Abstract
Objective
To investigate the effectiveness of high-dose glucocorticoids on hemolysis, elevating liver enzymes, and reducing platelets (HELLP) syndrome.
Methods
A total of 151 patients with HELLP syndrome were analyzed and divided into two groups. Six subgroups of treatment and control groups were divided into three grades in accordance with the American Mississippi Diagnostic Criteria.
Results
There were no differences in general characteristics of the patients, primipara rate, minimum platelet recovery time, postpartum hemorrhage volume, postpartum hemorrhage rate, cumulative average of maternal damage, intensive care unit admission rate, perinatal mortality rate, and overall incidence rate of adverse outcomes in fetuses among the groups. The primipara rate in the control group of the third grade was significantly higher than that in the treatment group of the third grade. The treatment group of the second grade (88.7%) had a significantly higher preterm delivery rate than that in the control group of the second grade (66.7%). There were no differences in minimum hemoglobin, and maximum lactate dehydrogenase, alanine aminotransferase, and aspartate aminotransferase levels among the groups and subgroups.
Conclusion
High-dose glucocorticoids cannot significantly improve maternal and fetal prognoses and laboratory indices. However, our results might offer some clinical evidence for HELLP syndrome therapy.
Keywords
Introduction
Hemolysis, elevating liver enzymes, and reducing platelets (HELLP) syndrome is a severe obstetric problem. HELLP syndrome has the main characteristics of hemolysis and increased hepatic enzymes and thrombocytopenia, and is often complicated by gestational hypertension, which poses a threat to the gravida and fetus. The incidence rate of HELLP syndrome is 0.17% to 0.85% during delivery and the mortality rates of gravidas and fetuses/neonates reach up to 23.1% and 56.9%, respectively. 1 There are no effective protective measures for HELLP syndrome because of the unknown precise pathogenesis. Currently, the main treatment for HELLP syndrome is symptomatic treatment. This treatment includes regular spasmolysis and lowering blood pressure, use of glucocorticoids to treat the patient’s condition and promote fetal lung maturation, proper addition of blood products, rectification of coagulation disorders, and close monitoring of the patient’s condition. Furthermore, evaluation of the fetus’s condition in the uterus and timely termination of pregnancy are performed in HELLP syndrome.2,3 Among them, glucocorticoids play a vital role in treating HELLP syndrome, but this treatment has been controversial in the past 20 years. Some studies have shown that high-dose hormonotherapy is effective for alleviating the maternal and fetal prognoses and accelerating postnatal recovery. 4 However, other random clinical experiments have not found that high-dose hormonotherapy is effective in maternal and fetal prognoses and accelerating postnatal recovery. 5 Furthermore, the long-term treatment effectiveness of high-dose hormonotherapy is unknown. Therefore, control studies are required to further ensure the effectiveness and safety of hormones in HELLP syndrome.
In this study, we aimed to investigate the effectiveness of high-dose glucocorticoids on HELLP syndrome to provide clinical evidence for hormone therapy in HELLP syndrome.
Materials and methods
Patients
Patients with HELLP syndrome who were admitted to our hospital (Affiliated Suzhou Hospital, Nanking Medical University) from December 2013 to August 2018 were selected. The selection and grading standards that were used were in accordance with the American Mississippi Diagnostic Criteria. 6 Exclusion criteria were as follows: patients who were using steroid hormones for a long time; patients with other hepatic dysfunction-induced complications; and patients with other thrombocytopenia-induced complications. For high-dose glucocorticoid treatment, methylprednisolone was administered intravenously by an infusion of 80 to 120 mg/day for a total of 3 to 7 days. The patients were divided into two groups as follows: the treatment group (89 patients) and the control group (62 patients). Six subgroups were classified in accordance with the American Mississippi Diagnostic Criteria: 7 treatment group of first grade (22 patients), control group of first grade (13 patients), treatment group of second grade (61 patients), control group of second grade (45 patients), treatment group of third grade (5 patients), and control group of third grade (4 patients). Patients who had premature birth and used normal-dose dexamethasone to promote fetal lung maturation were not excluded. However, these patients needed to have an interval exceeding 24 hours between dexamethasone to promote fetal lung maturation and the first dose of high-dose glucocorticoid in the early period of treatment.
Ethical approval was obtained from the Ethics Committee of Suzhou Affiliated Hospital of Nanjing Medical University. All participants signed a consent form before the study.
