Abstract
Metastases to the skull or upper cervical spine from hepatocellular carcinoma (HCC) are very rare. We herein report a unique case of two-site surgery for both skull and upper cervical spine metastases from HCC. The patient was a 64-year-old man with cervical pain. Computed tomography (CT) revealed osteolytic change related to metastatic cervical spine and occipital bone tumors. Two-stage surgery involving posterior occipitocervical fusion and occipital bone tumor resection was performed. The patient’s pain decreased in severity, and postoperative radiotherapy and chemotherapy could be conducted. The postoperative course was favorable, and the patient exhibited improvement in his activities of daily living. Neither cervical spine X-ray examination nor CT showed any instrumentation failure, such as screw loosening, before the patient died of liver failure 13 months after surgery. Patients with both skull and upper cervical spine metastases from liver cancer may have a markedly unfavorable prognosis. Even in these patients, however, surgery as an aggressive palliative treatment may prolong the survival period or maintain the quality of life as long as the patient’s general condition permits.
Keywords
Introduction
Bone metastasis from hepatocellular carcinoma (HCC) accounts for 1.6% to 16.0% of metastatic lesions, and this percentage is the second highest following lung metastasis.1,2 In contrast, skull or upper cervical spine metastases from HCC are very rare.3–6 To our knowledge, no previous case of both skull and upper cervical spine metastases from HCC has been reported in the English-language literature. The prognosis of patients with spine or skull metastases from HCC remains unfavorable.5,7,8 Metastatic bone lesions are evaluated as multiple spine metastases in many cases, and the prognosis is poor after bone metastasis has occurred. Therefore, surgery is indicated for a limited number of patients as long as the patient’s general condition permits, and radiotherapy is performed to relieve pain for many patients. This is the first report of two-site surgery for both skull and upper cervical spine metastases from HCC. We herein describe a patient who underwent two-stage surgery for posterior occipitocervical fusion and occipital bone tumor resection and showed a favorable course. This case is being reported to alert clinicians that aggressive palliative surgery can be beneficial even for patients with a poor prognosis due to both skull and upper cervical spine metastases from liver cancer.
Case report
This study was approved by the Nihon University Institutional Review Board and was conducted in conformity with ethical and humane principles of research. Written informed consent was obtained from the patient before treatment. The patient was a 64-year-old man with cervical pain. The cervical pain first appeared in April 2016, and he was referred to our department. His medical history included endoscopic variceal ligation for an esophageal varix and S8 segmentectomy/cholecystectomy for HCC in 2013 as well as transcatheter arterial chemoembolization (TACE) for recurrent liver cancer (intrahepatic recurrence) in 2014. Sacral metastasis was subsequently detected, and local radiotherapy (40 Gy/20 Fx) was performed. In 2015, TACE for intrahepatic recurrence was conducted three times.
At the initial consultation in our department, marked pain related to cervical movement was present, but examination revealed no abnormal neurological findings such as muscle weakness of the limbs or sensory disturbance. Computed tomography (CT) revealed osteolytic change related to metastatic cervical spine and occipital bone tumors (Figures 1(a) and 2(c), (d)). Contrast-enhanced magnetic resonance imaging (MRI) of the cervical spine showed tumor-related signal intensity changes in the right lateral mass of the atlas and C5/C6 vertebral bodies. However, no spinal cord compression was present (Figure 1(b), (c)). Head MRI revealed a tumor mass in the occipital region, with high signal intensity on T1-weighted images and low signal intensity on T2-weighted images (Figure 2(a), (b)). Based on these findings, a diagnosis of cervical spine and skull metastases from HCC was made. The revised Tokuhashi score 9 was 6 points, corresponding to a life expectancy of ≤6 months.

Preoperative computed tomography findings. (a) Coronal and (b) axial views showed osteolytic change in the right lateral mass of the atlas. (c) Three-dimensional head computed tomography showed osteolytic change in the occipital bone.
