Abstract
Objective
To investigate the potential antitumour effects of [2-(6-amino-purine-9-yl)-1-hydroxy-phosphine acyl ethyl] phosphonic acid (CP) against gastric adenocarcinoma.
Methods
Human BGC-823 xenotransplants were established in nude mice. Animals were randomly divided into control and CP groups, which were administered NaHCO3 vehicle alone or CP dissolved in NaHCO3 (200 µg/kg body weight) daily, respectively. Tumour volume was measured weekly for 6 weeks. Resected tumours were assayed for proliferative activity with anti-Ki-67 or anti-proliferating cell nuclear antigen (PCNA) antibodies. Cell apoptosis was examined using terminal deoxynucleotidyl transferase-mediated dUTP nick end labelling (TUNEL) assays and with caspase-3 immunostaining. Proteins were measured by Western blotting.
Results
There was a significant reduction in tumour volume and a reduced percentage of Ki-67-positive or PCNA-positive cells in the CP group compared with the control group. The percentage of TUNEL-positive or caspase 3-positive cells significantly increased following CP treatment compared with the control group. Tumours from the CP group had higher levels of phosphorylated-extracellular signal-regulated kinase (p-ERK) and phosphorylated-AKT (p-AKT) compared with control tumours.
Conclusion
CP treatment inhibited tumour growth and induced tumour cell apoptosis in a nude mouse model of BGC-823 gastric adenocarcinoma. Activation of the AKT and ERK signalling pathways may mediate this antitumour activity.
Introduction
Gastric carcinoma is a highly prevalent human disease and it is a leading cause of cancer-related deaths. For example, in 2012, there were approximately 951 600 newly diagnosed cases and 723 100 deaths due to gastric carcinoma. 1 Therapeutic treatments for gastric carcinoma typically involve surgery, chemotherapy, radiation therapy, or a targeted therapy.2,3 Despite considerable progress in the management of this disease, the prognosis of gastric carcinoma remains unsatisfactory. In addition, the toxicity and drug resistance associated with adjuvant therapies for gastric carcinoma support the urgent need for novel therapeutic strategies and drugs with improved effectiveness and reduced side-effects.
Bisphosphonates have been widely used for the treatment of bone disease due to their efficacy in inhibiting bone resorption. 4 The antitumour activity of bisphosphonates for the treatment of lung cancer, 5 colon cancer, 6 breast cancer, 7 prostate cancer, 8 and multiple myeloma 9 has also been demonstrated. Nevertheless, the therapeutic effects of bisphosphonates on gastric carcinoma remain poorly characterized. In our previous study, we synthesized a novel bisphosphonate derivative, [2-(6-amino-purine-9-yl)-1-hydroxy-phosphine acyl ethyl] phosphonic acid (referred to hereafter as CP). 10 CP efficiently suppressed the proliferation of four human gastric cancer cell lines in vitro, including BGC-823, SGC-7901, MKN-28, and MKN-45. 10 However, the potential for CP to mediate antitumour activity in vivo has not been fully investigated. It is recognized that the mechanism of the antitumour action by bisphosphonates is complex, as bisphosphonates may affect both tumour cells and tumour microenvironments, thereby yielding both direct and indirect antitumour activities. 11 Consequently, various factors and signalling pathways are involved.
In this present study, a xenotransplant model of human gastric adenocarcinoma was established in nude mice with the human gastric cancer cell line BGC-823. The effects of CP on tumour growth and apoptosis were subsequently examined. Associations between CP-mediated antitumour activity and phosphatidylinositol 3 kinase (PI3K)/protein kinase B (AKT) and mitogen-activated protein kinases (MAPK) signalling were also examined, since both pathways regulate various cellular functions, including cell proliferation, invasion, metastasis, and apoptosis.12,13
Materials and methods
Reagents
The School of Pharmaceutical Chemistry, Hebei Medical University, Shijiazhuang, China kindly provided CP. The chemical structure of CP has been described previously. 10
Cell culture
Human gastric adenocarcinoma BGC-823 cells were purchased from the American Type Culture Collection (Manassas, VA, USA). Cells were cultured in RPMI-1640 culture medium supplemented with 10% fetal bovine serum, 1% nonessential amino acids, and antibiotics. Cell cultures were maintained in a 5% CO2 incubator with controlled temperature and humidity.
