Abstract
Oesophageal foreign bodies (OFBs) are a relatively common emergency in young children. OFBs are complicated by significant morbidity and mortality because their ingestion often occurs without witnesses, leading to a delay in diagnosis and treatment. We report an occult OFB in an 11-month-old infant who initially presented without any specific respiratory symptoms, mimicking a respiratory infection. Worsening of the patient’s cough, which did not show any improvement, despite treatment, and progressive onset of gastrointestinal manifestations (dysphagia, vomiting, and drooling) led to the diagnosis of an OFB (metallic spring). The complex and long-term clinical course of the patient highlights the need of promptly recognizing the presence of an occult OFB. This is because rapid diagnosis and treatment are essential for preventing severe and sometimes irreversible complications.
Introduction
Oesophageal foreign bodies (OFBs) are a relatively common emergency in young children. OFBs are often complicated by significant morbidity and mortality because their ingestion often occurs without a witness, leading to a delay in diagnosis and treatment. 1
We report here a case of an occult OFB in an 11-month-old infant who initially presented without any specific respiratory symptoms, but a respiratory infection was suspected. The infant’s cough worsened and did not improve, despite medical treatment. Progressive onset of gastrointestinal manifestations (dysphagia, vomiting, and drooling) led to the diagnosis of an OFB. This case is unusual because of the insidious presentation, which led to a delay in diagnosis and complicated treatment. Therefore, a non-standardized procedure, tailored to this specific case was applied, and this enabled endoscopic removal and preservation of the oesophagus.
Case Report
An 11-month-old female infant presented to our Paediatric Emergency Department (PED) with a 10-day history of metallic cough and intermittent fever. These symptoms were complicated by progressive dysphagia and episodes of mucus regurgitation accompanied by choking and dyspnoea in the last few days before admission. The symptoms started at the end of the flu epidemic season. Therefore, she was initially diagnosed by a general practitioner with a respiratory tract infection and treated with a 7-day course of antibiotics and a short-course of corticosteroids without any relief. During this course, she developed progressive dysphagia, initially for solid food, and then also for liquid food. In the last few days before admission, her parents reported nocturnal regurgitation of thick mucus followed by choking and dyspnoea. At the moment of admission to the PED, the patient was in a fair general condition, apyretic, and without any apparent signs of respiratory distress, but she had drooling and refused food intake. During a physical examination, she suddenly presented with an abrupt onset of coughing with a metallic sound and regurgitation of thick saliva and mucus. Pulse and oxygen saturation levels were within the normal range, while a thoracic examination showed bilateral rhonchi.
Therefore, chest radiography was performed and it showed a radiopaque OFB (Figure 1a). To better characterize the location of the OFB and its anatomical relationship with adjacent tissues, a chest computed tomography (CT) study was performed (Figure 1b). The CT scan confirmed a radiopaque OFB, which was a 2.5- x 1.5-cm spring with five helixes, and two of them were embedded in the oesophageal mucosa. The OFB appeared to be dislocated in the proximal oesophagus, and projected at the level of the thoracic vertebrae T2–T3 and leaned on the aortic arch. Cranially, the oesophagus appeared to be patent. No active parenchymal lesion or pleural effusion was found. Unfortunately, the presence of many artefacts did not allow study of the tracheal wall.
