Abstract
Objective
This study was performed to identify risk factors for postoperative rectovaginal fistula (PRF) in patients with deep infiltrating endometriosis (DIE).
Methods
Data were retrospectively obtained from the medical records of 104 patients with DIE, and statistical analysis was used to detect risk factors for PRF.
Results
Five of 104 (4.8%) patients developed PRF from 5 to 16 days postoperatively. The operative procedures included 84 (80.8%) superficial excisions, 6 (5.8%) full-thickness disc excisions, and 14 (13.5%) bowel resections. Most lesions were located in the cul-de-sac, and the mean lesion size was 2.6 cm (range, 0.5–7.0 cm). The univariate analysis showed that lesion location, larger lesion size, and surgical technique were statistically significant risk factors for PRF.
Conclusion
Surgical procedures should be very carefully executed in patients with DIE lesions of ≥4 cm.
Keywords
Introduction
Endometriosis is a common benign gynecological condition that is defined as the presence of endometrial tissue outside the uterus and affects about 10% to 15% of women of childbearing age. 1 About 5.3% to 12.0% of patients with endometriosis 2 develop deeply infiltrating endometriosis (DIE), which is characterized by a solid mass that is situated deeper than 5 mm under the peritoneum and mainly involves the rectum, bladder, ureter, and uterosacral ligament.
Although some patients with endometriosis are asymptomatic, such as patients with ureteral endometriosis, 3 most patients develop severe dysmenorrhea, dyspareunia, rectorrhagia, diarrhea, and defecation pain. 4 All of these symptoms substantially impair patients' psychological and social function, and decrease their quality of life. Besides the unbearable pain associated with endometriosis, infertility is also a common reason for affected women to consult clinics.6,7 Up to 50% of infertile women reportedly have endometriosis. Studies have revealed that women with endometriosis are at high risk for anxiety and depressive symptoms.8,9
Because the pathogenesis of DIE is still unclear10,11 and the European Society of Human Reproduction and Embryology guidelines clearly state that no specific medication with which to resolve the disease-related symptoms is available, 12 complete lesion excision is usually performed and has been shown to notably improve patients’ quality of life.13,14 Thus, surgery is considered the first-line and gold standard treatment for DIE.15,16 The surgical procedure can be very complex because of the high risk of bowel and urinary tract involvement in this disease. 17 The most worrisome complication associated with the surgical treatment of DIE is the development of a postoperative rectovaginal fistula (PRF), which is defined as an abnormal connection between the rectum and vagina. 18 The reported occurrence rate of PRF after surgical treatment of DIE ranges from 2.9% to 10.6%.16,19 Patients with PRF may require longer hospitalization, experience slower recovery to work, and have a higher risk of the need for multiple surgical repairs.
Studies of the risk factors for PRF have not generated a consensus opinion to date, although it has been reported that a higher number of radical surgeries performed increases the risk of PRF. 2 However, which factors may truly contribute to PRF remains unclear.
Therefore, the aim of the current study was to explore the clinical characteristics of this postoperative complication and analyze the risk factors for PRF in patients with DIE in our single university-based tertiary hospital.
Materials and methods
This retrospective cohort study involved 104 patients diagnosed with DIE from January 2013 to October 2014 at the Obstetrics and Gynecology Hospital of Fudan University, Shanghai, China. This study was approved by the institutional ethics board of our hospital. All patients who participated in the study provided verbal informed consent.
The patients’ medical records were reviewed to obtain data on their presurgical treatments and surgical information, demographics, body mass index (BMI), preoperative and postoperative visual analogue scale (VAS) score, and recovery information.
Preoperative assessment
Records of the patients’ rectovaginal examination, transvaginal ultrasonography, and pelvic magnetic resonance imaging findings were collected to assess the extension of the DIE lesions. Colonoscopy was performed in selected patients with severe bowel symptoms such as cyclic constipation, dyschezia, or hematochezia.
Decisions regarding operations were made cautiously and involved the whole medical team, including gynecologic, gastrointestinal, and urological surgeons. Because no standard criteria have been established, the choice of the surgical technique depended on the surgeons’ experience and patients’ preference. Generally, both patients and doctors preferred the least aggressive surgery that might remove most of the lesion.
