Abstract
Wellens’ syndrome is characterised by particular changes in electrocardiogram (ECG) precordial lead T-waves accompanied by proximal stenosis of the left anterior descending (LAD) artery. Two cases of electrocardiographic changes associated with Wellens’ syndrome are presented here. Case 1, a 55-year-old female, was transferred to the First Affiliated Hospital of Xi’an Jiaotong University with intermittent and laborious angina pectoris. Her first ECG on admission revealed T-wave inversion in leads V1–V3 and biphasic T-waves in V4. Case 2, an 85-year-old female, presented with dyspnoea and paroxysmal chest pain. Her admission ECG displayed asymmetrical T-wave inversion in leads V1–V3, I, and aVL, and depressed ST segments in leads V2–V5. In this patient, drug-eluting stents were placed on a LAD artery lesion and right coronary artery occlusion. The potential of ECGs to aid decision-making in severe myocardial infarction is straightforward, particularly in patients with characteristic ECGs, however, Wellens’ syndrome has a wide spectrum of clinical manifestations and the ECG patterns may manifest itself persistently over a period of weeks. Therefore, ECG parameters should be combined with coronary angiography to confirm the presence of lesions.
Introduction
Wellens’ syndrome consists of particular T-wave changes in the precordial leads of an electrocardiogram (ECG) accompanied by proximal stenosis of the left anterior descending (LAD) artery, and is often associated with sudden cardiac death and acute myocardial infarction,1–4 however, this syndrome is not always an acute process. The T-wave changes in Wellens’ syndrome are typically observed in asymptomatic patients and although these patients may initially respond well to medical management, they ultimately fare poorly with conservative therapy and require revascularization strategies. 4 It is important to identify the electrocardiogram characteristics of Wellens’ syndrome in order to provide an appropriate intervention, or to be able to intervene before myocardial infarction develops. 5 Here, two cases of electrocardiographic changes in patients with Wellens’ syndrome show different electrocardiogram characteristics, are presented.
Case reports
This study complied with the Declaration of Helsinki and was approved by the Ethics Committee of the First Affiliated Hospital of Xi’an Jiaotong University. Both patients provided written informed consent.
CASE 1
A 55-year-old female was transferred to the First Affiliated Hospital of Xi’an Jiaotong University in June 2016 due to intermittent and laborious angina pectoris. Her medical history and physical examination provided unremarkable findings. The ECG at hospital admission revealed T-wave inversion in the V1–V3 leads and biphasic T-waves in the V4 lead (Figure 1a). The serum level of cardiac high-sensitivity troponin T was <0.003 ng/ml (normal value < 0.014 ng/ml), creatine kinase (CK) was 55 U/l (normal value <200 U/l) and CK-MB was 6 U/l (normal value <24 U/l). Coronary angiography (CAG) revealed 70–90% LAD stenosis (Figure 1b), which was resolved by percutaneous coronary intervention (PCI) using drug-eluting stents (specification: 2.75 × 28 mm or 3.5 × 18 mm; JW Medical Systems, Weihai, Shandong, China) (Figure 1c). An ECG obtained following PCI showed that the biphasic T-waves in the V4 lead disappeared (Figure 2a). The persistently inverted deep T-wave in the V1–V3 leads were observed and no clinical outcome occurred at the scheduled one-month follow-up visit after PCI (Figure 2b).

Representative images obtained for CASE 1, a 55-year-old female who was transferred to the First Affiliated Hospital of Xi’an Jiaotong University with intermittent or laborious angina pectoris: (a) electrocardiogram (ECG) obtained at hospital admission showing deeply inverted T waves (red arrowhead) in leads V1–V3, and biphasic T-waves (black arrowhead) in V4; (b) Coronary angiography revealed 70–90% left anterior descending artery stenosis (red arrowhead); and (c) treatment with drug-eluting stents resolved the stenosis (red arrowhead).
