Abstract
Objectives
Human JC polyomavirus (JCPyV) infection has an increased risk of developing progressive multifocal leukoencephalopathy (PML). Different JCPyV subtypes differ in the virulence with which they cause PML. Currently, the JCPyV infection status and subtype distribution in patients with human immunodeficiency virus-1 (HIV-1) in China are still unclear. This study aimed to investigate the epidemiology and subtype distribution of JCPyV in HIV-1-infected patients in China.
Methods
Urine samples from 137 HIV-1-infected patients in Zhejiang Province in China were tested for the presence of JCPyV DNA. The detected VP1 sequences were aligned and analysed using BioEdit and MEGA software.
Results
Among urine samples from HIV-1-infected patients, 67.2% were positive for JCPyV DNA (92/137). Primarily, the type 7 strains of JCPyV were detected, among which 45.5% (15/33) were subtype 7A, 30.3% (10/33) were 7B, and 24.2% (8/33) were 7C. Six nucleotide mutations, as well as one amino acid substitution, were isolated from the patients.
Conclusions
Urine samples from HIV-1-infected patients from Zhejiang Province show a high JCPyV infection rate. The most common JCPyV strains are subtypes 7A, 7B, and 7C.
Keywords
Introduction
The JC polyomavirus (JCPyV) is a member of the Polyomaviridae family and was originally discovered by Padgett in 1971 from a patient with progressive multifocal encephalopathy (PML). 1 PML is a rare and fatal demyelinating disease of the central nervous system, caused by replication of JCPyV in oligodendrocytes and astrocytes. This virus can lead to cell lysis and multifocal white matter lesions.2–5 PML is frequently reported in patients with severe immunosuppressive conditions, including malignant haematological disorders and acquired immunodeficiency syndrome (AIDS). PML is also found in patients undergoing long-term immunosuppressive therapy with biological agents because of organ transplantation or autoimmune diseases.2,4,6–9
JCPyV is a cyclic double-stranded DNA consisting of an early region, a noncoding regulatory region, and a late region. The late region encodes the capsid proteins VP1, VP2, VP3, and agnoprotein.10–12 Based on the nucleotide difference in the JCPyV VP1 region, eight JCPyV subtypes have been defined, and each subtype is associated with a specific geographical region. Subtypes 1, 2, and 4 are mostly distributed in Europe. Subtypes 3 and 6 are found in Africa, subtype 8 is found in Papua New Guinea and the Pacific Islands, and subtypes 2, 4, and 7 are found in Asia. In the general healthy Chinese population, the most common JCPyV subtypes are 7A, 7B, 7C, and 2D 4 10,12–16.
JCPyV has drawn widespread attention because it mediates lytic effects on neurons and can lead to PML. JCPyV type 2 is found with PML in Europe and Asia. JCPyV type 1 with PML occurs in French patients, and 3, 4, and 7 strains are found in African patients diagnosed with PML. Among all of the JCPyV subtypes, type 2 is considered most closely related to PML. Types 3, 7, and 4 show weaker lytic effects on neurons.14,15,17
No reports have been published on JCPyV epidemiology in Chinese human immunodeficiency virus-1 (HIV-1)-infected patients. Therefore, this study aimed to investigate JCPyV infection and subtype distribution in Chinese HIV-1-infected patients and provide virological evidence that is useful for clinical diagnosis and therapy of PML.
Study design and methods
Study population
A total of 137 HIV-1-infected patients from the Department of Infectious Disease of the First Affiliated Hospital of Zhejiang University, without any selection, were included in this study. The cohort included 115 patients who were receiving highly active antiretroviral therapy (HAART) and 22 patients who were not being treated with antiretroviral therapy at the time of enrolment in the study. We explained the purpose of this experiment and obtained verbal informed consent from these participants. We obtained approval from the Ethics Committee of the First Affiliated Hospital, College of Medical, Zhejiang University (approval number: 2014320).
DNA extraction
At the beginning of the study, we asked patients to preserve midstream urine in a urine container. A total of 10 mL of urine was divided into four centrifuge tubes, each of which was centrifuged at 12000 rpm (9982 × g) for 10 min. The liquid supernatant was discarded. The remaining urinary sediment was mixed in 100 µL of sterile phosphate-buffered saline. Viral DNA was extracted using a QIAamp DNA Mini Kit (Sangon Biotech, Shanghai, China) in accordance with the manufacturer’s instructions.
