Abstract
Objective
This study aimed to summarize the clinical experience of severe intrathoracic anastomotic leakage encountered in clinical practice by using cervical end-esophageal exteriorization.
Methods
We undertook a retrospective review of four patients who developed severe anastomotic leakage after subtotal esophagectomy at our department. Four patients with a life-threatening condition and failed conservative management were re-operated on from the original incision using an exteriorized cervical end-esophageal gastric conduit. We returned the gastric conduit to the abdomen and placed a feeding jejunostomy or gastrostomy catheter. Until inflammation was controlled, we re-established intestinal continuity with the gastric or colon conduit, pulled up to the neck by a retrosternal channel.
Results
Four patients with esophagectomy and severe intrathoracic anastomotic leakage underwent re-operation. The gastric conduit was returned to the abdomen and cervical end-esophageal exteriorization was performed. Inflammation was rapidly controlled after surgery. Three patients received a second re-operation to re-establish intestinal continuity on days 63, 63, and 16 after the first re-operation. One patient refused re-operation to re-establish intestinal continuity. All four patients survived.
Conclusion
Cervical end-esophageal exteriorization in patients with severe intrathoracic anastomotic leakage results in rapid control of inflammation. This creates an opportunity to re-establish gastrointestinal continuity, leading to survival of patients.
Keywords
Introduction
Severe intrathoracic anastomotic leakage after esophagectomy is a life-threating complication of esohpageal resection, often leading to the patient’s death. We describe our experience with cervical end-esophageal exteriorization for patients in extremis. From November 2005 to January 2017, we encountered four patients who had severe, uncontained, intrathoracic esophagogastric anastomotic leaks after esophagectomy was performed for cervical end-esophageal exteriorization. All four patients were saved by this treatment. Three patients underwent staged gastric or colon interposition by a retrosternal channel to re-establish intestinal continuity, and one of the patients refused re-operation.
Case Presentation
Case 1: A 58-year-old man was diagnosed with middle thoracic esophageal cancer in our hospital after being admitted for dysphagia (Table 1). On 25 July 2016, he was treated with radical resection of esophageal cancer via right thoracotomy and median laparotomy. The whole procedure was successfully performed. However, from the 3rd day, the patient suffered from fever and the volume of thoracic tube drainage increased from 500 mL up to 1500 mL per day. The drainage fluid gradually turned from clear to filthy with gas and saliva. On the 10th day, an endoscopic examination showed large gastric wall necrosis of approximately 4 × 4 cm2 around the anastomosis. The patient suffered from increasing sepsis and multiple organ failure. On 5 August 2016, emergency re-operative explorative surgery was performed. We discovered that an anastomosis was located above the aortic arch in the apex of the right cavity. There was full-thickness gastric wall necrosis near the anastomotic gastric conduit tip. The necrosis bandwidth was approximately 4 cm, with a serious pleural and mediastinal abscess. Therefore, we debrided the abscess, resected the nonviable gastric necrosis, flushed the thoracic cavity, and placed several drainage and flushing tubes. We considered that repair or redo of esophagogastric anastomosis was a high risk. Therefore, we resected the gastric necrotic wall using a linear cutter stapler and returned the viable remnant gastric conduit to the abdominal cavity through the transhiatal approach. A feeding jejunostomy was placed by laparotomy and the proximal esophagus was exteriorized by the cervical subcutaneous route. Postoperative ventilator-assisted breathing, continued blood purification, broad-spectrum antibiotics, chest flushing and drainage, and parenteral and enteral nutrition were provided to the patient, who had a fever and coma for up to 48 hours. After this time, sepsis was gradually controlled. Images of end-esophageal exteriorization and reconstructive surgery for this patient are shown in Figures 1 and 2. At 63 days after the second operation (8 October 2016), the patient underwent successful retrosternal colonic interposition, where a colon conduit was harvested from the left side. A postoperative examination showed no obvious symptoms and restored oral intake.
Characteristics and clinical data of the patients

The three-tube method included application of a thoracic closed drainage tube, gastrointestinal decompression tube, and enteral nutrition tube. TNM: tumor, node, metastasis.

Cervical subcutaneous end-esophageal exteriorization on the 48th day after the first re-operation in case 1.
