Abstract
Objective
The optimal surgical intervention on the treatment for proximal humeral fractures (PHFs) remains uncertain. The aim of this study was to evaluate clinical outcomes following fixation of PHFs by intramedullary nails or locking plates
Methods
The Cochrane Library, PubMed, EMBASE, China Knowledge Resource Integrated (CNKI), Chongqing VIP and Wanfang databases were systematically searched for studies published between January 01, 1996 and December 31, 2016 that investigated intramedullary nail vs. locking plate in the surgical treatment of PHFs. A meta-analysis examined incision length, blood loss, operation time, fracture healing time, Constant scores and post-operative complications. The methodological and evidence quality were also assessed by MINORS and GRADE system.
Results
From the original 1024 references, 20 studies involving 1384 patients met the eligibility criteria. Analyses showed that intramedullary nails were superior to locking plates in incision length, peri-operative bleeding time, operation time and fracture healing time. However, there were no differences between treatments in Constant score or post-operative complications.
Conclusion
Although the evidence quality was poor, the results suggest that compared with locking plates, intramedullary nails may be a better choice for the repair of PHFs.
Introduction
Proximal humeral fracture (PHF) is a common shoulder fracture of increasing prevalence which is common in elderly patients, many of whom have osteoporosis. 1–3 Recent estimates suggest that proximal humeral fractures account for 4–5% of all fractures and 20% of all fragility fractures.4,5 Although most PHFs do not require surgical intervention, surgical treatment is still necessary for comminuted or seriously displaced fractures including two, three, and four-part fractures. 6 While, conventional plate and screw fixation has a high failure rate 7 , recent reports suggest that intramedullary nail and locking plates may provide good clinical outcome for unstable PHFs with rigid internal fixation. 8
Although several studies have compared clinical outcomes following the use of intramedullary nail or locking plates for PHFs, the optimal management for the surgical treatment of these fractures remains controversial. 9–28 A meta-analysis of eight studies conducted in 2015 that evaluated clinical outcomes and complications following insertion of locking plates or intramedullary nails for PHFs did not conclusively show their benefits and suggested more research is needed. 29 In addition, the study did not analyse the outcomes of the different types of PHFs according to their Neer classification. 30 Therefore, the purpose of the present meta-analysis was to evaluate evidence from studies that compared clinical outcomes following surgical treatment with intramedullary nail or locking plates in different types of PHFs.
Methods
The Cochrane Library, PubMed, EMBASE, China Knowledge Resource Integrated (CNKI), Chongqing VIP and Wanfang databases were systematically searched for studies published between January 01, 1996 and December 31, 2016 that investigated intramedullary nail vs. locking plate in the surgical treatment of PHFs. Key words/terms included: PHF; humeral neck fracture; PHN; PHILOS; intramedullary nail; proximal intramedullary nail; locking plate; locking proximal humerus plate. In addition, the reference lists of all included studies were checked for any potential additional publications. No restrictions were made on the publication language.
For a published report to be included in the meta-analysis, it had to fulfil the following criteria: (1) comparative randomized, controlled clinical trial or retrospective study of level III and above (Canadian Task Force on the Periodic Health Examination’s Levels of Evidence), 31 that reported intramedullary nail vs. locking plate in the treatment of PHF; (2) reported at least one variable (e.g., incision length, blood loss, operation time, fracture healing time, Constant score 32 and/or postoperative complications); (3) follow-up time was at least 12 months. Single case reports, reviews, abstracts, letters, meeting proceedings and non-comparative studies were excluded.
Two reviewers [M.L., Y.H.W.] independently screened the papers from their titles and abstracts and selected relevant studies. The reviewers were not blinded to the journals, organizations, financial assistance, conflict of interest and/or researchers’ information. The reviewers then assessed the full text to determine if the study should be included. Any discrepancy was resolved through discussion.
