Abstract
This present case report describes a 64-year-old female patient with type 2 diabetes mellitus who also had emphysematous pyelonephritis (EPN) and emphysematous cystitis (EC). Computed tomography revealed well defined emphysematous pyelonephritis and cystitis. Broad-spectrum antibiotic and percutaneous drainage of the right kidney were used as part of a conservative management regimen. The patient achieved clinical recovery and was discharged 12 days after admission. Furthermore, 13 other cases of EPC and EC that were reported between 1962 and 2017 were reviewed and discussed. The overall mortality was 15.4% (two of 13 patients), compared with 25% for EPN alone or 7.4% for EC alone as reported in the literature. The primary pathogen identified in the 13 patients was Escherichia coli (53.8%). All 13 patients were treated with antibiotics.
Introduction
Emphysematous pyelonephritis (EPN) is a type of severe renal infection that results in gas production in the renal parenchyma, collecting system, or perinephric tissue. 1 Almost 60–70% of cases are associated with uncontrolled diabetes mellitus. 2 EPN complicated by coexisting emphysematous cystitis (EC) is one category of EPN and if not treated promptly and properly, the clinical progress can be rapid, severe and life-threatening. 3
This present case report describes a 64-year-old female patient with type 2 diabetes mellitus with EPN complicated by coexistent EC. Computed tomography (CT) and laboratory evaluations confirmed EPN.
Case report
A 64-year-old female patient with type 2 diabetes mellitus who had been experiencing nausea, vomiting, and right flank pain for 7 days was admitted to the Department of Urology, First Hospital of Jilin University, Changchun, Jilin Province, China in November 2017. She had been suffering from type 2 diabetes mellitus for 20 years without systematic treatment. A physical examination revealed the following: temperature, 37.5°C; heart rate, 90 beats per minute; and blood pressure, 103/42 mmHg. Percussion in the right flank region elicited pain. Routine laboratory studies revealed the following: white cell count, 22.43 × 109/l; platelets, 15 × 109/l; fibrinogen, 8.0 g/l; K+, 2.9 mmol/l; glucose, 14.80 mmol/l; serum creatinine, 274.4 mmol/l; C-reactive protein, 179.03 mmol/l. The subsequent CT results showed gas in the right renal parenchyma (Figure 1a) and gas in the urinary bladder wall (Figure 1b).

Nonenhanced computed tomography (CT) images showing gas in the right kidney (red arrows) (a) and in the urinary bladder wall (red arrows) (b).
Empirical antibiotics (1.0 g meropenem intravenously every 8 h for 9 days), fluid resuscitation, control of blood glucose, and platelet transfusion were performed immediately after the diagnosis of EPN complicated by coexistent EC. The blood culture isolated gram-negative bacilli. Urine culture showed Candida albicans. After the inflammation was relieved, percutaneous drainage (PCD) of the right kidney was performed. The patient achieved clinical recovery and was discharged 12 days after admission.
Discussion
Emphysematous pyelonephritis is a severe necrotizing renal infection. 1 It was first described in 1898 and ‘emphysematous pyelonephritis’ was defined in 1962. 4 Mortality rates are reported to be up to 40–50%. 5 EPN complicated with EC is a rarer form of EPN. 3 This current case report describes a rare case of EPN complicated by coexistent EC. To date, there have been less than 15 cases of EPN complicated by coexistent EC reported in the literature as described below.
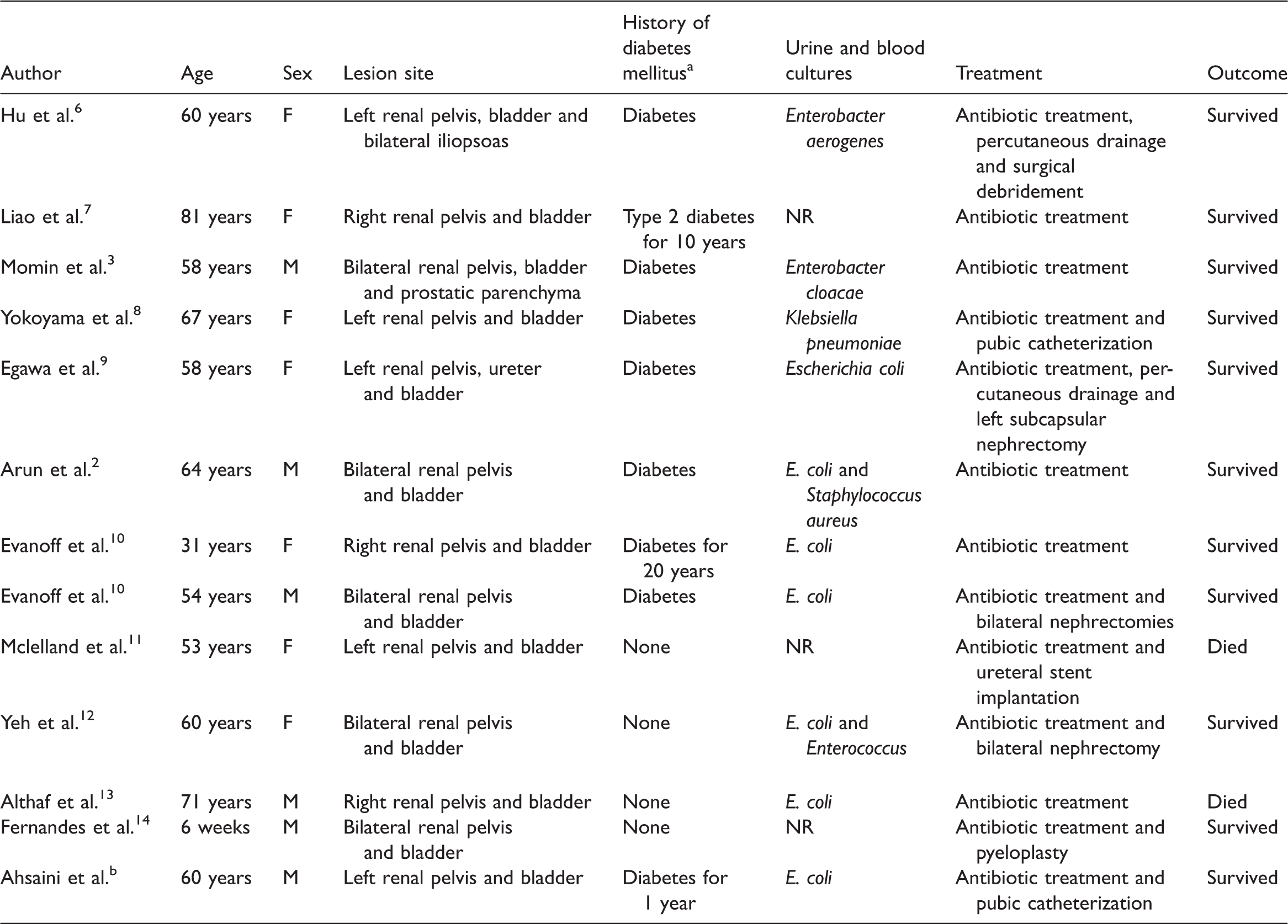
In order to review the epidemiology, theranostic and treatment strategies for EPN complicated with EC, a search of the PubMed®, Embase® and Google Scholar bibliographic databases was undertaken using the following search strategy: emphysematous (all fields), and pyelonephritis (all fields) or pyelonephritis (mesh term), and cystitis (all fields) or cystitis (mesh term). After filtering for unrelated results and duplicates, the data from 13 patients in 12 publications (one retracted) from 1962 to 2017 were collected and analysed (Table 1).2,3,6–14