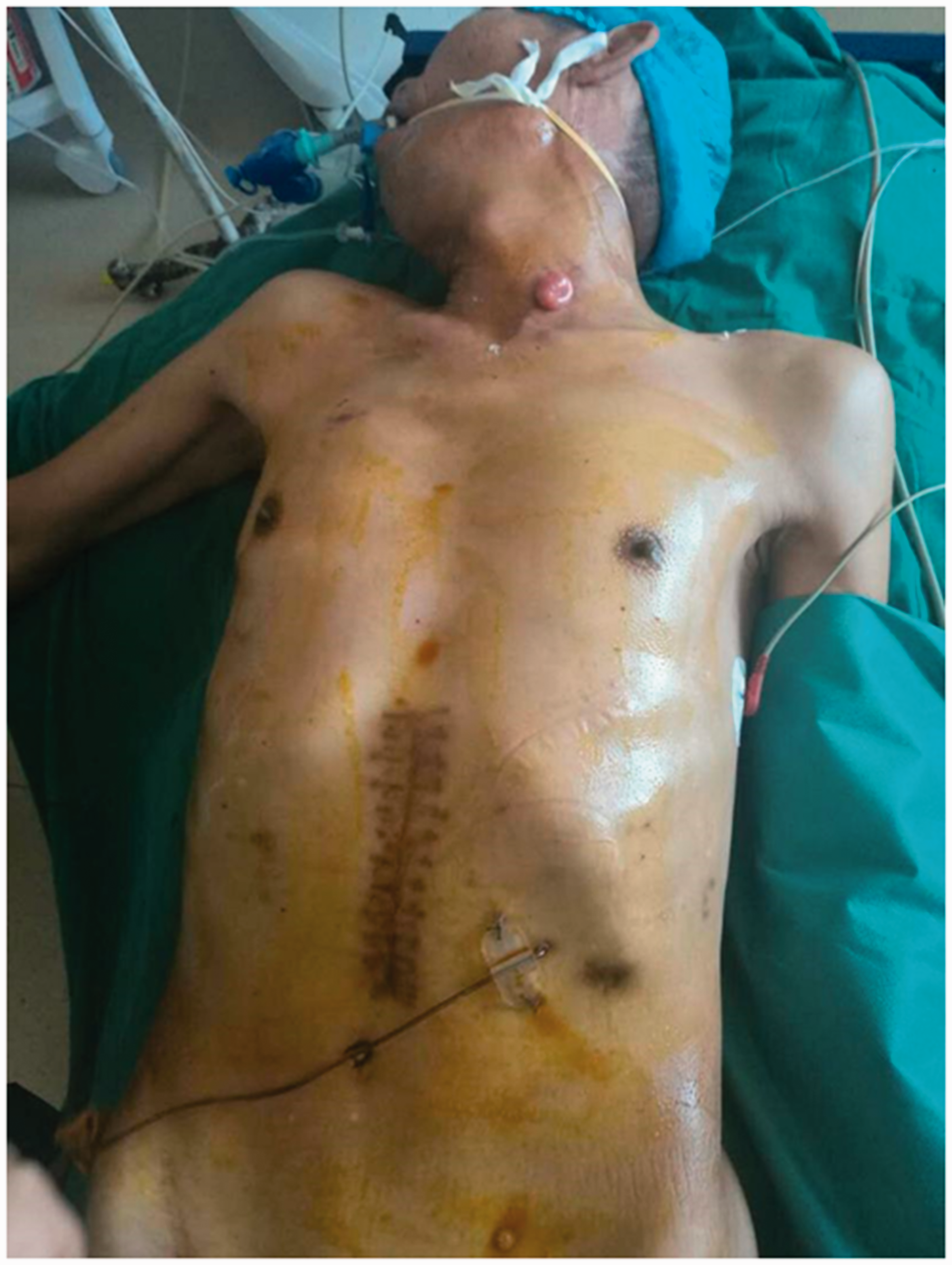
Photograph of reconstructive surgery (taken on the operating table) in case 1.
Case 2: A 59-year-old man suffered from middle esophageal cancer. On 26 November 2010, through left thoracotomy, he underwent subtotal esophageal resection and gastroesophageal anastomosis above the aortic arch (Table 1). On day 4, the patient was diagnosed with anastomotic leakage after oral contrast radiography. A video showed that almost all of the contrast material directly went into the chest. The patient manifested a sustained fever and had a high white blood cell count and C-reactive protein level, hypoalbuminemia, circular collapse, and multiple organ failure. We discussed the case with a multidisciplinary team and decided to re-operate. On day 8 after the first operation, we performed an explorative operation from the original incision. We found two thirds of anastomosis dehiscence and a serious thoracic infection. Therefore, we closed the gastric conduit by a linear cutter stapler and returned it to the abdominal cavity. At the proximal esophagus, we performed cervical end-esophageal exteriorization and placed a feeding gastrostomy tube by laparotomy. The patient recovered well, but refused to accept a third operation to reconstruct gastrointestinal continuity for long-term replacement of the feeding gastrostomy tube once the tube was occluded. The patient died because of malnutrition and pneumonia, which resulted in respiratory failure after 26 months.