Treatment
All of the patients were admitted to high-risk wards. Their vital signs and fetal intrauterine conditions were monitored, their laboratory indices were dynamically observed, and their treatment plan was adjusted according to their conditions. Magnesium sulfate was provided for spamolysis until 48 hours postnatally. Labetalol or nifedipine was used for lowering blood pressure when blood pressure was 140 to 150/90 to 100 mmHg. Glutathione was used for hepatoprotection when transaminase levels were too high and albumin was used to rectify hypoproteinemia. An erythrocyte suspension or fresh frozen plasma was transfused when necessary to complement blood volume and improve coagulation function. Diuresis was properly managed and pregnancy was terminated in accordance with the maternal and fetal conditions. Dexamethasone 10 mg/day for 2 days was intravenously injected into the preterm patient before delivery to promote fetal lung maturation. Methylprednisolone 80 to 120 mg/day for 3 to 7 days was intravenously provided to patients in the treatment group and its dose was gradually decreased after postnatal indicators improved. Measures were taken to prevent all types of complications. Consultation of doctors in the Neonatal Department was established before terminating pregnancy. The neonate was immediately transferred to the neonatal intensive care unit (ICU) after birth to continue treatment.
Observed indices
Differences in relative indices between the two groups were recorded and compared, and differences among different subgroups were further compared. Indices included the following. 1) General characteristics, such as age, primipara rate, cesarean section rate, gestational weeks of admission, gestational weeks of termination, and hospitalization time, were recorded. 2) Maternal and fetal prognoses included the minimum platelet recovery time, postpartum hemorrhage volume, postpartum hemorrhage rate, cumulative average of maternal damage (including vital organ failure, eclampsia, placental abruption, disseminated intravascular coagulation, and subhyaloid hemorrhage), ICU admission rate, preterm delivery rate, perinatal mortality rate, and overall incidence rate of adverse outcomes in fetuses (including fetal distress, asphyxia neonatorum, and perinatal death). 3) Use of blood products was recorded, including suspended red blood cells, where these cells were suspended in isotonic saline to obtain a mixture of 2% (v/v) red blood cell suspension, plasma, albumin, and platelets. 4) Main laboratory indices at the disease peak included the minimum hemoglobin value, minimum blood platelet count (BPC) value, and maximum lactate dehydrogenase (LDH), alanine aminotransferase (ALT), and aspartate aminotransferase (AST) values. 5) Improvement of laboratory indices included increased BPC values and decreased LDH, ALT, and AST values.
Statistical analysis
SPSS Statistics for Windows, Version 17.0 (Chicago, IL, USA) was used for statistical analysis. Measurement data are shown as mean ± standard deviation. The t-test was used to compare measurement data. The χ2 test was used to compare enumeration data. Values of P < 0.05 indicate statistical significance.
Results
General characteristics
We studied a total of 151 patients with HELLP syndrome. There were no significant differences in the mean age, cesarean section rate, gestational weeks of admission, and gestational weeks of termination among the groups and subgroups (Table 1). The primipara rate in the control group of third grade (four primiparas) was significantly higher than that in the treatment group of third grade (P < 0.05). The primipara rate was not significantly different between the treatment and control groups, as well as between first and second grade subgroups. General characteristics between both groups and among all subgroups were mostly similar.
Comparison of general characteristics of the patients.

*P < 0.05.
Comparison of maternal and fetal prognoses in different groups
The mean hospitalization time was not significantly different between the treatment and control groups, and among the subgroups (Table 1). The minimum platelet recovery time, postpartum hemorrhage volume, postpartum hemorrhage rate, cumulative average of maternal damage, ICU admission rate, perinatal mortality rate, and overall incidence rate of adverse outcomes in fetuses were not significantly different between the treatment and control groups. The preterm delivery rate was significantly higher in the treatment group of second grade than in the control group of second grade (P < 0.05). There were no significant differences in the preterm delivery rate between the treatment and control groups, and among the other subgroups (Table 2).
Comparison of maternal and fetal prognoses.

*P < 0.05. ICU: intensive care unit.
Comparison of blood product use
Use of MAP and albumin was not significantly different between both groups and among all subgroups. None of the 151 patients had transfusion of platelets. Mean plasma use in the treatment group was significantly higher than that in the control group (P < 0.05). Mean plasma use was not significantly different among the subgroups (Table 3).
Comparison of blood product use.

*P < 0.05.
Comparison of main laboratory indices at the disease peak
Minimum hemoglobin and maximum LDH, ALT, and AST levels were not significantly different between the two groups and among all subgroups. The severity of illness between the two groups and among all subgroups was comparable (Figure 1).