PCR and sequence analysis
JCPyV DNA primers were designed specifically to the JCPyV VP1 fragment. The forward and reverse primer sequences were JLP15 (PR 5′-ACAGTGTGGCCAGAA TTCCACTACC-3′) and JLP16 (PF 5′-TAAAGCCTCCCCCCCAACAGAAA-3′), respectively.12,18–21 The target sequence was amplified in a reaction and performed in a volume of 25 µL containing the following: 1 µL of template, 2.5 µL 10 × PCR buffer, 10 µM of each primer, 0.5 µL deoxyribonucleoside triphosphates , 2.5 µL MgCl2, and 2.5 U/reaction Taq polymerase.
The amplification profile was as follows. Double-stranded DNA was initially denatured for 5 min at 95°C, followed by 35 cycles of 95°C (30 s), 55°C (35 s), and 72°C (1 min), and then 72°C for 8 min for a final extension step. DNA sequencing was performed using an automated sequencer (ABI 3730 DNA sequencer. The length of the obtained fragment was 215 bp. 22
Phylogenetic analysis
35 JCPyV whole-genome sequences were obtained from GenBank. The accession numbers of the referenced sequences were as follows: 701A AF295737, 715A* AF300965, 710A* AF300960, 713A* AF300963, 702A AF295738, 803A AF281625, 811A AF396430, 233E AF281605, 251E AF396423, CB-2 AB048550, 707C* AF300957, 709C* AF300959, CY AB038249, 725B* AF300950, 726B* AF300951, 247D* AF363833, 246D* AF363832, 230 AF015536, 228 AF015534, GS/B AF004350, 227 AF015533, 801B AF281623, 808B AF396432, GH-1 AB038252, 601 AF015537, 310A AF295732, ET-3 AB048547, 313B AF295735, 311 U73501, GR-3 AB048563, 402 AF015528, G2 AB038251, MAd-1 J02226, N2 AB048574, UK-2 AB048576 3,18,23–25.
A total of 68 sequences (33 detected the VP1 coding region of JCPyV DNA) were aligned and analysed using BioEdit version 7.0.9 (www.bioedit.updatestar.com) and MEGA version 7.0.20 (www.megasoftware.net). A phylogenetic tree was constructed by the neighbour joining with Kimura 2-parameter method model for identification of JCV genotypes. 20 1000 bootstrap replicates were performed to determine the confidence level of the branching patterns in the tree.
Statistical analysis
The t-test or Wilcoxon’s rank test was performed for numerical data, while the chi-square test and Fisher’s exact test were used for categorical variables. Values of P < 0.05 were considered significant. All data were analysed using IBM SPSS Statistics for Windows, Version 23.0 (IBM Corp., Armonk, NY, USA).
Results
High JCPyV excretion rate in HIV-1-infected patients
The JCPyV-DNA excretion rate was 67.2% (92/137) in the urine samples from HIV-1-infected patients in Zhejiang Province (Table 1). Among the 137 HIV-1-infected patients included in the study, the youngest was 20 years old at the time of recruitment, the oldest was 83 years old, and the mean age was 39.44 years. The patients were divided into four age groups. The 21–40 years age group was the largest, comprising 64.2% (88/137) of all patients, followed by the 41–60 years age group, accounting for 25.5% (35/137) of the patients (Table 1).
Comparison of the JCPyV excretion rate among HIV-1-infected patients
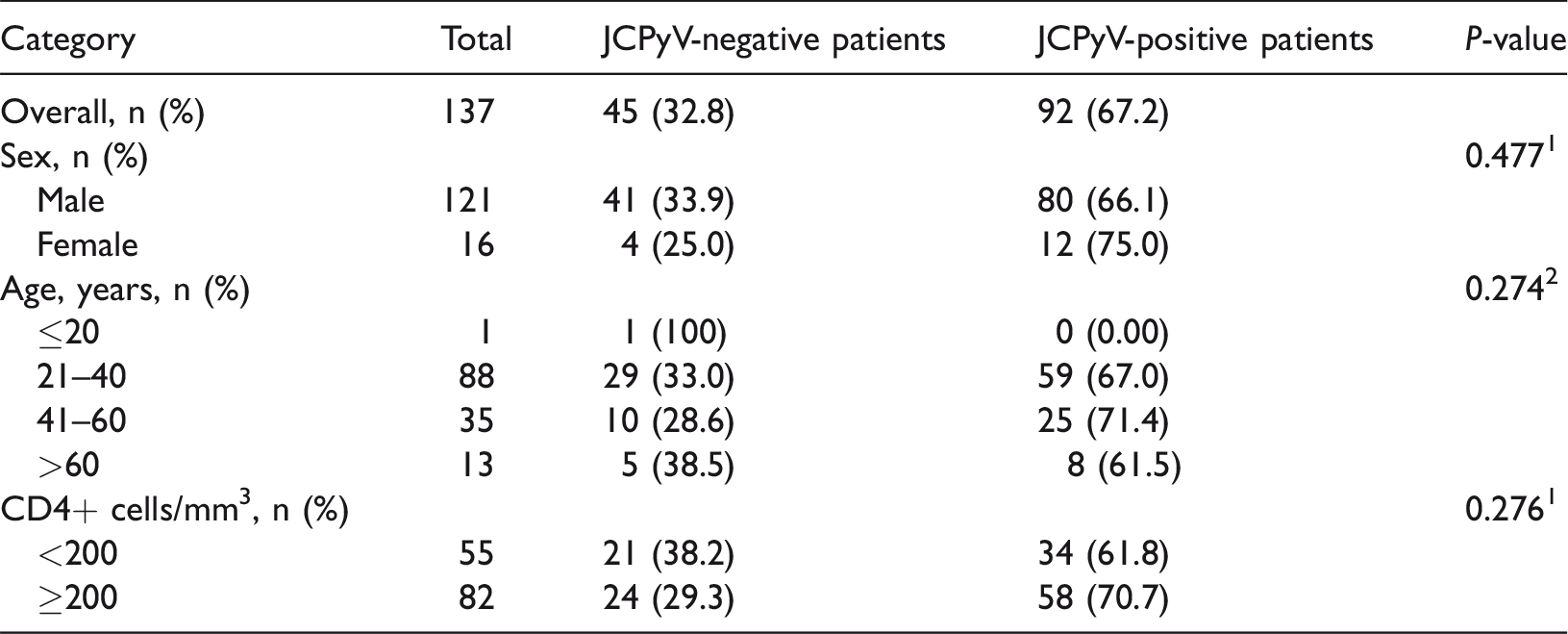
Pearson chi-square test, continuity correction, and Fisher’s exact test were used for categorical variables.