Surgical procedure
The operative route was either laparoscopy or laparotomy according to the consensus of the whole medical team. The different surgical techniques used were as followings:
20
Simple lesion cut (SLC): superficial shaving, excision, or shaving of serosal and subserosal bowel endometriosis without opening of the bowel wall. Full-thickness disc excision (FDE): excision of bowel endometriosis with a small opening followed by closure of the bowel wall. Bowel resection and anastomosis (BRA): resection of a bowel segment affected by endometriosis followed by stapling together of the two remaining ends. Ileostomy: resection of a bowel segment followed by attachment of the small intestine to the abdominal wall to bypass the large intestine.
Diagnosis of DIE
The diagnosis of DIE was confirmed both clinically and pathologically based on the following criteria: 1) typical symptoms (cyclic pelvic pain, infertility, etc.) and a suspicious nodule with tenderness found on physical examination, 2) a blue or brown lesion infiltrating >5 mm beneath the peritoneum as observed by at least two experienced surgeons during the surgery, and 3) confirmation of the diagnosis of endometriosis by two independent gynecological pathologists (N.Y. and Z.X.).
Statistical analysis
Statistical analysis was performed with SPSS software, version 19.0 (IBM Corp., Armonk, NY, USA), and
Results
Clinical characteristics
The demographic characteristics, symptoms, and presurgical treatment of the 104 patients are summarized in Table 1. The mean age was 35.1 ± 6.2 years (range, 20–52 years), and the mean BMI was 21.0 ± 2.2 kg/m2 (range, 16.1–28.0 kg/m2). Most patients complained of dysmenorrhea (71/104, 68.27%), followed by tenesmus (24/104, 23.08%), dyspareunia (17/104, 16.35%), and other symptoms. The mean VAS score before surgery was 5.83 (range, 0–10). Most of the patients experienced long-term symptoms; the mean duration of symptoms was 36.4 months (range, 1–180 months). Eleven (10.58%) patients had undergone a previous surgery for endometriosis, and 56/104 (53.8%) had received conservative treatment before surgery, including a gonadotropin-releasing hormone agonist (GnRH-a) (17/104, 16.35%), traditional Chinese medicine (19/104, 18.27%), and other treatments.
Clinical characteristics of patients with deep infiltrating endometriosis (n = 104)

Data are presented as mean ± standard deviation or n (%) patients. BMI: body mass index; VAS: visual analogue scale; GnRH-a: gonadotropin-releasing hormone agonist; USL: uterosacral ligament; GIS: gastrointestinal surgeon; US: urological surgeon.
Surgical findings
In total, 99 (95.2%) patients underwent laparoscopic surgery, 4 underwent laparotomy because severe pelvic adhesion was predicted, and 3 underwent vaginal surgery (among the latter, 2 underwent vaginally assisted laparoscopic surgery). Three of 99 the laparoscopic procedures were converted to laparotomy because of unexpectedly severe pelvic adhesion. The mean operation time was 148.4 minutes (range, 24–440 min) with a mean blood loss of 195.9 ml (range, 20–1400 ml). The operative techniques included 84 SLCs, 6 FDEs, 10 BRAs, and 4 ileostomies. An ovarian endometrioid cyst was the most common accompanying disease, with an occurrence rate of 46.1% (48/104).
DIE lesions
The mean DIE lesion size was 2.6 cm (range, 0.5–7.0 cm) as measured intraoperatively. The cul-de-sac was involved in all patients; other common sites of involvement were the rectum/intestine (23/104, 22.1%) and ureter (14/104, 13.5%). Thirty-two patients (30.8%) had multiple DIE lesions (Table 1). To investigate the lesion locations in more detail, we divided the cul-de-sac into a central area and a lateral area coronally; the involving rate in each area was 77% and 42%, respectively.