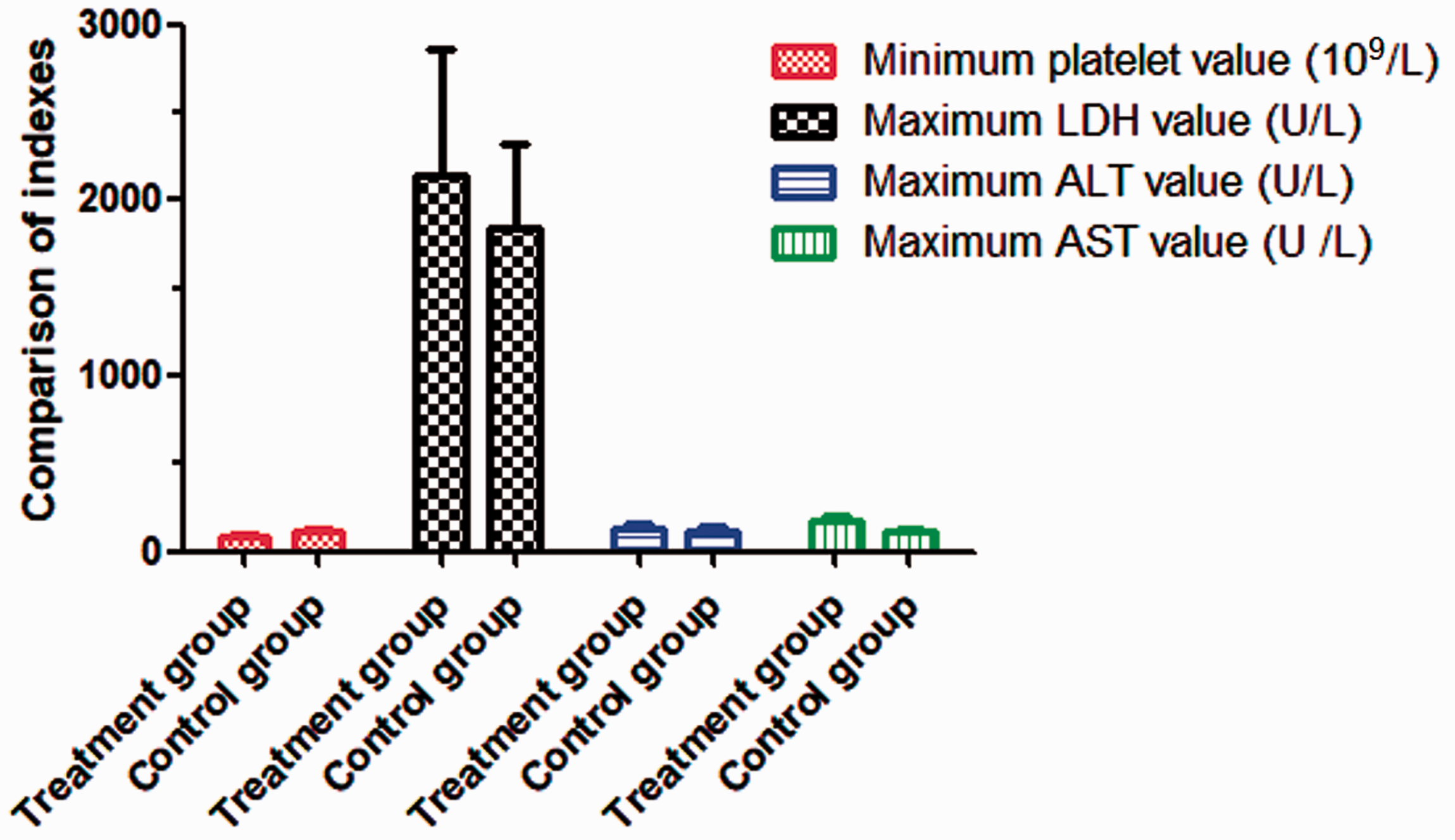
Comparison of main laboratory indices at the disease peak.
Comparison of recovery of main laboratory indices
BPC values and LDH, ALT, and AST values in the recovery period were not significantly different between the two groups and among all subgroups (Table 4).
Comparison of recovery of the main laboratory indicators.

LDH: lactate dehydrogenase; ALT: alanine aminotransferase; AST: aspartate aminotransferase.