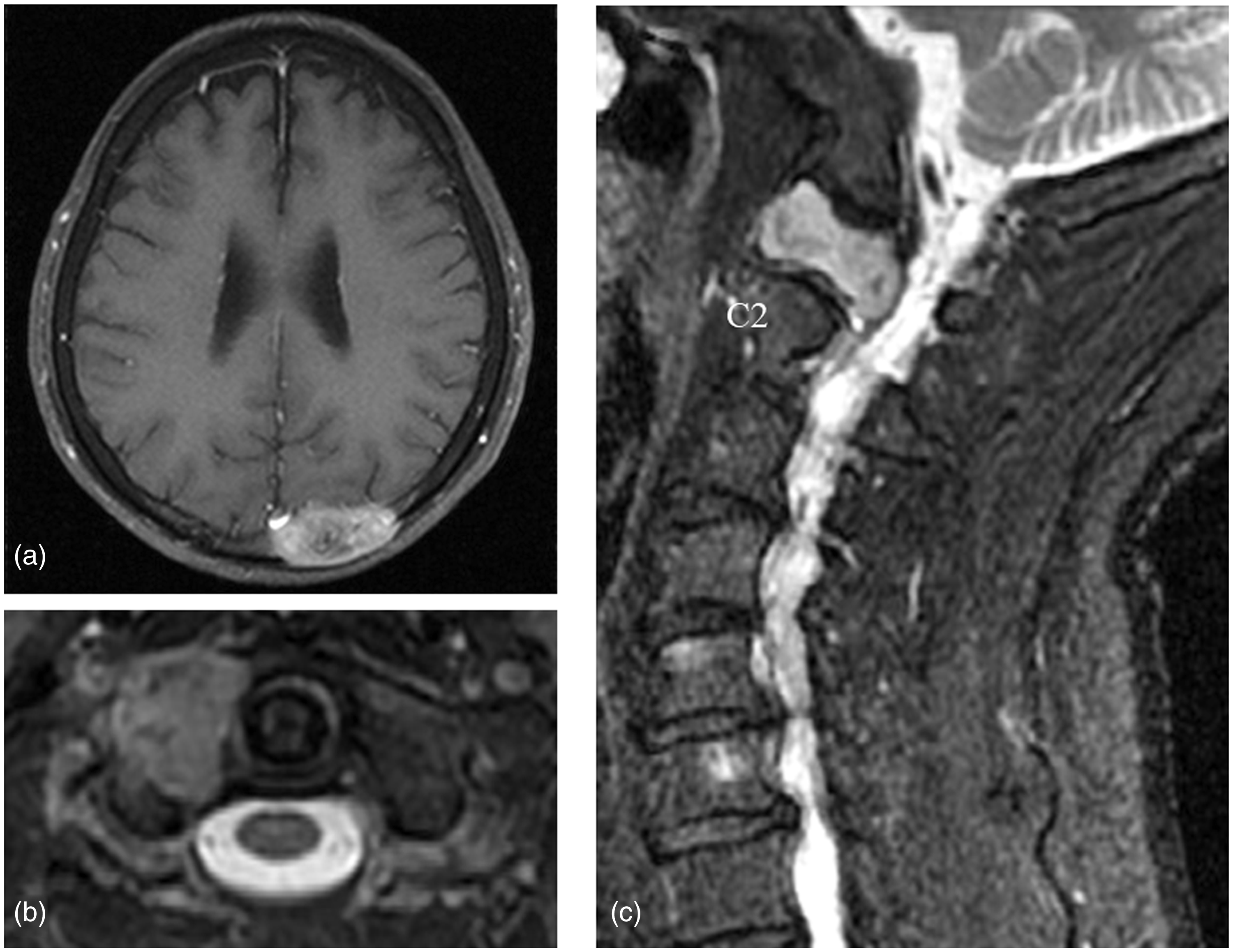
Preoperative magnetic resonance imaging (MRI) findings. (a) T1-weighted MRI of the head showed tumor mass-related compression of the cerebral parenchyma. (b) Axial and (c) parasagittal views of contrast-enhanced MRI of the cervical spine showed tumor-related signal intensity changes in the right lateral mass of the atlas and C5/C6 vertebral bodies. However, no spinal cord compression was present.
Surgery was performed to relieve the pain related to the cervical instability, improve the patient’s activities of daily living (ADL), and achieve local tumor control. Initially, posterior occipitocervical fusion was performed. An occipital bone plate was placed, and a pedicle screw was inserted into the second cervical vertebra. Lateral mass screws were inserted into the third and fourth cervical vertebrae and connected/fixed with rods (Figure 3(a), 3(b)). Tumor curettage of the right lateral mass of the atlas was not performed. Two weeks later, occipital bone tumor resection was performed by neurosurgeons. The craniotomy was performed by incising the periosteum and bone in a circular shape, and the pachymeninx and tumor were exfoliated. The tumor involving the bone and periosteum was then resected. Bone cement was placed at the site of the bone defect and fixed with silk thread (Figure 3(c), (d)).

Postoperative plain radiographs of the cervical spine. (a) Anteroposterior view. (b) Lateral view.
Local radiotherapy for the metastatic cervical spinal tumor was performed 2 weeks after the occipital bone tumor resection (30 Gy/15 Fx). Furthermore, TACE was conducted to treat intrahepatic recurrence. Denosumab was subcutaneously injected every 4 weeks. Neither cervical spinal X-ray examination nor CT showed any instrumentation failure, such as screw loosening (Figure 4), before the patient died of liver failure 13 months after surgery. Furthermore, the patient had no neck pain, local recurrence derived from cervical spinal/skull tumors, or pain-related disturbances in his ADL.

