Abstract
Objectives
Early recognition of acute myocardial infarction (AMI) and early activation of emergency medical services (EMS) are essential to reduce delays in patient care. We investigated public awareness of the need to call EMS at onset of AMI and evaluated associated factors.
Methods
In January 2008, a nationwide population-based survey using quota sampling was conducted in Japan. The primary outcome measure was responsiveness to promptly calling EMS at AMI onset, subdivided by on-time (daytime) and off-time (nights and holidays) hours.
Results
In total, 1200 participants were surveyed. Their mean age was 46.3 years (standard deviation, 17.4), and 50.3% (n=604) were women. A total of 11.6% (n=139) answered that they would call EMS during on-time hours, and 27.5% (n=330) stated that they would call during off-time hours. Multivariable analysis showed that the participants’ age, female sex, education level, and self-confidence regarding their understanding of AMI were significant associated factors. The associated factors were almost identical during the off-time hours; only sex was no longer significant.
Conclusions
Public awareness of the need to call EMS at AMI onset in Japan was low. Previous intervention studies that were not effective may not have targeted groups with significant risk factors.
Keywords
Introduction
Acute myocardial infarction (AMI) is associated with serious morbidity and mortality worldwide. Patients with AMI require early diagnosis and therapy because timely reperfusion therapy can result in dramatically improved clinical outcomes.1–3 Treatment-seeking delay has three phases. The patient decision time is the time from symptom onset to the decision to request medical support. The transportation time is the time from deciding to request support to first medical contact. Finally, the in-hospital time is the time from hospital admission to initiation of therapy. 4 Patient delay is an issue associated with the patient decision time. Early symptom recognition by patients and prompt calling of emergency medical services (EMS) are essential to reduce pre-hospital delay from AMI onset to reperfusion therapy; however, there has been little change in the seeking of emergency care over the past several decades.5–7 Although many factors have been associated with patient delay, the findings among previous studies are inconsistent.8–10 Most studies have focused on post-AMI survival, but some relevant public health studies involving patients without AMI have been performed.11,12 Therefore, this is not only a clinical problem but also a public health issue. To determine the risk factors for patient delay, we conducted a population-based survey to identify factors associated with the prompt, correct response to the onset of AMI symptoms; i.e., immediately calling EMS.
Participants and methods
Study design
A cross-sectional nationwide population-based survey was conducted in Japan in January 2008. The sample was selected using two-stage weighted quota sampling of the national population. Quota sampling does not involve random selection; instead, participants are selected from each segment (sex, age, and geographical region) based on a specified proportion of the population in Japan. Therefore, this method cannot be used to calculate the response rate. The sample and sampling frame were provided by a marketing research company because the research budget was limited. Eligible participants lived in Japan, were 15 to 70 years of age because we believe that persons in this age range can appropriately perform emergency calls in Japan, and could read and write in Japanese. This population was expected to constitute a large portion of Japan and have direct and/or indirect impacts on encouraging public awareness, but it may not be a specific high-risk population. Power analysis showed that a planned sample size of 1200 participants was sufficient to detect an effect 1.4 times different from a control group with a 10% incidence at 80% statistical power and a two-tailed alpha level of 0.05. Ethical approval was given by the ethical review committee of the National Cardiovascular Center (NCVC), Japan. All participants provided written informed consent.
Measurements and outcome measure
The questionnaire was used to collect data by the placement mail method (i.e., the researcher gave the survey form to the survey target person and later revisited the person to collect the survey form). The original language in the questionnaire was Japanese. The components of the questionnaire were based on previous studies. 12 The content validity of the questionnaire items was checked by expert cardiologists and nurses in the NCVC in the pilot phase of the study. The participants were asked to provide demographic information on their age, sex, marital status, education, and profession and clinical information on their history and present status of hypertension and diabetes and their history of AMI and stroke onset. They were also asked to list their symptoms at onset and risk factors for AMI. Finally, they were asked to state their self-confidence in their understanding of AMI (“I am confident that I can explain an overview of AMI to other persons by myself”) and their experiences receiving advice from a physician about AMI onset.
The primary outcome measure was the participant’s responsiveness, indicating that one would promptly call EMS at AMI onset. We divided the outcome measure into two separate periods: daytime (on-time) and combined nights and holidays (off-time) because a previous study indicated that the responses differed between these two periods. 13 The correct response was “if I feel any strong malaise in my body or any abnormal physical or psychological symptoms, including pain, that I had never before experienced, I will definitely call EMS during the daytime, nighttime, and holidays.” If the participant did not respond that they would call EMS, we asked for other response options and their reasons. If the participant responded that they would wait, we asked about the reasons for doing so and until what time they would wait to decide to act on the situation.