Animals
Four-week-old female BALB/c nude mice (15-,17 g) were obtained from the Beijing Vital River Laboratory Animal Technology Company (Beijing, China). All animals were housed under specific pathogen free/viral antibody free conditions. Two or three mice were housed per cage at 22°C (12-h light/12-h dark cycle) with free access to food and water. Animal experiments were conducted according to the Guidelines of Animal Experiments from the Committee of Medical Ethics, National Health Department of China, and the procedures were approved by the Animal Ethics Committee of Hebei Medical University (2013-012).
Establishment of tumour-bearing nude mice and drug administration
To establish a xenotransplant model of human gastric adenocarcinoma, BGC-823 cells were washed with 10 mM phosphate-buffered saline (PBS; pH 7.4) and collected after trypsin digestion. Intraperitoneal (i.p.) injections were made in the left armpit of nude mice and included a total of 2 × 106 cells resuspended in 0.2 ml 10 mM PBS (pH 7.4) per inoculation. When an obvious tumour mass was observed, these animals were randomly divided into a control group and a CP group (six mice/group). The latter was administered CP dissolved in NaHCO3 at a concentration of 200 µg/kg body weight via an i.p. injection into the enterocoelia as described previously. 10 The injections were administered daily for 44 days. In parallel, the control group was administered the same volume of NaHCO3 solution (vehicle solution). The width and length of each tumour mass was measured every three days using a vernier calliper. Tumour size was calculated as: width 2 × length/2. After approximately 6 weeks of treatment, the animals were sacrificed and each tumour was carefully resected. Half of each tumour was fixed in 4% formalin for histological, immunohistochemical, and terminal deoxynucleotidyl transferase-mediated dUTP nick end labelling (TUNEL) assays. The other half of the tumour was immediately immersed in liquid nitrogen and then stored at –80°C for Western blotting analysis.
Histological analysis
Fixed tumour tissues were embedded in paraffin wax and sectioned. For routine histological examination, 5-µm-thick sections were stained with haematoxylin and eosin.
TUNEL assay
Cell apoptosis in 5-µm tumour tissue sections was examined by TUNEL assay with a commercially available In Situ Cell Death Detection Kit, Fluorescein (Roche Diagnostics, Mannheim, Germany). Nuclei were stained with haematoxylin. TUNEL-positive cells were counted using a Zeiss Axioplan 2 fluorescence microscope (Carl Zeiss Microscopy, München, Germany). For data quantification, at least four non-overlapping fields were selected and the mean number of TUNEL-labelled cells was divided by the total number of cells counted in 40 micrographs.
Immunohistochemical analyses
Specimens were fixed in 4% paraformaldehyde and 5-µm-thick sections were obtained from the embedded blocks and examined under light microscopy (BX-UCB; Olympus, Tokyo, Japan). The sections were deparaffinized, rehydrated, and incubated in 3% H2O2 to eliminate endogenous peroxidase activity. After rinsing in 10 mM PBS (pH 7.4), the sections were treated with blocking serum and then incubated with primary antibody for Ki-67 and proliferating cell nuclear antigen (PCNA) (Santa Cruz Biotechnology, Santa Cruz, CA, USA). Primary antibodies were diluted to 1:100 using 10 mM PBS (pH 7.4) and incubated overnight at 4°C, then the sections were washed with 10 mM PBS (pH 7.4) three times. The sections were then incubated with horseradish peroxidase rabbit antimouse secondary antibody (Santa Cruz Biotechnology) diluted in 10 mM PBS (pH 7.4) for 20 min at 37°C according to the manufacturer’s instructions. After washing the sections with 10 mM PBS (pH 7.4) three times, the sections were then incubated with SABC reagent (Strept Avidin Biotin-peroxidase Complex method; Sigma-Aldrich, St Louis, MO, USA). Peroxidase activity was identified by the reaction with diaminobenzidine according to the manufacturer’s instructions. Results were expressed as the mean optical density of 10 random fields for each slide using a digital medical image analysis system (Motic Medical 6.0 Digital Medical Image Analysis System; Motic, Xiamen, China).