Three reviewers [M.L., M.Y., Y.P.Z.] independently extracted data from each study using a standard data extraction form. The following items were extracted: title; authors; date; country; study design; number of intramedullary nail and locking plate cases; number of female patients; Neer classification 30 ; age, duration of follow-up; clinical outcomes; level of evidence. 31
The methodological quality of the included randomized controlled trials was independently assessed by two authors [M.L., Y.H.W.] using the ‘Cochrane collaboration’s tool for assessing the risk of bias’. 33 Disagreements were resolved by discussion or consensus and a third author [M.Y] was the adjudicator when no consensus was reached. The tool covers seven domains: (1) random-sequence generation (selection bias); (2) allocation concealment (selection bias); (3) blinding of participants and personnel (performance bias); (4) blinding of outcome assessment (detection bias); (5) incomplete outcome data (attrition bias); (6) selective reporting (reporting bias); (7) other biases. All other studies were assessed by the same two authors using the methodological index for non-randomized studies (MINORS). 34 This is a validated instrument which is used to assess the quality of comparative or non-comparative controlled clinical trials. MINORS contain 12 items and each is scored as 0-2 (0= not reported; 1=reported but inadequate; 2= reported adequately). A MINORS score >12 was considered the level for inclusion in the meta-analysis.
The level of evidence quality was estimated according to the guidelines of Grading of Recommendations, Assessment, Development, and Evaluation (GRADE). 35 Although the GRADE working group acknowledges the importance of RCTs, it also recognizes circumstances in which observational studies generate high quality evidence of treatment effects. The GRADE approach applies a sequential assessment of the evidence quality and a subsequent judgment on the strength of the recommendations. The evidence grades were classified into four categories: (1) high grade (further research is unlikely to change confidence in the effect estimate); (2) moderate grade (further research is likely to alter confidence in the effect estimate and may change the estimate); (3) low grade (further research is likely to alter confidence in the effect estimate significantly and to change the estimate); (4) very low grade (any effect estimate is uncertain). GRADEpro Guideline Development Tool (GDT) software version 3.6 for Windows was used to grade evidence and make recommendations.
Statistical analyses
The meta-analysis was performed by two authors [M.L., Y.H.W.] using Review Manager (RevMan) [Computer program] Version 5.3. Copenhagen: The Nordic Cochrane Centre, The Cochrane Collaboration, 2014. A P-value <0.05 was considered to indicate statistical significance.
Prior to data analysis, heterogeneity was assessed according to Cochrane’s χ2 (Q) test and I2 statistic. 36 No heterogeneity was defined as P > 0.1, I2=0%, low heterogeneity was P > 0.1, I2<50% and high heterogeneity was P < 0.1, I2 > 50%. For low statistical heterogeneity, a fixed effects model was applied to the data and for high heterogeneity a random effects model was used. Sensitivity analyses were performed by removing one study at a time and repeating the analyses. Weighted mean difference (WMD) and standardized mean difference (SMD) were used to measure the continuous variables and the relative risk (RR) was used for dichotomous variables (±95% confidence intervals [Cis]). Publication bias was investigated with the use of a funnel plot graph. 29
Results
The literature search yielded an initial pool of 1024 references from which 20 articles ultimately met the eligibility criteria (Figure 1).9–28 Twelve studies were performed in China, three in Germany, two in France, and one each in USA, Brazil and Spain (Table 1). Three studies were prospective and 17 were retrospective. Nine studies investigated Neer type II PHFs, one study investigated Neer type III and one type IV. Three other studies investigated Neer types II and III PHFs, two studies investigated Neer types III and IV PHFs, and four studies investigated Neer types II, III and IV PHFs.

Flowchart of the study selection process.
Characteristics of the 20 studies included in the meta-analysis of intramedullary nail (IN) vs locking plate (LP) for the treatment of proximal humeral fractures.