aThe type of diabetes mellitus was not always stated.
bAlthough this article was retracted by the authors, this rare case was still worth analysing (Ahsaini M, Kassogue A, Tazi MF, et al. Emphysematous cystitis and emphysematous pyelitis: a clinically misleading association. Pan Afr Med J 2013; 16: 18).
F, female; NR, not recorded; M, male.
As shown in Table 2, the mean age of patients that were affected by EPN complicated by coexistent EC was 55 years. The overall mortality rate was 15.4% (two of 13 patients) compared with 25% for EPN alone 15 or 7.4% for EC alone. 16 Escherichia coli was the most common causative pathogen (53.8%; seven of 13 patients), compared with Enterobacter aerogenes (7.7%; one of 13 patients), Enterobacter cloacae (7.7%; one of 13 patients) and Enterococcus (7.7%; one of 13 patients). A history of diabetes mellitus was observed in the majority of patients (69.2%; nine of 13 patients). High blood glucose levels in patients with poorly controlled diabetes mellitus can provide gas-forming bacteria with a good environment. 3 Almost 95% of patients with EPN suffer from underlying uncontrolled diabetes, 17 67% patients with EC have diabetes, 16 and urinary tract obstruction has been observed in 29% of EPN patients. 15 However, diabetes mellitus is not related to mortality.5,17
Data presented as mean ± SD or n of patients (%).
aOne article was retracted by the authors, but the rare case was still worth analysing (Ahsaini M, Kassogue A, Tazi MF, et al. Emphysematous cystitis and emphysematous pyelitis: a clinically misleading association. Pan Afr Med J 2013; 16: 18).
A diagnosis of EPN can be established radiographically. On abdominal radiographs, gas in the renal parenchyma is often mistakenly identified as bowel gas. To demonstrate obstruction, retrograde pyelography is more appropriate than excretory urography because the function of the focal kidney is usually poor.18,19 Diagnosis of EPN relies on the reporting of gas patterns on CT scans. 1 CT can be used to estimate the extent of the emphysematous process and to guide disease management.18,20
Choosing the most appropriate treatment for EPN complicated with coexistent EC is very important if a cure is to be achieved. As gram-negative bacteria are the most common causative pathogens, the initial antibiotic therapy should target them using agents such as quinolones and cephalosporins. Once the results of the microbiological culture is available, then the antibiotics should be adjusted according to the type and individual sensitivities of the identified pathogen.16,21,22 The use of antibiotic treatment alone is related to a higher mortality risk when compared with the use of additional interventions such PCD of the abscess.15,23,24 As shown in Table 1, four of five (80.0%) patients treated with antibiotic alone survived, while seven of eight (87.5%) patients who received more extensive treatment regimens survived. Delayed elective nephrectomy may be required as a salvage procedure.14,25,26
In summary, this current case report described a rare case of EPN complicated by coexistent EC and presented the findings of a systematic review of the published literature regarding such cases. EPN complicated by coexistent EC is a rare and life-threatening urinary system infection. Diagnosis of EPN complicated by coexistent EC relies on the reporting of gas patterns in the urinary system on CT scans. Antibiotic treatment with additional interventions such as PCD appear to be more effective than the use of antibiotics alone. These findings provide guidance to physicians about how to treat patients with EPN complicated by coexistent EC.
Footnotes
Declarations of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was financially supported by the Graduate Innovation Fund of Jilin University (Grant No. 2017096).