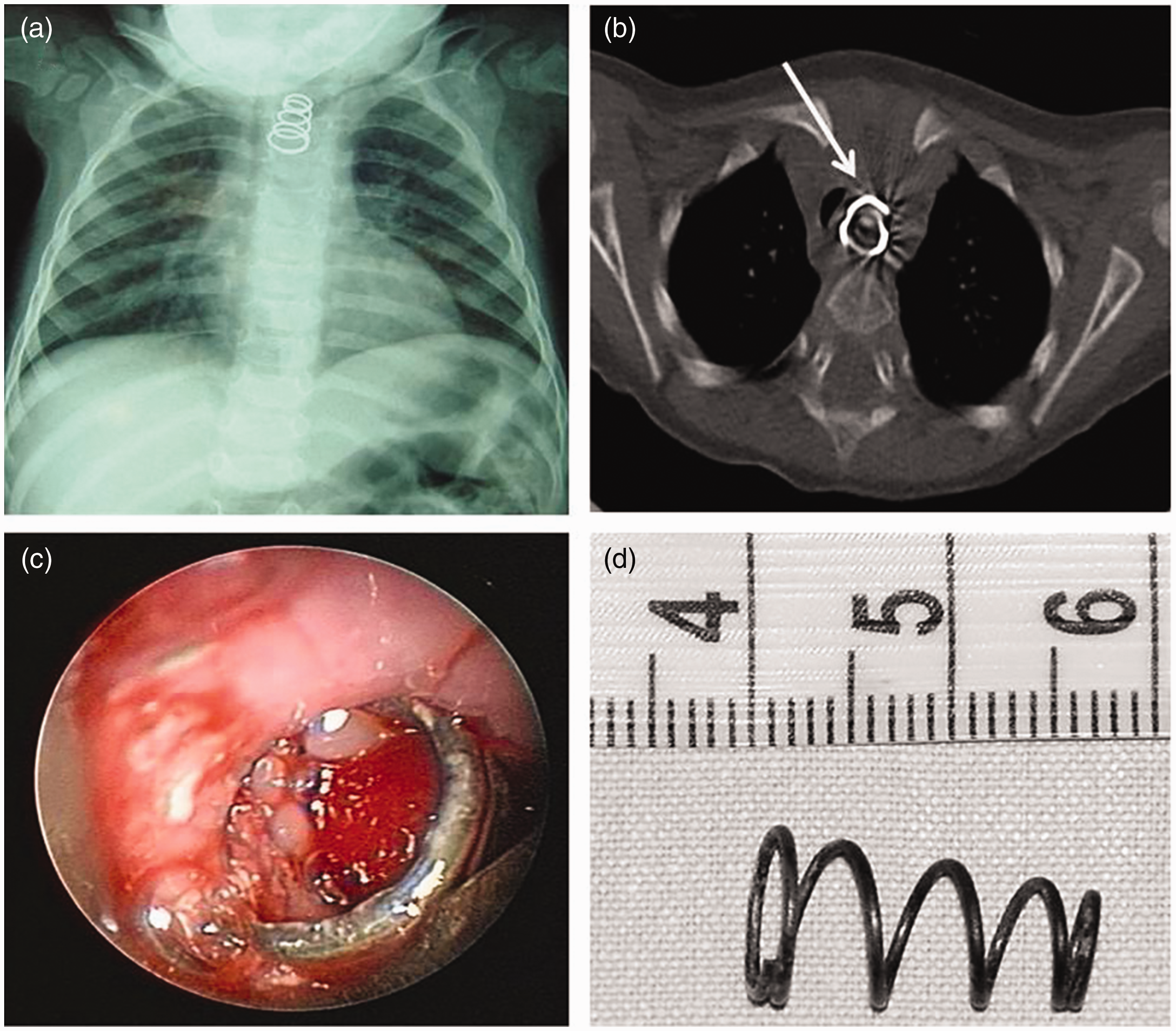
(a) Chest radiography showing the spring in the oesophagus; (b) computed tomography showing a high-density object; (c) oesophagoscopy showing considerable granulation tissue inside the spring; and (d) the removed spring
The patient was then referred to the Paediatric Anaesthesiology and Surgery Unit of a tertiary level PED. She underwent a rigid and then flexible oesophagoscopy, which showed considerable granulation tissue inside the spring (Figure 1c). Because of proximity of the spring to the aorta, consultation of a vascular and heart surgeon was requested during the procedure. The first attempt of endoscopic removal failed. With the aim of preserving the oesophagus and removing the OFB endoscopically, a laparoscopic plier was anchored to the spring and was rotated in the opposite direction of the spiral. This technique enabled successful endoscopic removal at the second attempt (Figure 1d). As expected, the oesophageal mucosa was seriously damaged by the caustic effect of rust. This resulted in oedema and surrounding granulating tissues, as well as almost complete erosion of the oesophageal wall (Figure 1c).
Total parenteral nutrition was provided for 2 weeks. The infant was then fed with enteral nutrition through nasogastric tubes and treated with a long-term course of antacids. Because of subsequent oesophageal stenosis, she underwent several endoscopic oesophageal dilations with Savary nasogastric tubes ((Savary-Gilliard dilator; Cook Medical, Bloomington, IN, USA) of increasing size (5-7-9 Ch). She was discharged after 2 months of hospitalization. Currently, after 19 endoscopic oesophageal dilations, she is in good general condition and has obtained acceptable food transit. The patient’s parents provided written informed consent to publish.