The independent samples t-test was used for numerical data.
JCPyV, JC polyomavirus; HIV-1, human immunodeficiency virus-1.
The patients were divided into two groups based on their CD4+ T lymphocyte counts (ranging from 1–1133 cells/mm³): CD4 < 200 and ≥200 cells/mm³. The mean CD4 count of all patients was 289.12 cells/mm³. The JCPyV DNA positive rates were 70.7% and 61.8% in patients with CD4 ≥200 and CD4 < 200 cells/mm³, respectively, with no significant difference between the groups. There were no significant differences in sex, age, and CD4 counts between JCPyV-positive patients and negative patients.
Subtypes 7A, 7B, and 7C are the most common JCPyV strains in HIV-1-infected patients
According to the order of entry of participants into the cohort, the first 45 of 92 positive urine specimens were selected for sequencing. Only 33 JCPyV amplicons were successfully sequenced. We generated a JCPyV phylogenetic tree of HIV-1-infected patients by comparing 33 JCPyV DNA VP1 sequences with 35 standard whole-genome sequences from GenBank (Figure 1). Type 7 was the most common strain. This group was further divided into three subtypes of 7A, 7B, and 7C, with bootstrap values from 51% to 67%. Among all three subtypes, 7A was the most common, accounting for 45.5% (15/33) of all participants. Type 7B accounted for 30.3% (10/33) and 7C for 24.2% (8/33) of all participants. Figure 1 shows a neighbour-joining phylogenetic tree with the Kimura 2-parameter method consisting of 33 specimens and 35 complete JCPyV DNA sequences from GenBank. A total of 1000 bootstrap replicates were performed (only bootstrap values above 50% are shown).

Isolation subtypes of JCPyV analysed by a phylogenetic tree. The black solid diamonds show the 33 specimens from the current study.
New JCPyV mutants
By analysing the nucleotide sequences of the isolated DNA, we found the following (Table 2). (1) Six nucleotide variant sequences (ZJV-32, ZJV-13, ZJV-31, ZJV-16, ZJV-17, ZJV-21) had nucleotide mutations at positions 1747, 1796, 1804, 1809, 1811, 1813, 1843, 1858, and 1885 by comparing them with selected sequences (using the complete JCPyV genome sequence CY AB038249 as the standard). (2) Among the 15 isolated JCPyV 7A sequences, 14 samples showed sequences identical to 710A* VP1 and a new variant at position 1858 (A→T). (3) Among the 10 isolated JCPyV 7B sequences, seven samples had identical sequences to CY AB038249 VP1, one had a point mutation at position 1885 (T→C), one had a point mutation at position 1811 (T→C), and one had a sequence mutation at 1813 (G→A). (4) Among the eight isolated JCPyV 7C sequences, five samples had sequences identical to 707C* VP1 and one was identical to that of CB-2 VP1. In another two samples, one sequence showed a point mutation at position 1809 (C→G). The other sequence showed double nucleotide substitutions (C→T) and (T→C) at positions 1796 and 1885, respectively. (5) Among these six JCPyV nucleotide mutants, we found that only the sequence ZHE-31 represented an amino acid substitution. The threonine was replaced by serine (T→S) corresponding to a nucleotide substitution (ACT→AGT) at positions 1808 to 1810.