Western blotting
Tumour tissues were homogenized with lysis buffer containing 0.1 mM phenylmethylsulphonyl fluoride, 200 mM HEPES (pH 7.4), 1 mM dithiothreitol, 250 mM sucrose, 10 mM KCl, 1.5 mM MgCl2, 1 mM ethylene glycol-bis(β-aminoethyl ether)-N,N,N',N'-tetraacetic acid, 1 mM ethylenediaminetetra-acetic acid, and 1% protease and phosphatase inhibitor cocktails (Sigma-Aldrich). The tissue samples were then centrifuged at 10 000 g for 10 min at 4°C and supernatants were collected (Eppendorf, Hamburg, Germany). Total protein concentrations were determined using a ProteoPrep® Total Extraction Sample Kit (Sigma-Aldrich). Equal amounts of protein (80 µg) were separated by 10% sodium dodecyl sulphate–polyacrylamide gel electrophoresis (Invitrogen, Carlsbad, CA, USA). The proteins were then electrotransferred to a polyvinylidene difluoride membrane (Millipore, Billerica, MA, USA). After blocking with 5% nonfat dry milk dissolved in 10 mM PBS (pH 7.4), the membrane was probed with primary antibodies raised against pro-caspase 3, activated-caspase 3, pro-caspase 9, activated-caspase 9, AKT, phosphorylated-AKT (p-AKT), extracellular signal-regulated kinase (ERK), phosphorylated-ERK (p-ERK), p38, phosphorylated p38 (p-p38), c-Jun N-terminal kinase (JNK), phosphorylated-JNK (p-JNK), and β-actin (Santa Cruz Biotechnology) at dilutions ranging from 1:1000 to 1:500 according to the manufacturer’s instructions. After incubating the membranes with the appropriate primary antibodies for 3 h at room temperature, or overnight at 4°C, the membranes were washed three times with Tris-buffered Tween-20 buffer (50 mM Tris pH 7.5, 500 mM NaCl, and 0.05% Tween 20) at room temperature. The membranes were then incubated with horseradish peroxidase-conjugated anti-immunoglobulin G secondary antibodies (goat antirabbit or goat antimouse antibodies; Santa Cruz Biotechnology) diluted in 10 mM PBS (pH 7.4) for another 2 h at room temperature according to the manufacturer’s instructions. Bound antibodies were visualized using an enhanced chemiluminescence kit (GE Healthcare, Piscataway, NJ, USA). Integrated signal densities of the target bands were quantified with Quantity One software (Bio-Rad, Hercules, CA, USA) and relative protein expression was normalized to β-actin levels.
Statistical analyses
All statistical analyses were performed using the SPSS® statistical package, version 12.0 (SPSS Inc., Chicago, IL, USA) for Windows®. Results are expressed as the mean ± standard error of the mean (SEM). Comparisons between the two groups were made with Student’s t-test. Tumour sizes for the experimental groups were compared with analysis of variance. A P-value <0.05 was considered statistically significant.
Results
To clarify the potential antitumour activity of CP in vivo, a xenotransplant model of human gastric adenocarcinoma was established in nude mice with BGC-823 cells (Figures 1a and 1b). Animals were administered CP or a vehicle control daily via i.p. injection for 44 days. Six weeks later, no significant difference in food intake or weight gain was observed between the two experimental groups (data not shown). In addition, the animals appeared to tolerate the CP injections and no drug-induced toxicities were observed during the experimental period. However, mice in the CP group exhibited a significant reduction in tumour volume after 24 days compared with the control group (P < 0.05) (Figure 1c). Histological examination revealed that treatment with CP greatly increased tumour cell death, and this was accompanied by an irregular shape and condensed nuclei phenotype for the BGC-823 tumour cells (Figure 2). Currently, Ki-67 and PCNA are standard proliferative indices that have been widely applied for determinations of tumour cell proliferation.14,15 In the immunohistochemical analyses that were performed with specific antibodies raised against Ki-67 and PCNA, the control sections were found to exhibit greater tumour cell proliferation compared with the CP-treated specimens (Figure 3a). Specifically, the mean ± SEM percentages of Ki-67-positive and PCNA-positive cells were significantly lower in the CP-treated mice compared with the percentages in the control mice (Ki-67: control, 81.7 ± 10.7%; CP, 25.7 ± 4.5%; P < 0.05; PCNA: control, 86.7 ± 8.5%; CP, 23.8 ± 5.7%; P < 0.05) (Figure 3b).

