Abstract
Local infiltration analgesia has been widely used for pain relief in patients undergoing total knee arthroplasty. However, the effectiveness and major weakness of this technique have not been clarified; therefore, improvements in the technique have been limited. We searched PubMed, Embase, and the Cochrane Central Register of Controlled Trials and conducted a meta-analysis of randomized controlled trials comparing local infiltration analgesia with placebo infiltration in patients undergoing total knee arthroplasty. Fourteen trials involving 1305 knees were eligible. The results showed that local infiltration analgesia significantly reduced early perioperative pain and total narcotic consumption. However, postoperative functional outcomes were not significantly different between local infiltration analgesia and placebo. The pain-relieving effect of local infiltration analgesia was found to be strong but short in duration. In the future, modified delivery methods and formulas with longer durations of action and analgesia may provide a better environment for patients and therefore improve their function outcomes.
Keywords
Introduction
Conventional perioperative opioid-based analgesia techniques for total knee arthroplasty (TKA), such as patient-controlled analgesia and spinal or epidural analgesia, are associated with side effects including respiratory depression, sedation, postoperative nausea and vomiting, urinary retention, and constipation. 1
A comparatively new technique known as local infiltration analgesia (LIA), popularized by doctors from Sydney, Australia, 2 has been applied to TKA for more than 5 years. This technique has achieved inspiring goals in reducing the overall narcotic consumption, therefore decreasing the incidence of adverse effects.3,4 However, some other researchers found that LIA was not superior to placebo infiltration with respect to outcome indicators such as pain scores and range of motion (ROM).5,6 These divergent findings may cause confusion among practitioners. The questions that still remain unanswered are: Is LIA effective for TKA? What is the major weakness of LIA? How can LIA be improved?
We conducted a systematic review and meta-analysis of randomized placebo-controlled trials of LIA in patients undergoing TKA to examine the efficacy and major weakness of this technique.
Methods
Search strategy
A literature search for randomized controlled trials comparing LIA versus saline was performed independently by two authors (Z.H.Z., B.S.) using PubMed (1966 to January 2016), Embase (1984 to 2016), and the Cochrane Central Register of Controlled Trials (issue 1 to January 2016). All relevant English-language articles were retrieved, and the last data search occurred on 10 January 2015. References of the retrieved articles were also reviewed to broaden the database search. The search strategy used is listed in the Appendix.
Eligibility criteria and data extraction
We included all published articles describing randomized controlled trials that compared LIA versus saline, regardless of the publication year or country. All selected articles provided adequate data for quantitative analysis, especially the means and standard deviations for continuous variables and the ratio of patients who developed adverse events to the total number of patients for dichotomous variables.
The exclusion criteria were as follows: the study focused on irrelevant procedures, the study did not involve primary clinical research, indispensable data were missing or unavailable, and duplicate publications were present. Two reviewers (Z.H.Z., B.S.) independently screened the titles, abstracts, and full texts of all articles to determine their eligibility for inclusion after consensus. Data were extracted from the included articles based on a preformed sheet.
Quality assessment of the included studies
The methodological assessment of the included trials was based on the modified Jadad score7,8 and was completed independently by two reviewers (Z.H.Z., B.S.). Articles with ≥4 points were considered high-quality studies, and divergences were solved by discussion.
Statistical analysis
The meta-analysis was performed using Review Manager Version 5.0 software for Windows (The Nordic Cochrane Centre, The Cochrane Collaboration, Oxford, England). The mean difference (MD) and 95% confidence interval (CI) were calculated for continuous variables, and the odds ratio and 95% CI were calculated for dichotomous variables. Heterogeneity was estimated by the chi-square test. A P-value of 0.10 was defined as the level of statistical significance in the tests for heterogeneity (P ≤ 0.10 indicated the presence of heterogeneity). A fixed-effects model was employed when heterogeneity was absent; otherwise, a random-effects model was employed. Data are presented by forest plots.
Ethics statement
This study was totally based on online published articles without the direct use of any data from or interventions involving patients or animals. Therefore, the requirement for ethics committee approval was waived.
Results
Screening results
In total, 297 articles were retrieved on the basis of the predefined search strategy. After screening the titles, abstracts, and full texts, we included 14 articles3–6,9–18 that met the eligibility criteria. A total of 960 patients with 1305 knees in 14 randomized controlled trials were included in the quantitative analysis. Among the 14 included trials, ropivacaine was used as the infiltration drug in 7 trials, while bupivacaine was used alone in 6 trials and together with levobupivacaine in 1 trial. Epinephrine was used as a supplement in seven trials. A flow chart of the study inclusion process is shown in Figure 1. Table 1 shows the general demographic characteristics of the included trials, and Table 2 shows the surgical and anesthetic data. All included studies used a similar operative anesthetic technique between the LIA and saline groups.

Flow chart of study inclusion process.
General demographic characteristics.

Pts, patients; LIA, local infiltration analgesia; NS, normal saline; M, male; F, female; BMI, body mass index; ASA, American Society of Anesthesiologists physical status; OA, osteoarthritis; RA, rheumatoid arthritis.