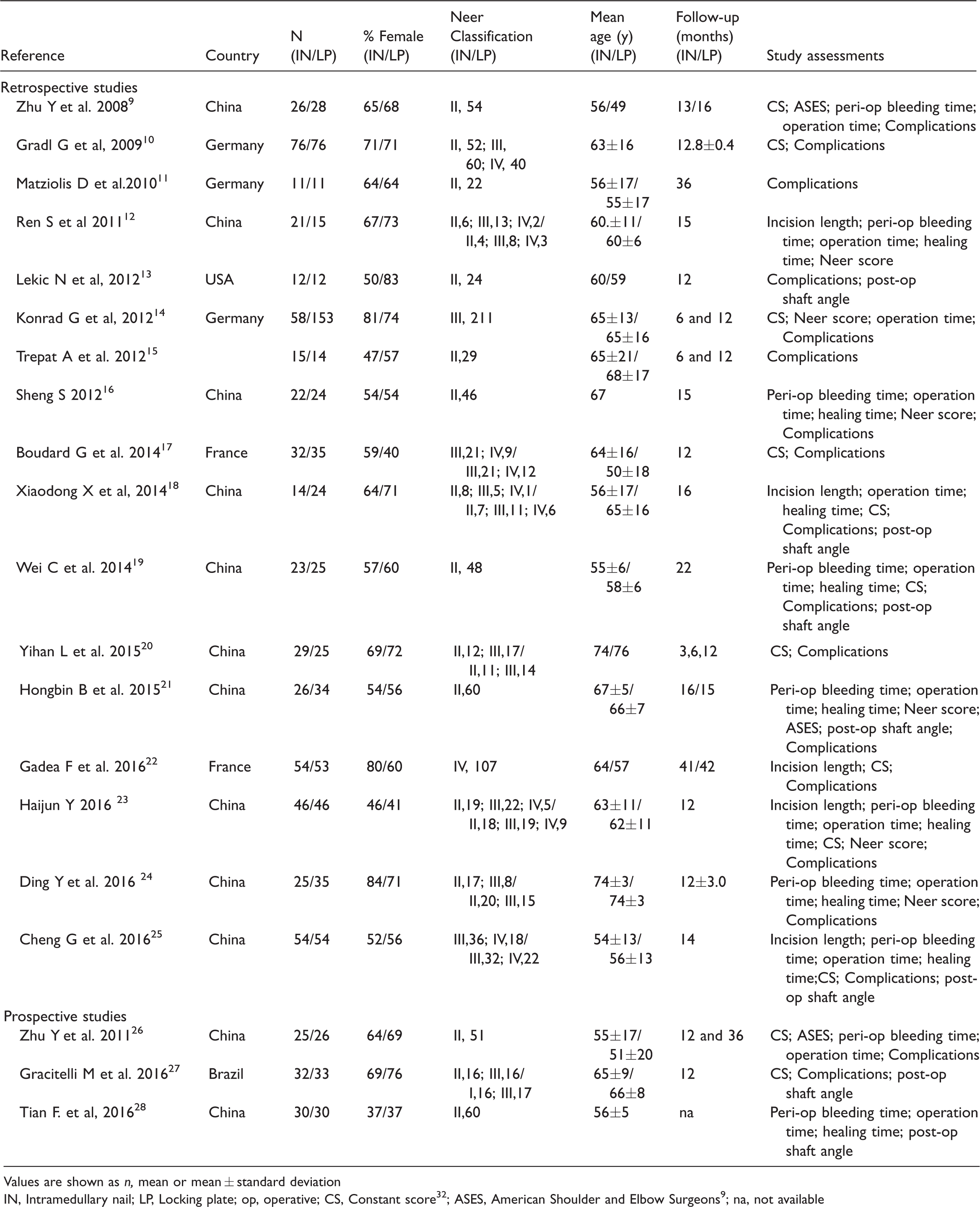
Values are shown as n, mean or mean ± standard deviation
Grading of Recommendations, Assessment, Development, and Evaluation (GRADE) evidence quality for each outcome 35 .

In total, 1384 patients with PHFs were involved in the 20 studies, (631 patients in the intramedullary nail group and 753 in the locking plate group). Individual sample sizes ranged from 22 to 211 patients, the male/female ratio was similar across the studies and mean ages ranged from 49 to 76 years (Table 1).
Using the Cochrane collaboration’s tool, 33 the methodological quality of the three randomised controlled trials26–28 was assessed. The three studies had low risk of random sequence generation and allocation concealment (i.e., selection bias) but had high risk of blinding of outcomes (i.e., attrition and detection biases).
The mean MINOR score from the 17 non-randomised studies9–25 was 16.7 (range, 15-17) which corresponded to a 70% score for the methodological quality of the included studies.
Five studies assessed incision length. Data from one study was separated into two parts according to Neer classification. 25 There was high heterogeneity between the results (I2=97%, P<0.05) and analysis showed that there was a statistically significant difference in incision length between the intramedullary nail group and the locking plate group (Figure 2). The incision length for the intramedullary nail group was shorter compared with that for the locking plate group.