Discussion
HELLP syndrome is a serious complication in the gestational period. This can lead to severe maternal complications, such as placental abruption, disseminated intravascular coagulation, acute kidney failure, pulmonary edema, and subcapsular hemorrhage of the liver. HELLP syndrome can also can lead to fetal complications of fetal growth restriction and premature birth, affecting maternal and fetal prognoses. This syndrome can ultimately lead to maternal and fetal death. 8 Many scholars believe that HELLP syndrome is a complication of preeclampsia, but some argue that it is a dependent disease. Researchers have found that heredity, immunity, inflammation, metabolism, and blood coagulation have close relations with HELLP syndrome.8,9 Many factors are intertwined and interact with each other, causing HELLP syndrome. The actual cause of HELLP syndrome is unknown and there is no targeted intervention for its pathogenesis. Once this syndrome occurs, it is fatal. Therefore, timely diagnosis and qualified treatment are important.
There is no specificity of HELLP syndrome, and thus its diagnosis mainly depends on laboratory examinations. There are two diagnostic standards for HELLP syndrome, as follows: the Tennessee diagnostic standard 10 and Mississippi diagnostic standard. 6 Treatment of HELLP syndrome includes many aspects. Once this syndrome is finally diagnosed, qualified obstetric management should be provided and more attention should be paid to monitoring of laboratory indices. Common evaluations are performed in the fields of obstetrics, critical care medicine, anesthesiology, neonatology, general medicine, neurology, and nephrology.4,11 The treatments of spasmolysis, lowering blood pressure, glucocorticoids, and blood products (including plasma exchange) are flexibly used, and termination of pregnancy is used to prevent progress of this disease.
Glucocorticoids have an important role in treating HELLP syndrome. Glucocorticoids not only can promote fetal lung maturation and prevent hyaline membrane disease, but they also can improve maternal laboratory indices, especially BPC values. However, in the past 20 years, glucocorticoid treatment, especially high-dose glucocorticoids, has been controversial. The main mechanism of glucocorticoid treatment is alleviating dropsy, inhibiting endothelial activation, reducing vascular endothelial injury, increasing hepatic blood flow, preventing thrombotic microvascular hemolysis, and reducing platelet consumption. Some studies have shown that glucocorticoids can significantly improve BPC, LDH, ALT, and AST levels, blood pressure, and urinary volume. The lower primary BPC is, the more significant improvement is after glucocorticoid treatment. 2 However, some scholars argue that glucocorticoids do not change maternal and fetal prognoses, and the mortality and complication incidence rates do not change with glucocorticoid treatment. Additionally, the long-term effectiveness of glucocorticoid treatment is unknown. Fetal growth and development indicators are unknown and high-dose glucocorticoids may lead to inhibition of the adrenal axis and postpartum depression.12,13 To date, there have been insufficient large-sample, randomized, controlled studies to support regular glucocorticoids to treat HELLP syndrome. Because glucocorticoid treatment can increase BPC levels, there is the belief that that it can be clinically applied.
This study was a retrospective analysis of high-dose glucocorticoid treatment for treating HELLP syndrome. Clinical information of 151 patients with HELLP syndrome was compared to analyze the role of high-dose glucocorticoid in improving maternal and fetal prognoses and laboratory indices. We found that general characteristics and disease progress, postpartum hemorrhage volume, postpartum hemorrhage rate, cumulative average of maternal damage, ICU admission rate, perinatal mortality rate, and overall incidence rate of adverse outcomes in fetuses were similar in the treatment and control groups. These findings suggest that high-dose glucocorticoids do not significantly improve maternal and fetal prognoses. Furthermore, high-dose glucocorticoids could not reduce use of blood products. These findings are consistent with previous reports. 5 In our study, improvement of hemoglobin, BPC, LDH, ALT, and AST levels in the treatment group was the same as that in the control group. This finding suggests that high-dose glucocorticoids do not significantly improve laboratory indices. This finding is not consistent with previous reports. 4 However, our study was a retrospective analysis, and not a randomized, controlled trail, with low verification efficiency. Furthermore, the number of enrolled patients in our study was insufficient. Therefore, large, controlled studies are required in the future to ensure the efficiency and safety of high-dose hormones.
In summary, we investigated the role of high-dose glucocorticoids in treating HELLP syndrome. Although high-dose glucocorticoids cannot significantly improve maternal and fetal prognoses and laboratory indices, our findings can offer some clinical evidence for treating HELLP syndrome. In the future, more patients should be enrolled in clinical, randomized, controlled trails, which are more scientific and robust to investigate this problem.
Footnotes
Consent for publication
All data concerning personal information have been allowed for publication by all participants.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
Our study was supported by the Suzhou People’s Well-being Project in China (grant number: SS201710), the Suzhou Maternity Disease of Clinical Center Project, China (grant number: SZZX201605), and the Suzhou Introduction of Clinical Expert Team Project, China (grant number: SZYJTD201709).