Anesthetic and surgical information.

MP, medial parapatellar approach; MV, midvastus approach; SV, subvastus approach; PCA, patient-controlled analgesia; IM, intramuscular; FNB, femoral nerve block; SQ, subcutaneous; IV, intravenous; LIA, local infiltration analgesia; NS, normal saline infiltration.
Methodological quality assessment
We summarized the modified Jadad score of the included articles in Table 3 for quality assessment. The results showed that all 14 included articles were of high quality, with a minimum modified Jadad score of 4 points. The level of bias in all 14 studies was low according to the modified Jadad score scale.
Quality assessment using the modified Jadad score.

Meta-analysis results
In this meta-analysis, we included eight outcome indicators that were reported by no less than two trials: the visual analogue scale (VAS) score, narcotic dose equivalent, adverse effects, ROM, ambulation distance, straight-leg raise (SLR), Oxford score, and length of stay (LOS). Only two of these eight indicators, the VAS score and narcotic dose equivalent, were significantly different between the LIA group and saline group as described below.
VAS score
Five of the included articles reported the VAS score.4,6,9,10,12 The VAS score at 24 hours postoperatively was analyzed. There was no evidence of statistical heterogeneity among the studies (I2 = 6%), and a fixed-effect model was used. The meta-analysis results (see Table 4) showed that patients in the LIA group had significantly lower VAS scores (MD, −0.66; 95% CI, −1.08 to −0.23; P = 0.003).
Meta-analysis results of outcome indicators.
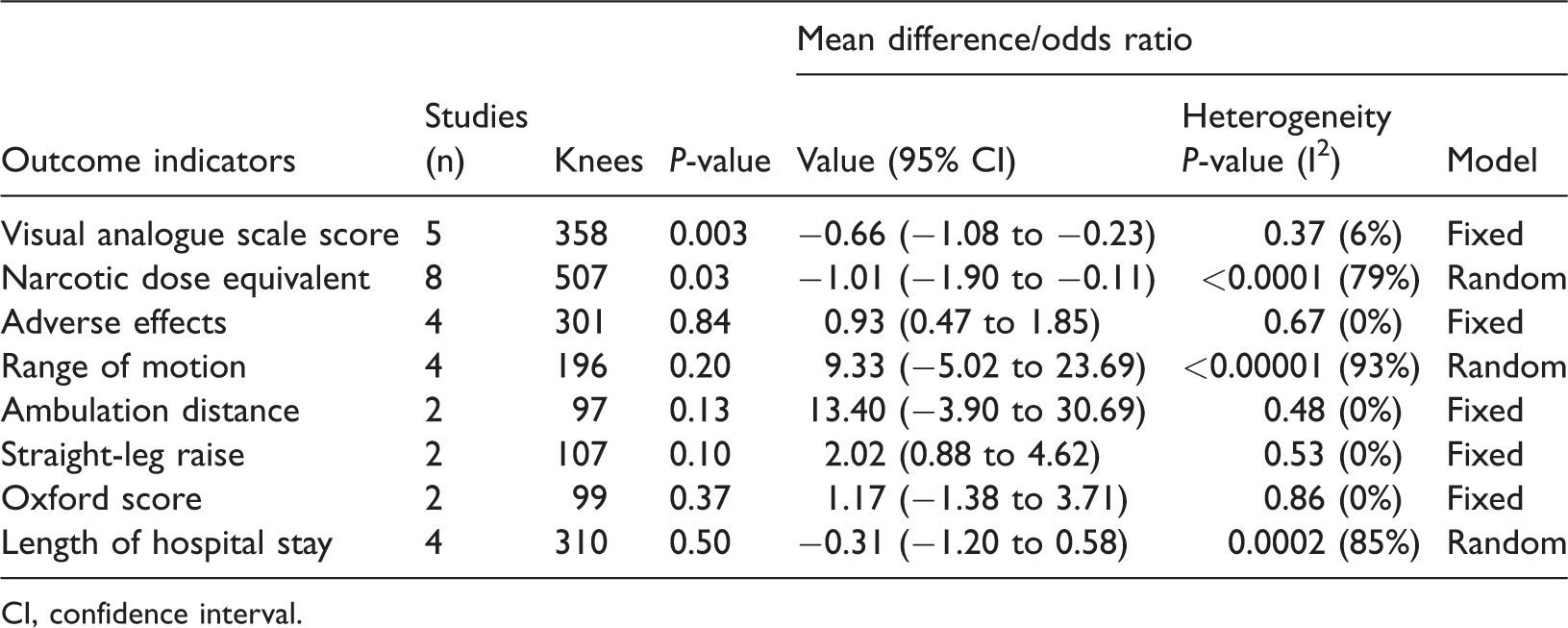
CI, confidence interval.
Narcotic dose equivalent
Eight of the included articles reported the narcotic dose equivalent at 24 and/or 48 hours postoperatively.3,4,6,9,10,12,13,15 Statistical heterogeneity was found among the studies (P < 0.0001, I2 = 79%), so a random-effects model was used. The meta-analysis results (see Table 4) showed that patients in the LIA group had significantly lower narcotic dose equivalents (MD, −1.01; 95% CI, −1.90 to −0.11; P = 0.03).