Discussion
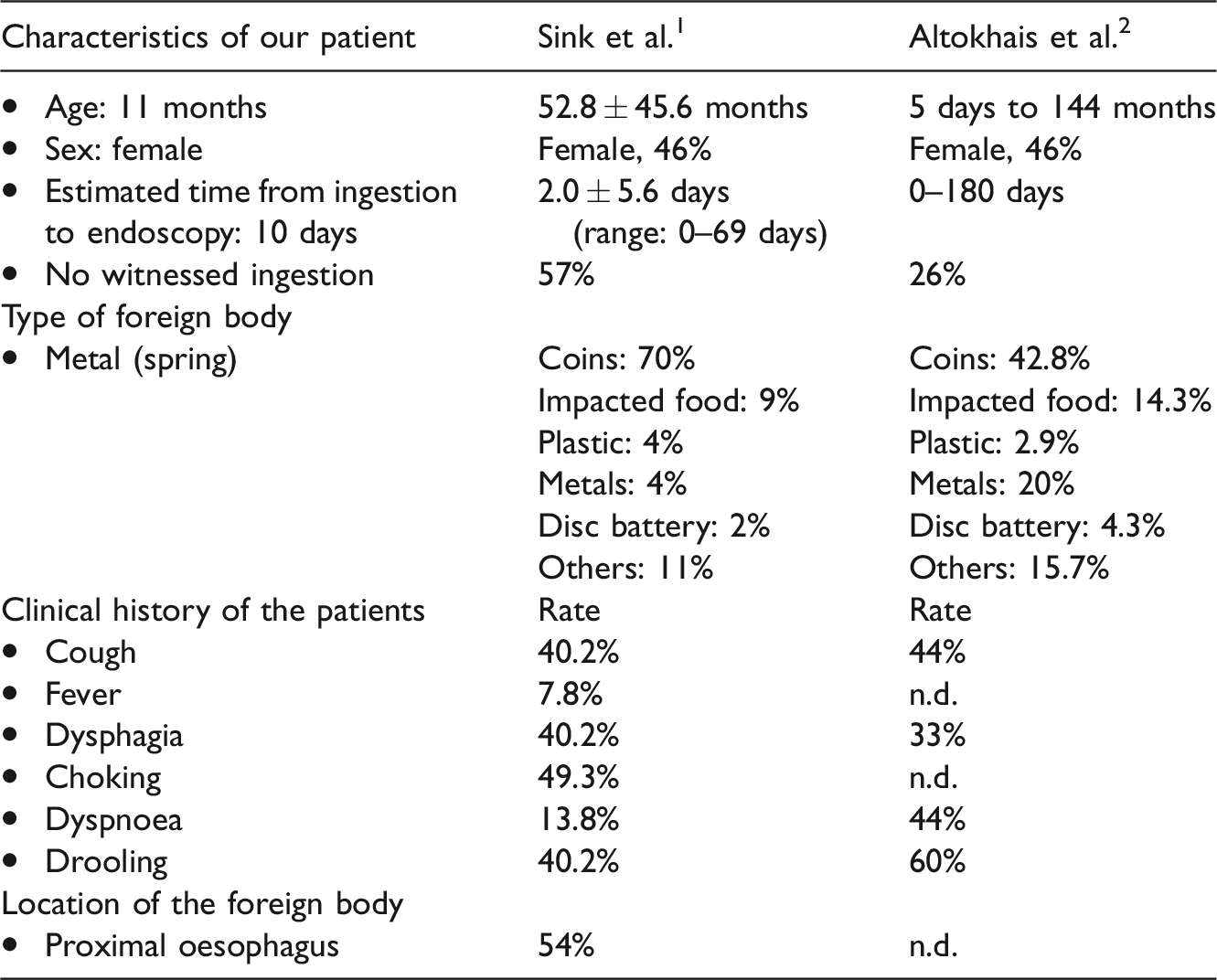
OFBs are relatively common in young children and are complicated by significant morbidity and mortality. 1 The most common characteristics, clinical history, and endoscopic findings of paediatric patients with OFBs are shown in Table 1.1,2
Abbreviation: n.d., not determined.