Administration of CP inhibited the growth of BGC-823 tumours established in nude mice. Animals bearing gastric adenocarcinoma BGC-823 tumours received injections of CP (200 µg/kg body weight) or 0.16% NaHCO3 vehicle control (six mice/group). Images of the gross morphology of the two experimental groups (a) and their tumour masses (b) after 6 weeks of treatment are shown. (c) Tumour volume was measured and the mean tumour volume (mm3) was calculated on the indicated day after CP or vehicle solution injections were performed. Results are expressed as mean ± SEM. CP, [2-(6-amino-purine-9-yl)-1-hydroxy-phosphine acyl ethyl] phosphonic acid. *P < 0.05 versus vehicle control; analysis of variance.

Representative photomicrographs of sections of gastric adenocarcinoma BGC-823 tumours established in nude mice following approximately 6 weeks of treatment with CP (200 µg/kg body weight) or 0.16% NaHCO3 vehicle control (six mice/group). Haematoxylin and eosin; scale bar, 50 µm. CP, [2-(6-amino-purine-9-yl)-1-hydroxy-phosphine acyl ethyl] phosphonic acid. The colour version of this figure is available at: http://imr.sagepub.com.

Immunohistochemical analysis of Ki-67 and proliferating cell nuclear antigen (PCNA) levels in tumour samples. (a) Representative photomicrographs of tumour sections of gastric adenocarcinoma BGC-823 tumours established in nude mice following approximately 6 weeks of treatment with CP (200 µg/kg body weight) or 0.16% NaHCO3 vehicle control stained with anti-Ki-67 or anti-PCNA antibodies (six mice/group). Cells with brown staining were considered immunopositive. Scale bar, 50 µm. (b) The mean ± SEM percentage of immunopositive cells. *P < 0.05 versus control; Student’s t-test. CP, [2-(6-amino-purine-9-yl)-1-hydroxy-phosphine acyl ethyl] phosphonic acid. The colour version of this figure is available at: http://imr.sagepub.com.