Univariate analysis of risk factors for PRF
After a mean follow-up of 23.2 months, PRF occurred in 5 (4.8%) of 104 patients (Table 2) at 5 to 16 days postoperatively. The clinical characteristics of these patients are summarized in Table 2. Thus, the patient cohort was divided into those with a PRF (Group A) and those without a PRF (Group B). The results of the univariate analysis are shown in Table 3. No differences in age, BMI, surgical type, or whether the vaginal cuff was simultaneously cut open were found between the two groups. Significantly more patients in Group B than A underwent SLC [83/99 (83.8%) and 1/5 (20.0%), respectively;
Clinical characteristics of patients with DIE with postoperative rectovaginal fistula
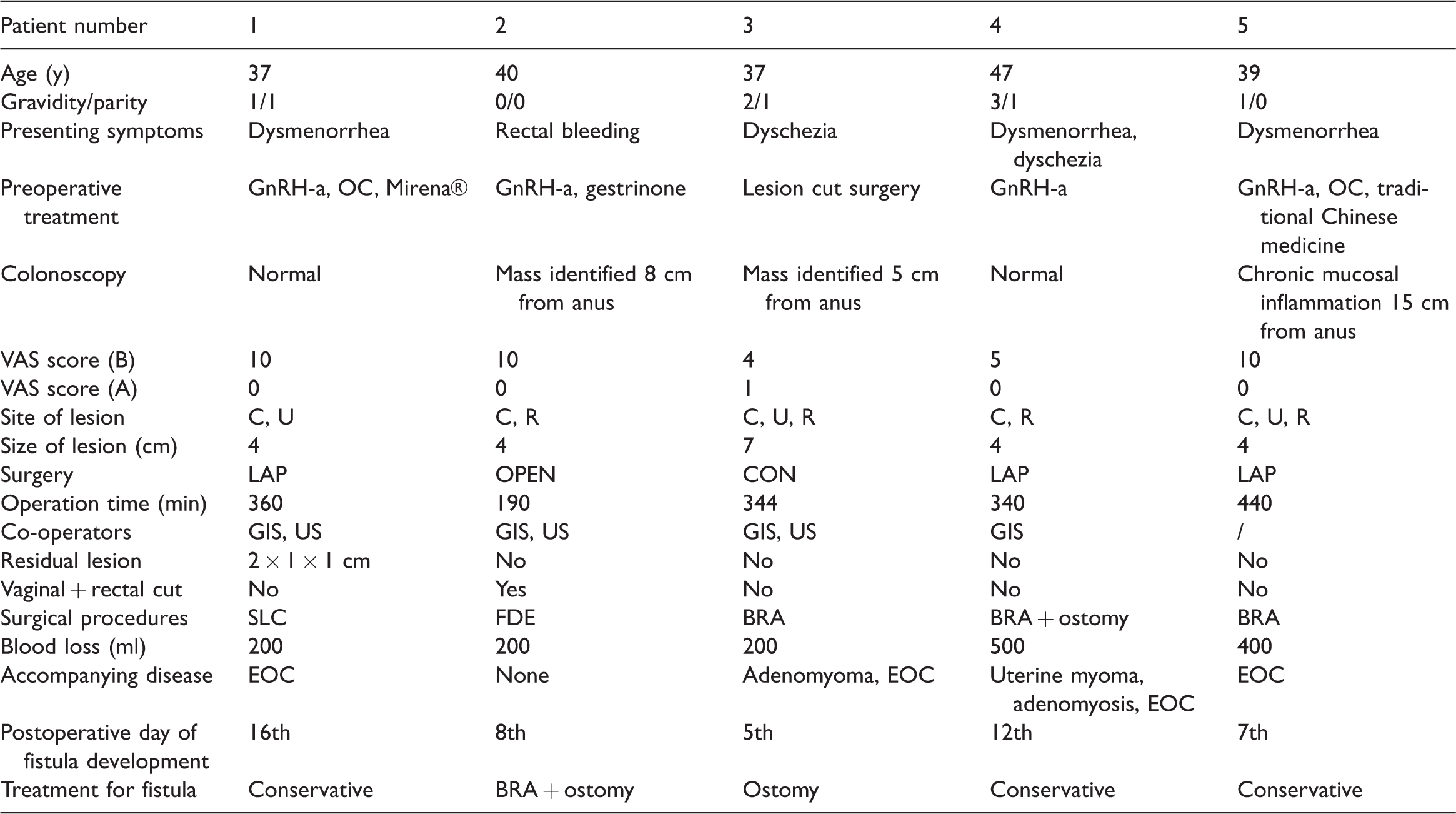
