Abstract
Primary endometrial squamous cell carcinoma is an extremely rare tumor that tends to occur in postmenopausal women. We report on a 33-year-old woman who presented with a history of irregular vaginal bleeding for more than 2 years, and a vaginal mass for more than 1 month. Biopsy of the vaginal mass revealed an invasive poorly differentiated squamous cell carcinoma. The patient underwent radical hysterectomy, bilateral salpingo-oophorectomy, omentectomy, pelvic lymph node dissection, peritoneal sampling and vaginal tumor resection. On the basis of her medical history, auxiliary examination and postoperative pathology, the patient was diagnosed with stage IV endometrial squamous cell carcinoma. The patient was followed-up regularly and remained in good condition.
Keywords
Introduction
Primary endometrial squamous cell carcinoma (PESCC) is an extremely rare tumor defined as a primary carcinoma of the endometrium composed of squamous cells with varying degrees of differentiation, with a characteristic onset age, clinical manifestation, pathological diagnosis, treatment and prognosis. Since it was first reported by Gebhard in 1892, 1 only sporadic cases of PESCC have been reported, all in postmenopausal woman.2–4 Here, we report a case of PESCC in a woman of reproductive age at Hebei General Hospital, China.
Case report
A 33-year-old married woman presented with a history of irregular vaginal bleeding for more than 2 years and a vaginal mass for more than 1 month. She had been diagnosed with endometrial thickening 2 years previously. She had been taking a Chinese herbal medicine (composition unknown) for 1 year. The patient had no family history of cancer. A peanut-sized tumor had been detected at the vaginal orifice 1 month previously, and she reported that the tumor had enlarged obviously 10 days previously. The patient was therefore admitted to our hospital on 17 April 2017.
Gynecologic examination revealed a 4-cm-diameter tumor at the vaginal orifice. The tumor was attached to the vaginal wall with a cauliflower-like growth form, and was hard and susceptible to bleeding. The patient’s uterus was enlarged, corresponding to the size of a 4-month-pregnant uterus. Gynecologic ultrasonography confirmed that the uterus was enlarged, and the anterior wall of the cervix and lower segment of the anterior wall were hypoechoic (Figure 1a).
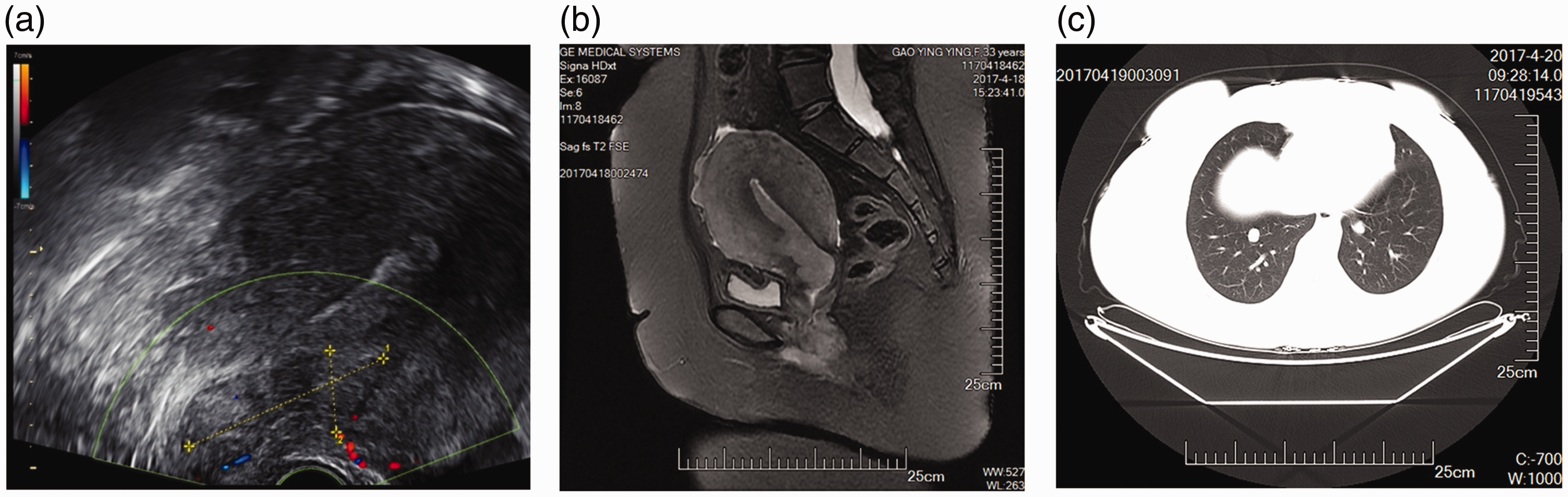
Preoperative examination. (a) Gynecological ultrasound image. (b) Pelvic magnetic resonance imaging scan. (c) Lung computed tomography (lung window) image.
Pelvic magnetic resonance imaging revealed that the mass involved the uterus, cervix and vaginal cavity, and a small amount of pelvic effusion. Lumps were present in the myometrium, some of which protruded out of the line of the uterus. The lymph nodes beside the iliac vessels appeared enlarged (Figure 1b). Computed tomography examination of the chest, liver, gallbladder, pancreas, spleen and kidney suggested the presence of multiple lymph node metastases in both the lungs and retroperitoneum (Figure 1c). Biopsy of the vaginal mass indicated that it was an invasive poorly differentiated squamous cell carcinoma, negative for SCC antigen and human papillomavirus (HPV). Her carbohydrate antigen 125 level was 80.09 U/mL.