Adverse effects
Four trials provided data regarding adverse effects.4,9,10,13 There was no evidence of statistical heterogeneity among the studies (I2 = 0%), and a fixed-effects model was used. No significant difference in adverse effects was observed between the LIA group and saline group (see Table 4) (odds ratio, 0.93; 95% CI, 0.47 to 1.85).
Function indicators
ROM
Four trials provided data regarding ROM.6,10,12,15 Statistical heterogeneity was found among the studies (P < 0.00001, I2 = 93%), so a random-effects model was used. No significant difference in ROM was observed between the LIA group and saline group (see Table 4) (MD, 9.33; 95% CI, −5.02 to 23.69).
Ambulation distance
Two articles reported the ambulation distance.10,12 There was no evidence of statistical heterogeneity between the two studies (I2 = 0%), and a fixed-effects model was used. No significant difference in the ambulation distance was found between the LIA group and saline group (see Table 4) (MD, 13.40; 95% CI, −3.90 to 30.69).
SLR
Data regarding the SLR were available in two articles.3,12 There was no evidence of statistical heterogeneity between the studies (I2 = 0%), and a fixed-effects model was used. No significant difference in the SLR was observed between the LIA group and saline group (see Table 4) (odds ratio, 2.02; 95% CI, 0.88 to 4.62).
Oxford score
Pooled data regarding the Oxford score from two articles6,15 were analyzed. There was no evidence of statistical heterogeneity between the studies (I2 = 0%), and a fixed-effects model was used. The meta-analysis results showed no significant difference in the Oxford score between the LIA group and saline group (see Table 4) (MD, 1.17; 95% CI, −1.38 to 3.71).
LOS
Data regarding the hospital LOS were available in four articles.4,6,13,15 Statistical heterogeneity was found between the studies (P = 0.0002, I2 = 85%), so a random-effects model was used. No significant difference in the LOS was observed between the LIA group and saline group (see Table 4) (MD, −0.31; 95% CI, −1.20 to 0.58).
Discussion
The efficacy of LIA, which is an emerging and aspiring technique, remains controversial. Considering the uncertain efficacy of LIA,5,6 orthopedic surgeons are not willing to apply this technique without the ability improve it. Clarification in this field is urgently needed.
The present meta-analysis indicated that patients who underwent TKA who had received LIA treatment had significantly lower VAS scores than those in the placebo groups. Patients in the LIA group also had significantly lower narcotic dose equivalents. No significant differences were found in most of the other outcome indicators, including the ROM, SLR, and Oxford score. The meta-analysis results regarding the VAS score show promise with respect to improvement in the patients’ subjective feeling after undergoing LIA.4,6,9,12 However, the LOS was not significantly different between the two groups, which is consistent with a previous systematic review. 19
The meta-analysis results regarding the function outcome indicators implicate that LIA is not effective for postoperative function improvement, which is in contrast to the results of a former clinical trial. 20 Application of a pressure bandage and ice pack on the wound area may help to prolong the duration of action of LIA and therefore improve the postoperative function of patients who have undergone TKA. 2
Besides the findings regarding the VAS score, the significantly lower narcotic dose equivalent in the LIA group confirms the potential capacity of LIA in replacing some routinely used narcotics, which could be the foundation of further studies comparing LIA with femoral nerve block 21 or patient-controlled analgesia. 22
Compared with a previous non-quantitative systematic review, 19 the present meta-analysis has higher power. First, more high-quality trials were included in our study, substantially advancing the evidence level of the concerned topic. Second, a comprehensive collection of outcomes was considered in this meta-analysis, broadening the study overview. Finally, and importantly, this meta-analysis is more persuasive because of the use of a quantity analysis technique.
This current study still has several limitations. Heterogeneity in the local analgesic drug combinations, infiltration sites, and volumes was present among the studies. One of the included studies 5 was conducted in simultaneous bilateral patients, which may have bias because of the systemic effect of LIA. In addition, the periods of use of LIA were not long enough, and the results therefore may not reflect the long-term effects. Finally, the small quantity of included studies may restrict the statistical persuasion.
In summary, the efficacy of LIA in improving short-term postoperative pain relief and reducing total narcotic consumption has been confirmed. No consensus has been reached regarding the best infiltration sites, volumes, or timings of LIA,23,24 and additives of LIA are variable. For example, the addition of steroids and ketorolac has been questioned because of the potentially increased risk of intra-articular infection 25 and possible renal and gut toxicity, 2 respectively. LIA is still a recommended analgesic option, but it does not have the ability to improve the functional outcomes compared with placebo infiltration in patients undergoing TKA. Additional high-quality prospective randomized controlled trials focusing on different delivery methods (e.g., controlled and slow-release techniques), infiltration sites, volumes, timings, drug combinations,26,27 and local bandaging techniques are needed to prolong the action time of LIA and thus improve its effectiveness.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
