from both study groups, and this may require additional research.
In conclusion, for the surgical management of four-level CSM, both anterior and posterior approaches allow for similar clinical outcomes. When a posterior approach is considered, the innovative modified laminoplasty with fusion technique described herein may avoid C5 root palsy, one of the most common complications of the posterior approach. The described surgical approach to the present series may provide surgeons with an alternative technique to traditional laminoplasty and fusion technique for multilevel CSM, which may preclude C5 nerve root palsy.
Footnotes
Acknowledgment
The authors are indebted to the Imaging Department of the Affiliated Hospital of Qingdao University for data collection and analysis.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