The patient underwent radical hysterectomy, bilateral salpingo-oophorectomy, omentectomy, pelvic lymph node dissection, peritoneal sampling and vaginal tumor resection on April 21, 2017. During the operation, about 500 ml of bloody ascites was found in the abdominal cavity. Multiple nodules 1–3 cm in diameter, some ulcerated, were spread over the surface of the uterus. Her bilateral ovaries were enlarged to approximately 5 × 5 ×4 cm and were polycystic. Both Fallopian tubes were normal. The pelvic and aorta abdominalis lymph nodes were markedly enlarged (largest 5 × 3 × 2 cm) and adhered tightly to the blood vessels, with a rough surface. Dissection of the uterus revealed a brittle endometrium and invasion of the entire muscular layer by tumor tissues. Frozen pathological examination revealed invasive carcinoma in the corpus uteri.
Macroscopically, the uterus measured 10 × 11 × 7 cm, and the cervix was 3.5 cm long with an outer diameter of 2.5 cm. The endometrium was 0.1–1 cm thick, with local roughness covering 7 × 3.5 cm, and infiltrated into the uterine wall. The uterine wall was about 3.5 cm thick, with several nodules 0.5–3.5 cm in diameter in the section of the wall, with slightly harder grey and white matter (Figure 2a).

Postoperative pathological diagnosis. (a) Gross features of the uterus. (b) Histopathology of ascites. Hematoxylin–eosin staining, 100×. (c) Ki-67 immunohistochemistry (positive region 80%). 3,3′-Diaminobenzidine staining, 400×. (d) p53 immunohistochemistry. 3,3′-Diaminobenzidine staining, 400×.
Histochemical staining confirmed a poorly differentiated squamous cell carcinoma, with multiple intravascular tumor emboli. The full-thickness of the uterus wall was remarkable for tumor invasion. The tumor infiltrated into the mucosa and stroma of the inner cervical canal and the soft tissue of the right uterus. The cervix uteri showed mild chronic inflammation, with squamous epithelial hyperplasia, and partial glands with squamous metaplasia. Metastasis was found in the lymph nodes in the right and left obturator foramen. However, there was no cancer in the right iliac bone, right peritoneum of the pelvic wall, omental tissue or intraoperative washings (Figure 2b). Immunohistochemical analysis was positive for E-cadherin, Ki-67 (positive region 80%) (Figure 2c) and mutant p53 (Figure 2d), weakly positive for CK5/6, P63, CK7 and CK20, and negative for P40, HPV16, HPV18 and HPV31.
After consultation at the Cancer Hospital of the Chinese Academy of Medical Sciences, the patient was diagnosed with stage IV endometrial squamous cell carcinoma. The recommended treatment was paclitaxel (150–175 mg/m2) and cisplatin (60–70 mg/m2) for 2–3 days, combined with pelvic radiotherapy. Ten days after her operation, the patient was transferred to the cancer department for chemoradiotherapy. The patient was sensitive to chemotherapy and developed bone marrow suppression, nausea and vomiting and hair loss, but her liver and kidney function were unaffected. The patient was followed-up regularly and remained in good condition.
The patient provided written informed consent for participation in and for publication of this case report.
Discussion
The most common histological type of endometrial cancer is adenocarcinoma, followed by adenosquamous carcinoma, while PESCC is very rare. PESCC usually occurs in older or postmenopausal women, with similar clinical manifestations to adenocarcinoma. 5 Here, we present a rare clinical case of PESCC according to the criteria proposed by Fluhmann and the World Health Organization (WHO), which occurred in a 33-year-old patient of reproductive age.6,7
The etiology and pathogenesis of PESCC remains obscure, but a theory of endometrial squamous metaplasia is generally accepted. 8 PESCC has been associated with chronic pelvic inflammation, nulliparity, pyometra, estrogen levels and radiation.9,10 The current patient was admitted to our hospital because of scanty menstruation, and was diagnosed with polycystic ovary syndrome. In addition, the patient had high androgen levels and primary infertility, suggesting that high levels of androgens, infertility and scanty menstruation may be predisposing factors for PESCC.
HPV is known to be the main cause of cervical cancer, but its role in PESCC remains controversial. Although one study by Kataoka et al. 11 demonstrated HPV 31 in one patient with PESCC by polymerase chain reaction, HPV analysis of published PESCC case reports failed to find any evidence of HPV.8,12–15 Similarly, we found no signs of HPV in our patient, thus supporting the idea that HPV infection is not a causative factor for PESCC. In line with a report by Giordano et al., 15 we also detected mutant p53 expression in our patient, suggesting that mutation of the p53 tumor suppressor gene may be associated with PESCC. In addition, immunohistochemical analysis showed a high Ki-67 labelling index (80%) in the present case, in line with the aggressive and malignant nature of the lesion.
PESCC has a high malignancy grade and poor prognosis, with a 5-year survival rate of zero. The present patient had stage IV endometrial squamous cell carcinoma and was treated with surgery and chemotherapy. The chemotherapy reduced the size of the lymph node metastases in the lung, and imaging showed no recurrence of the pelvic lesions. However, although the effects of postoperative radiochemotherapy are better, patients with stage IV squamous cell carcinoma of the endometrium should be followed-up for a prolonged period.
In conclusion, PESCC is a rare type of endometrial carcinoma with an unclear etiology. The current case report indicated that PESCC can occur not only in postmenopausal women, but also in women of childbearing age, though its pathogenesis and therapeutic regimen remain controversial. Surgery combined with radiochemotherapy is considered to be the optimal therapy. Biological targeted therapy is also developing rapidly, and we suggest that combined biological therapy may further improve the adverse prognosis of PESCC.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