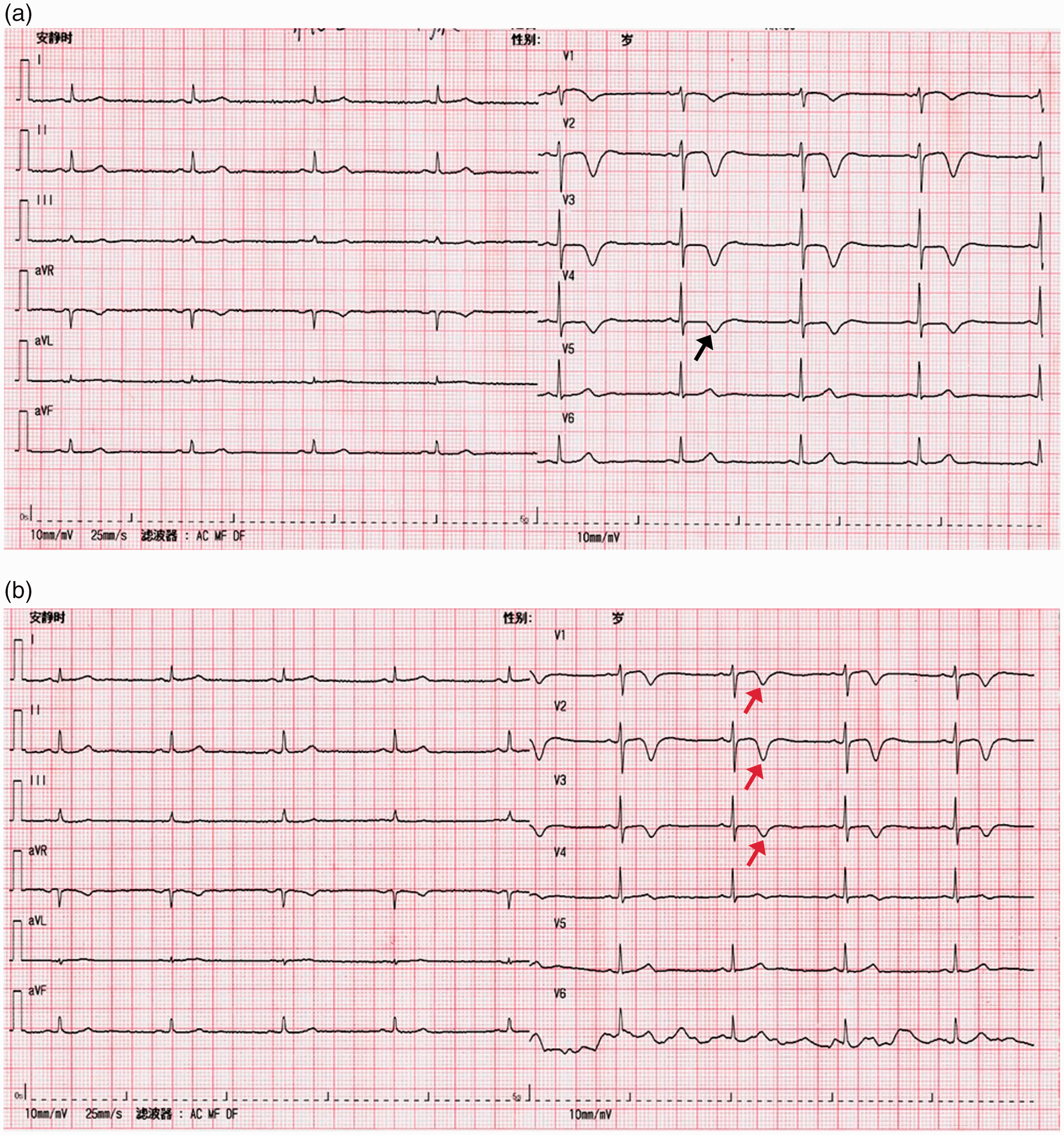
Representative images obtained for CASE 1, a 55-year-old female who was transferred to the First Affiliated Hospital of Xi’an Jiaotong University with intermittent or laborious angina pectoris: (a) electrocardiogram (ECG) following percutaneous coronary intervention (PCI) showing the resolution of biphasic T-waves in the V4 lead (black arrowhead); and (b) persistent deep T-wave inversions (red arrowhead) in leads V1–V3 were observed during a scheduled one-month follow-up visit after PCI.