DIE: deep infiltrating endometriosis; GnRH-a: gonadotropin-releasing hormone agonist; BMI: body mass index; VAS score (B): visual analogue scale score before surgery; VAS score (A): visual analogue scale score after surgery; EOC: endometrioid ovarian cyst; OC: oral contraceptives; C: cul-de-sac; U: ureteral; R: rectum; LAP: laparoscopic; OPEN: open surgery; CON: conversion to open surgery; SLC: simple lesion cut; FDE: full-thickness disc excision; BRA: bowel resection and anastomosis; GIS: gastrointestinal surgeon; US: urological surgeon
Univariate analysis of clinical factors of patients with and without postoperative rectovaginal fistula after surgical treatment of DIE
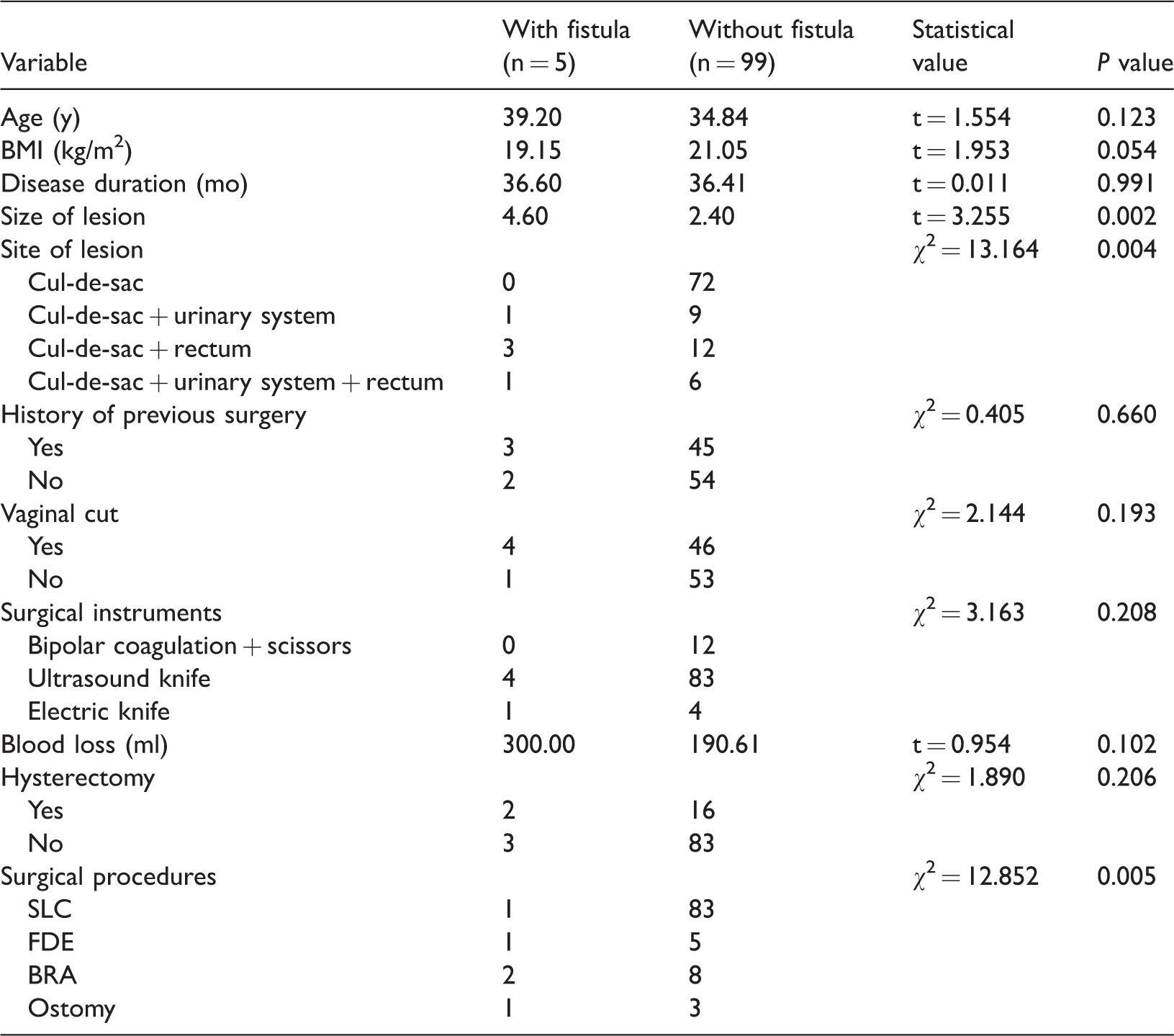
DIE: deep infiltrating endometriosis; SLC: simple lesion cut; FDE: full-thickness disc excision; BRA: bowel resection and anastomosis.