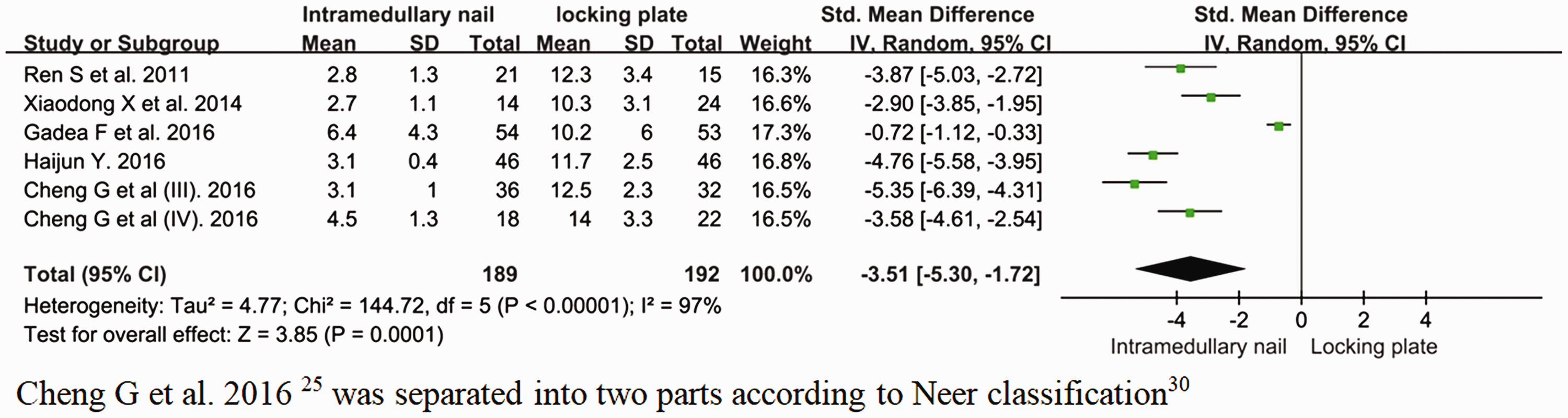
Forest plot for meta-analysis of incision length between the intramedullary nail and locking plate groups using random effects model. Data from studies that assessed this parameter.
Six studies of Neer type II fractures and four of Neer type II, III and IV fractures (one study was separated into two parts according to Neer classification. 25 ) reported peri-operative bleeding times. There was high heterogeneity between the studies (I2=94%, P<0.05) and analysis showed that there was a statistically significant difference in bleeding times between the intramedullary nail group and the locking plate group (Figure 3). The blood loss for the intramedullary nail group was less than that for the locking plate group.
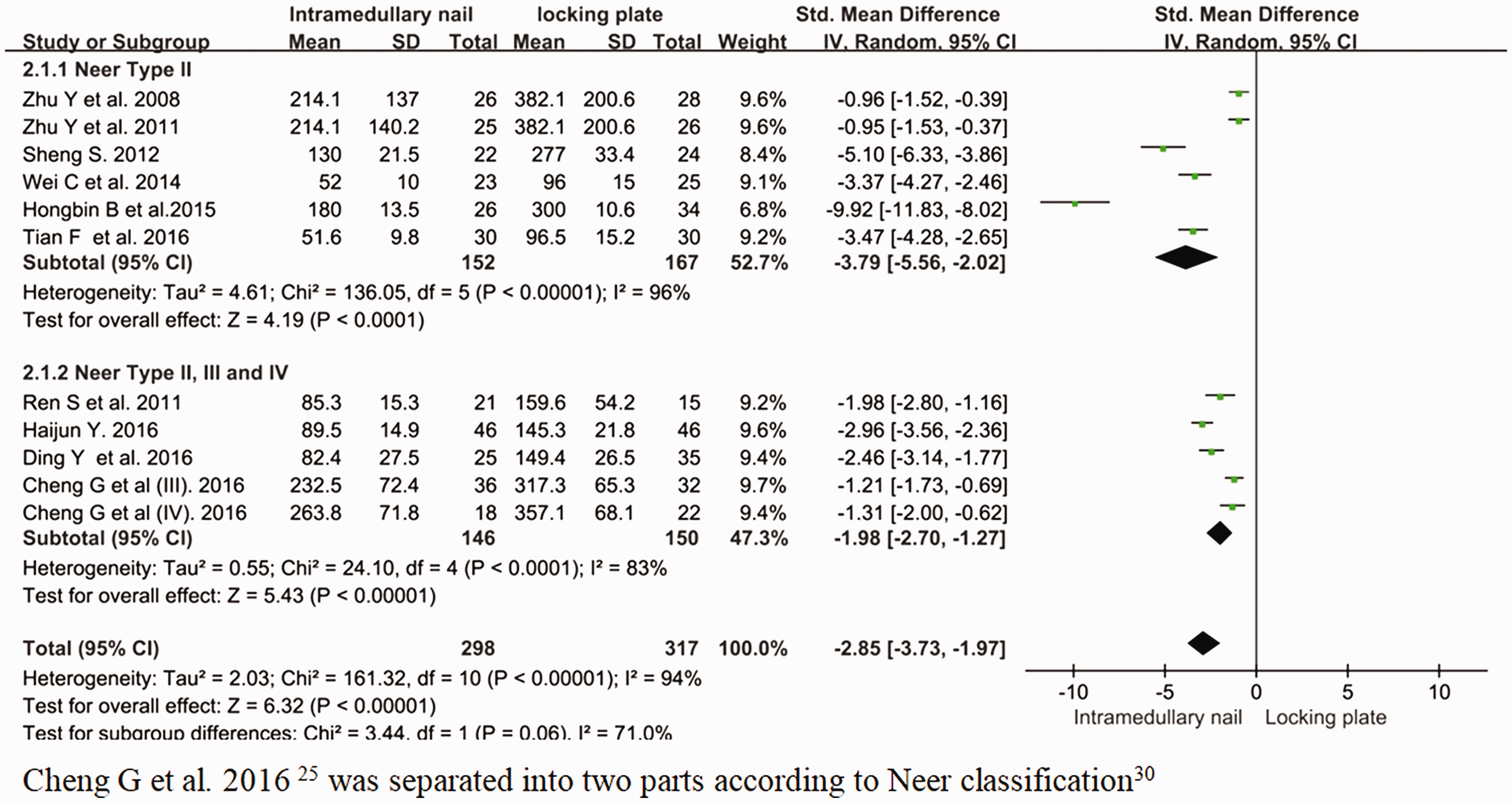
Forest plot for meta-analysis of peri-operative bleeding loss for the intramedullary nail and locking plate groups using random effects model. Data from studies that assessed this parameter.
Six studies of Neer type II fractures and six of Neer type II, III and IV fractures (one study was separated into two parts according to Neer classification. 25 ) reported operation time. There was high heterogeneity between the studies (I2=78%, P<0.05) and analysis showed that there was a statistically significant difference in operation time between the intramedullary nail group and the locking plate group (Figure 4). The operation time for the intramedullary nail group was shorter than for the locking plate group.

Forest plot for meta-analysis of operation time between intramedullary nail and locking plate groups using random effects model. Data from studies that assessed this parameter.
Four studies of Neer type II fractures and five of Neer type II, III and IV fractures (one study was separated into two parts according to Neer classification. 25 ) reported fracture healing time. There was high heterogeneity between the studies (I2 = 81%, P < 0.05) and analysis showed that there was a statistically significant difference in fracture healing times between the intramedullary nail group and the locking plate group (Figure 5). The fracture healing time for the intramedullary nail group was shorter than for the locking plate group.