Nucleotide polymorphisms of JCPyV genotypes in the VP1 gene fragments

Prototype sequence for subtype 7A (accession number: 702A AF295738).
Prototype sequence for subtype 7C (accession number: CB-2 AB048550).
Prototype sequence for subtype 7C (accession number: 707C* AF300957).
Prototype sequence for subtype 7B (accession number: CY AB038249).
A new variant (ZHE-32) of subtype 7A was found with nucleotide polymorphisms.
New variants (ZHE-31 and ZHE-13) of subtype 7C were found with nucleotide polymorphisms.
New variants (ZHE-17, ZHE-21, and ZHE-16) of subtype 7B were found with nucleotide polymorphisms.
JCPyV, JC polyomavirus.
Discussion
PML, which is a disease of the central nervous system, is rare and fatal in patients with HIV. The incidence of PML in these patients is slightly lower than that of toxoplasma encephalitis and HIV-1 encephalopathy. Currently, there is no effective treatment available for PML.2,26,27
The JCPyV DNA excretion rate was 67.2% in HIV-1-infected patients in Zhejiang Province, China. JCPyV can be detected in urine samples from healthy populations at a rate of 10% to 30%.10,12,28–31 In immunosuppressed patients, the JCPyV detection rate ranges mostly from 25% to 50%. Among HIV-1-infected patients, the excretion rate was 44.1% in Serbia, 32% in Brazil, and 47.6% in Italy.16,19,28,32 The high frequency of polyomavirus excretion indicates that activation of viral reaction results from the interaction between polyomavirus and HIV. Differences in selection of primers and demographics of patients may account for the divergent results on the prevalence of JCPyV.
In our study, according to the order of participants’ entry into the cohort, 33 VP1 regions of 92 positive urine specimens were sequenced and the distribution of JCPyV genotypes was examined in HIV-1-infected patients in Zhejiang Province. VP1 gene sequencing analysis showed that, in accordance with the results acquired from the general Chinese population, the most common JCPyV stain in HIV-1-infected patients in China was type 7. 13 The six newly discovered JCPyV nucleotide mutants have not been previously published. Most of these mutants presented with point substitutions, and among these six nucleotide mutants, only the sequence of ZHE-31 expressed an amino acid substitution. However, none of these new subtypes were discovered by analysing the phylogenetic tree.
Before HAART, the incidence of PML in HIV-1-infected patients ranged from 5% to 8%, accounting for 80% of the total numbers of PML, and the 1-year survival rate was below 10%.2,26,33–35 HAART, which can slow development and progression of PML in individual patients with HIV/AIDS, has become widespread, but the incidence of PML remains at approximately 3% to 5%.2,33,36 JCPyV is asymptomatic and in a latent state in the kidney, and it can spread to the central nervous system through blood flow or lymphatic transmission, causing PML.7,24,33,37,38 In non-coding control region DNA of JCPyV, the archetype is mostly detected in urine of non-PML individuals, while the DNA rearrangement is more common isolated from blood, peripheral blood mononuclear cells, and cerebrospinal fluid in patients with PML. During the process of JCPyV transmission, gene mutations, including point mutations, deletion, and duplication, may occur in the viral genome.2,5,7,33 In this study, JCPyV-positive HIV-1-infected patients were followed up, and none of them were diagnosed with PML. The JCPyV strains detected in this study, including the variants, were still mostly latent. The virulence of these mutants needs to be further studied through clinical observation and diagnosis.
This study is the first to report JCPyV detection in urine samples from HIV-1-infected patients in China. A total of 67.2% of HIV-1-infected patients were infected with JCPyV. Therefore, JCPyV infection should be monitored early and longitudinally. In the future, we will continue our research on JCPyV using urine, blood, and cerebrospinal fluid samples from patients with PML to better understand the pathogenic characteristics of JCPyV at the genetic level.
Footnotes
Ethical Approval
All procedures performed in study involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Verbal informed consent was obtained from all individual participants included in the study.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Author contributions
CH extracted DNA and drafted the article. YH acquired and interpreted the data. JS critically revised the article for important intellectual content. MW and QZ made partial contributions to data acquisition and DNA extraction. BZ conceived the idea of this study. All authors approved the version to be published.
Funding
This work was supported by the National Special Research Program for Important Infectious Diseases (No. 2014ZX10001002-002-002 and No. 2017ZX10202102-002-002).