Statistical analysis
We investigated factors of the primary outcome variable by performing a multivariable logistic analysis. Age, sex, education, profession, current disease status, disease history of the participant and his or her family, knowledge of symptoms and risk factors, understanding of AMI, and doctors’ advice were used as potential confounders in the multivariable logistic analysis because they were significant in the univariate analysis. Missing data were eliminated from the analysis. Odds ratios (ORs) and 95% confidence intervals (CIs) were calculated. We analyzed the daytime and night/holiday groups separately. The statistical software JMP (version 10.0; SAS Institute Inc., Cary, NC, USA) was used for all data analyses.
Results
The survey was administered to 1200 participants. Their mean age was 46.3 years (standard deviation, 17.4), 16.8% (n=226) were aged >65 years, and 50.3% (n=604) were women. These results are similar to the total population distribution in Japan. The proportion of self-reported healthy participants was 74.3% (n=891). The frequency of a history of an AMI diagnosis was 0.8% (n=9), a history of a stroke diagnosis was 0.9% (n=11), AMI onset in the participant’s family was 12.9% (n=155), and reported stroke onset was 16.2% (n=196) (Table 1).
Participant demographics by EMS call or other response in on-time (daytime) or off-time (nights and holidays) hours
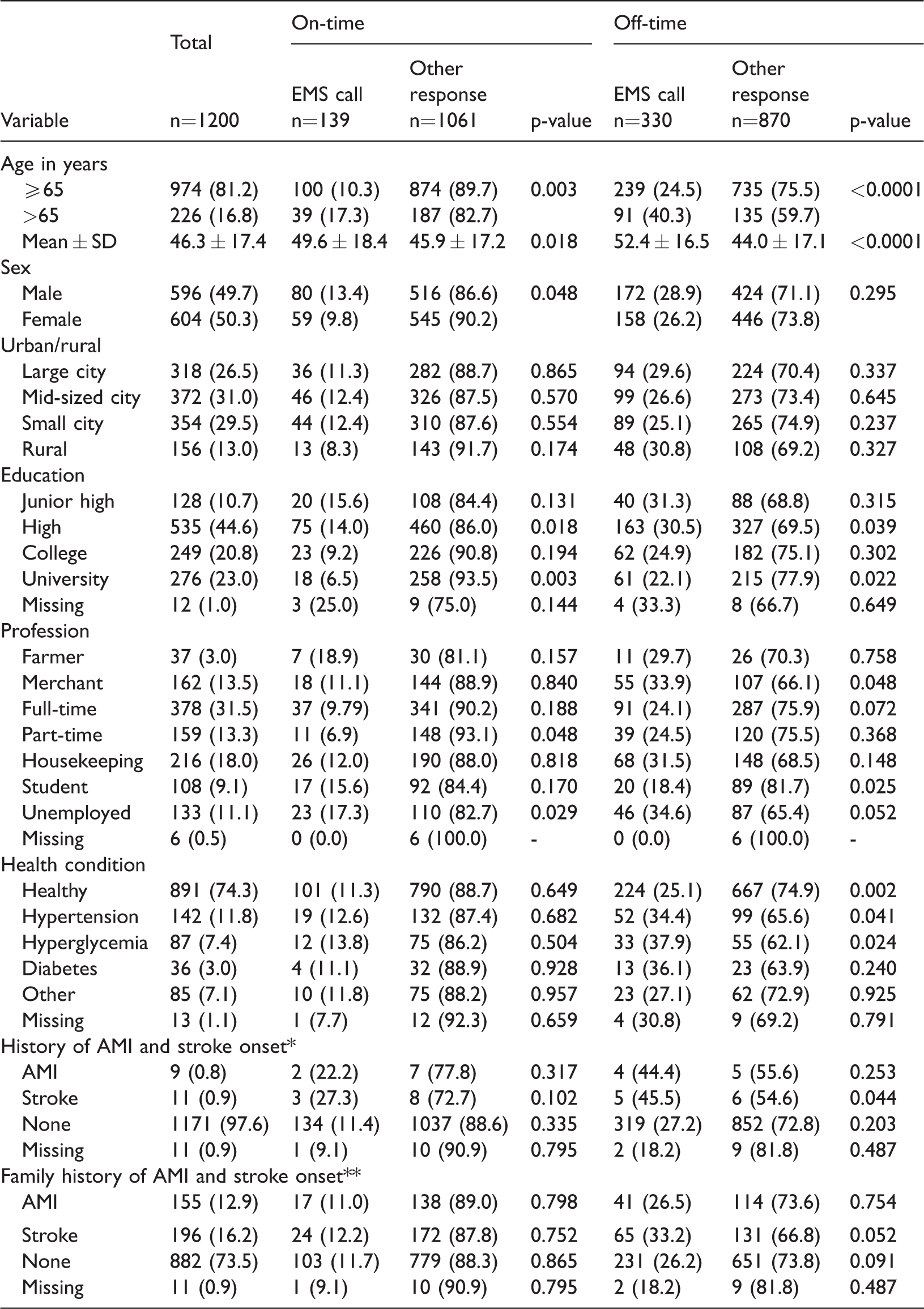
Data are presented as n (%) unless otherwise indicated. SD, standard deviation; EMS, emergency medical services; AMI, acute myocardial infarction.