Case 3: A 39-year-old man experienced spontaneous esophageal rupture after forceful vomiting as a result of drinking a large volume of beer (Table 1). He initially underwent subtotal esophagectomy and gastroesophageal anastomosis at the apex of the cavity at a different hospital on 21 July 2008 (by right thoracotomy and a midline laparotomy). From the 5th day after operation, there was copious bilious drainage from the chest tubes. The patient was diagnosed with anastomosis by oral contrast radiography and treated with conservative management. However, with increasing sepsis, he was transferred to our hospital after the primary procedure at 16 days. We examined the patient via the original incision and found esophagogastric anastomosis dehiscence and heavy thoracic infection. We then performed wide debridement of the pleural cavity and mediastinum. We flushed the thoracic cavity, improved drainage, closed the gastric conduit with a linear cutter stapler, and returned it to the abdominal cavity. A feeding jejunomy was then placed by laparotomy. The proximal esophagus underwent cervical end-esophageal exteriorization. The general condition of the patient rapidly improved. On post-re-operation day 63, the patient received a third operation to reconstruct the gastrointestinal continuity. We found that the gastric conduit could not be pulled to the neck. Therefore, we used the right side of the colon for restoring gastrointestinal continuity by the retrosternal channel. After the operation, the patient suffered from slight leakage of the anastomotic neck. The patient recovered well with only a neck dressing and there were no follow-up anastomotic stricture.
Case 4: A 63-year-old man had middle esophageal cancer (Table 1). On 26 November 2005, subtotal esophagectomy was performed through the left sixth intercostal space. From the 5th day, the patient had complex signs and symptoms, including fever, shortness of breath, increasing sepsis, and a large volume of chest drainage. An oral methylene blue test showed that methylene blue drained into the chest tube. By a radiography swallow contrast examination, we found that all of the water-soluble contrast medium had extravasated into the pleural space and drained into the chest tube. The patient was initially managed conservatively after diagnosis of the leak. After strict conservative therapy, the patient showed an increasing amount of sustained sepsis and multiple organ failure. On postoperative day 14, we had to perform thoracotomy from the primary incision, and found two thirds of anastomosis dehiscence. Although the anastomosis dehiscence was large and all of the contents of digestive fluid went directly into the cavity, chest tube drainage was efficient, and thus the cavity infection was not serious. There was gastric outlet obstruction and high tension between the gastric conduit and esophagus. Primary anastomotic repair was difficult and high risk. Therefore we closed the gastric conduit with a linear cutter stapler and returned it to the abdominal cavity. In the proximal esophagus, cervical end-esophageal exteriorization was performed and a feeding gastrostomy was placed. Prompt clinical improvement was noted under supportive therapy within the first few days, and the patient’s general condition quickly improved. In a second re-operation, the patient underwent a successful gastric conduit interposition by retrosternal channel on the 16th day after the second operation. The patient began oral intake on reconstructive postoperative day 9 and was discharged on reconstructive postoperative day 16. The total hospital stay was 55 days.
Written informed consent for the patients’ information and images to be published was provided by the patients and authorized by the Ethics Committee of the Tumor Hospital of Wuwei.
Discussion
In this group of four patients who suffered from severe intrathoracic anastomotic leakage, conservative management was ineffective and their lives were endangered. Therefore, we performed cervical end-esophageal exteriorization. Three patients underwent staged gastric or colon interposition by a retrosternal channel for restoring gastrointestinal continuity, and all of them survived. One patient refused to receive a reconstruction operation because of other factors. Four patients with severe intrathoracic anastomotic leakage were rescued.