As shown in Table 1, the most common OFBs are coins (up to 70%), while metals (e.g., metallic spring ingested by our patient), were involved in 4% to 20% of cases. Despite the finding that button batteries are rare (2%–4.3% of OFBs) their effect on the oesophageal mucosa represents an endoscopic emergency because complications of caustic injury can quickly lead to oesophageal wall perforation, with dramatic and life-threatening consequences. 2
In case of foreign body ingestion not being witnessed, which occurs in up to 57% of cases and is typical in children younger than 4 years old, the clinical picture may be insidious. This can lead to a delayed diagnosis and to subsequent complications due to prolonged retention. 2 Therefore, the primary care physician should be aware that the combination of symptoms and signs (e.g., drooling, cough, and dysphagia) might be suggestive of ingesting a foreign body, even in the absence of a witnessed symptomatic event or ingestion. Our case, which unfortunately occurred at the end of the flu season, was misdiagnosed with a respiratory tract infection. This situation led to a delay in the final diagnosis. For this reason, the coexistence of respiratory symptoms (e.g., metallic cough and choking) and gastrointestinal manifestations (e.g., dysphagia, drooling, and vomiting) should be recognized as “red flags” and promptly alert the physician to exclude an OFB. 1
As shown in Table 1, OFBs are usually located in the upper oesophagus. 2 A chest radiograph should be the first-line investigation in suspected OFB cases because it can easily detect the presence of a radiopaque OFB. 3 Frontal and lateral radiographs are usually required to better locate and identify the nature of a radiopaque OFB. 4 Otherwise, radiolucent OFBs, which are less common than radiopaque OFBs, can only be detected through indirect findings (e.g., signs of airway compression). For this reason, if the presence of a nonradiopaque OFB is strongly suspected, contrast-enhanced oesophagography can be helpful. 4
Furthermore, CT evaluation can be useful for better characterizing the nature, shape, and anatomical location of the OFB. CT is also helpful for assessing possible complications of prolonged retention (e.g., abscesses, near-full or full-thickness erosion of the oesophageal wall) and the risks related to endoscopic procedures (e.g., oesophageal rupture). 4 Despite description of some non-endoscopic techniques (e.g., Foley balloon extraction, oesophageal bougienage), the endoscopic approach is still considered the gold standard procedure in treatment of an OFB. 5 While immediate removal of an OFB usually has an excellent prognosis, long-retained OFBs are associated with a high rate of complications, including perforation, abscesses, fistulae, and as in our case, stenosis.2,5 As previously reported, 2 in our case, endoscopic removal was seriously complicated by deep erosion of the oesophageal wall (Figure 1c). This situation required a non-standardized procedure, which involved using a pair of laparoscopic pliers to remove the spring with a rotational motion. This endoscopic technique, tailored for this specific case, allowed removal of metallic spring at the second attempt.
Because incorrect adult supervision is related to more frequent episodes of OFBs, prevention of accidental ingestion of OFBs in paediatric patients is still an important challenge for all general paediatricians. For this reason, educational tools (e.g., informative sheets) and informative campaigns should be provided to all families and safety measures should be verified at each visit to the doctors. 6
In conclusion, young patients with suggestive symptoms (drooling, chocking, dyspnoea, and dysphagia) should be promptly investigated with a chest radiograph to exclude the presence of an OFB, even in case the caregivers deny a symptomatic event or a witnessed ingestion. The complex clinical course of our patient highlights how early diagnosis and treatment are essential for preventing severe and sometime irreversible complications.
Footnotes
Authors’ contributions
EC conceived and drafted the manuscript, performed data acquisition and a literature search, and revised the manuscript; TG helped draft the manuscript, performed data acquisition and a literature search, and revised the manuscript; SB helped draft the manuscript, performed data acquisition, and revised the manuscript; PB helped draft the manuscript, performed a literature search, and revised the manuscript; ML and ML helped conceive the manuscript and drafted and revised the manuscript. All authors approved the final version of the manuscript.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Ethics
The manuscript complies with the current ethical considerations. The publication of intraoperative images is only authorized for scientific purposes.