With regard to the induction of tumour cell apoptosis, administration of CP greatly increased the number of TUNEL-positive cells compared with the control group (P < 0.01) (Figures 4a and 4b). In addition, the levels of cleaved caspase 3 and cleaved caspase 9 proteins were significantly increased in the tumour tissues examined from the CP group compared with the control group (P < 0.05) (Figures 4c and 4d).
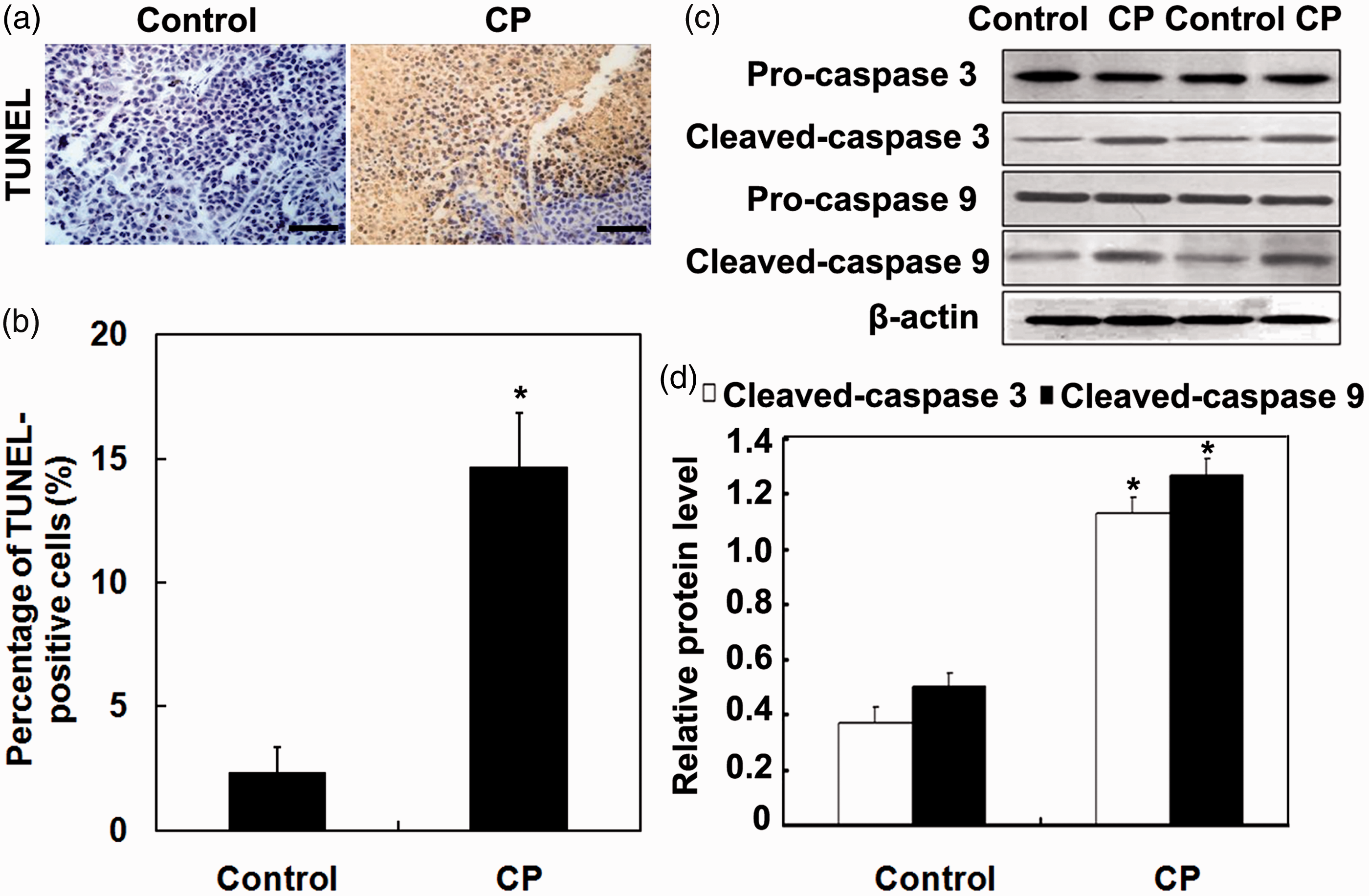
Effects of CP on tumour cell apoptosis. (a) Representative photomicrographs of tumour sections of gastric adenocarcinoma BGC-823 tumours established in nude mice following approximately 6 weeks of treatment with CP (200 µg/kg body weight) or 0.16% NaHCO3 vehicle control stained with terminal deoxynucleotidyl transferase-mediated dUTP nick end labelling (TUNEL) (six mice/group). Scale bar, 50 µm. (b) The mean ± SEM percentage of TUNEL-positive cells was calculated. (c) Western blotting analysis of the pro- and cleaved forms of caspase 3 and caspase 9. (d) Mean ± SEM relative protein levels of cleaved caspase-3 and cleaved caspase-9 were normalized to β-actin (internal control). *P < 0.05 versus control; Student’s t-test. CP, [2-(6-amino-purine-9-yl)-1-hydroxy-phosphine acyl ethyl] phosphonic acid. The colour version of this figure is available at: http://imr.sagepub.com.
To elucidate the molecular mechanism(s) that may mediate tumour growth suppression and cell apoptosis induced by CP in this animal model, protein levels of several crucial regulators of the PI3K/AKT and MAPK signalling pathways were determined. As shown in Figure 5, the overall protein levels of AKT, p38, JNK, and ERK were unchanged by CP treatment compared with the control group. Moreover, there was no significant difference in the levels of activated (i.e. phosphorylated) p38 or JNK between the two experimental groups. However, higher levels of both p-AKT and p-ERK were observed in the CP group compared with the control group.