Forest plot for meta-analysis of fracture healing time between intramedullary nail and locking plate groups using random effects model. Data from studies that assessed this parameter.
Three studies of Neer type II fractures and nine of Neer type II, III and IV fractures (one study was separated into two parts according to Neer classification. 25 ) reported Constant scores. There was low heterogeneity between the studies (I2=30%) and analysis showed that there was no statistically significant difference in Constant scores between treatment groups (Figure 6).

Forest plot for meta-analysis of Constant score between the intramedullary nail and locking plate groups using a fixed effects model. Data from studies that assessed this parameter.
Seven studies of Neer type II fractures and eleven of Neer type II, III and IV fractures reported post-operative complications. There was low heterogeneity between the studies (I2 = 40%) and analysis showed that there was no statistically significant difference in postoperative complications between treatment groups (Figure 7).

Forest plot for meta-analysis of post-operative complications between intramedullary nail and locking plate groups using a fixed effects model. Data from studies that assessed this parameter.
The above six outcomes were evaluated using the recommendations of the GRADE system 35 for level of evidence quality and the results were classed as ‘very low grade’ (Table 2).
Discussion
With the increasing aging population, PHFs have become one of the most common osteoporotic fractures seen in the elderly. 4 In recent years, intramedullary nails and locking plates have improved the surgical outcome of PHFs and have gradually replaced rigid internal fixation by conventional plates.9–28 However, there is currently no consensus in the literature on the best surgical technique for the different types of PHFs.