One participant had AMI and stroke. **Six participants had AMI and stroke.
For the primary outcome measure, 11.6% (n=139) participants reported that they would call EMS following the onset of AMI symptoms during the day, and 27.5% (n=330) reported that they would call EMS during the nights and holidays.
Among participants who responded that they would not place an EMS call (n=780 during the day, n=622 during nights and holidays) (Table 2), the primary reason given was “I think I do not need to call for this symptom by itself ” (n=588 [74.8%] during the day, n= 422 [67.8%] during nights and holidays). Among participants who responded that they would wait to call (n=273 [22.8%] during the day, n=229 [19.1%] during nights and holidays), the primary reason given for waiting was “I hope the symptom will diminish soon” (n=200 [73.3%] during the day, n=172 [75.1%] during nights and holidays). Among the respondents who reported that they would wait, about half reported that they would wait, observe the symptoms, and decide by the next day.
Reasons for not responding “EMS call” by time

Data are presented as n (%). EMS, emergency medical services.
Multiple answers.
During the daytime, the multivariable analysis showed significant independent associations for age (by 10-year increments, p=0.0449), female sex (p=0.0219), lower education (junior high school, p=0.0303; high school, p=0.0004; college, p=0.0449; reference is university education), student status (p=0.0028), and self-confidence (p=0.0191). During nights and holidays, the multivariable analysis showed significant independent associations for age (by 10-year increments, p<0.0001), education (high school, p=0.0297), student status (p=0.0371), and self-confidence (p=0.0321) (Table 3).
Factors associated with EMS calling by time

OR, odds ratio; CI, confidence interval; EMS, emergency medical services; AMI, acute myocardial infarction.
Discussion
This study examined public awareness regarding appropriate actions following the onset of AMI symptoms in Japan using a nationwide sample survey. The two main findings were as follows: 1) There was low public awareness of the correct response to AMI symptom onset (placing an EMS call) in Japan. The participants’ age, sex, education level, and self-confidence about understanding AMI were significant factors affecting the AMI onset response. 2) There were small but significant differences in awareness of the appropriate response, as well as in the factors associated with this response, between the on-time and off-time.
Our findings are similar to those of some previous reports. Public awareness of symptoms, AMI risk factors, and the need to call EMS at the onset of AMI symptoms was relatively low, as some authors have reported.12,14–20 Receiving advice from a physician did not affect the calling of EMS, which is similar to a finding in a study of Polish adults. 11 Age, sex, education level, and student status were still associated with EMS call awareness in the multivariable analysis. A previous study showed similar results in a non-professional group. 14
Some of our findings are different from those of previous reports. Although older women were found to be a high-risk group in a systematic review based on a post-AMI patient registry, 9 paradoxically, older women in the general public were not found to be a low-awareness group in our study. Additionally, in the general public, there was only a small difference in AMI-onset decisions between the on-time and off-time.
The participants’ self-confidence regarding their understanding of AMI was a significant factor. Otherwise, we found no association between symptoms of AMI and risk factors for an EMS call response. Therefore, richer, more direct interventions that specifically target high-risk groups, rather than mass-media campaigns might be needed. This recommendation is consistent with findings from some intervention trials.20–22 We might need to continuously support personalized information, education, and suggestions to affect the patient’s prompt decision to call EMS through channels such as social media and smart media.
Our study had some limitations. The study design was cross-sectional, and our findings are therefore associations that cannot imply causal relationships. We adjusted for some potential confounders in the multivariable analysis, but there are still effects from unmeasured confounders. These findings are from Japan; findings from other countries may differ. EMS is also dependent on the specific healthcare systems in different countries and regions. However, we expect that our findings will be applicable to other developed countries because the challenges of pre-hospital delay are similar internationally.
Conclusion
Public awareness of the prompt, correct response at the onset of AMI was low in Japan. Poor responses were shown among lay persons who were older, were men, had a low education level, and had low self-confidence regarding their understanding of AMI. There were some differences in the factors associated with the awareness that one should promptly call EMS between daytime and nights/holidays.
Footnotes
Acknowledgements
The authors thank Ms. Kumiko Hayashi and Ms. Hiromi Muramatsu for providing secretarial assistance. The authors also thank all of the investigators in the study group “J-PULSE III” for participating in a helpful discussion and providing comments.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article: The work was supported by research grants for Cardiovascular Disease (H19-Shinkin-03, “The study for the establishment of the prehospital system in acute myocardial infarction and stroke” and H22-Sinkin-02, “The study for the establishment of the emergency medical system with prehospital care for acute myocardial infarction and telemedicine”) from the Ministry of Health, Labour and Welfare, Japan, and a Grant-in-Aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology, Japan. The funder had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