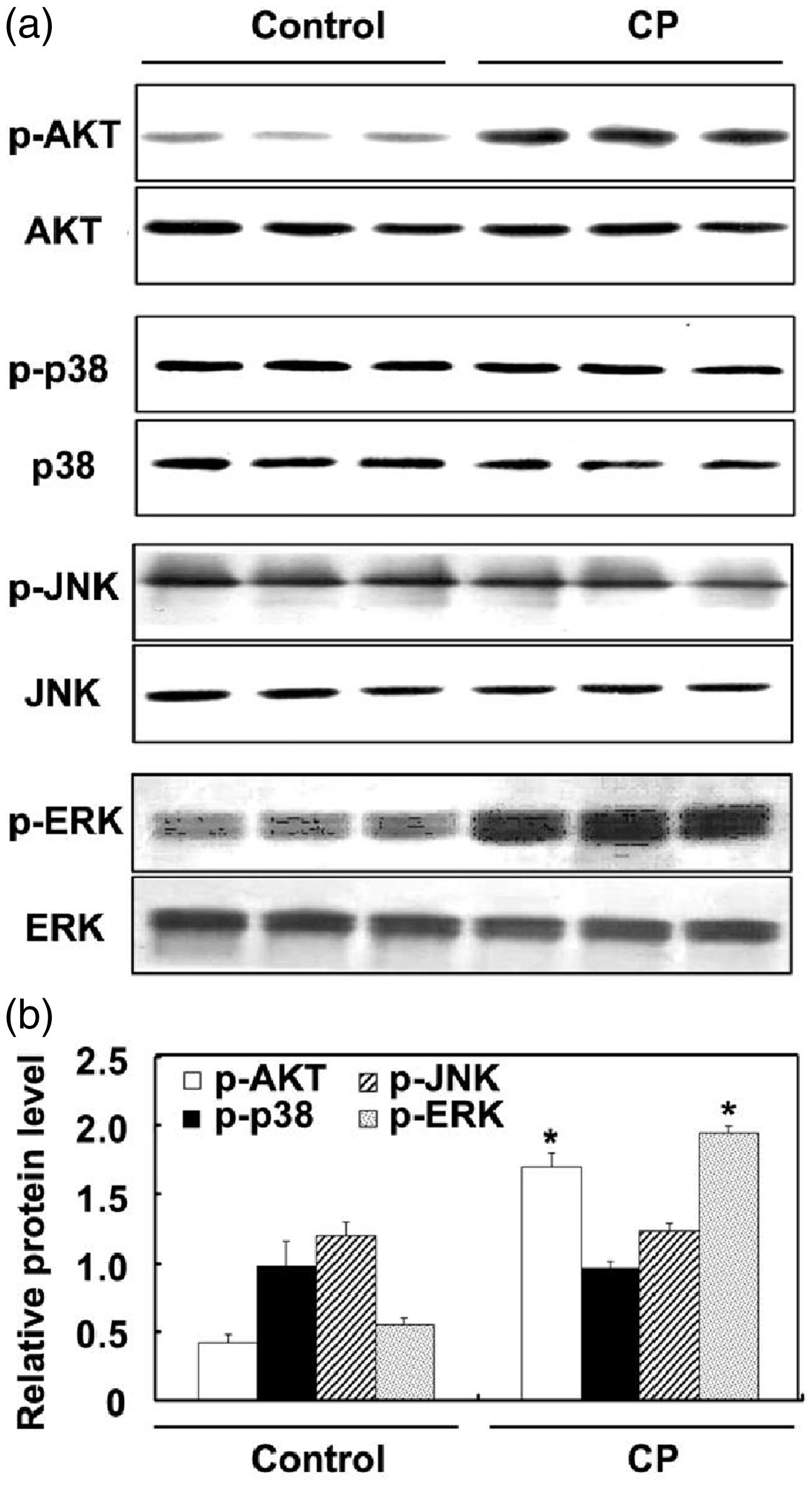
Western blotting analysis of the levels of proteins regulating the phosphatidylinositol 3 kinase (PI3K)/protein kinase B (AKT) and mitogen-activated protein kinase (MAPK) pathways in BGC-823 tumours established in nude mice following approximately 6 weeks of treatment with CP (200 µg/kg body weight) or 0.16% NaHCO3 vehicle control. (a) After 6 weeks of CP and control treatments, levels of the phosphorylated and unphosphorylated forms of AKT, p38, c-Jun N-terminal kinase (JNK), and extracellular signal-regulated kinase (ERK) were detected in tumour samples collected from each of the experimental groups by Western blotting analysis (six mice/group). Representative immunoblots are shown. (b) Mean ± SEM relative levels of p-AKT, p-p38, p-JNK, and p-ERK were normalized to those of AKT, p38, JNK, and ERK, respectively. *P < 0.05 versus control; Student’s t-test. CP, [2-(6-amino-purine-9-yl)-1-hydroxy-phosphine acyl ethyl] phosphonic acid.
Discussion
When this present study examined the antitumour effects of CP in a xenotransplant model of gastric carcinoma in nude mice, it demonstrated that CP inhibited tumour growth and induced tumour cell apoptosis. It was subsequently hypothesized that the AKT and ERK signalling pathways contributed to the antitumour actions of CP.