For routine Neer type II PHFs both intramedullary nails and locking plates have been shown to achieve good clinical results. 27 However, the use of these two methods for the treatment of complicated PHFs of type III and IV is a contentious issue. For example, one study reported intramedullary nail was not appropriate for Neer type III and IV PHFs because of the high rate of revision surgery required and low Constant score, 11 whereas, another study reported that intramedullary nail insertion for complicated PHFs produced satisfactory results. 37 Because surgeons, particularly those in less developed countries, often select techniques according to their personal preferences, it is important to provide an evidence base so that they can decide which is the best surgical method for the treatment of different types of PHF. To our knowledge, this current report is the first meta-analysis to use the GRADE system to evaluate results from studies comparing intramedullary nails and locking plates for PHFs. In addition, we evaluated data from different types of PHF which has not previously been considered. 29
Results from this current meta-analysis of 20 published reports suggested that although the fixation of PHFs with intramedullary nails or locking plates produced similar outcomes in terms of Constant score and post-operative complications, the incision length, blood loss, operation time and fracture healing time were significantly shorter for the intramedullary nail group. Moreover, these results were independent of the type of PHF. One study suggested that the decreased operation time for the intramedullary nail procedure may be related to the minimal invasive approach of the nail implant. 14 However, stabilizing the PHF before implanting the nail required longer radiographic screening compared with implanting the locking plate. 14 Another study suggested that the shorter operation time for implantation of the intramedullary nail resulted in less blood loss compared with implantation of the locking plate. 38
Post-operative complications following repair of PHFs are of serious concern and may include, pain, infection, nonunion, osteonecrosis, secondary fracture, screw breakage, rotator cuff injury and impingement syndrome.20,29 While some studies have reported pain scores 2-3 times greater in the locking plate group than the intramedullary nail group, 14 other studies have found more post-operative complications in the intramedullary nail group than in the locking plate group. 17 Each procedure is associated with inherent difficulties. For example, although the insertion of a locking plate for PHFs can reduce the risk of subacromial impingement syndrome and promote the recovery of shoulder function, due to its relatively larger volume, the procedure may cause iatrogenic injuries which may cause nonunion and avascular necrosis. In addition, although insertion of intramedullary nails can provide adequate fixation and favourable curative effects, defective surgery may damage important tendons and nerves and give rise to rotator cuff injuries and impingement syndromes. Moreover, intramedullary nails cannot be used in cases of severe osteoporosis. Some authors have suggested that the occurrence of post-operative complications following repair of PHFs are dependent on the experience and technique of the surgeon and not the surgical method. 15 Nevertheless, this current meta-analysis showed that, overall, there was no statistically significant difference between the surgical groups in the complication rate.
Using MINORS to assess the methodological quality of the included studies, a number of limitations of this meta-analysis were identified. For instance, poorly designed retrospective studies were more likely to suffer from various tapes of bias, especially publication bias including detection bias, selection bias, performance bias or attrition bias. In addition, due to the limited number of studies in the analysis, the potential difference between fixation with intramedullary nails and locking plates on Neer type III and IV PHFs could not be fully explored. Another limitation of the meta-analysis was that according to the GRADE recommendations for level of evidence quality, the results were classed as ‘very low grade’. 35
In summary, although the evidence quality was ‘very low’ in this meta-analysis because of clinical heterogeneity and limited information, the data tend to suggest that intramedullary nails may be superior to locking plated for the repair of PHFs. Further research is required and future studies should include analysis of assessments at 3, 6, 12 and/or 24 months and follow-up after removal of the implants.
Footnotes
Author contributions
M.L., and Y.H.W. conducted literature search and determined studies for exclusion and inclusion. M.L., M.Y., Y.P.Z., extracted data from the included studies, performed the meta-analysis, and drafted the manuscript. B.G.J., M.L., and P.X.Z. conceived the idea of the study, designed the study, and critically revised the manuscript for important intellectual content. All authors reviewed the paper and approved the final manuscript.
Acknowledgements
This work was funded by Chinese National Key Basic Research 973 Program (2014CB542201), Beijing science and technology new star cross subject (2018019), Chinese National Natural Science Foundation (31571235, 31771322) and Fund for Fostering Young Scholars of Peking University Health Science Centre BMU2017PY013). Peking University People's Hospital Research and Development Fund (RDY2016-07); National Keyresearch and Development Program (2016YFC1101604).
Declaration of conflicting interests
The authors declare that there are no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