Intrathoracic esophagogastric anastomotic leakage following esophagectomy is a life-threatening complication of esophageal resection. This condition is associated with a high morbidity and mortality,1,2 with a probability of 5% to 35% morbidity,3,4 with mortality rates as high as 30% to 60%.5–7 Despite advances in surgical techniques and critical care, persistent sepsis from an esophagogastric anastomotic leakage has almost 100% mortality. 8 Most of the treatments for intrathoracic anastomotic leakage are still considered conservative, including adequate drainage, enhancing nutrition, stent placement,9,10 and endoscopic vacuum-assisted closure. 11
The mainstay of treatment for intrathoracic esophagogastric anastomotic leakage is prompt prevention of further soilage, elimination of infection, debridement of devitalized tissue, lavage and wide bore drainage of the infected pleura and mediastinum, and optimization of nutrition. Management of intrathoracic esophagogastric anastomotic leakage can be non-operative if the patient is stable and sepsis is controlled. Generally, surgery is reserved for cases that do not respond to a conservative approach. Successful treatment of intrathoracic esophagogastric anastomotic leakage poses challenges for physicians and patients. Particularly for severe intrathoracic leakage, the above-mentioned methods often fail to work, leading to death of the patient.
All of our four patients had more serious symptoms of systemic sepsis, a body temperature of higher than 39°C, tachycardia, weakness, shortness of breath accompanied by water and electrolyte imbalance, a large amount of digestive juice, and air in the chest cavity. This caused uncontrollable chest infections and pneumothorax, and increased thoracic drainage volume, even up to 1000 to 2500 mL daily. Discussion within our multidisciplinary team led to the decision that an endoscopic stent and vacuum-assisted closure were not suitable for our patients. Generally, endoscopic stenting is limited to leaks involving < 30% of the anastomotic circumference and without extensive necrosis of the gastric conduit. Patients with extensive devitalization of esophageal anatomy, large leaks, or a nonviable conduit are not suitable for endoscopic management with stent placement. 12 All available managements in our patients had failed. Esophageal exclusion and diversion is the final option in patients when all conservative treatments fail. Cervical end-esophageal exteriorization prevents ongoing leakage of salivary and gastric secretions into the thoracic cavity. Our patients were provided anti-shock treatment. Furthermore, we performed a thoracotomy, re-operation from the original incision, and decortication and drainage of empyema. We removed pleural abscesses and necrotic tissue, released adhesions, and lavaged and improved chest cavity drainage. Because of severe symptoms of infection, persistent sepsis, and development of multiorgan failure, we considered that repair or repeat esophagogastric anastomosis was a high risk. The surgery needed to be completed in the shortest time. Therefore, we completely separated the original esophagogastric anastomosis, the proximal esophagus was pulled out from the neck to cervical end-esophageal exteriorization, and necrotic gastric tissue was resected. The viable residual gastric conduit was then closed by a linear stapler and returned to the abdominal cavity. Finally, we placed a gastrostomy or jejunostomy feeding tube for enteral nutrition.
After the operation of cervical end-esophageal exteriorization, the patients’ inflammation was rapidly controlled. The patients were provided enteral and parenteral nutritional support, and gradually recovered a positive nitrogen balance. The patients then had the opportunity for a staged re-operation to reconstruct the esophageal continuity. Colon or gastric conduit interposition was pulled up to the neck with cervical esophageal anastomosis to reconstruct the continuity.. This method of reconstruction operation was chosen to avoid re-opening the chest cavity, and this surgery is easy and safe.
The timing of reconstruction gastrointestinal continuity is still controversial. Some studies have reported that a reconstruction operation should be postponed for at least 6 months. 13 However, according to our experience, 6 months is not necessary, for the following reasons. First, we observed that inflammation had sufficiently subsided. Second, patients had a positive nitrogen balance restored. Third, the first two surgeries caused great pain for the patients and the patient’s acceptance was also a problem. If the time of the previous operation is too long, the stomach might shrink, and often cannot be pulled up to the neck. Therefore, more attention needs to be paid to make the stomach stretch as much as possible. Only the colon can be used if the stomach cannot be pulled up to the neck. Therefore, before surgery, patients should have colonoscopy or colonic angiography to confirm the situation of the colon.
In 1956, Johnson reported that esophageal exclusion and division was used in treatment of patients with spontaneous esophageal rupture. 14 However, reports of this method in patients with severe intrathoracic anastomotic leakage after esophagectomy are still rare. 12 We believe that cervical end-esophageal exteriorization in patients with severe intrathoracic anastomotic leakage after esophageal cancer surgery has a strong practical value for saving patients’ lives. However, this approach commits the patient to a prolonged and potentially hazardous intestinal reconstruction. 15
The cervical end-esophageal exteriorization procedure is relatively easy and quick, and should be familiar to all esophageal surgeons. This procedure should be performed early in patients with increasing sepsis and when conservative management has failed. This procedure should be used as a final option to save a patient’s life.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