Clinical characteristics of each patient with PRF
Case 1: A 37-year-old woman (gravidity 1 parity 1) with a 75-month history of dysmenorrhea underwent conservative treatment including GnRH-a, oral contraception, and Mirena® (Bayer Oy, Guangzhou Branch, China) before surgery. However, her VAS score before surgery still reached 10. Laparoscopic surgery was performed, and a 4-cm lesion was found at the cul-de-sac, which also infiltrated the ureter. laparoscopic superficial excision was performed, and a 2- × 1- × 1-cm lesion was left according to the patient’s desire to preserve the integrity of the intestine. However, 16 days postoperatively, she felt feces exiting the vagina, and a rectovaginal fistula was confirmed by computed tomography. The patient underwent conservative treatment for the fistula.
Case 2: A 40-year-old woman (gravidity 0, parity 0) with a 50-month history of rectal bleeding underwent treatment with GnRH-a and gestrinone before surgery. Her preoperative VAS score was 10. Colonoscopy showed a narrowed ring that extended 8 cm up to the anus, and she therefore underwent open surgery. A 4-cm lesion was identified at the cul-de-sac and was infiltrating the intestine; thus, FDE was performed. However, 8 days postoperatively, feces appeared in the drainage bag. The patient underwent a second surgery involving BRA + ostomy.
Case 3: A 37-year-old woman (gravidity 2, parity 1) with a 10-month history of difficult defecation had undergone an endometriosis-related surgery 2 years previously. Colonoscopy was performed before surgery this time. A 5- × 6-cm mass with an anabrotic surface was identified 5 cm from the anus. The pathologic examination confirmed chronic inflammation. Because of technical difficulties, laparoscopic surgery was converted to open surgery. The lesion was 7 cm in size, located at the cul-de-sac as well as the bilateral ureterosacral ligaments, and infiltrated all layers of the sigmoid colon. Thus, BRA was performed, and a scleroid drainage tube was placed in the pelvic cavity. Five days postoperatively, the patient felt feces partially exiting the vagina and developed a fever. A temporary colostomy was established for 3 months, and the patient completely recovered.
Case 4: A 47-year-old woman (gravidity 3, parity 1) had a >10-year history of dysmenorrhea and had experienced dyschezia for most recent 6 months. Five years previously, she had received a GnRH-a injection 6 months preoperatively, and the dysmenorrhea resolved. The patient had experienced dyschezia during the most recent 6 months, but no positive findings were revealed by preoperative colonoscopy this time. A 3-cm lesion was detected at the preoperative physical examination. BRA + ostomy was performed laparoscopically. During the surgery, a 4-cm lesion was found at the cul-de-sac and was infiltrating all layers of the sigmoid colon. The patient then developed a fever and discharge of pale yellow fluid with a fecal odor from the vagina. Conservative and symptomatic treatments were performed until discharge from the hospital.
Case 5: A 39-year-old woman (gravidity 1, parity 0) with a 6-year history of severe dysmenorrhea underwent treatment with oral contraceptives, 6 months of cyclic GnRH-a injections, and traditional Chinese medicine. However, her symptoms were not relieved. Colonoscopy showed chronic mucosal inflammation 15 cm from the anus. Physical examination revealed a 4-cm lesion at the cul-de-sac, which was consistent with the surgical findings. Seven days after BRA, the patient felt feces exiting from the vagina and developed a fever of 38.9°C. After 2 weeks of conservative treatment, she was discharged with a healed PRF.
Discussion
Although medical treatments such as hormonal contraceptives, progestogens and anti-progestogens, and GnRH-a, and GnRH antagonists have been widely used for endometriosis, there is no overwhelming evidence to support the effects of any of these medications.12,21 In the present study, several medical therapies were performed in 56 of 104 (53.8%) patients preoperatively, including GnRH-a injection, oral contraception, gestrinone, danazol, and Mirena®, but it seemed unlikely that the patients benefited from these medical therapies. To obtain long-term outcomes of pain relief and fertility, surgery is still regarded as the first-choice treatment for DIE, 22 especially for endometriosis that has deeply infiltrated the bowel.23,24
However, postoperative complications are a great challenge for surgeons and can be divided into two categories: major and minor complications. The former include rectovaginal fistulas, bowel leakage, severe infection, and large blood loss volumes, while the latter include temporary intestinal and urinary dysfunction and superficial infection. 25 Most patients with PRF experience malodorous vaginal discharge, fever, and lower abdominal pain, which slow their postoperative recovery while increasing their costs and hospitalization duration. 26 The reported incidence of PRF among patients who have undergone DIE-related surgeries ranges from 2.9% to 10.6%.2,27–29 In the present study, 5 (4.8%) of 104 patients who underwent surgical treatment of DIE in our single tertiary hospital developed PRF from 5 to 16 days postoperatively.