CASE 2
An 85-year-old female who presented with paroxysmal chest pain and dyspnoea was admitted to the First Affiliated Hospital of Xi’an Jiaotong University in June 2016. The ECG obtained on admission displayed asymmetrical T-wave inversion in leads V1–V3, I, and aVL, and depressed ST segments in leads V2–V5 (Figure 3a). The serum level of cardiac high-sensitivity troponin T was 0.02 ng/ml (normal value <0.014 ng/ml), CK was 364 U/l (normal value <200 U/l) and CK-MB was 61 U/l (normal value <24 U/l). The patient was diagnosed as acute coronary syndrome and received dual antiplatelet therapy as follows: initial immediate therapy, 100 mg aspirin (BAYER, Germany) and 150 mg clopidogrel (Sanofi, France); regularly followed by 100 mg aspirin, oral, daily, 75 mg clopidogrel, oral, daily, 20 mg atorvastatin (Pfizer, USA), oral, daily and 30 mg isosorbide mononitrate (AstraZeneca, UK), oral, daily. ECGs obtained after 4 h of dual antiplatelet therapy, and prior to PCI, revealed bradycardia and progressive pseudo-normalization from inversion to upright T waves in the right precordial leads (Figure 3b–e). Elevated levels of the myocardial enzymes CK at 454 U/l (normal value <200 U/l) and CK-MB at 59 U/l (normal value <24 U/l) were observed. CAG indicated approximately 50–60% stenosis of the mid–left anterior descending artery and 100% occlusion of the right coronary artery (RCA) (Figure 4a and b). Drug-eluting stents (specification, 3.0 × 38 mm Abbott Vascular XIENCE Xpedition LL and 2.5 × 18 mm Endeavor Resolute) were placed on the LAD artery lesion and on the RCA occlusion (Figure 4c). The ECG following PCI displayed persistent pseudo-normalization of T waves in the right precordial leads (Figure 4d).

Representative images obtained for CASE 2, an 85-year-old female who presented with paroxysmal chest pain and dyspnoea and was admitted to the First Affiliated Hospital of Xi’an Jiaotong University: (a) electrocardiogram (ECG) obtained on admission revealed asymmetrically inverted T waves in leads V1–V3, I, and aVL (red arrowhead) and depressed ST segments in leads V2–V5 (black arrowhead); (b–e) subsequent ECGs obtained prior to percutaneous coronary intervention (PCI) revealed bradycardia and progressive pseudo-normalization from inversion to upright T waves in the right precordial leads, with premature ventricular contractions.

Representative images obtained for CASE 2, an 85-year-old female who presented with paroxysmal chest pain and dyspnoea and was admitted to the First Affiliated Hospital of Xi’an Jiaotong University: (a) coronary angiography (CAG) indicated approximately 50–60% stenosis of the mid–left anterior descending artery (red arrowhead) and (b) 100% occlusion of the right coronary artery (red arrowhead); (c) CAG showing that treatment with drug-eluting stents resolved the stenosis and occlusion (red arrowhead); and (d) an electrocardiogram obtained following percutaneous coronary intervention displayed persistent pseudo-normalization of T waves in the right precordial leads.
Discussion
The characteristic ECG patterns associated with Wellens’ syndrome can provide evidence for decision-making before severe MI develops.4,6–8 Regarding the two cases described in the present report, the first case was more consistent with Wellens’ syndrome due to the severe LAD occlusion, however, only 50–60% LAD stenosis but 100% RCA occlusion was observed in the second case, which did not conform to the typical Wellens’ syndrome. This discrepancy suggests that Wellens’ syndrome has a wide spectrum of clinical manifestations, and although characteristic ECG identification of Wellens’ syndrome can provide diagnostic evidence, additional CAG is needed to make a definite diagnosis.5,9
The mechanism of these dynamic ECG changes in the present two cases remains obscure. Some studies have shown that these types of ECG abnormalities may be caused by stunning and reperfusion of the myocardium.10,11 Severe LAD obstruction causes myocardial ischaemia and angina.12 When coronary flow is compensated by the collateral circulation, repolarization abnormalities caused by reperfusion injury result in T-wave symmetrical inversion or biphasic T-waves in the precordial leads.10 A study conducted by Migliore et al., 13 showed that myocardial oedema rather than stunning and reperfusion of the myocardium underlies the ECG changes of Wellens’ syndrome. However, more studies are needed to explain this phenomenon.
In conclusion, Wellens’ syndrome always involves severe occlusion of the proximal LAD artery, but has a wide spectrum of clinical manifestations. Therefore, ECG parameters should be combined with CAG to confirm the cardiovascular lesions.
Footnotes
Acknowledgements
The authors extend their gratitude to Professor Danjun Zhu, Department of Cardiovascular Medicine, First Hospital of Xi’an Jiaotong University, Xi’an, China, for discussion of the manuscript.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