The effects of bisphosphonates on bone have previously been characterized, while the antitumour activities of bisphosphonates have been gaining increasing attention. 16 For example, in a recent study, the potential for bisphosphonates to treat cancers in the digestive system was demonstrated. 17 However, the use of bisphosphonates for the management of gastric carcinoma still lacks adequate evidence. This present study demonstrated that daily intraperitoneal injections of a novel bisphosphonate derivative, CP, significantly reduced the in vivo growth of human gastric adenocarcinoma BGC-823 tumours in nude mice. Moreover, after 6 weeks of CP treatment, the proliferative ability of the tumour cells was greatly reduced. It has been indicated that the bisphosphonate, zoledronic acid, suppresses cell proliferation by inducing S phase arrest18,19 or by perturbing the activities of cyclin and Ras. 20 Therefore, it is possible that the antitumour action mediated by CP is related to adverse influences of CP on the cell cycle of BGC-823 gastric carcinoma cells.
Administration of CP was also associated with a dramatic induction of cell apoptosis based on the increased number of TUNEL-positive cells that were detected in the tissues obtained from tumour-bearing mice. It has been demonstrated that caspase-3 and caspase-9 play pivotal roles in modulating the intrinsic apoptotic process. 21 Here, increased levels of cleaved caspase-3 and cleaved caspase-9 were observed in the tumour tissues of the CP-treated tumour-bearing mice. Thus, CP treatment may activate the mitochondrial apoptotic pathway by regulating initiators of the pathway, such as caspase-3 and caspase-9. However, the possible involvement of extrinsic apoptosis in the CP-induced apoptotic pathway cannot be ruled out.
The PI3K/AKT and MAPK signalling cascades play universal roles in mammalian cells, and they also regulate several biological activities in various types of tumour cells, including gastric carcinoma cells.22–25 In this present study, protein levels of the main regulators in these pathways, including AKT for the PI3K/AKT pathway and p38, JNK, and ERK for the MAPK signalling pathway, 26 were compared between the CP and control groups. Among these regulators, CP markedly activated AKT and ERK signalling, while the other regulators that were examined remained unaffected. Similarly, increased levels of p-ERK were previously reported in SGC-7901 gastric cancer cells that were exposed to CP both in vitro and in vivo. 10 In combination with the present findings, these data suggest that ERK may represent a novel target for antitumour therapy of gastric carcinoma. Regarding the AKT signalling pathway, aberrant activation of AKT has been detected in gastric cancer tissues, as well as in gastric cancer cell lines. 27 In contrast with the potential carcinogenic role for PI3K/AKT that was recently described,28,29 an increase in p-AKT levels were detected in the CP-treated gastric tumours in the present study. Activation of AKT has also been closely associated with caspase-9 activity in gastric carcinoma. 30 Thus, it is possible that CP may induce caspase-9- and caspase-3-dependent apoptosis via activation of AKT signalling in gastric carcinoma cells. However, the present results do not exclude the possibility that CP may mediate inhibition of tumour growth and cell apoptosis via other signalling pathways. For example, bisphosphonates have been found to induce cell cycle arrest and trigger cell apoptosis by blocking signalling by human epidermal growth factor receptors. 31 In addition, autophagic cell death potentially plays an essential role in executing the death of gastric carcinoma cells, 32 while the potential influence of bisphosphonates on cellular autophagy remains unknown. Therefore, further studies are needed to distinguish these possibilities.
In conclusion, the present results demonstrate that the bisphosphonate derivative, CP, was associated with antitumour activity in nude mice bearing BGC-823 gastric adenocarcinoma tumours, and such action may be associated with its capacity to modulate the PI3K/AKT and MAPK/ERK signalling cascades. In various human malignancies, the inhibitory effects of bisphosphonates have been widely observed. However, the safety of this group of agents remains to be carefully determined considering the adverse effects reported for these agents, including gastric disturbance, particularly with the use of oral preparations of bisphosphonates. 33
Footnotes
Acknowledgement
The authors would like to thank Ye Jiang from Hebei Medical University, China, for providing CP.
Declaration of conflicting interests
The authors declare that there are no conflicts of interest.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: publication of this paper was funded by the National Natural Science Foundation of China (No. 81072033; No. 81500317), the Key subjects of Hebei Health Department (No. 20170600) and Hebei Natural Science Foundation (No. H2017423033).