Belghiti et al.
29
found that DIE lesions more commonly involved the vagina in patients with than without PRF [8/9 (89%) vs. 55/189 (29%), respectively;
Tarjanne et al.
30
found that among patients with DIE who underwent colorectal resection, more major complications occurred in patients with nodules of >4 than ≤4 cm [12/68 (10%) vs. 6/87 (7%), respectively;
Inappropriate use of energy instruments may reportedly increase the risk of PRF. Darai et al. 31 reported that two of six PRFs developed as a result of electrocoagulation. In the current study, although the rate of using energy instruments was higher in patients with than without PRF, there was no significant difference between the two groups [5/5 (100.0%) vs. 87/99 (87.8%), respectively].
No consensus regarding the choice of surgical procedures in treating DIE has yet been reached.
32
All surgeries can be divided into two categories: conservative (including SLC and FDE) and radical (BRA and/or ostomy).33,34 Whether conservative surgeries would be more suitable for bowel endometriosis is controversial.
35
Although previous studies have shown that radical surgeries could more substantially improve patients’ quality of life,26,36 they are associated with a greater risk of postoperative complications. Mohr et al.
37
reported that the complication rate of shaving, disc excision, and segmental resection was 6%, 23%, and 38%, respectively. Kondo et al.
38
and Maytham et al.
39
showed similar results. However, Roman et al.
40
reported more postoperative complications in the conservative than radical surgery group [25/51 (49.0%) vs. 10/24 (41.6%), respectively]. Koh et al.
22
reported similar findings for patients undergoing disc resection; they found that segmental resection may not increase the risk of complications [8/71 (11.3%) vs. 5/29 (17.2%), respectively]. In our cohort, the univariate analysis revealed that conservative surgery was associated with a lower risk of PRF (
Belghiti et al.
28
reported that colpectomy might increase the incidence of PRF because the proportion of patients who underwent colpectomy was higher in the PRF group than in the control [8/9 (89%) vs. 55/189 (29%), respectively;
Jelenc et al. 41 found that 2 of 52 patients with DIE developed PRF and that both of them had undergone concomitant vaginal and rectal resection without protective ileostomy. Whether a protective ileostomy can truly prevent PRF remains unclear. Moreover, a temporary colostomy would be very invasive for patients with benign disease. 42 Milone et al. 43 conducted a prospective multicenter case-control study involving 90 patients with bowel DIE. More ileostomies were performed in patients without than with complications (18/68 vs. 4/22, respectively). In the present study, we found that only one of four patients who underwent BRA with prophylactic ileostomy developed PRF.
Some scholars have mentioned that the surgeon’s experience may influence the development of complications both intraoperatively and postoperatively. Dubernard et al. 19 reported that 9 of 58 (15.5%) patients developed postoperative complications, which was a relatively higher rate than in other studies. They considered that a lack of experience in laparoscopic colorectal resection for endometriosis was a possible reason for this high rate. Actually, when treating DIE, a multidisciplinary team comprising gynecologists, urologists, and general surgeons should work together in a specific center.44,45 Radiological assessment is also quite important to assess the disease. 46 Fortunately, all patients in our cohort underwent their operations by the same surgical team, which might have reduced bias and allowed for consistency in the diagnosis and management of DIE.
In summary, we suggest great caution in treating patients with large DIE lesions. Because of its retrospective nature, this study has some inherent limitations such as recall bias, selection bias, and others. A prospective study with more patients will be necessary to draw more solid conclusions. Moreover, specialized centers with multidisciplinary collaboration involving radiologists and a surgical team with an experienced urological surgeon and/or gastrointestinal surgeon would be quite essential in treating patients with DIE. Additionally, adequate communication before surgery should be ensured, and patients should be fully informed of the risk of potentially severe complications such as PRF.
Footnotes
Authors’ note
Yunxi Zheng contributed to performance of the clinical study and participated in the manuscript writing. Ning Zhang contributed to the patient follow-up. Ying Zhang contributed to the case organization and statistical analysis. Yan Ning performed the histopathological examination. Weiqi Lu and Liang Zhang were the gastrointestinal surgeon and urological surgeon respectively, and they worked together with the gynecological surgeons in the DIE-related surgeries. Xiaofang Yi and Keqin Hua contributed equally to the design of this study.
Acknowledgments
The authors thank Dr. Xianrong Zhou from the Obstetrics and Gynecology Hospital of Fudan University for providing support in the pathological diagnosis.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