Postoperative head computed tomography findings. (a) Axial view. (b) Sagittal view. (c) A three-dimensional image showed that the bone defect site was filled with artificial bone (arrow).
Discussion
The incidence of HCC varies among geographical regions. The highest rates are found in Asia, especially Taiwan, Korea, China, and Japan. 10 Advances in surgical techniques and TACE have prolonged the survival period of patients with HCC. 11 However, the number of patients with epidural spinal cord compression related to spinal metastases from HCC has increased despite control of the primary tumor. 12
The incidence of lung metastasis is highest among all types of remote metastases from HCC, and the incidence of bone metastasis is second highest. Bone metastasis accounts for 1.6% to 16.0% of metastatic lesions.1,2 The most frequent site is the spine, followed by the iliac bone and rib. However, skull or upper cervical spine metastases, as detected in the present case, are very rare.3–6 To our knowledge, no previous case of both skull and upper cervical spine metastases from HCC has been reported in the English-language literature. This is the first report of two-site surgery for both skull and upper cervical spine metastases from HCC.
Cervical spine metastasis causes pain or paralysis, reducing the patient’s quality of life (QOL).1,2 The most frequent symptom related to skull metastasis is a subcutaneous mass, which is occasionally painful, followed by cranial nerve deficits, headache, and limb weakness. 5 A recent study revealed the usefulness of positron emission tomography–CT (PET-CT) for the diagnosis of extrahepatic metastasis, especially osteolytic metastatic bone leisions. 13 In the present case, cervical spine and skull metastases were detected during detailed examination of the patient’s cervical pain. Early diagnosis of bone metastasis using PET-CT is necessary during postoperative follow-up of HCC. If spinal metastasis is detected, the possibility of skull metastasis should be considered.
One study revealed the presence of advanced extrahepatic metastases at the time of bone metastasis diagnosis in most patients in whom radical HCC resection could be performed. 14 The prognosis of patients with extrahepatic metastases from HCC is unfavorable, and the median survival time is 6.7 months. 4 Another study indicated that the median survival time in patients with spinal metastases was 108 days. 7 A review of 152 patients with spinal metastases from HCC (26 articles) showed that the median survival time was 0.7 months in untreated patients, 6 months in those who underwent chemotherapy combined with radiotherapy, 7 months in those who underwent surgery alone, and 13.5 months in those who underwent surgery combined with multidisciplinary treatment. 8 Another review of 68 patients with skull metastasis from HCC (60 articles) indicated that the median survival time in 41 of 68 patients who could be evaluated was 8.9 months. 5 In the present case, the revised Tokuhashi score was 6 points, corresponding to a life expectancy of ≤6 months.
In many patients with bone metastases, drug therapy, radiotherapy, and palliative therapy are selected to relieve pain, reduce neurological symptoms, and maintain the QOL. Surgery is indicated for a limited number of patients as long as their general condition permits. Many patients cannot undergo surgery because the metastatic lesion is present at a non-resectable site or multiple metastases are present. 14 One study showed that radiotherapy markedly reduced pain, with an improvement rating of 58% to 95%. 15 However, other investigators have indicated that the effects of radiotherapy on paralysis are unclear. 16 In contrast, a higher survival rate and prolonged median survival were achieved in patients who underwent surgery. 4 Kim et al. 17 investigated the surgical outcomes of 33 patients with spinal metastases from HCC. They reported that the mean survival time of six of the patients with multiple spinal metastases was 194 days. Thus, we believe that the improvement in the survival time of our patient was due to the multidisciplinary therapy including palliative posterior occipitocervical fusion, occipital bone tumor resection, postoperative local radiotherapy, additional TACE, and denosumab injection.
Indications for surgery include maintenance of the performance status and control of intrahepatic recurrence.4,14 In the present case, the patient’s general condition was maintained, and local radiotherapy for sacral metastasis as well as several sessions of TACE for intrahepatic recurrence were conducted, leading to favorable local control. Therefore, surgery was performed.
The prognosis of patients with spinal/skull metastases is not always improved, which differs from the situation of patients with primary cancer. 7 However, posterior occipitocervical fusion is the best surgical option for upper cervical spine metastasis, and it markedly reduces cervical pain and paralysis. 6 In the present case, the patient had no pain recrudescence or deterioration in QOL until he died of liver failure 13 months after surgery.
Conclusions
We performed two-stage surgery involving posterior occipitocervical fusion and occipital bone tumor resection for both skull and upper cervical spine metastases from HCC. The patient’s cervical pain decreased in severity, and postoperative radiotherapy and chemotherapy could be conducted. The course was favorable without ADL restrictions. Patients with metastasis from liver cancer may have an unfavorable prognosis. Even in these patients, however, surgery as an aggressive palliative treatment and additional adjuvant therapy may prolong the survival period or maintain the QOL as long as the patient’s general condition permits.
Footnotes
Declaration of conflict of interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
